US Pharm. 2019;44(6):15-18.
ABSTRACT: Medication adherence among adults and adolescents remains suboptimal in the United States. Medication nonadherence is a complex issue, and one strategy that may be helpful for improving adherence is a combination of behavioral theory and medication education. The pharmacist must take the patient’s health literacy into account when offering intervention and education. Patients are more likely to be receptive to change when they believe that they are acting independently to make that change. Motivational interviewing and use of the three prime questions have been found to be effective and may be used to improve patients’ medication knowledge, self-efficacy, intrinsic motivation, and—ultimately—medication adherence.
Medication adherence among adults and adolescents remains suboptimal in the United States. Former U.S. Surgeon General C. Everett Koop once stated, “Drugs don’t work in patients who don’t take them.”1 To help patients take their medications, pharmacists must be conversant with communication and behavioral strategies that can be used to improve adherence. Medication nonadherence has been recognized as a challenge that primary care providers increasingly face in practice, and pharmacist assistance is welcomed.2 Medication adherence is the “active, voluntary, and collaborative involvement of the patient in a mutually acceptable course of behavior to produce a therapeutic result.”1-3 Further, the term describes the patient’s ability to follow provider recommendations for prescribed treatments.4
Types of—and reasons for—nonadherence are diverse and complex. Patients may not believe that the medication is necessary, may never begin taking it, or may take more or less than prescribed; they may even prematurely stop taking it.4 To effectively increase patient medication adherence, pharmacists must adjust their approach based on the cause and type of nonadherence and on patient-specific needs. Tailored patient counseling that targets the underlying causes of nonadherence is one method of helping patients increase their medication-taking behaviors.4 Patients have specifically identified the pharmacist as a source of medication education.5 Therefore, pharmacists have a key opportunity to address medication nonadherence through patient communication. The use of behavioral theory in patient education and counseling can inform and improve medication adherence.6
Barriers to Adherence
Pharmacists should never assume that a patient is adherent. Patients should be assessed for adherence—ideally, at each visit—with a validated tool.4 Several reasons for patient nonadherence have been proposed. Provider-reported barriers to patient medication adherence include lack of knowledge about the disease state, fears about the medication, reliance on media or neighbors for information, present lack of symptoms, and challenges in implementing lifestyle changes.2 Medication nonadherence is not only a patient-mediated issue but also a provider issue. Provider barriers to supporting and increasing patient adherence include failure to perform a thorough review of medication information and unsatisfactory coaching and self-management skills.2
Patients are less likely to fill medication prescriptions post discharge when they live alone or take more than 11 medications. Medication nonadherence is more common in patients who are younger and have lower health literacy.6 Approximately 35% of Americans have basic or below-basic health literacy (i.e., have a kindergarten-6th grade reading level), meaning that their comprehension is limited to reading and following a set of directions from their healthcare provider or reading a medication brochure and identifying the purpose. Another 53% of Americans have intermediate health literacy (i.e., are at a 7th-8th grade reading level)—e.g., they can read a prescription label for a medication that should be taken twice daily and figure out on their own that the doses should be taken 12 hours apart.7 Pharmacists should be cognizant of their patients’ health literacy. All patient-education materials should be designed for a maximum reading level of 6th grade, and pharmacists should consider implementing health-literacy assessments in their practice so that patient education, counseling, and interventions can be targeted appropriately. Potential health-literacy assessments include the Rapid Estimate of Adult Literacy in Medicine and the Short Assessment of Health Literacy–English.7
Ostini and Kairuz found that the relationship between nonadherence and health literacy generally is not significant.8 Therefore, improving a patient’s health literacy is unlikely to improve medication adherence when the pharmacist focuses solely on improving knowledge. Self-efficacy enhancement is crucial to improving medication adherence in patients with poor health literacy.8 (Self-efficacy is the belief in one’s own abilities, particularly the ability to meet challenges and achieve goals.9) However, Mayo-Gamble and Mouton found that older African American patients and patients with limited health literacy are more likely to forget to take their medications and to take less medication than instructed.10 Therefore, although efforts to improve health literacy may not be the best use of pharmacists’ time in patient interactions, the pharmacist should assess the patient’s health literacy and provide education and written materials at a level appropriate for the patient. Medication adherence requires multimodal responses addressing social isolation, polypharmacy, and cost in addition to education designed to improve adherence.11
The literature has shown that inconvenience and forgetfulness are common causes of poor adherence.6,12 Pharmacists should work with patients in the use of tools (e.g., apps, timers, pillboxes) and medication dosing strategies (e.g., planning around work schedule) to improve medication adherence. Poor understanding and lack of medication knowledge are frequent barriers to patient adherence. Nelson and colleagues found that not seeing an immediate benefit and believing that brand medications work better than generics were common barriers to adherence.6 By using medication counseling and behavioral frameworks, pharmacists can address these barriers, thereby increasing adherence.
