US Pharm. 2018;(43):10-12.
By 2025, the prevalence of diabetes mellitus (DM) across the globe is expected to surpass 300 million, with approximately one-quarter of cases developing a foot ulcer.1 Importantly, when a diabetic foot ulcer—both neuropathic and ischemic—is infected, the risk of lower-extremity amputation is markedly increased, particularly when accompanied by osteomyelitis.2-4 Osteomyelitis, the inflammation of bone secondary to infection, is a common infectious disease among older patients.5,6
At presentation, more than 50% of diabetic foot ulcers are clinically infected, and among these infections, up to 50% involve bone.7-9 Osteomyelitis can affect any bone: the forefoot (90%); midfoot (5%); or hindfoot (5%).2 The prognosis is better for osteomyelitis in the forefoot than it is for the midfoot and hindfoot, with above-the-ankle amputation risk significantly higher for the hindfoot (50%) than midfoot (18.5%) and forefoot (0.33%).10-12
It is inherently difficult to treat infections in patients with DM because of their impaired microvascular circulation, which ultimately limits access of phagocytic cells to the infected area and causes poor concentration of antibiotics in the infected tissues.13 Compounding this treatment difficulty, older adults require careful antibiotic dosage adjustment for age-associated renal function in order to ensure adequate doses and duration of treatment. Pharmacists can provide recommendations for appropriate antibiotic selection, proper guidance regarding dosing, and specific and ongoing monitoring (e.g., renal and hepatic function, CBC), which are particularly important in the long-term treatment of diabetic foot osteomyelitis.
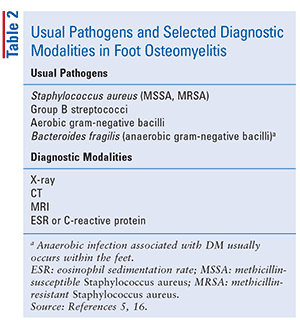
Hematogenous osteomyelitis (TABLE 1) is more common in young patients than adults, with most cases occurring in children under age 16 years.14,15 However, older age is considered a risk factor for hematogenous osteomyelitis; predisposing factors include IV catheters, indwelling urinary catheters, and DM. Contiguous osteomyelitis (TABLE 1) is more common in adults and in the feet of patients with DM or peripheral vascular disease; it causes approximately 80% of osteomyelitis cases.16 Most patients with contiguous osteomyelitis in association with severe vascular insufficiency have DM or severe atherosclerosis and are between age 50 to 70 years.15 This chronic form of osteomyelitis occurs secondary to contiguous spread from adjacent soft-tissue infection, and is more commonly polymicrobial as compared with hematogenously spread osteomyelitis.15,16 Staphylococcus aureus (including both methicillin-sensitive and methicillin-resistant strains) is present in 50% or more of patients with osteomyelitis; usual pathogens in foot osteomyelitis associated with DM in elderly patients are noted in TABLE 2.16 Anaerobic infection associated with DM usually occurs in the feet.16
Presentation and Diagnosis
Older adults with DM-associated osteomyelitis of the feet present with deep ulcers; the usual anatomical involvement is the plantar surface of the foot, or, to a lesser extent, ulcers between the toes.5 This presentation contrasts with other patients who present with a chronic draining sinus tract without an ulcer. According to Yoshikawa and colleagues, diabetic patients who present with chronic, deep-penetrating foot ulcers and/or a chronic draining sinus tract of the foot should be considered as having chronic osteomyelitis until proven otherwise. Data indicate a high positive correlation between these conditions and chronic osteomyelitis on bone scan.17,18 An early and accurate diagnosis is required to reduce the risk of amputation.2 General diagnostic modalities used for foot osteomyelitis associated with DM in older adult patients, and general features of chronic osteomyelitis in patients with DM, are outlined in TABLES 2 and 3, respectively.
