US Pharm. 2020:45(5)HS2-HS-10.
ABSTRACT: Burnout is affecting the American workforce. While it is an important consideration for all workers, burnout is especially concerning in healthcare workers, such as pharmacists, because it can increase negative patient outcomes. Studies have shown that pharmacists have levels of reported burnout higher than many physicians. Data suggest both pharmacists and pharmacy residents are affected by burnout and identify potential causes and solutions. Pharmacist burnout can be caused by numerous factors, but common issues include time constraints and performance metrics. Professional organizations have created resources available to pharmacists and physicians in order to prevent burnout.
It is no secret that the American workforce is struggling with work-related stress and burnout. Published surveys have demonstrated that a substantial portion of full-time employees report feelings of burnout.1 This is concerning, as excess stress and burnout are associated with increases in negative physical outcomes such as cardiovascular diseases and obesity, as well as mental health impacts such as anxiety and depression.2 These quantifiable outcomes of burnout exemplify the importance of understanding this phenomenon. This renewed emphasis on work-related stress and burnout led to the most recent revision of the International Classification of Diseases (ICD-11) formally updating the definition of burnout to emphasize a more detailed and encompassing description as an occupational phenomenon (TABLE 1).3 This has led to renewed interest in evaluating, treating, and perhaps preventing work-related burnout.

Work-related stress and burnout are a concern for all workers, but those within the healthcare field are facing a particularly complex challenge. While burnout in traditional occupations focuses on the well-being of the individual worker, burnout in the healthcare setting must also consider the potential negative effects on patients’ healthcare outcomes. Research has identified multiple ways in which such effects can manifest, such as decreases in physician and nurse professionalism, which, in turn, may lead to decreases in patient satisfaction.4,5 However, more serious negative effects can include an increased frequency of medical errors and diminished patient safety.6,7 This is particularly concerning when considering that medical errors are the third leading cause of death in the United States behind only cardiovascular disease and cancers.8,9
Pharmacists are no exception to these concerns. More and more evidence supports the assertion that pharmacists are experiencing substantial work-related burnout and stress. Recent survey results reveal that 61.2% of pharmacists report experiencing a high level of burnout in practice, which is one of the highest rates among healthcare professionals. This rate is higher than that found in surgeons, oncologists, and emergency-medicine practitioners.10
Assessing Burnout
Accurately assessing burnout is complex. The Maslach Burnout Inventory (MBI) is generally considered the gold-standard assessment tool. Responses to the 22-item instrument are given based on frequency of a described feeling associated with burnout and related to a numerical score.11-13 Different versions of the MBI have been created to increase specificity for individual groups. Since the original instrument was intended to evaluate workers in healthcare and human services, it may be less efficient for evaluating workers in other fields. To solve this problem, other versions, such as the Educators Survey (MBI-ES) and General Survey (MBI-GS), were developed to evaluate educators and a broader number of occupations, respectively. Once these new variations were created, the original MBI tool became known as the Human Services Survey (MBI-HSS), which is now the preferred tool for analyzing healthcare workers.11-13 The MBI-HSS survey measures emotional exhaustion, personal accomplishment, and depolarization to identify not only burnout, but also the specific cause of the subject’s stress. By identifying the context of an individual’s burnout, efforts to address and correct these feelings can be considered.
Emotional exhaustion is measured with nine statements, such as “I feel emotionally drained from work” and “I feel used up at the end of the workdays.” Subjects scoring between 0-18 points on this section are thought to have low levels of emotional exhaustion, whereas subjects scoring 27 or more points are thought to have high levels.
For personal accomplishment, the survey uses eight statements, such as “I can easily understand how my recipients feel about things,” and “I deal very effectively with the problems of my recipients.” Scores of 40 or more points indicate a high level of personal accomplishment, or a low likelihood of burnout being impacted by a lack of personal accomplishments. Scores of 0 to 33 points indicate a low level of personal accomplishments, which suggests that a subject’s feeling of burnout could be due to a lack of personal accomplishment.
