US Pharm. 2007:32(7):38-47.
One
in 15 Americans suffers from asthma, and every day in the United States
40,000 people miss work or school and 11 people die from the disease.1
Although there is no cure, asthma can be managed with appropriate treatment
and these daily occurrences can be avoided. With hundreds of prescriptions
filled at a given pharmacy each day, the pharmacist is in a unique position to
improve the quality of life (QOL) in those with asthma. This article will
describe the pathophysiology of asthma and why it plays an important role in
medication selection; provide educational tips that will improve the care of
asthmatic patients; and detail medications and their evidence.
Pathophysiology
Understanding of
the underlying pathophysiology of asthma will allow the pharmacist to better
evaluate drug therapy for appropriateness. Current drug therapies target the
two basic components of asthma: airway inflammation and bronchoconstriction.
Chronic inflammation plays a key role in the changes that occur in patients.
2
Airway inflammation can be
classified as either acute or chronic.2,3 Acute inflammation can be
further characterized as either early-phase or late-phase reactions. In the
early-phase reaction, immunoglobulin (Ig) E antigens initiate the activation
of mast cells and macrophages.2-4 Activated mast cells release
prostaglandins, leukotrienes, and other proinflammatory mediators. These
mediators cause airway smooth muscle constriction and mucous secretion,
ultimately decreasing the airway lumen. In the late-phase reaction, T
lymphocytes, eosinophils, basophils, neutrophils, and macrophages are
activated.3 Eosinophils enhance the inflammatory process further by
releasing proteins, leukotrienes, and cytokines, which damage airway
epithelial cells and lead to hyperreactivity and bronchospasm.5 The
proinflammatory cells and mediators involved in acute inflammation also
contribute to chronic inflammation. Over time, activation of the airway immune
system, epithelial cell destruction, and thickening of the basement membrane
cause airway remodeling, resulting in an increase in airflow resistance.3
Mucous secretion and subsequent formation of mucous plugs further complicate
airflow-resistance problems. Inflammation also causes an increase in the
sensitivity of the bronchioles to stimuli, or triggers, causing
bronchoconstriction.
Patient Education
Patient education
is essential in the long-term success of asthma management. Education provided
by pharmacists, nurses, and physicians has proved effective. The patient plays
a vital role in this process and should be considered a partner. Pharmacists
should offer counseling on the following to all patients with asthma:
Basic facts about asthma:
The difference between normal lung function and that of a patient with
asthma, especially during an attack.
Trigger management:
Identification and management of triggers of asthma attacks.
Skills:
Appropriate inhaler technique and use of a spacer device with metered-dose
inhalers (MDIs). Peak flow monitors are an easy way to monitor long-term
control and detect early deterioration. Written asthma action plans can
supplement peak flow use.
Role of controller
medications:
Controller medications target the underlying cause of asthma and prevent
attacks from occurring. Compliance with these medications should be
emphasized, even if the patient has not had an attack in some time.
Role of rescue
medications: Rescue
medications relax muscles around the airway, helping reverse an acute attack.
They should not be used on a scheduled basis, and frequent use may be a sign
of worsening.
In combination with
medications, limiting exposure to triggers plays a vital role in controlling
asthma symptoms and decreasing the number of attacks.2 Triggers
include allergens, irritants, infections, and medications.6-8 The
pharmacist can play a role in asthma control by providing patients with tips
and techniques for minimizing contact with triggers.
Strategies for reducing
exposure to animal dander involve either the removal of the pet from the house
or minimizing contact by not allowing the pet in the patient's bedroom. Weekly
washings can also help to decrease the accumulation of dander. Dust mites are
found in bedding, upholstered furniture, carpets, clothes, and soft toys.
Encasing bedding in allergen-impermeable covers, along with regular washing in
hot water (>130F), will help to control mites.2,9 Soft
toys should be washed regularly in hot water, and there should be a limited
number of toys available to the child to sleep with. Dust mites are also
prevalent in areas of high humidity, and reducing the indoor humidity with a
dehumidifier to below 50% can reduce a patient's exposure.2 Simple
household hygiene may also reduce asthma attacks. However, there is little
evidence to suggest extensive measures, such as high-efficiency particulate
air filters, are of any benefit.2 Steps to minimize exposure to
outdoor allergens include keeping windows closed, using air conditioners, and
staying indoors during the afternoon when the pollen and spore levels peak.