Antibiotic Therapy
In the treatment of osteomyelitis with acute presentation, the most important points regarding antibiotic therapy are:15
• Appropriate agent (culture and sensitivity data are not always available)
• Adequate doses
• Sufficient length of time
For mild infections, oral therapy covers skin flora including streptococci and Staphylococcus aureus. For moderate-to-severe infections, empiric parenteral therapy should cover streptococci, methicillin-resistant S aureus (MRSA), aerobic gram-negative bacilli, and anaerobes: 1) MRSA is covered by vancomycin, linezolid, or daptomycin; 2) Acceptable choices for gram-negative aerobic organisms and anaerobes include ampicillin-sulbactam, piperacillin-tazobactam, meropenem, or ertapenem; 3) Alternatively, ceftriaxone, cefepime, levofloxacin, moxifloxacin, or aztreonam plus metronidazole would be sufficient to cover aerobic gram-negative and anaerobic organisms; 4) Tigecycline; however, published studies of this drug are limited.13
It is worth noting that:19
• No adjustment for renal function is necessary with ceftriaxone in the elderly.
• The risk of torsades de pointes and tendon inflammation and/or rupture associated with the concomitant use of corticosteroids and quinolones is increased in the elderly.
• Total and unbound AUCs were increased in healthy men and women aged 65 years receiving ertapenem.
Although current guidelines recommend at least 3 months or more of antibiotic therapy when diabetic foot osteomyelitis is not treated surgically or when residual dead bone remains after surgery, according to a recent randomized prospective study, even in the absence of surgery, a 6-week course of antibiotics may be sufficient to treat patients with diabetic foot osteomyelitis.13,20,21 The study indicated remission in those patients treated for 6 weeks (12 patients, 60%) and in those patients treated for 12 weeks (14 patients, 70%) (P = 0.50).20,21 For authoritative guidelines addressing evaluation and management of diabetic foot infections, including antimicrobial agents, refer to Reference 22.
Surgical Debridement
In addition to antimicrobial therapy, adequate surgical debridement is necessary to cure chronic osteomyelitis, because systemic antibiotics do not penetrate devascularized bone fragments; immobilization is also important in both acute and chronic osteomyelitis.13 Dry gangrene and wet gangrene should be managed with surgical debridement and/or antimicrobial therapy as appropriate.13 With regard to long-term monitoring, acute osteomyelitis requires monitoring the patient’s condition to ensure that the infection has resolved; chronic osteomyelitis monitoring must ensure that debridement is complete so that residual infected bone is no longer present.13
Role of the Pharmacist
Osteomyelitis is a common infectious disease among older adults and one of the most common expressions of diabetic foot infection. Since infections may complicate diabetic foot ulcers in both neuropathic and ischemic ulcers, osteomyelitis in the foot of a patient with DM requires an early and accurate diagnosis. Pharmacists may guide tailored treatment for older adults to provide appropriate antibiotic therapy, in adequate doses, for a sufficient length of time, to ensure targeted treatment and reduce the risk of major amputation.
REFERENCES
1. Singh N, Armstrong DG, Lipsky BA. Preventing foot ulcers in patients with diabetes. JAMA 2005;293:217-228.
2. Giurato L, Meloni M, Izzo V, et al. Osteomyelitis in diabetic foot: a comprehensive overview. World J Diabetes. 2017;8(4):135-142.
3. Carmona GA, Hoffmeyer P, Herrmann FR, et al. Major lower limb amputations in the elderly observed over ten years: the role of diabetes and peripheral arterial disease. Diabetes Metab. 2005;31:449-454.
4. Lavery LA, Armstrong DG, Wunderlich RP, et al. Risk factors for foot infections in individuals with diabetes. Diabetes Care 2006;29:1288-1293.
5. Yoshikawa TT, Cunha BA. Osteomyelitis in elderly patients. Clin Infect Dis. 2002;35(3):287-293.
6. Zagaria MA. Risk of osteomyelitis with joint replacement. US Pharm. 2018;43(4):16-18.
7. Aslangul E. M’Bemba J, Caillat-Vigneron N et al. diagnosing diabetic foot osteomyelitis in patients without signs of soft tissue infection by coupling hybrid 67Ga SPECT/CT with bedside percutaneous bone puncture. Diabetes Care 2013; 36(8):2203-2210.