Lastly, depersonalization is measured with five statements, such as “I’ve become more callous toward people since I took this job” and “I worry that this job is hardening me emotionally.” Subjects scoring between 0 and 5 points have low levels of depersonalization, whereas those scoring 10 or more points have high levels of depersonalization.
Other scales have been developed to examine similar factors. For example, the Perceived Stress Scale (PSS-10) is also used in research. The survey includes 10 questions, such as “In the last month, how often have you been upset because of something that happened unexpectedly?” and “In the last month, how often have you felt nervous or stressed?” Scores from 0 to 13 indicate low levels of stress, and scores from 27 to 40 suggest the subject has high stress levels.14,15
While these scales have been widely used to assess pharmacist burnout, there is no scale that is specific to the pharmacist work environment. Therefore, when individual pharmacists are assessed using these scales, there may be limited consistency on the interpretation and application of the questions. This may cause variations in the level of burnout reported when employing these assessments. A scale developed to be more relatable to the work environment of pharmacists would likely provide a more accurate view of burnout in pharmacists and pharmacy residents.10
Causes of Burnout
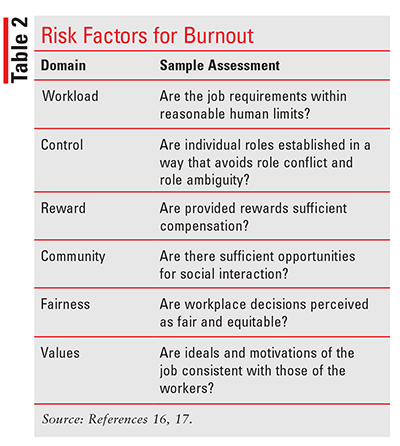
Given the individual-specific nature and expansive collection of associated symptoms of burnout, its causes can be difficult to isolate. A 2008 article by Maslach and Leiter compiled evidence from previously established findings and identified a set of predictive risk factors for workers regardless of profession.16 These risk factors were divided into six domains (TABLE 2) providing general areas of concern for typical workers.16,17 More healthcare-specific risk factors have also been published (TABLE 3).18,19 Many of these closely relate to the generalized domains identified by Maslach.
Burnout in Pharmacists
Among hospital pharmacists, the rates of reported burnout are similar across all practice settings and areas. Most pharmacists who reported significant levels of burnout were unmarried or not in a stable relationship, had no children, and worked more than 40 hours per week.10 Having too many nonclinical duties was the number-one reported cause of burnout in hospital pharmacists, with feelings of uncertainty surrounding healthcare reform and inadequate time for teaching also being highly reported.10
For community pharmacists, reported burnout rates mirror those in hospital settings; however, those in community pharmacies often report differing causes for their feelings of burnout. Time constraints, performance metrics, and lack of control are typically associated with burnout in community pharmacists.18,19 Similar to hospital pharmacists, those who are single, without children, and work longer hours are most at risk.10
Burnout in Pharmacy Residents
The requirements of postgraduate pharmacy residency programs may create situations with many associated risk factors for burnout. Although most research on postgraduate residents focuses on medical residents, there is evidence that supports the risk of burnout in pharmacy residents as well. Data on medical residents largely outlines the stressors associated with the resident experience, including time and deadline pressure, long working hours, and difficult financial situations. These factors are all strongly correlated with the stress, burnout, and depression found in residents.15,20-21 Published studies evaluating pharmacy residents specifically have found similar results.