2
Exposure to irritants should
be assessed. Examples of common irritants can include tobacco smoke, chemical
gases or sprays, fumes, and any chemical with a strong odor.7
Patients and parents of children with asthma who smoke should be encouraged to
stop. Pharmacists who notice increased use of rescue medications can offer
counseling on these adjunctive measures to aid in improving control of asthma
symptoms and decreasing attacks.
Allergic rhinitis is a common
trigger, and the use of intranasal corticosteroids or
antihistamine/decongestant combination medications is recommended to relieve
symptoms. Asthma attacks can be induced by respiratory viral infections.
Annual influenza vaccinations should therefore be offered to all patients.
Pharmacists should review all
medications to avoid drug-induced asthma attacks. Severe and even fatal
attacks have been associated with the use of aspirin or nonsteroidal
anti-inflammatory drugs.8 All patients with asthma should be
counseled on the potential risk of attacks with these medications and
instructed to ask their pharmacist or physician before starting any OTC
products that contain these agents. Safer alternatives such as acetaminophen
or salsalate may be recommended. Nonselective beta-blockers (propranolol,
nadolol, and timolol) are not recommended for asthma patients. Cardioselective
beta-blockers (atenolol, bisoprolol, and metoprolol) can be used if patients
require this medication class to control other conditions.
Peak Flow Monitoring and
Asthma Action Plans
A peak flow meter
is a simple and inexpensive device that can aid in assessing a patient's
current asthma control.2 A peak flow meter measures the peak
expiratory flow (PEF) rate. Peak flow monitoring is recommended for patients
with moderate to severe persistent asthma. Daily peak flow measurements can
serve as a tool for the physician and the patient to judge responses to
controller medications and aid in early recognition of worsening asthma.
Pharmacists can provide peak flow education to patients with asthma.10
While relatively simple to use, patients will require training on the
appropriate technique and how to monitor and record their peak flow readings.
Education and evaluation of patient technique should be offered during each
pharmacy consultation. Peak flow meters are often used in conjunction with
action plans.
Self-management through the
use of written action plans has been found to decrease emergency department
visits and hospitalization.2,11 Action plans are based on personal
best peak flow (PBPF) measurements and divided into green (>80% PBPF), yellow
(50%-80% PBPF), and red (<50% PBPF) zones. Instructions are based on which
zone the patient is currently in. Patients in the green zone will continue
their controller medications, and those in the yellow zone are instructed to
make adjustments to their regimen with the goal to return to their green zone.
Patients falling in the red zone may require immediate attention by medical
professionals. Counseling on how to use written action plans provides
pharmacists with another opportunity to impact patient care.
Symptoms and Classification
Patients may
experience long periods of time with little or no symptoms, followed by
episodes of acute attacks. Common symptoms include shortness of breath, chest
tightness, wheezing, or coughing, particularly at night. Severe asthma
episodes may involve audible wheezing, rapid respirations or heart rate, and
difficulty speaking. Acute episodes may last from several minutes to hours or
even days and resolve spontaneously or with treatment.
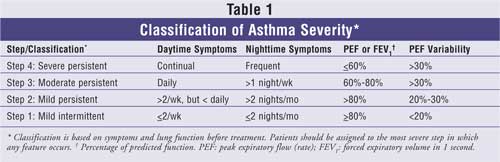
Early and accurate
classification of asthma severity ensures appropriate use of medications
because drug therapy recommendations are based upon severity. The National
Asthma Education and Prevention Program (NAEPP) classifies patients as having
either mild, intermittent, or persistent asthma (TABLE 1).12
†Persistent asthma is further classified as mild, moderate, or severe.
Exercise-induced asthma is a form of intermittent asthma, and patients can be
managed by using a rescue medication such as albuterol 15 minutes before
physical activity. Patients with persistent asthma are classified by frequency
of their day and nighttime symptoms, PEF rates, forced expiratory volume in
one second (FEV1), and daily PEF variability. Over time, patients
can move up or down in severity level based on control.

