US Pharm. 2015;40(8):HS20-HS24.
ABSTRACT: Smoking contributes to comorbidities that may lead to hospitalization. When smokers are admitted to a hospital, healthcare professionals are in an optimal position to implement effective strategies to promote smoking cessation. Whether the smoker is admitted to the ICU or to a general medical floor, research shows that nicotine replacement therapy (NRT) in conjunction with behavioral counseling increases the chance of abstinence. Data supporting initiation of NRT in the ICU patient are conflicting, while its benefits in the general hospitalized patient support a longer duration of smoking cessation post discharge.
Smoking is the leading cause of preventable death in the United States; in 2013, 17.8% of adults were smokers.1 Of the estimated 42.1 million active U.S. smokers, more than 70% visit a clinician every year.2 Active smokers admitted to the hospital often receive nicotine replacement therapy (NRT) to prevent nicotine withdrawal and reduce the risk of complications.3 Researchers have assessed NRT in various hospital settings; however, results of these trials complicate a clinician’s decision about whether to provide NRT to hospitalized patients. Some researchers report negative outcomes such as increased mortality in the critically ill.4,5 Successful smoking cessation after discharge appears to be more common in hospitalized patients prescribed NRT who also receive behavioral counseling.3,6 The aim of this article is to review the use of NRT in hospitalized patients.
Nicotine
Nicotine is a ganglionic (nicotinic) cholinergic-receptor agonist that has sympathomimetic properties. It increases myocardial oxygen demand while diminishing supply through vasoconstriction, thereby resulting in increased blood pressure and heart rate.7 Most smokers will become addicted to nicotine, placing them at risk for withdrawal.8 NRT provides an alternative source of nicotine. Stimulation of nicotine receptors minimizes withdrawal symptoms and cravings. Peak withdrawal symptoms, which occur within the first 72 hours of cessation, include nicotine cravings, irritability, anxiety, restlessness, sleep disturbances, and decreased heart rate. In the hospital setting, the primary goal of NRT is to reduce withdrawal symptoms and prevent associated com-plications that may worsen comorbidities (e.g., coronary artery disease, myocardial infarction, asthma).9 Hospitalization provides smokers with the opportunity to stop smoking.
NRT When Hospitalized
Upon admission to the hospital, smokers should first be assessed for willingness to quit, as with patients in the outpatient setting. Although current smokers may not be willing or ready to quit, treatment to decrease potential withdrawal and maximize the patient’s chance of cessation should be considered.10 NRT has been previously studied in patients admitted to the emergency department, ICU, or general medical floor.4,5,9-17 Although there is benefit in screening and treating patients at every transition of care, administration of NRT and counseling in the emergency department is difficult because of time restraints, available resources, and cost of care.10 Some have advocated that NRT be used when smoking is restricted, such as in the hospital setting, unless contraindicated.3,18
Intensive Care Unit
The ICU patient differs from other hospitalized patients because of complex medication regimens and disease severity. Authors of a recent systematic review of NRT in the ICU patient concluded that NRT may cause increased toxicity and should not be routinely prescribed, except when potential benefit clearly outweighs risk.4 This was based on results of five observational studies. Of these, two studies showed increased mortality in ICU patients who received NRT compared to those who do not.5,10
Lee and Afessa designed a retrospective case-control study in which smokers admitted to the medical ICU who received NRT were compared to those who did not.10 Hospital mortality rate was 20% (18/90) in the NRT group and 7% (6/90) in the control group (P = .0085). ICU-free days were lower in the NRT group compared to the control group: 20.7 10.5 days versus 23.4 7.1, respectively (P = .0488). However, when severity of illness and use of invasive ventilation were considered, NRT was associated with greater odds of mortality (odds ratio [OR] 24.6, 95% CI, 3.6-167.6; P = .0011). The retrospective nature of the study, the fact that patients were not matched according to current or lifetime tobacco use, and the fact that the use of NRT was physician-driven may impact validity.
