US Pharm. 2015;40(6):HS4-HS-8.
ABSTRACT: HIV ocular infections are becoming more common as HIV/AIDS continues to transition to a chronic disease. Ocular infections, which range from minor to severe, can be caused by organisms that would not normally result in infection in immunocompetent individuals. There are many causative organisms, and they can be protozoal, bacterial, fungal, or viral in origin. Because of the number and diversity of organisms, the treatment approach is varied and may require the use of less common medications. Proper identification and treatment of HIV ocular infections is important because of potentially serious sequelae, such as blindness. Pharmacists can play a pivotal role in the treatment of HIV ocular infections.
Approximately 35 million people worldwide have HIV, with about 1 million of these in the United States.1,2 HIV affects many areas of the body, including the eyes, and 70% of HIV patients will experience HIV-related ocular disease as the virus progresses to the final stage of infection (AIDS). Ocular manifestations in HIV patients range from less severe, cosmetic issues to complete blindness.3 With the development and implementation of highly active antiretroviral therapy in 1996, the incidence of more severe ocular conditions has diminished, but the incidence of less severe, chronic ocular disorders—including viral, protozoal, bacterial, and fungal infections—has increased.3,4 This article will discuss some common HIV ocular infections that may be encountered routinely in many pharmacy practices.
Protozoal Infections
Microsporidia and Toxoplasma gondii are two types of protozoal parasites known to cause eye infections in HIV and other immunocompromised patients. Microsporidia are intracellular obligate protozoal parasites that can cause keratoconjunctivitis, keratitis, or corneal microsporidiosis in HIV-infected patients.3
Microsporidial Infections: Microsporidial ocular infections in AIDS patients and other immunocompromised patients differ from those in healthy patients. Microsporidial keratoconjunctivitis in HIV patients is characterized by bilateral involvement, as opposed to infections in healthy patients, which are usually unilateral. Patients may complain of photophobia and grittiness in the eye. Microsporidial keratitis can eventually cause blindness. HIV patients with CD4 (cluster determinant 4) counts <200 cells/mcL are at increased risk for microsporidial infections. To prevent disease, it is recommended that such patients avoid untreated water sources, since microsporidia are waterborne parasites. It is also advisable for these patients to practice good hand hygiene, refrain from eating undercooked meat or seafood, and avoid animals known to be infected with microsporidia. Early initiation of antiretroviral therapy (ART) is recommended to prevent microsporidial and other opportunistic infections in HIV patients.3 Treatment options for microsporidiosis are listed in TABLE 1.
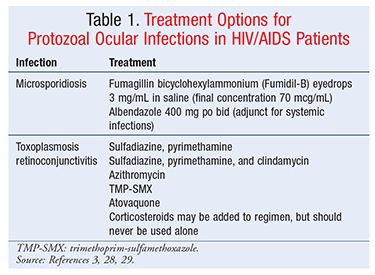
T gondii Infections: T gondii is an obligate intracellular protozoal parasite that affects 1% to 2% of HIV-positive patients. Cats are the only known primary hosts of T gondii, which can be spread to humans through direct and indirect ingestion of spores shed in cat feces. T gondii usually infects the choroid and retina of HIV patients, causing retinochoroiditis. Up to 66% of these patients present with anterior uveitis or vitritis. Patients may complain of ocular redness and/or pain or the presence of black floating spots in their vision field. HIV patients with T gondii retinochoroiditis tend to have bilateral or multifocal disease, whereas immunocompetent patients usually present with unilateral or isolated disease. However, patients with a primary infection may present with anterior uveitis without retinal lesions. Up to 50% of HIV patients presenting with ocular toxoplasmosis also have T gondii encephalitis. Toxoplasmosis is rare in patients with CD4 counts >200 cells/mcL and usually affects those with CD4 counts <50 cells/mcL.3-5
To minimize the risk of exposure to T gondii, HIV patients should be counseled not to consume raw or undercooked meats or shellfish. HIV patients should wash their hands thoroughly after handling raw meats and after gardening or having other contact with soil, and they should be advised to wash fruits and vegetables well before consuming them raw. HIV-infected patients may own house cats; however, they should not change the litter box themselves. If it is necessary for an HIV-infected patient to clean the litter box, the hands should be thoroughly washed afterward. Primary prophylaxis is indicated in all HIV patients with a CD4 count <100 cells/mcL and is continued until CD4 counts are >200 cells/mcL for ≥3 months in response to ART. After successful treatment of toxoplasmosis, secondary prophylaxis is indicated until the patient’s CD4 count increases to >200 cells/mcL for ≥6 months and the patient has no signs and symptoms of active infection.3-5 Treatment options for ocular toxoplasmosis are outlined in TABLE 1.