8. Lavery LA, Peters EJ, Armstrong DG, et al. Risk factors for developing osteomyelitis in patients with diabetic foot wounds. Diabetes Res Clin Pract. 2009;83:347-352.
9. Richard JL, Lavigne JP, Got I, et al. Management of patients hospitalized for diabetic foot infection: results of the French OPIDIA study. Diabetes Metab. 2011;37:208-215.
10. Aragón-Sánchez FJ, Cabrera-Galván JJ, Quintana-Marrero Y, et al. Outcomes of surgical treatment of diabetic foot osteomyelitis: a series of 185 patients with histopathological confirmation of bone involvement. Diabetologia. 2008;51:1962-1970.
11. Aragón-Sánchez J, Lázaro-Martínez JL, Hernández-Herrero C, et al. Does osteomyelitis in the feet of patients with diabetes really recur after surgical treatment? Natural history of a surgical series. Diabet Med. 2012;29:813-818.
12. Faglia E, Clerici G, Caminiti M, et al. Influence of osteomyelitis location in the foot of diabetic patients with transtibial amputation. Foot Ankle Int. 2013;34:222-227.
13. Bronze MS. Diabetic foot infections treatment & management. Medscape.com. Updated March 5, 2018. https://emedicine.medscape.com/article/237378-treatment#d9. Accessed September 11, 2018.
14. Orenstein R. Infectious diseases. In: Habermann TM, Ghosh AK, eds. Mayo Clinic Internal Medicine Concise Textbook. Mayo Clinic Scientific Press and Informa Healthcare USA, Inc. 2008: 514-515.
15. Armstrong EP, Shehab Z. Bone and joint infections. In: DiPiro JT, Talbert RL, Yee GC, et al. Pharmacotherapy: A Pathophysiologic Approach, 10th ed. New York, NY:McGraw-Hill Education; 2017:1885-1895.
16. Schmitt S. Osteomyelitis. merckmanuals.com. Last full review/revision May 2017. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/infections-of-joints-and-bones/osteomyelitis. Accessed September 12, 2018.
17. Braun TI, Lorber B. Chronic osteomyelitis, In: Schlossberg D, ed. Orthopedic Infection. New York: Springer-Verlag;1988:9-20.
18. Waldvogel FA, Medoff G, Swarz MN. Osteomyelitis: a review of clinical features, therapeutic considerations, and unusual aspects. 3. Osteomyelitis associated with vascular insufficiency. N Engl J Med. 1970;282:316-22.
19. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 20th ed. Hudson, OH: Lexicomp; 2015:96,253,287,914,957,1169.
20. Tucker M. Short-course antibiotics good in diabetic foot osteomyelitis. Medscape Medical News. November 26, 2014.
21. Tone A, Nguyen S, Devemy F, et al. Six-versus twelve-week antibiotic therapy for nonsurgically treated diabetic foot osteomyelitis: a multicenter open-label controlled randomized study. Diabetes Care. Epub November 20, 2014.
22. Lipsky BA, Berendt AR, Cornia PB, et al. 2012 Infectious Diseases Society of America clinical practice guideline for the diagnosis and treatment of diabetic foot infections. Clin Infect Dis. 2012;54(12):e132-e173.
23. Hellman DB, Imboden JB. Rheumatologic, immunologic, & allergic disorders. In: Papadakis MA, McPhee SJ, Rabow MW, eds. Current Medical Diagnosis & Treatment, 56th ed. New York, NY: McGraw Hill Education; 2017:870-871.
24. Schmitt S. Prosthetic joint infectious arthritis. Merckmanuals.com. Last full review/revision May 2017. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/infections-of-joints-and-bones/prosthetic-joint-infectious-arthritis. Accessed March 1, 2018.
25. Cunha BA. Antibiotic selection for diabetic foot infections: a review. J Foot Ankle Surg. 2000;39:253-257.
To comment on this article, contact rdavidson@uspharmacist.com.