US Pharm. 2019;44(4):HS2-HS6.
ABSTRACT: The production of a beta-lactamase—a type of bacterial enzyme—is the most common mechanism of resistance to beta-lactam antibiotics among gram-negative bacteria. Extended-spectrum beta-lactamases (ESBLs) hydrolyze most penicillins, extended-spectrum cephalosporins, and aztreonam. Infections due to ESBL-producing organisms are associated with increased mortality. Once an ESBL is detected, appropriate treatment is important in order to ensure optimal patient outcomes. Infections caused by ESBLs are challenging to treat for various reasons, including difficulty in detecting ESBL-producing organisms as well as mixed data on how to best treat these infections. The increasing worldwide prevalence of infections caused by ESBL-producing organisms highlights the importance of antimicrobial-stewardship programs to promote appropriate use of antibiotics and lessen the risk of subsequent development of resistance.
Beta-lactam resistance to Escherichia coli was identified prior to the release of penicillin for clinical use, foreshadowing the importance of understanding the role of beta-lactamases—bacterial enzymes that cause resistance to beta-lactam antibiotics—in relation to drug selection.1 The early 1980s heralded the introduction of extended-spectrum cephalosporins, which became widely used for the treatment of serious infections at that time. Shortly after these antibiotics were introduced, extended-spectrum beta-lactamases (ESBLs) were first identified.2
ESBLs, which are produced by certain bacteria, preferentially hydrolyze extended-spectrum cephalosporins. ESBLs confer resistance to most beta-lactam antibiotics, including the penicillins, oxyimino-cephalosporins (e.g., ceftriaxone, cefotaxime, and ceftazadime), and monobactams (e.g., aztreonam). Notably, ESBLs can be inhibited—albeit to various degrees—by beta-lactamase inhibitors. Over the past 30 years, several beta-lactamase inhibitors have been introduced to combat resistance to these beta-lactamases, including ESBLs.
ESBLs continue to be a major clinical concern owing to an increased incidence throughout the United States that has resulted in increased risks of morbidity and mortality for patients.3,4 More than 200 ESBLs have been described in the past 30 years. ESBLs have been identified most commonly in Klebsiella pneumoniae, E coli, and Proteus mirabilis and in other gram-negative bacteria, such as Pseudomonas aeruginosa and Acinetobacter species.
ESBLs can be challenging to accurately detect. In June 2010, the Clinical Laboratory Standards Institute published new minimal inhibitory concentration (MIC) and susceptibility breakpoints for Enterobacteriaceae for cephalosporins and aztreonam. MIC breakpoints were lowered for many beta-lactam antibiotics, including extended-spectrum cephalosporins, to improve the detection of known resistance in Enterobacteriaceae. These new breakpoints simplified susceptibility testing for ESBL-producing organisms and rendered phenotypic confirmation unnecessary. Urinary tract infections (UTIs) constitute many of the clinical infections caused by ESBL-producing organisms; however, ESBLs have been implicated in a wide spectrum of infections ranging from superficial to invasive, including bacteremia, wound infections, pneumonia, intra-abdominal infections, and osteomyelitis.5,6
Epidemiology