Bacterial Infections
Two of the most common intraocular bacterial infections in HIV-positive patients are caused by Mycobacterium tuberculosis and Treponema pallidum. M tuberculosis produces one of the most common systemic opportunistic infections found in AIDS patients. Tuberculosis may be spread from person to person by coughing, sneezing, or even speaking. Ocular tuberculosis is rare and usually seen only in developing countries.6 HIV patients with CD4 counts <200 cells/mm3 are at increased risk for acquiring this infection.7 Intraocular infection, which is often a result of hematogenous spread during pulmonary tuberculosis, has been shown to manifest as a unilateral and asymmetrical infection often causing anterior uveitis and sclerokeratitis.6
Rarely, cutaneous tuberculosis can occur at the conjunctiva or cornea as a result of primary cutaneous infection. It is often characterized as a granulomatous anterior uveitis in which the severity of the inflammation correlates with the CD4 cell count.8 Eyelid lesions may present with erythema and swelling and may sometimes be mistaken for chalazia.7 Such scleral lesions may necrotize if left untreated.9 Standard tuberculosis treatment should be initiated, with consideration of extended treatment duration and selection of additional drugs designed to treat multidrug-resistant tuberculosis.8 In some cases, patients have been treated with topical and subconjunctival streptomycin sulfate, along with systemic antituberculous therapy, for scleral treatment of lesions.8 Patients with HIV are at higher risk for acquiring tuberculosis when traveling internationally or working in a high-prevalence area, and accordingly should be cautious in such environments.7 Treatment options for ocular tuberculosis, which mirror the standard therapy for systemic tuberculosis, appear in TABLE 2.
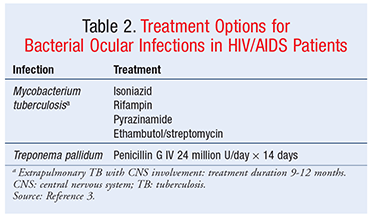
T pallidum Infections: Better known as syphilis, T pallidum infection often manifests as a more aggressive, severe, and relapsing disease in HIV-positive patients compared with immunocompetent hosts.10-12 T pallidum has been associated with an increased risk of sexual acquisition and transmission of HIV.3 It is estimated that 20% of HIV patients with concurrent syphilis will have ocular manifestations capable of causing both anterior and posterior segment inflammation.13 T pallidum often presents as a diffuse intraocular inflammation capable of involving the optic nerve and retina, leading to compromised visual acuity and even blindness.14 Cataracts can also develop in patients with syphilis, as a result of uveal inflammation.15
Ocular manifestations of T pallidum can sometimes distinguish the stage of infection. For example, painless chancres in the conjunctiva may be seen in primary syphilis; in the secondary stage, conjunctivitis, papillitis, and retrobulbar neuritis may present; and, in the tertiary stage, cranial nerve palsies and optic atrophy may occur.16 Despite these various stages of infection, ophthalmic abnormalities are usually a manifestation of neurosyphilis and can occur at any time. Several studies have demonstrated that, in HIV-infected patients with syphilis, clinical and cerebrospinal-fluid abnormalities consistent with neurosyphilis are associated with CD4 counts ≤350 cells/mm3. Patients with syphilitic eye findings should receive the same treatment prescribed for neurosyphilis.4 Because of the high relapse rate, it is recommended that HIV-positive patients have extensive follow-up over the next 2 years.15 Patients should be counseled on safe-sex practices, which will reduce the risk of acquiring sexually transmitted diseases and HIV.3 Treatments for T pallidum are found in TABLE 2.
Fungal Infections
Fungal species known to cause keratitis in HIV/AIDS patients include Candida albicans and Aspergillus. Cryptococcus neoformans is another fungus that can cause eye problems.