A 2018 study by Zinurova and DeHart evaluated the pharmacy-resident experience with a focus on stress and individual stressors during the program.15 The researchers evaluated 505 postgraduate year 1 (PGY1) residents with a Web-based survey that included questions regarding background demographics, the PSS-10, and the number of hours spent weekly either working or sleeping. They found an average PSS-10 score of 17.6, indicating a moderate level of perceived stress. Residents working more than 60 hours per week were found to have the most elevated PSS-10 scores. These findings are consistent with studies evaluating medical residents, emphasizing the similar situations pharmacy residents find themselves in when compared with the more thoroughly evaluated population.15,20
Residents were also asked what techniques they used to cope with the associated stress and burnout. Some of the most common responses included spending time with family/friends, staying optimistic, and engaging in enjoyable activities. The authors concluded that most subjects reported using generally positive techniques as coping mechanisms, offering further insight into consideration for burnout prevention.15
A similar 2017 study by Le and Young used a similar approach.21 Web-based surveys were distributed to practicing pharmacy residents, including both PGY1 and PGY2 pharmacists. This survey evaluated background demographics as well as the PSS-10. Researchers found an average PSS-10 score of 19 and also identified the correlation between residents working more than 60 hours a week and higher levels of stress, depression, hostility, and dysphoria. Interestingly, PGY2 residents had higher reported levels of hostility than PGY1 residents, while other effects such as anxiety, dysphoria, and depression were not significantly different.21
Preventing Burnout
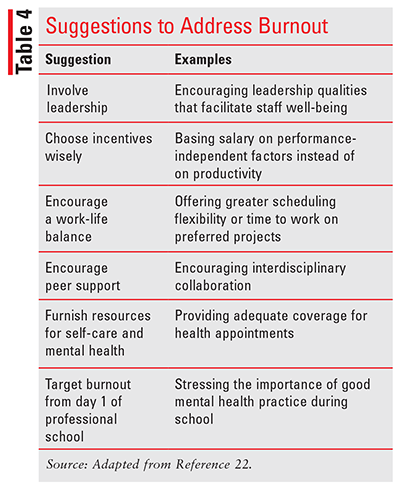
Preventing burnout is complicated. While factors causing burnout in pharmacists can be unique to this career, more pervasive risk factors present in similar healthcare professions suggest an encompassing problem. For this reason, expanding the search for answers to similar fields may be appropriate.17,18 For instance, a 2018 narrative review by Reith evaluated burnout in a broad array of healthcare professionals. He evaluated examples of reported strategies for burnout prevention in available literature and identified six suggestions for addressing burnout (TABLE 4).22 These suggestions outline various reported methods of burnout prevention from compiled literature and offer a framework from which to formulate ideas and considerations.
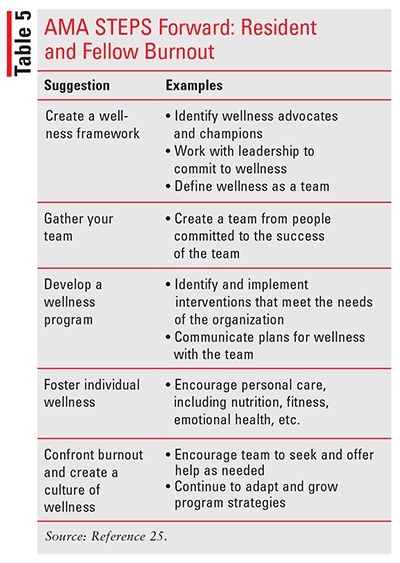
Health organizations have also taken actions to combat burnout. For example, the American Medical Association (AMA) created a dedicated program to maintain the well-being of its physicians.23 Using findings from the AMA-RAND study, a 2013 evaluation of physician satisfaction and its effects on patient care, they created a resource designed to empower teams to identify and attain goals to thrive in the changing healthcare environment.24 This resource is called the AMA STEPS Forward program, a module-based, interactive, practice-transformation series. Of the 50 currently available modules, three cover topics on or closely related to burnout and stress: Resident and Fellow Burnout (TABLE 5), Improving Physician Resiliency, and Preventing Physician Burnout.24,25 Each module provides useful insights and recommendations for creating a plan to prevent burnout and empower physicians. The material in these modules is largely transferrable to pharmacists, as it focuses on identifying and improving many associated risk factors for pharmacist burnout.