ESBL-producing organisms have been reported throughout the world. Originally, these organisms were identified in large academic medical centers, but they have become more frequent causes of infection in smaller community hospitals and in outpatient settings.7 The rate of ESBLs has been increasing throughout the U.S. and worldwide. A recent study by McDanel and colleagues showed an increase in the incidence of ESBL-producing E coli and Klebsiella species from 1997 to 2011 in the U.S. In 2017, the incidence of ESBLs was about 16.64 infections per 10,000 discharges.8 The prevalence of ESBLs has also been increasing throughout the rest of the world, especially in Asia, Latin America, and the Middle East. The increasing rate of community-acquired ESBL infections has resulted from fecal colonization by ESBL-producing bacteria throughout the world, perpetuating the spread of this type of resistance.9
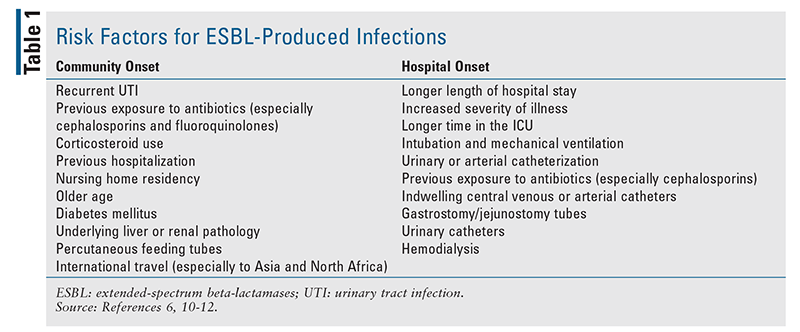
Many risk factors have been identified for infections that are caused by ESBL-producing organisms (TABLE 1). The gastrointestinal tract is the main reservoir for ESBL-producing Enterobacteriaceae, and colonization with such organisms is a strong risk factor for subsequent infection.6,10-12
Treatment
The treatment of infections that are caused by ESBL-producing organisms is often challenging because patient-specific characteristics as well as mitigation of resistance to other drug classes must be considered. Empiric therapy should be based on the site and severity of infection as well as local resistance patterns. Definitive therapy should be based on multiple factors, including known susceptibilities, source of infection, and properties of the antibiotic.11
Carbapenems: Agents in this antibiotic class are considered the drugs of choice for treatment of invasive infections caused by ESBLs. Carbapenem treatment often leads to improved patient-survival outcomes. Studies have found similar rates of clinical and microbiological outcomes compared with other carbapenems; however, ertapenem may not be active in vitro against all ESBL-producing Enterobacteriaceae. This can lead to the development of resistance in a patient who is treated with ertapenem.13 Ertapenem’s once-daily dosing is convenient, but this agent should be reserved for susceptible isolates in patients with mild-to-moderate disease. In contrast, there have been no clear differences in mortality with the use of imipenem-cilastatin or meropenem. The choice of agent should be based on toxicity profile; for example, meropenem is favored over imipenem-cilastatin in the setting of seizure disorder owing to potential central nervous system toxicity.14 Despite the typical preference for carbapenems in treating ESBL infections, sparing of carbapenem has been suggested because of an increase in the rate of carbapenem resistance. Carbapenem-hydrolyzing enzymes (carbapenemases) confer drug-to-drug resistance that has led to carbapenem-resistant Enterobacteriaceae.6,11
Alternative Agents: Given the rise in carbapenem resistance, other agents have been used as part of carbapenem-sparing strategies. In infections that have a well-defined nidus, such as UTIs, alternative agents with in vitro activity may be employed. Other antibiotics with potential activity against ESBL-producing bacteria include cefepime, piperacillin-tazobactam, eravacycline, plazomicin, omadacycline, ceftolozane-tazobactam, ceftazidime-avibactam, fosfomycin, nitrofurantoin, fluoroquinolones, and tigecycline. Each of these agents has variable activity, and selection should be made based on susceptibility as well as the source of infection. The use of fluoroquinolones and nitrofurantoin is commonly debated, with their use often dependent on susceptibility and the patient’s clinical status.