Facilitators of Adherence
Kuntz and colleagues conducted a qualitative review of patient-centered interventions for improving medication management and adherence.13 Educational interventions often resulted in better adherence and improved medication knowledge, and the most successful interventions used behavioral support or coaching to support patients.13 In studies, a major challenge is limited long-term impact; diminished adherence often occurs during follow-up, when the intervention has ceased.13 When chronic medications are initiated during hospital admission, discharge medication counseling has been associated with improved drug knowledge and medication adherence.11
For patients with diabetes, the use of different learning styles during counseling and education on dealing with side effects and using insulin properly have been identified as strategies for improving adherence.5 When learning about side effects, patients want to know the probability of experiencing these side effects and potential timelines for side-effect development and subsequent cessation. Patients are also interested in understanding the reason for a medication and the long-term benefits of therapy.5 Patients with chronic conditions prefer these patient-centered approaches, in which shared decision making incorporates their needs, preferences, and values.5
Patient Counseling Techniques for Adherence
Motivational Interviewing (MI): This method of patient interviewing is structured to promote behavioral changes via “a set of targeted communication skills to motivate patients to change their own behaviors in the interest of their health.”14 MI aims to facilitate collaboration between the patient and his or her provider while respecting the patient’s autonomy.14,15 For increasing adherence, MI is used to explore the reasons for barriers to medication intake.4 Compared with traditional counseling approaches, MI is supportive (rather than argumentative or coercive) and focuses on the patient’s intrinsic motivation.15 TABLE 1 describes the foundational components of MI.16

The acronym “RULE” was developed to structure the intervention according to four guiding principles: resist the righting reflex; understand the patient’s own motivations; listen with empathy; and empower the patient.14 Additional microskills that should be used in conjunction with MI are enhancing patient understanding of disease and risk susceptibility, agenda-setting, using open-ended questions, asking for patient permission before offering advice, employing change talk, and setting incremental goals rather than goals that require radical change.17,18
When a face-to-face MI approach was used in older adults (≥65 years) with a chronic disease who met the definition of polypharmacy, MI was shown to improve adherence by 7.6%.15 Although the improvement was small, it was significant compared with the traditional “advice” approach. MI has also been shown to lead to improvements in adherence and symptom reduction in adolescents and young adults, according to a systematic review by Schaefer and Kavookjian.17 A few studies concluded that MI resulted in improved quality of life among patients.17 MI has also been found to be a predictor of reduced readmissions when used in acute-care settings.19 To use MI to improve adherence, the pharmacist should collaborate with the patient to elicit change talk, set goals for taking medication consistently, and work to resolve barriers to adherence. During these activities, it is crucial for the pharmacist to demonstrate empathy and rapport while educating the patient that change takes time, particularly to successfully maintain this change in the long term.17,18 MI has been demonstrated to support behavior change and improve self-efficacy, thereby facilitating improvements in medication adherence.20