Therapy Review
The NAEPP
recommends using a stepwise approach for the management of asthma. Based on
the classification, a treatment regimen is recommended (TABLE 2).12
Gaining control quickly is important in order to treat the patient
effectively. Once sustained control is achieved, a gradual, or step-down,
reduction in therapy is recommended. The step-up approach is required when a
patient is experiencing worsening symptoms requiring more medication. Patients
should be evaluated every one to six months to determine if therapy needs to
be stepped up or down. In some cases, clinical judgment is used to meet
individual needs.
Short-acting beta2
-agonists (SABAs), or rescue inhalers, provide quick relief for acute attacks
and are recommended in all patients despite severity classification. Long-term
controllers are dosed daily in those patients with persistent asthma to
prevent attacks. Counseling patients on compliance with long-term controllers
will allow them to receive the maximum benefit from their medications.

Mild Intermittent Asthma:
Patients do not require daily medications.12 A rescue inhaler is
recommended for symptom control. If the patient is experiencing an increase in
frequency and/or severity of symptoms, controller medications may be
necessary. Monitoring rescue inhaler use is an effective technique to
determine control. A patient's use of two or more doses per week or more than
one canister per month is a sign of worsening asthma. Severe exacerbations can
be treated with a short burst of systemic corticosteroids.
Mild Persistent Asthma:
The preferred treatment for mild persistent asthma is a low-dose inhaled
cortico-steroid (ICS).12 Most patients can be controlled using an
ICS alone. Other treatment options for this classification included
leukotriene modifiers, mast cell stabilizers, or sustained-release
theophylline. Inhaled corticosteroids have been proven to be superior to the
leukotriene modifiers.13 Alternative therapies are reserved for
those who cannot use or tolerate inhaled corticosteroids. Inhaled
corticosteroid dosing ranges are presented in TABLE 3.
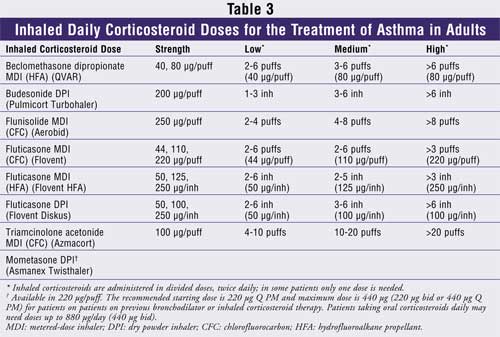
Moderate Persistent
Asthma: Low- to
medium-dose ICS plus a long-acting beta2-agonist (LABA) is the
preferred treatment. Alternative options include a medium-dose ICS or the use
of a low- to medium-dose ICS plus a leukotriene modifier. In patients with
recurring severe exacerbations, it is recommended to use a medium-dose ICS in
combination with a LABA, leukotriene modifier, or theophylline. Several
ICS/LABA combination products are available (TABLE 4).14-16
Inhaled corticosteroids used in combination with LABAs are superior to
monotherapy with either agent, higher doses of an ICS alone, or the addition
of a leukotriene modifier to an ICS.17-19
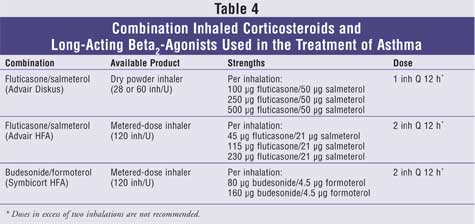
Severe Persistent Asthma:
A high-dose inhaled cortico-steroid along with a LABA is the preferred
treatment regimen.12 Systemic corticosteroids may also be used for
long-term control. Patients should receive the lowest strength possible to
maintain control, and every effort should be made to decrease the
corticosteroid to reduce the risk of side effects seen with chronic use.
Short-Acting Beta2
-Agonists:
Short-acting beta2-agonists are the most effective medications for
the treatment of acute symptoms and exercise-induced asthma. They provide
rapid bronchodilation via relaxation of the bronchial smooth muscle, which
occurs within minutes of inhalation. Albuterol is the most commonly prescribed
SABA and is available in nebulized and MDI formulations. Other SABAs include
terbutaline, pirbuterol, and levalbuterol. Common side effects include
tachycardia, palpitations, and nervousness.20 SABAs are not
adequate for long-term control and are only indicated for short-term relief.
OTC epinephrine inhalers (Bronkaid and Primatene Mist) should be avoided.