C albicans Infections: C albicans is the most common causative organism and is prevalent among IV drug users.17 Known to cause anterior segment keratitis, the organism produces a fluffy white “mound” of fungal lesions.18 C albicans may also cause endophthalmitis, which presents as a focal white infiltrate in the choroid and may break through the retina into the vitreous.18 Patients may experience blurred or decreased vision resulting from macular chorioretinal involvement or pain arising from anterior uveitis, which may be severe.19 Predisposing conditions associated with candidemia and the development of intraocular infection include hospitalization with a history of recent major gastrointestinal surgery, bacterial sepsis, systemic antibiotic use, indwelling catheters, hyperalimentation, debilitating diseases (e.g., diabetes mellitus), immunomodulatory therapy, prolonged neutropenia, organ transplantation, or a combination of these.19 The treatment of intraocular candidiasis includes IV and intravitreal administration of various antifungal agents, as described in TABLE 3.
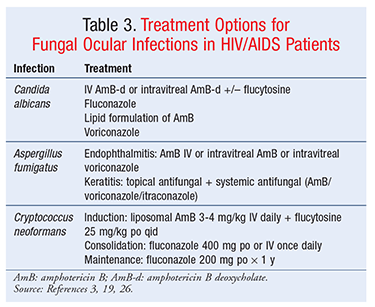
Aspergillus Infections: Aspergillus infections are relatively uncommon in patients with advanced HIV.20 Aspergillus endophthalmitis is a devastating infection that may result in permanent vision loss and rapid eye destruction. Infection may occur by one of several mechanisms: hematogenous dissemination, direct inoculation by trauma, and contamination by surgical procedure.21-23 Aspergillus species are ubiquitous in the environment, and exposure is unavoidable.3 Patients should avoid dusty environments, such as construction sites, since spore counts likely are higher in these areas.3 Another ocular manifestation of the fungus is aspergillus keratitis, which most commonly results from traumatic inoculation of Aspergillus into the cornea through injury or surgical procedures.24-27 Aspergillus keratitis is frequently observed in agricultural workers who suffer abrasions of the cornea from branches and leaves while working in fields. In addition to endophthalmitis and keratitis, cases of orbital lymphoma and orbital cellulitis have been reported, most often related to Aspergillus infection.18 Currently, antifungal therapy is not recommended for prevention of aspergillosis in HIV patients. Treatment in these patients has not been systematically examined; however, owing to drug-drug interactions between first-line therapy and antiretrovirals, preferred therapy with voriconazole should be used with caution.3 Second-line agents should be considered (TABLE 3).
C neoformans Infections: C neoformans is a budding, spore-forming, yeastlike fungus that is acquired by inhalation of spores often found in bird droppings. This life-threatening opportunistic pathogen may be acquired at CD4 counts <100 cells/mm3 and is often related to central nervous system (CNS) disease.3 The most common cause of neuro-ophthalmologic lesions in HIV/AIDS patients, C neoformans is often seen in association with cryptococcal septicemia or meningeal infection.26 C neoformans has been reported more in developing countries and is characterized as infecting the posterior segment of the eye.7 Patients may experience granulomatous conjunctivitis and multiple yellowish-white chorioretinal lesions. This can lead to visual loss, owing to involvement of the optic chiasm, nerve, and tract.27 Extrapulmonary cryptococcosis should be treated similarly to cryptococcal CNS disease.28 Treatment of cryptococcosis consists of three phases: induction, consolidation, and maintenance therapy.3 Therapy options are described in TABLE 3.
Viral Infections
HIV-infected patients may develop viral ocular infections, including herpes simplex virus, varicella zoster virus (VZV), cytomegalovirus (CMV), and molluscum contagiosum.3,29,30 Molluscum contagiosum, which is caused by a poxvirus, affects about 5% of HIV-infected patients.3,30 In adults, molluscum contagiosum is usually sexually transmitted, but it can also be transmitted through infected fomites, including bedding, towels, and clothing. Molluscum contagiosum occurs in both immunocompetent and immunocompromised patients; however, in HIV-infected patients, lesions of the eyelids and conjunctiva are more common, and the lesions are larger and more numerous. Additionally, infections in HIV-infected patients are usually more resistant to treatment. Molluscum contagiosum is characterized by wartlike umbilicated nodules that are usually pearly-white to pink in color and about 2 to 3 mm in size. There are few pharmacologic therapies for molluscum contagiosum, and even after treatment, the lesions may reappear. However, after ART is initiated and the patient regains his or her immune function, the lesions may resolve on their own.3,4,30 Treatment options for molluscum contagiosum appear in TABLE 4.