Pharmacist-specific groups are also working to prevent burnout. In 2017, the American Society of Health-System Pharmacists (ASHP) helped sponsor the National Academy of Medicine Action Collaborative on Clinician Well-being and Resilience. The three goals of this multidisciplinary network are to 1) raise the visibility of clinician anxiety, burnout, depression, stress, and suicide; 2) improve baseline understanding of challenges to clinician well-being; and 3) advance evidence-based, multidisciplinary solutions to improve patient care by caring for the caregiver. The ASHP Well-being & You program offers multiple resources for pharmacists in order to prevent burnout, including community connections, well-being tools, and webinar series.19
More novel data may also provide some insight into ways of decreasing burnout. One such example, a 2019 article by Funk and colleagues, may offer some interesting insight. The researchers created an interview protocol to evaluate the effect of pharmacist-led comprehensive medication management on primary care providers’ (PCP) clinical practice and overall work life, including burnout. Their results demonstrated improvement in several aspects of the PCP work-related stress. Specifically, improvements including decreased workload, decreased mental exhaustion, and improved achievement of quality measures were identified.26 While this did not assess stress and burnout effects in pharmacists, it did demonstrate an accumulated value of interdisciplinary teamwork, which improved both observable patient outcomes and work-life effects associated with burnout in physicians. This may be a positive sign that the continued trend of pharmacists integrating into the multidisciplinary team can offer benefits to all team members.
Overcoming Burnout
Many of the methods for overcoming burnout once it has occurred are similar to the prevention strategies. Focusing on development of an improved work-life balance can be critical for those who typically work more than 40 hours per week and are experiencing burnout.22 Ensuring individual wellness needs are also being met through fitness, balanced diet, and relaxation strategies can also improve burnout symptoms once they have occurred.25 Additionally, building support systems through family, friends, and coworkers can boost morale and reduce feelings of burnout.12
In some cases, those experiencing burnout can develop more severe symptoms such as anxiety, depression, or other mental health conditions.12,27 In these cases, mental health support should be sought out as early as possible through counseling or therapy. Individuals with mental health symptoms should be monitored closely, and personalized treatment should be sought if needed.27
Conclusion
Stress and burnout can affect pharmacists in all practice settings and are often associated with issues surrounding time constraints and performance metrics. Symptoms of burnout can include increases in negative physical outcomes such as cardiovascular diseases and obesity as well as mental health impacts such as anxiety and depression. Prevention strategies like focusing on work-life balance, peer support, and self-care are effective in reducing rates of burnout seen in pharmacists. In individuals who experience more severe mental health issues, such as anxiety or depression, mental health support through counseling or therapy is needed.
REFERENCES
1. Pazzanese C. The high price of workplace stress. July 2016. https://news.harvard.edu/gazette/story/2016/07/the-high-price-of-workplace-stress/. Accessed April 17, 2020.
2. Salvagioni DAJ, Melanda FN, Mesas AE, et al. Physical, psychological and occupational consequences of job burnout: a systematic review of prospective studies. PLoS One. 2017;12(10):e0185781.
3. World Health Organization. Burn-out an “occupational phenomenon”: International Classification of Diseases. May 28, 2019. www.who.int/mental_health/evidence/burn-out/en/. Accessed February 20, 2020.
4. Panagioti M, Geraghty K, Johnson J, et al. Association between physician burnout and patient safety, professionalism, and patient satisfaction; a systematic review and meta-analysis. JAMA Intern Med. 2018;178(10):1317-1331.
5. Vahey DC, Aiken LH, Sloane DM, et al. Nurse burnout and patient satisfaction. Med Care. 2004;42(2 Suppl):1157-1166.
6. Tawfik DS, Profit J, Morganthaler TI et al. Physician burnout, well-being, and work unit safety grades in relationship to reported medical errors. Mayo Clin Proc. 2018;93(11):1571-1580.