Increased mortality was reported by Paciullo et al, who conducted a two-phase retrospective study.5 Phase I assessed mortality in smokers undergoing coronary artery bypass surgery (CABG) admitted to the cardiothoracic ICU through a matched case-control design. Mortality was greater in the NRT patients (3/67) compared to controls (0/67); P = .080. During phase II, researchers determined a baseline incidence of mortality for all patients undergoing CABG surgery. Mortality was not significantly greater in the NRT group (3/90) compared to smokers who did not receive NRT (1/489); P = .084. However, when age and atrial fibrillation were considered, mortality differed significantly from smokers who received NRT compared to smokers who did not (OR 6.06, 95% CI, 1.65-22.21).
Conversely, Cartin-Ceba and colleagues concluded that an increase in mortality is not associated with NRT; however, no clear benefit was seen.11 A prospective, observational cohort study was conducted in which 174 current smokers received NRT and 156 did not. Hospital mortality did not significantly differ between groups: NRT, 14/174 (7.8%; 95% CI, 4%-12%) and non-NRT, 10/156 (6.3%; 95% CI, 2.6%-10.3%); P = .59. Length of hospital and ICU stay did not differ significantly between groups.
Panos et al assessed pharmacy and medical records of patients admitted to the neuro-ICU and determined that NRT does not result in unfavorable outcomes after discharge.12 Outcomes were classified as unfavorable (required inpatient rehabilitation, nursing home or hospice care, or death) or favorable (discharge to home with or without outpatient rehabilitation). Unfavorable discharge status did not differ significantly between groups: NRT (42%), non-NRT (33%), nonsmokers (44%); P = .17.
Seder et al conducted a retrospective cohort study to evaluate NRT (n = 128) and non-NRT (n = 128) in smokers with acute (aneurysmal) subarachnoid hemorrhage (SAH) admitted to a neuro-ICU.13 At baseline, smokers receiving NRT were more likely to be heavy smokers (>10 cigarettes daily; P <.001), have a diagnosis of diabetes (P <.006), and have a diagnosis of cerebral edema (P <.001). Death at 3 months was significantly lower in smokers who received NRT (9/128) compared to those who did not (18/106); (OR 0.37, 95% CI, 0.16-0.86).
A small double-blind, placebo-controlled study was conducted in which 40 smokers admitted to the medical/surgical ICU were randomized to receive NRT or placebo for 10 weeks.14 There were no statistically significant differences in days on ventilator (NRT, 1.9 ± 3.7 versus non-NRT, 3.5 ± 5.3; P = .47) and days in the ICU (NRT, 4.5 ± 3.8 versus non-NRT, 7.0 ± 5.8; P = .08). Despite concern about the use of NRT in patients who suffered an acute coronary event (e.g., myocardial infarction and increased myocardial workload), some cardiologists use NRT to treat withdrawal symptoms.15
General Medical Floor
There are limited data assessing the use of NRT and effects on withdrawal symptoms in patients admitted to the general medical floor. However, initiation of NRT with behavioral counseling increases the chance that the patient will become a nonsmoker post discharge.16 Inpatient pharmacotherapy along with counseling significantly increases the chance of smoking cessation after discharge.17 Similarly, when NRT and counseling are delivered together, abstinence after discharge is more likely.18 According to results from a 2012 meta-analysis of 25 randomized clinical trials, hospitalized smokers who received at least 1 hour of intense counseling during their hospital stay and least 1 month of counseling post discharge increased their likelihood of smoking cessation (relative risk [RR] 1.37, 95% CI, 1.27-1.48).3 When NRT was added to counseling, the likelihood of smoking cessation increased further (RR 1.54, 95% CI, 1.34-1.79).18
Murray et al conducted an open cluster (per hospital ward) trial in which current smokers were randomized to an intervention group or a usual care group and assessed for smoking cessation at 4 weeks post discharge.17 At hospital admission, the usual care group (n = 229) received smoking cessation support at the discretion of the clinical team, while the intervention group (n = 264) received behavioral therapy, which involved one-on-one counseling and NRT. Smoking cessation, determined by exhaled carbon monoxide output at 4 weeks post discharge, was achieved in 96/260 (38%) of the intervention group and 37/224 (17%) of the usual care group (OR 2.10, 95% CI, 0.96-4.61) and at 6 months in 47/250 (19%) of the intervention group and 47/219 (19%) of the usual care group (OR 1.53, 95% CI, 0.60-3.91).