Chlorofluorocarbon (CFC)-containing albuterol MDIs will not be available after
2008. Chlorofluorocarbons are used as a propellant for MDIs and have also been
shown to deplete the ozone. Therefore, the U.S. Food and Drug Administration
has mandated that production of CFC-containing products stop after 2008.
Metered-dose inhalers have been reformulated using hydrofluoroalkane (HFA) as
a propellant that will not cause deleterious effects to the environment.
Proventil HFA, Ventolin HFA, and ProAir HFA are CFC-free albuterol products.
Inhaled Corticosteroids:
Inhaled corticosteroids are the treatment of choice for persistent
asthma.12 When compared to all other classes of medications, ICSs
were proven to be more effective for improving symptoms and lung function.
21-24 The mechanism by which ICSs control asthma symptoms is the
production of a direct local anti-inflammatory effect on the lung mucosa.
These agents should not be used for acute exacerbations. Local side effects
include thrush and throat irritation, which is usually seen with high-dose
ICSs. Advising the patient to rinse the mouth with water after each dose will
reduce the incidence of thrush. Systemic adverse effects can be seen with high
doses of ICSs.25
Long-Acting
Bronchodilators:
NAEPP guidelines recommend adding a LABA to an ICS for the treatment of
moderate-to-severe asthma. The addition of a LABA to ICS reduces symptoms and
attacks when compared to similar ICS doses alone, but did not reduce the risk
of attacks when compared to a high-dose ICS alone.26,27 Clinical
study results linking LABA use to an increase in severe and life-threatening
attacks, as well as asthma-related deaths (one death per 1,000 patients using
LABAs for one year), prompted the FDA to issue a black box warning.28-30
Simply stated, LABAs should not be used as the first medication to treat
asthma and should never be used alone or for quick relief. Patients should not
stop their LABA without consulting their physician. Based on this, it may be
appropriate to maximize ICS doses and only add LABAs when symptoms remain.
Leukotriene Modifiers:
Montelukast (Singulair) and zafirlukast (Accolate) inhibit leukotriene
receptors, resulting in the reduction of leukotriene-induced
bronchoconstriction.31 They are considered an alternative to ICSs
for mild persistent asthma.12 Further evidence has proven that
switching from an ICS to a leukotriene modifier was associated with an
increase in exacerbations and asthma-related hospitalizations.32
The leukotriene modifiers are also beneficial in patients with concomitant
allergic rhinitis. Common side effects include dizziness, fatigue, stomach
upset, elevated liver enzymes, cough, and nasal congestion.31
Zileuton (Zyflo), a 5-lipoxygenase inhibitor, is not routinely prescribed due
to a cumbersome dosing schedule of four times a day and the potential for
liver function test elevations.
Mast Cell Stabilizers:
Cromolyn sodium and nedocromil sodium inhibit bronchoconstriction in response
to an allergen challenge. Both medications are considered to be nontoxic and
are used in childhood asthma, and there is no apparent difference in efficacy
between the two drugs. These agents are not used as monotherapy and should be
reserved as an adjunct to other controller medications.
Methyxanthines:
Theophylline use has declined since the introduction of newer, more effective
agents. The risks of severe toxicity, numerous drug interactions, and
questionable efficacy when compared to ICSs have limited their utilization.
Theophylline produces bronchodilation through phosphodiesterase inhibition.
Sustained-release theophylline is considered an adjuvant therapy to ICS for
nocturnal symptoms. Theophylline is not recommended for long-term use because
it has a narrow therapeutic index and serum levels need to be monitored
frequently. Symptoms of toxicity include nausea, vomiting, tachycardia,
jitteriness, insomnia, arrhythmias, and seizures.33
Monoclonal Antibodies:
Omalizumab (Xolair) is the first human recombinant anti-IgE antibody
approved for the treatment of allergic asthma with elevated IgE levels that
are not well controlled with high doses of ICSs. The dose is determined by the
patient's baseline serum IgE level and total body weight. It is administered
subcutaneously every two to four weeks in conjunction with ICS therapy.34
This therapeutic option is very costly.