7. Motluk A. Do doctors experiencing burnout make more errors? CMAJ. 2018;190(40):E1216-E1217.
8. Garcia CL, Abreu LC, Ramos JLS, et al. Influence of burnout on patient safety: systemic review and meta-analysis. Medicina (Kaunas). 2019;5(9).E553.
9. Makary AM, Daniel M. Medical error—the third leading cause of death in the US. BMJ 2016;353:2139.
10. Jones GM, Roe NA, Louden L, Tubbs CR. Factors associated with burnout among US hospital clinical pharmacy practitioners: results of a nationwide pilot survey. Hosp Pharm. 2017;52(11):742-751.
11. Bridgeman PJ, Bridgeman MB, Barone J. Burnout syndrome among healthcare professionals. Am J Health Syst Pharm. 2018;75(3):147-152.
12. Maslach C, Jackson SE, Leiter MP. Maslach Burnout Inventory Manual. 3rd ed. Palo Alto, CA: Consulting Psychologists Press; 1996:191-218.
13. Jones GM, Roe NA, Loudon L, Tubbs CR. Factors associated with burnout among US hospital clinical pharmacy practitioners: results of a nationwide pilot survey. Hosp Pharm. 2017. 52(11)742-751.
14. Cohen S, Williamson S. (1988). Perceived stress in a probability sample of the United States. In S. Spacapan & S. Oskamp, eds., The Claremont Symposium on Applied Social Psychology. The Social Psychology of Health. Newberry Park, CA: Sage Publications, Inc. 1988:31-67.
15. Zinurova E, DeHart R. perceived stress, stressors, and coping mechanisms among PGY1 pharmacy residents. Am J Pharm Educ. 2018;82(7):6574.
16. Maslach C, Leiter MP. Early predictors of job burnout and engagement. J Appl Psychol. 2008;93(3):498-512.
17. Bridgeman P, Bridgeman MB, Barone J. Burnout syndrome among healthcare professionals. Am J Health Syst Pharm. 2016;75:(3): 147-150.
18. Lyndon A. Burnout among health professionals and its effect on patient safety. Agency for Healthcare Research and Quality. January 1, 2015. https://psnet.ahrq.gov/perspective/burnout-among-health-professionals-and-its-effect-patient-safety. Accessed April 21, 2020.
19. Bridgeman P. Bridgeman M, Pop M, Scott B. Putting out the fire: beating burnout in pharmacy and healthcare. ASHP Well-Being and Resilience series. Webinar. December 2018.
20. Ishak WW, Lederer S, Mandilli C, et al. Burnout during residency training: a literature review. J Grad Med Educ. 2009; (2):236-242.
21. Le HM, Young SD. Evaluation of stress experienced by pharmacy residents. Am J Health Syst Pharm. 2017;74(8):599-604.
22. Reith TP. Burnout in United States healthcare professionals: a narrative review. Cureus. 2018;10(12) e3681.
23. American Medical Association. AMA launches STEPS Forward to address physician burnout [Press release]. June 8, 2015. www.ama-assn.org/press-center/press-releases/ama-launches-steps-forward-address-physician-burnout. Accessed April 21, 2010.
24. Friedberg MW, Chen PG, Van Busun KR et al. Factors affecting physician professional satisfaction and their implications for patient care, health systems, and health policy. Rand Health Q. 2014;3(4):1.
25. Okanlawon T. Resident and fellow burnout. AMA STEPS Forward. Continuing Medical Education Course. 2015.
26. Funk KA, Pestka DL, Roth McClurg MT, et al. Primary care providers believe that comprehensive medication management improves their work-life. J Am Board Fam Med. 2019;32(4):462-473.
27. Salvagioni DAJ, Melanda FN, Mesas AE, et al. Physical, psychological, and occupational consequences of job burnout: a systematic eview of prospective studies. PLoS One. 2017;12(10):e0185781.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article contact rdavidson@uspharmacist.com.