Molyneux et al randomized smokers admitted to the medical and surgical floor to receive either usual care (no additional formal interventions), counseling alone (trained specialists provided smoking cessation counseling) or counseling plus NRT.18 Smoking cessation rates, determined by exhaled carbon monoxide output, were significantly higher in patients who received NRT plus counseling (50/91, 54.9%; P = .04) compared to those who received counseling alone (39/91, 42.9%) or usual care (34/92, 37.0%). At 12 months post discharge, smoking cessation rates decreased for all groups; however, they were significantly higher for those patients who received NRT plus counseling (15/91, 16.5%; P = .03) compared to those who received counseling alone (5/91, 5.5%) or usual care (7/92, 7.6%).
Regan et al conducted an observational study to determine if smokers admitted to the hospital who received counseling with or without NRT were more likely to self-initiate or continue NRT within 2 weeks after discharge.19 Two weeks after discharge, patients were contacted by telephone and NRT use was determined; 72% responded to the survey, of which 42% (544/1,293) initiated NRT post discharge. Use of NRT post discharge was reported more often by patients who used NRT while in the hospital compared to those who used NRT prior to hospitalization (average rate ratio [ARR] 5.64, 95% CI, 3.95-8.05) or had never used NRT (ARR 4.68, 95%CI, 3.25-6.73).
Rigotti et al conducted a clinical trial in which hospitalized smokers (N = 397) were randomized to receive postdischarge sustained care (automated telephone calls plus NRT) or standard care (recommendations for therapy and counseling).20 At 6 months post discharge, tobacco abstinence rates were higher with sustained care (51/198, 25.8%) compared to standard care (30/199, 15%); P = .009. Initiating NRT in the hospital and providing postdischarge counseling and NRT encourage smoking cessation.
NRT Options and Counseling
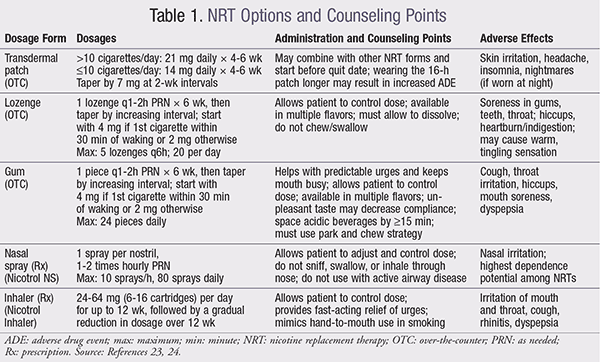
The American Heart Association and the U.S. Department of Health and Human Services recommend the use of NRT to help smokers quit smoking.21,22 FDA-approved NRT options include gum, lozenges, transdermal patches, a nasal spray, and an oral inhaler (TABLE 1).23,24 Patient counseling is specific to the dosage form. Although some patients may ask about e-cigarettes, these electronic nicotine delivery systems (ENDS) are not FDA-approved for NRT and cannot be recommended at this time. Varenicline and bupropion are FDA-approved for smoking cessation; data on use for NRT in hospitalized patients are lacking. A combination of NRT and counseling has proven to be beneficial for hospitalized patients.4,17-20
Conclusion
The benefits of NRT in the hospitalized patient include a greater chance that smokers will become nonsmokers when compared to smokers who are not offered NRT. Withdrawal symptoms in the ICU patient are undoubtedly managed through medical care received in the ICU. Although NRT has not been shown to unequivocally reduce hospital mortality or length of hospital stay, the benefits of NRT in conjunction with behavioral counseling support its use in hospitalized patients admitted to the general medical floor.
REFERENCES
1. CDC. Current cigarette smoking among adults—United States, 2005-2013. MMWR Morb Mortal Wkly Rep. 2014;63(47):1108-1112.
2. A clinical practice guideline for treating tobacco use and dependence: a U.S. Public Health Service report. The Tobacco Use and Dependence Clinical Practice Guideline Panel, Staff, and Consortium Representatives. JAMA. 2000;283(24):3244-3254.