Oral Corticosteroids:
Systemic corticosteroids may be used for quick relief of a severe
attack or daily for those with severe, difficult-to-control asthma.12
Daily use for long periods of time is not recommended due to the potential
for adrenal suppression. Low doses for three to 10 days are recommended for
severe exacerbations. Doses of prednisone 60 mg used for up to 10 days do not
require tapering.12,35 Side effects from oral corticosteroid use
include insomnia, nervousness, increased appetite, indigestion, arthralgia,
and hyperglycemia.36
Conclusions/Pharmacist's
Role
There are more than
4,000 asthma-related deaths per year, many of which are preventable.1
As one of the most conspicuous health care system practitioners, pharmacists
are in the opportune position to impact QOL in their patients with asthma.
Reviewing the underlying causes of asthma will help us to teach controller and
rescue medications better. Several opportunities exist for the pharmacist to
participate in the care of the asthmatic patient,37 including
certification as an asthma educator.
References
1. Asthma and
Allergy Foundation of America. (n.d.). Asthma facts and figures. AAFA home
page. Available at: http://www.aafa.org/display.cfm?id=8&sub=42. Accessed
April 1, 2007.
2. National Institutes
of Health, National Heart, Lung, and Blood Institute. National Asthma
Education and Prevention Program, Expert Panel Report 2. Guidelines for the
Diagnosis and Management of Asthma. NIH Publication No. 97-4051. Bethesda,
Md: US Department of Health and Human Services; 1997.
3. Bousquet J, Jeffery
PK, et al. Asthma--from bronchoconstriction to airways inflammation and
remodeling. Am J Respir Crit Care Med. 2000;161:1720-1745.
4. Busse WW, Lemanske
RF. Advances in immunology: asthma. N Engl J Med. 2001;344:350-362.
5. Kay AB. Advances in
immunology: allergy and allergic diseases. N Engl J Med.
2001;344:30-37.
6. Von Mutius E. The
environmental predictors of allergic disease. J Allergy Clin Immunol.
2000;105:9-19.
7. Malo J, Chan-Yeung
M. Occupational asthma. J Allergy Clin Immunol. 2001;108:317-328.
8. Szczeklik A,
Stevenson DD. Aspirin-induced asthma: advances in pathogenesis and management.
J Allergy Clin Immunol. 1999;104:5-13.
9. National Institutes
of Health, National Heart, Lung, and Blood Institute. Global Initiative for
Asthma (GINA). Global Strategy for Asthma Management and Prevention Revised
(2002). NHLBI/WHO Workshop Report. NIH publication No. 02-3659. Bethesda,
Md: US Department of Health and Human Services; 2002.
10. NHLBI, The Role
of the Pharmacist in Improving Asthma. NIH Publication No. 95-3280.
Bethesda, Md: US Department of Health and Human Services; 1995.
11. Gibson PG, Powell
H, Coughlan J, et al. Self-management education and regular practitioner
review for adults with asthma. Cochrane Database of Systematic Reviews.
2002, Issue 3. Art. No.: CD001117. DOI: 10.1002/14651858.CD001117.
12. National Institutes
of Health, National Heart, Lung, and Blood Institute. National Asthma
Education and Prevention Program, Expert Panel Report: guidelines for the
diagnosis and management of asthma update on selected topics 2002. J
Allergy Clin Immunol. 2002;110:S142-S219.
13. Ducharme FM, Di
Salvio F. Anti-leukotriene agents compared to inhaled corticosteroids in the
management of recurrent and/or chronic asthma in adults and children.
Cochrane Database of Systematic Reviews. 2004, Issue 1. Art. No. CD002314.
DOI: 10.1002/14651858.CD002314.pub2.
14. Symbicort [package
insert]. Wilmington, Del: AstraZeneca; July 2006.
15. Advair [package
insert]. Research Triangle Park, NC: GlaxoSmithKline; March 2006.
16. Advair HFA [package
insert]. Research Triangle Park, NC: GlaxoSmithKline; June 2006.
17. Stoloff S,
Poinsett-Holmes K, Dorinsky PM. Combination therapy with inhaled long-acting
beta2-agonists and inhaled corticosteroids: a paradigm shift in
asthma management. Pharmacotherapy. 2002;22:212-226.
18. Heyneman CA, Crafts
R, et al. Fluticasone versus salmeterol/low-dose fluticasone for long-term
asthma control. Ann Pharmacother. 2002:212-226.