In practice, when assessing adherence to a therapy such as immunosuppressants in a post–kidney transplantation patient, instead of the pharmacist asking “You’ve been taking all of your pills in your antirejection therapy regimen, right?” a judgment-free, MI-centered question would be “How many pills in your antirejection therapy regimen would you say you missed this week?” This rephrasing establishes that nonadherence is normal and does not evoke preconceived judgments on the part of the pharmacist about the patient and his or her behavior. Patients are more likely to be receptive to change when they feel that they acting independently to make that change. To assist patients in setting medication-taking goals to improve adherence, the pharmacist should ask questions such as “Which strategy seems like something you could try to increase your statin taking?”17 Prior to giving advice, the pharmacist should ask the patient for permission; for example, “May I share with you some ideas that other patients with diabetes have tried to help them remember to take their basal insulin?”17
Three Prime Questions: This technique, developed by the Indian Health Service, uses three open-ended questions rather than lecture-style counseling to verify patients’ understanding of their prescription medications. Any gaps in understanding can be corrected before the pharmacist moves on to the next prime question and before the patient leaves the practice.21 TABLE 2 lists the three prime questions for new prescriptions. Following completion of these questions, final verification of patient understanding should be confirmed via the teach-back method (i.e., patient restates the information in his or her own words). To help patients feel more comfortable and lessen their embarrassment if they miss or misinterpret information, the pharmacist should always attribute the error to himself or herself. To verify patient understanding, the pharmacist should say, “Just to be sure I didn’t leave anything out, please tell me how you are going to take this medication.”21
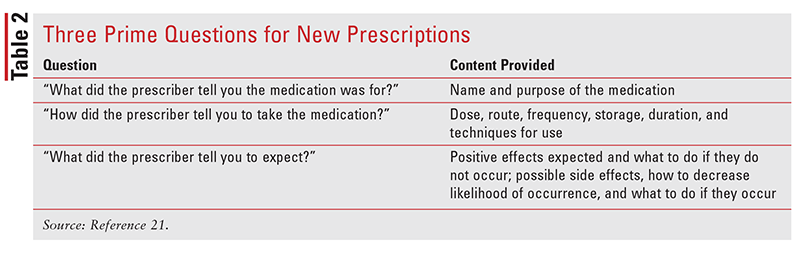
When patients are asked to verbalize their understanding through use of the three prime questions and teach-back, the covered information becomes part of their long-term or gist memory, and the information is retained longer compared with traditional or lecture-style counseling.22 Periodic assessment of the patient’s understanding of how to take long-term medications should be conducted, as misunderstanding could influence adherence. In asking the three prime questions about a refill medication, the pharmacist should use the show-and-tell method, in which he or she shows the patient the medication and the patient answers questions about its use.21 TABLE 3 lists the three prime questions modified for refill medications. Colvin and colleagues found that the three prime questions resulted in significant improvements in adherence to medications for diabetes, hypertension, and hyperlipidemia. Over a 6-month period, there was an average increase of 11% in the proportion of days covered, a common measure of adherence.12 Although the study was of short duration and did not assess whether adherence was maintained after the intervention ceased, it suggests that patient counseling using the three prime questions may be useful in improving patient adherence.

Auxiliary Labels: A prospective, randomized study by Pham and colleagues found that the use of auxiliary labels in combination with patient counseling for antibiotics had a high recall (77%) 5 to 7 days after receipt of medication information.22 The most commonly misunderstood information concerned dietary restrictions, which suggests that auxiliary labels for food are confusing to patients.23
Conclusion
Medication adherence is a complex issue that is affected by a number of different factors. Medication education and patient counseling have shown promise as a strategy for improving patient adherence. Behavioral interventions and counseling that actively engage the patient in his or her own healthcare should be used by pharmacists when attempting to improve patients’ medication knowledge and adherence.
REFERENCES
1. Ho PM, Bryson CL, Rumsfeld JS. Medication adherence: its importance in cardiovascular outcomes. Circulation. 2009;119:3028-3035.
2. Kvarnström K, Airaksinen M, Liira H. Barriers and facilitators to medication adherence: a qualitative study with general practitioners. BMJ Open. 2018;8:e015332.
3. Delamater AM. Improving patient adherence. Clin Diabetes. 2006;24:71-77.
4. Hugtenburg JG, Timmers L, Elders PJ, et al. Definitions, variants, and causes of nonadherence with medication: a challenge for tailored interventions. Patient Prefer Adherence. 2013;7:675-682.