3. Rigotti NA, Clair C, Munafò MR, Stead LF. Interventions for smoking cessation in hospitalized patients. Cochrane Database Syst Rev. 2012;5: CD001837.
4. Wilby KJ, Harder CK. Nicotine replacement therapy in the intensive care unit: a systematic review. J Intensive Care Med. 2014;29(1):22-30.
5. Paciullo CA, Short MR, Steinke DT, et al. Impact of nicotine replacement therapy on postoperative mortality following coronary artery bypass graft surgery. Ann Pharmacother. 2009;43:1197-1202.
6. U.S. Preventive Services Task Force. Counseling and interventions to prevent tobacco use, and tobacco-caused disease in adults, and pregnant women: U.S. Preventive Services Task Force reaffirmation recommendation statement. Ann Intern Med. 2009;150:551-555.
7. Hibbs RE, Zambon AC. Chapter 11. Agents acting at the neuromuscular junction and autonomic ganglia. In: Brunton LL, Chabner BA, Knollmann BC, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 12th ed. New York, NY: McGraw-Hill; 2011.
8. National Institute on Drug Abuse. Research Report Series: Is Nicotine Addictive? Bethesda, MD: National Institutes of Health; 2012.
9. Bernstein SL, Boudreaux ED, Cydulka RK, et al. Tobacco control interventions in the emergency department: a joint statement of emergency medicine organizations. Ann Emerg Med. 2006;48(4):e417-e426.
10. Lee AH, Afessa B. The association of nicotine replacement therapy with mortality in a medical intensive care unit. Crit Care Med. 2007;35(6): 1517-1521.
11. Cartin-Ceba R, Warner DO, Hays JT, Afessa B. Nicotine replacement therapy in critically ill patients: a prospective observational cohort study. Crit Care Med. 2011;39(7):1635-1640.
12. Panos NG, Tesoro EP, Kim KS, Mucksavage JJ. Outcomes associated with transdermal nicotine replacement therapy in a neurosurgery intensive care unit. Am J Health Syst Pharm. 2010;67(16):1357-1361.
13. Seder DB, Schmidt JM, Badjatia N, et al. Transdermal nicotine replacement therapy in cigarette smokers with acute subarachnoid hemorrhage. Neurocrit Care. 2011;14:77-83.
14. Pathak V, Rendon IS, Lupu R, et al. Outcome of nicotine replacement therapy in patients admitted to ICU: a randomized controlled double-blind prospective pilot study. Respir Care. 2013;58(10):1625-1629.
15. U.S. Department of Health and Human Services. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health; 2014.
16. Williams JH, Jones TE. Smoking cessation post-discharge following nicotine replacement therapy use during an inpatient admission. Intern Med J. 2012;42(2):154-159.
17. Murray RL, Leonardi-Bee J, Marsh J, et al. Systematic identification and treatment of smokers by hospital based cessation practitioners in a secondary care setting: cluster randomised controlled trial. BMJ. 2013;347:f4004.
18. Molyneux A, Lewis S, Leivers U, et al. Clinical trial comparing nicotine replacement therapy (NRT) plus brief counseling, brief counseling alone, and minimal intervention on smoking cessation in hospital inpatients. Thorax. 2003;58(6):484-488.
19. Regan S, Reyen M, Richards AE, et al. Nicotine replacement therapy use at home after use during a hospitalization. Nicotine Tob Res. 2012;14(7):885-889.
20. Rigotti NA, Regan S, Levy DE, et al. Sustained care intervention and postdischarge smoking cessation among hospitalized adults: a randomized clinical trial. JAMA. 2014;312(7):719-728.
21. Kernan WN, Ovbiagele B, Black HR, et al. Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2014;45:2160-2236.
22. Fiore MC, Jaén C, Baker T, et al. Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guideline. Rockville, MD: U.S. Department of Health and Human Services, Public Health Service; 2008.
23. Carpenter MJ, Jardin BF, Burris JL, et al. Clinical strategies to enhance the efficacy of nicotine replacement therapy for smoking cessation: a review of the literature. Drugs. 2013;73(5):407-426.
24. Drug information. LexiComp Online Drug Database. www.lexi.com. Accessed April 1, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.