Beta-Lactam/Beta-Lactamase Inhibitors: Although beta-lactam antibiotics do not act against ESBL-producing organisms, studies have reported mixed outcomes in the use of some beta-lactam/beta-lactamase inhibitors compared with carbapenems. A meta-analysis conducted by Vardakas and colleagues evaluated 21 articles that compared mortality rates between carbapenems, beta-lactam/beta-lactamase inhibitors, and non–beta-lactam/beta-lactamase–inhibiting agents (primarily cephalosporins and fluoroquinolones) in patients with ESBL bloodstream infections.15 This meta-analysis, however, did not differentiate between community-acquired versus nosocomial infection sources, varying ages, levels of illness severity, or different sites of infection. Carbapenems were used mainly as definitive therapy. There were no statistically significant differences in mortality rates between carbapenems and beta-lactam/beta-lactamase inhibitors when given as empiric versus definitive therapy.15
Rodríguez-Baño and colleagues reported 740 cases of bacteremia due to ESBL-producing E coli in adult patients treated with either a beta-lactam/beta-lactamase inhibitor (IV piperacillin-tazobactam or IV amoxicillin-clavulanate) or a carbapenem.16 Most cases (~75%) were considered to have a urinary source. There was no statistically significant difference in mortality rates at day 30 for beta-lactam versus carbapenem treatment. They concluded that piperacillin-tazobactam and amoxicillin-clavulanate are suitable alternatives to carbapenems for treating patients with bloodstream infections due to ESBL E coli.16
The recent MERINO trial was the first to prospectively evaluate piperacillin-tazobactam versus meropenem as definitive treatment of bloodstream infections caused by ESBL E coli or K pneumoniae that displayed in vitro susceptibility to piperacillin-tazobactam but resistance to ceftriaxone.17 This noninferiority, parallel-group, randomized clinical trial included hospitalized patients from 26 sites in nine countries who were assigned 1:1 to IV piperacillin-tazobactam or meropenem. Treatment of ESBL E coli or K pneumoniae bacteremia with piperacillin-tazobactam was associated with increased 30-day mortality compared with meropenem. The MERINO trial was halted early by the safety monitoring board after a discussion with site investigators on the grounds of harm and futility based on the data.17 This trial provided some insight into preferred therapy in the setting of ESBL bacteremia.
Cephalosporins: There is limited evidence that selected cephalosporins could be an option for treating patients with ESBL-producing infections. Most studies do not support the use of cefepime, especially for bloodstream infections; however, some evidence exists that high-dose cefepime (2 g every 8 hours) can be effective for infections with a low bacterial burden, such as those originating in the urinary tract.6 Other studies, however, have found that cefepime is a suboptimal agent for the treatment of infections due to ESBL-producing organisms, especially invasive infections.18 At present, cefepime should not be considered a reliable treatment option for ESBL infections. The use of newer agents, such as ceftolozane-tazobactam and ceftazidime-avibactam, appears to be promising; however, data are too limited for the routine use of these agents to be recommended for ESBL infections.19,20
Oral Options: Because of the increasing risk of contracting an ESBL-producing pathogen in the community, it is important to understand potential oral treatment options in the outpatient setting. Current oral options for outpatient treatment of simple cystitis include fosfomycin, nitrofurantoin, fluoroquinolones, and amoxicillin-clavulanate. Fosfomycin is an oral broad-spectrum antibiotic that acts against many multidrug-resistant pathogens in the urinary tract. Multiple studies have showed success with fosfomycin 3 g every 48 to 72 hours for three doses.20 Nitrofurantoin is another potential option for simple cystitis, but it should be avoided in patients with compromised renal function. The renal elimination of nitrofurantoin is reduced in patients with low glomerular filtration rates; this can increase the risk of treatment failure and increase the risk of adverse drug events because of the drug not being eliminated.21,22 Fluoroquinolones may also be a possible option; however, high rates of resistance and unintentional harm limit their use.6 Owing to the recent findings of the MERINO trial, patients who have invasive disease should be considered for IV therapy.17
The Pharmacist’s Role
Pharmacists play a significant part in antimicrobial stewardship, including optimizing treatment in antimicrobial-therapy patients who have multidrug-resistant pathogens. It is estimated that up to 50% of antibiotic orders in hospitals are unnecessary.23 During the past 30 years, antibiotic development has slowed considerably, and options for treating increasingly resistant infections are becoming increasingly limited.24 It is important for the pharmacist to be cognizant of ESBL-producing pathogens and understand which antibiotics have the strongest data and outcomes. The pharmacist should be aware of the source of infection as well as the treatment options available.