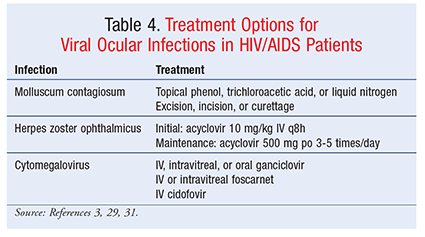
CMV Infections: CMV is a common pathogen that usually remains asymptomatic in immunocompetent patients. However, CMV retinitis is the leading cause of ocular opportunistic infections in HIV/AIDS patients. The incidence of CMV retinitis has decreased significantly since the development of ART, but it continues to be a concern for patients with low CD4 counts and progressed HIV. CMV retinitis presents in one of three forms: hemorrhagic, granular, or perivascular. Patients with CMV retinitis usually report a gradual loss of vision, as well as floaters in their field of vision. CMV retinitis is most common in patients with CD4 counts <50 cells/mcL and is rare in those with CD4 counts >100 cells/mcL. Treatment options include oral, IV, and intravitreal antiviral agents like foscarnet and ganciclovir; however, the best regimen is still being investigated.3,26,30
VZV Infections: VZV primary infection causes varicella (chickenpox), which becomes latent in sensory neurons and, when reactivated, causes herpes zoster (shingles). If VZV becomes reactivated in the ophthalmic division of the trigeminal nerve, it gives rise to herpes zoster ophthalmicus (HZO). HZO is a rare manifestation of HZV even in HIV patients, but may be the first sign of HIV infection. HZO has a variety of sequelae, ranging from zoster keratitis and uveitis to more severe acute retinal necrosis and peripheral ulcerative keratitis. Unlike immunocompetent patients, HIV-infected patients are more likely to have corneal involvement, including perforation. HZO lesions manifest along the trigeminal nerve dermatome as a vesiculobullous rash. The presentation of HZO in HIV-infected patients requires aggressive initial treatment followed by chronic maintenance therapy to prevent recurrence. Following the successful treatment of HZO and other VZV manifestations, a patient may experience postherpetic neuralgia, which may be more severe in HIV-infected patients than in their immunocompetent counterparts.3,31
Conclusion
As HIV/AIDS has become a more chronic condition over the years, there are now more opportunities to encounter patients with HIV-related ocular infections. Many of these infections are much more common in the HIV/AIDS population, and they vary greatly in both etiology and treatment because of the diversity of organisms causing them. Some of these infections are almost exclusively found in this immunocompromised population. Pharmacists in every setting should be familiar with HIV/AIDS ocular infections and how they are treated.
REFERENCES
1. UNAIDS. Fact sheet 2014. www.unaids.org/sites/default/files/en/media/unaids/contentassets/documents/factsheet/2014/20140716_FactSheet_en.pdf. Accessed February 10, 2015.
2. AVERT. HIV& AIDS in USA. www.avert.org/hiv-aids-usa.htm. Accessed February 10, 2015.
3. Guidelines for the prevention and treatment of opportunistic infections among HIV-exposed and HIV-infected children. MMWR. 2009;58:1-166.
4. Panel on Opportunistic Infections in HIV-Infected Adults and Adolescents. Guidelines for the prevention and treatment of opportunistic infections in HIV-infected adults and adolescents: recommendations from the Centers for Disease Control and Prevention, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. http://aidsinfo.nih.gov/contentfiles/lvguidelines/adult_oi.pdf. Accessed February 17, 2015.
5. Park YH, Nam HW. Clinical features and treatment of ocular toxoplasmosis. Korean J Parasitol. 2013;51:393-399.
6. Biswas J, Sudharshan S. Anterior segment manifestations of human immunodeficiency virus/acquired immune deficiency syndrome. Indian J Ophthalmol. 2008;56:363-375.
7. Bramante CT, Talbot EA, Rathinam SR, et al. Diagnosis of ocular tuberculosis: a role for new testing modalities? Int Ophthalmol Clin. 2007;47:45-62.