5. Unni EJ, Van Wagoner E, Shiyanbola OO. Utilizing a 3S (strategies, source and setting) approach to understand the patients’ preferences when addressing medication non-adherence in patients with diabetes: a focus group study in a primary outpatient clinic. BMJ Open. 2019;9:e024789.
6. Nelson LA, Wallston KA, Kripalani S, et al. Assessing barriers to diabetes medication adherence using the Information-Motivation-Behavioral skills model. Diabetes Res Clin Pract. 2018;142:374-384.
7. Thomas S. Health literacy in the pharmacy. www.pharmacytimes.com/contributor/swana-thomas-pharmd-mph-candidate-2018/2016/08/health-literacy-in-the-pharmacy. Accessed March 28, 2019.
8. Ostini R, Kairuz T. Investigating the association between health literacy and non-adherence. Int J Clin Pharm. 2014;36:36-44.
9. Akhtar M. What is self-efficacy? Bandura’s 4 sources of efficacy beliefs. http://positivepsychology.org.uk/self-efficacy-definition-bandura-meaning. Accessed March 28, 2019.
10. Mayo-Gamble TL, Mouton C. Examining the association between health literacy and medication adherence among older adults. Health Commun. 2018;33:1124-1130.
11. Wooldridge K, Schnipper JL, Goggins K, et al. Refractory primary medication non-adherence: prevalence and predictors after pharmacist counseling at hospital discharge. J Hosp Med. 2016;11:48-51.
12. Colvin NN, Mospan CM, Buxton JA, et al. Using Indian Health Service (HIS) counseling techniques in an independent community pharmacy to improve adherence rates among patients with diabetes, hypertension, or hyperlipidemia. J Am Pharm Assoc. 2018;58:S59-S63.
13. Kuntz JL, Safford MM, Singh JA, et al. Patient-centered interventions to improve medication management and adherence: a qualitative review of research findings. Patient Educ Couns. 2014;97:310-326.
14. Zolnierek KB, DiMatteo MR. Physician communication and patient adherence to treatment: a meta-analysis. Med Care. 2009;47:826-834.
15. Moral RR, de Torres LA, Ortega LP, et al. Effectiveness of motivational interviewing to improve therapeutic adherence in patients over 65 years old with chronic diseases: a cluster randomized clinical trial in primary care. Patient Educ Couns. 2015;98:977-983.
16. WIC Learning Online. Principles of motivational interviewing. https://health.mo.gov/living/healthcondiseases/chronic/wisewoman/pdf/MIPrinciplesofMI.pdf. Accessed March 27, 2019.
17. Schaefer MR, Kavookjian J. The impact of motivational interviewing on adherence and symptom severity in adolescents and young adults with chronic illness: a systematic review. Patient Educ Couns. 2017;100:2190-2199.
18. Kavookjian J. Motivational interviewing. In: Richardson M, Chant C, Chessman KH, et al, eds. Pharmacotherapy Self‐Assessment Program. 7th ed. Lenexa, KS: American College of Clinical Pharmacy; 2011:1-18.
19. Hyrkas K, Wiggins M. A comparison of usual care, a patient-centred education intervention and motivational interviewing to improve medication adherence and readmissions of adults in an acute-care setting. J Nurs Manag. 2014;22:350-361.
20. Gesinde B, Harry S. The use of motivational interviewing in improving medication adherence for individuals with asthma: a systematic review. Perspect Public Health. 2018;138:329-335.
21. Lam N, Muravez SN, Boyce RW. A comparison of the Indian Health Service counseling technique with traditional, lecture-style counseling. J Am Pharm Assoc (2003). 2015;55:503-510.
22. Pham JA, Pierce W, Muhlbaier L. A randomized, controlled study of an educational intervention to improve recall of auxiliary medication labeling and adherence to antibiotics. SAGE Open Med. 2013;1:2050312113490420.
23. Brainerd CJ, Wright R, Reyna VF, Payne DG. Dual retrieval processes in free and associative recall. J Mem Lang. 2002;46:120-152.
To comment on this article, contact rdavidson@uspharmacist.com.