Additionally, pharmacists can implement antimicrobial stewardship throughout their healthcare system, such as avoiding unnecessary use of antibiotics and de-escalating as soon as possible, which can help prevent patients from developing resistant pathogens. Antimicrobial stewardship can provide pharmacists with the tools necessary to avoid the overuse of antibiotics and to help prevent forms of antimicrobial resistance such as ESBLs.25 Pharmacists can play an integral role in assisting providers with the selection of appropriate antibiotics for these multidrug-resistant pathogens in order to improve patient outcomes.
Conclusion
ESBL-producing pathogens are increasing in prevalence around the world. Treatment strategies for these pathogens are becoming increasingly important owing to the limited number of treatment options and the high mortality risk. Infections with ESBL-producing organisms are associated not only with higher mortality rates but also with longer hospital stays and an increased cost burden on the healthcare system. ESBL-producing pathogens can be difficult to identify, and although an antibiotic may show susceptibility to the organism, resistance may still be a concern. The practitioner should weigh the risks and benefits as well as consider the current literature when selecting the most appropriate antibiotic for each patient. More data are needed to support the use of carbapenem-sparing strategies for infections with ESBL-producing pathogens, especially infections that are severe. Although the literature varies regarding the treatment of bloodstream infections, findings of the recent MERINO trial support the use of carbapenems over piperacillin-tazobactam specifically in patients who are bacteremic. Pharmacists can help improve patient outcomes by assisting in the selection of antibiotics appropriate for treatment of these multidrug-resistant pathogens.
REFERENCES
1. Abraham EP, Chain E. An enzyme from bacteria able to destroy penicillin. 1940. Rev Infect Dis. 1988;10(4):677-678.
2. Bradford PA. Extended-spectrum beta-lactamases in the 21st century: characterization, epidemiology, and detection of this important resistance threat. Clin Microbiol Rev. 2001;14(4):933-951.
3. Paterson DL, Bonomo RA. Extended-spectrum beta-lactamases: a clinical update. Clin Microbiol Rev. 2005;18(4):657-686.
4. Ghafourian S, Sadeghifard N, Soheili S, Sekawi Z. Extended spectrum beta-lactamases: definition, classification and epidemiology. Curr Issues Mol Biol. 2015;17:11-21.
5. Curello J, MacDougall C. Beyond susceptible and resistant, part II: treatment of infections due to gram-negative organisms producing extended-spectrum b-lactamases. J Pediatr Pharmacol Ther. 2014;19(3):156-164.
6. Chastain DB, White BP, Cretella DA, Bland CM. Is it time to rethink the notion of carbapenem-sparing therapy against extended-spectrum b-lactamase-producing Enterobacteriaceae bloodstream infections? A critical review. Ann Pharmacother. 2018;52(5):484-492.
7. Thaden JT, Fowler VG, Sexton DJ, Anderson DJ. Increasing incidence of extended-spectrum b-lactamase-producing Escherichia coli in the community hospitals throughout the Southeastern United States. Infect Control Hosp Epidemiol. 2016;37(1):49-54.
8. McDanel J, Schweizer M, Crabb V, et al. Incidence of extended-spectrum b-lactamase (ESBL)–producing Escherichia coli and Klebsiella infections in the United States: a systematic literature review. Infect Control Hosp Epidemiol. 2017;38(10):1209-1215.
9. Woerther PL, Andremont A, Kantele A. Travel-acquired ESBL-producing Enterobacteriaceae: impact of colonization at individual and community level. J Travel Med. 2017;24(suppl 1):S29-S34.