19. Ducharme FM,
Lasserson TJ, Cates CJ. Long-acting beta2-agonists versus anti-leukotrienes as
add-on therapy to inhaled corticosteroids for chronic asthma. Cochrane
Database of Systematic Reviews. 2006, Issue 4. Art. No. CD003137. DOI:
20.1002/14651858.CD003137.pub3.
20. Albuterol sulfate.
In: Klasco RK, ed. DRUGDEX System (electronic version). Thomson
Micromedex, Greenwood Village, Colo. Available at: www.thomsonhc.com. Accessed
April 30, 2007.
21. Ducharme FM.
Inhaled glucocorticoids versus leukotriene receptor antagonists as single
agent asthma treatment: systematic review of current evidence. BMJ.
2003;326:621-623.
22. Meltzer EO, Lockey
RF, et al. Efficacy and safety of low-dose fluticasone propionate compared
with montelukast for maintenance treatment for persistent asthma. Mayo Clin
Proc. 2002;77:437-445.
23. Brabson JH,
Clifford D, et al. Efficacy and safety of low-dose fluticasone propionate
compared with zafirlukast in patients with persistent asthma. Am J Med.
2002;113:15-21.
24. Lazarus SC, Boushey
HA, et al. Long-acting beta2-agonists monotherapy vs continued therapy with
inhaled corticosteroids in patients with persistent asthma: a randomized
controlled trial. JAMA. 2001;285:2583-2593.
25. Fluticasone. In:
Klasco RK, ed. DRUGDEX System (electronic version). Thomson Micromedex,
Greenwood Village, Colo, USA. Available at: www.thomsonhc.com. Accessed April
30, 2007.
26. Greenstone IR, Ni
Chroinin MN, Masse V, et al. Combination of inhaled long-acting beta2-agonists
and inhaled steroids versus higher dose of inhaled steroids in children and
adults with persistent asthma. Cochrane Database of Systematic Reviews
2005, Issue 4. Art. No. CD005533. DOI: 10.1002/14651858.CD005533.
27. Ni Chroinin M,
Greenstone IR, et al. Long-acting beta2-agonists versus placebo in addition to
inhaled corticosteroids in children and adults with chronic asthma.
Cochrane Database of Systematic Reviews. 2005, Issue 4. Art. No. CD005535.
DOI: 10.1002/14651858.CD005535.
28. Nelson HS, Weiss
ST, et al. The salmeterol multicenter asthma research trial. A comparison of
usual pharmacotherapy for asthma or usual pharmacotherapy plus salmeterol.
Chest. 2006;129:15-26.
29. Castle W, Fuller R,
et al. Serevent nationwide surveillance study: comparison of salmeterol with
salbutamol in asthmatic patients who require regular bronchodilator treatment.
BMJ. 1993;306:1034-1037.
30. Salpeter SR,
Buckley NS, et al. Meta-analysis: effect of long-acting beta2
-agonists on severe asthma exacerbations and asthma-related deaths. Ann
Intern Med. 2006;144:904-912.
31. Montelukast. In:
Klasco RK, ed. DRUGDEX System (electronic version). Thomson Micromedex,
Greenwood Village, Colo. Available at: www.thomsonhc.com. Accessed April 30,
2007.
32. Stempel DA, Pinto
L, Stanford RH. The risk of hospitalization in patients with asthma switched
from an inhaled corticosteroid to a leukotriene receptor antagonist. J
Allergy Clin Immunol. 2002;110:39-41.
33. Theophylline. In:
Klasco RK, ed. DRUGDEX System (electronic version). Thomson Micromedex,
Greenwood Village, Colo. Available at: www.thomsonhc.com. Accessed April 30,
2007.
34. Omalizumab. In:
Klasco RK, ed. DRUGDEX System (electronic version). Thomson Micromedex,
Greenwood Village, Colo. Available at: www.thomsonhc.com. Accessed April 30,
2007.
35. Boehringer SK.
Tapering after short courses of corticosteroids: is it necessary. Pharmacist's
Letter/Prescriber's Letter. 2003;10:191210.
36. Prednisone. In:
Klasco RK, ed. DRUGDEX System (electronic version). Thomson Micromedex,
Greenwood Village, Colo. Available at: www.thomsonhc.com. Accessed April 30,
2007.
37. Zive JL. A
pharmacist's role in asthma care. US Pharm. 1999;32(7):41-48.
To comment on this article, contact
editor@uspharmacist.com.