8. Bloomfield SE, Mondino B, Gray GF. Scleral tuberculosis. Arch Ophthalmol. 1976;94:954-956.
9. Wood R, Maartens G, Lombard CJ. Risk factors for developing tuberculosis in HIV-1-infected adults from communities with a low or very high incidence of tuberculosis. J Acquir Immune Defic Syndr. 2000;23:75-80.
10. McLeish WM, Pulido JS, Holland S, et al. The ocular manifestations of syphilis in the human immunodeficiency virus type 1-infected host. Ophthalmology. 1990;97:196-203.
11. Becerra LI, Ksiazek SM, Savino PJ, et al. Syphilitic uveitis in human immuno-deficiency virus-infected and noninfected patients. Ophthalmology. 1989;96:1727-1730.
12. Musher DM, Hamill RJ, Baughn RE. Effect of human immunodeficiency virus (HIV) infection on the course of syphilis and on the response to treatment. Ann Intern Med. 1990;113:872-881.
13. Biotti D, Bidot S, Mahy S, et al. Ocular syphilis and HIV infection. Sex Transm Dis. 2010;37:41-43.
14. Ali R, Kim JY, Henderson BA. Adnexal and anterior segment manifestations of HIV/AIDS. Int Ophthalmol Clin. 2007;47:15-32.
15. Margo CE, Hamed LM. Ocular syphilis. Surv Ophthalmol. 1992;37:203-220.
16. Ah-Fat FG, Batterbury M. Ophthalmic complications of HIV/AIDS. Postgrad Med J. 1996;72:725-730.
17. Rocha Lima B. Opthalmic manifestations of HIV infection. Digital J Ophthalmology. 2004;10(3).
18. Ahmed I, Ai E, Chang E, Luckie A. Ophthalmic manifestations of HIV. http://hivinsite.ucsf.edu/InSite?page=kb-04-01-12. Accessed January 17, 2015.
19. American Academy of Ophthalmology. Candida endophthalmitis. http://one.aao.org/bcscsnippetdetail.aspx?id=df51235c-c34b-4295-85a5-9365558cb82d. Accessed January 17, 2015.
20. Holding KJ, Dworkin MS, Wan PC, et al. Aspergillosis among people infected with human immunodeficiency virus: incidence and survival. Adult and Adolescent Spectrum of HIV Disease Project. Clin Infect Dis. 2000;31:1253-1257.
21. Aziz AA, Bullock JD, McGuire TW, et al. Aspergillus endophthalmitis: a clinical and experimental study. Trans Am Ophthalmol Soc. 1992;90:317-342.
22. Callanan D, Scott IU, Murray TG, et al. Early onset endophthalmitis caused by Aspergillus species following cataract surgery. Am J Ophthalmol. 2006;142:509-511.
23. Demicco DD, Reichman RC, Violette EJ, Winn WC Jr. Disseminated aspergillosis presenting with endophthalmitis. A case report and a review of the literature. Cancer. 1984;53:1995-2001.
24. Rahimi F, Hashemian MN, Rajabi MT. Aspergillus fumigatus keratitis after laser in situ keratomileusis: a case report and review of post-LASIK fungal keratitis. Eye (Lond). 2007;21:843-845.
25. Kuo IC, Margolis TP, Cevallos V, Hwang DG. Aspergillus fumigatus keratitis after laser in situ keratomileusis. Cornea. 2001;20:342-344.
26. Walsh TJ, Anaissie EJ, Denning DW, et al. Treatment of aspergillosis: clinical practice guidelines of the Infectious Diseases Society of America. Clin Infect Dis. 2008;46:327-360.
27. Cunningham ET Jr, Margolis TP. Ocular manifestations of HIV infection. N Engl J Med. 1998;339:236-244.
28. Kupfer C, McCrane E. A possible cause of decreased vision in cryptococcal meningitis. Invest Ophthalmol. 1974;13:801-804.
29. Butler NJ, Thorne JE. Current status of HIV infection and ocular disease. Curr Opin Ophthalmol. 2012;23:517-522.
30. Chiotan C, Radu L, Serban R, et al. Posterior segment ocular manifestations of HIV/AIDS patients. J Med Life. 2014;7:399-402.
31. Sanjay S, Huang P, Lavanya R. Herpes zoster ophthalmicus. Curr Treat Options Neurol. 2011;13:79-91.
To comment on this article, contact rdavidson@uspharmacist.com.