10. Lee JA, Kang CI, Joo EJ, et al. Epidemiology and clinical features of community-onset bacteremia caused by extended-spectrum b-lactamase-producing Klebsiella pneumoniae. Microb Drug Resist. 2011;17(2):267-273.
11. Pitout JD, Laupland KB. Extended-spectrum beta-lactamase-producing Enterobacteriaceae: an emerging public-health concern. Lancet Infect Dis. 2008;8(3):159-166.
12. Oteo J, Pérez-Vázquez M, Campos J. Extended-spectrum b-lactamase producing Escherichia coli: changing epidemiology and clinical impact. Curr Opin Infect Dis. 2010;23(4):320-326.
13. Lartigue MF, Poirel L, Poyart C, et al. Ertapenem resistance of Escherichia coli. Emerg Infect Dis. 2007;13(2):315-317.
14. Paterson DL, Ko W-C, Von Gottberg A, et al. Antibiotic therapy for Klebsiella pneumoniae bacteremia: implications of production of extended-spectrum b-lactamases. Clin Infect Dis. 2004;39(1):31-37.
15. Vardakas KZ, Tansarli GS, Rafailidis PI, Falagas ME. Carbapenems versus alternative antibiotics for the treatment of bacteraemia due to Enterobacteriaceae producing extended-spectrum b-lactamases: a systematic review and meta-analysis. J Antimicrob Chemother. 2012;67(12):2793-2803.
16. Rodríguez-Baño J, Navarro MD, Retamar P, et al. b-Lactam/b-lactam inhibitor combinations for the treatment of bacteremia due to extended-spectrum b-lactamase-producing Escherichia coli: a post hoc analysis of prospective cohorts. Clin Infect Dis. 2012;54(2):167-174.
17. Harris PNA, Tambyah PA, Lye DC, et al. Effect of piperacillin-tazobactam vs meropenem on 30-day mortality for patients with E coli or Klebsiella pneumoniae bloodstream infection and ceftriaxone resistance: a randomized clinical trial. JAMA. 2018;320(10):984-994.
18. Wang R, Cosgrove SE, Tschudin-Sutter S, et al. Cefepime therapy for cefepime-susceptible extended-spectrum b-lactamase-producing Enterobacteriaceae bacteremia. Open Forum Infect Dis. 2016;3(3):ofw132.
19. Levasseur P, Girard A-M, Miossec C, et al. In vitro antibacterial activity of the ceftazidime-avibactam combination against Enterobacteriaceae, including strains with well-characterized b-lactamases. Antimicrob Agents Chemother. 2015;59(4):1931-1934.
20. Farrell DJ, Flamm RK, Sader HS, Jones RN. Antimicrobial activity of ceftolozane-tazobactam tested against Enterobacteriaceae and Pseudomonas aeruginosa with various resistance patterns isolated in U.S. hospitals (2011-2012). Antimicrob Agents Chemother. 2013;57(12):6305-6310.
21. Reffert JL, Smith WJ. Fosfomycin for the treatment of resistant gram-negative bacterial infections. Insights from the Society of Infectious Diseases Pharmacists. Pharmacotherapy. 2014;34(8):845-857.
22. Singh N, Gandhi S, McArthur E, et al. Kidney function and the use of nitrofurantoin to treat urinary tract infections in older women. CMAJ. 2015;187(9):648-656.
23. Tulara NK. Nitrofurantoin and fosfomycin for extended spectrum beta-lactamases producing Escherichia coli and Klebsiella pneumoniae. J Glob Infect Dis. 2018;10(1):19-21.
24. Fleming-Dutra KE, Hersh AL, Shapiro DJ, et al. Prevalence of inappropriate antibiotic prescriptions among US ambulatory care visits, 2010-2011. JAMA. 2016;315:1864-1873.
25. Doron S, Davidson LE. Antimicrobial stewardship. Mayo Clin Proc. 2011;86(11):1113-1123.
To comment on this article, contact rdavidson@uspharmacist.com.






