US Pharm. 2016;41(2):48-50.
Beginning on the first of this year, pharmacists in Oregon are able to prescribe and dispense hormonal birth control products to adult women without a prescription from a physician.1 California pharmacists are likely next to enjoy this privilege.2 Other states are in line to follow. This differs from emergency contraception, where the drug used to be obtained by prescription only, then could be dispensed by pharmacists from behind-the-counter, and finally become available OTC.3
Overview of the Oregon Law
The Oregon law lets pharmacists “prescribe and dispense hormonal contraceptive patches and self-administered oral hormonal contraceptives” to any woman who is at least 18 years old and to a girl under the age of 18 if she has “evidence of a previous prescription from a primary care practitioner or women’s healthcare practitioner.”4 Under the law, pharmacists are forbidden from requiring patients to schedule appointments with them in order to get a prescription for birth control. At the same time, pharmacists cannot write or dispense prescriptions for women who do not “have evidence” of a visit to a women’s health provider within 3 years of the pharmacist’s initial prescription for birth control.5 The Board of Pharmacy Rules state that a qualified pharmacist may prescribe hormonal contraceptives to a patient pursuant to the “Standard Procedures Algorithm for Oregon RPh Prescribing of Contraceptives” (FIGURE 1).6,7 The process involves obtaining the patient’s medical history, pregnancy status, medication use, and a blood pressure screening prior to authorizing the prescription.
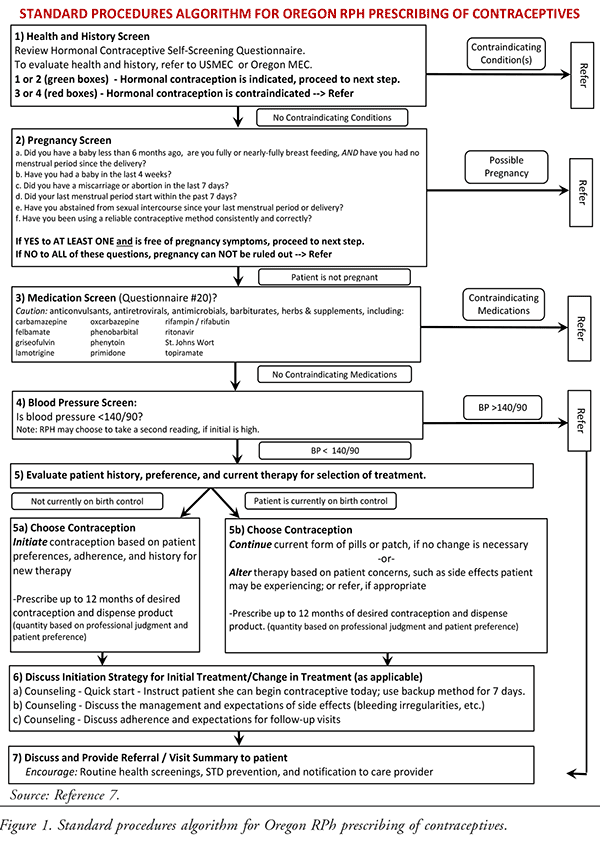
Eligible women can fill in a one-page health questionnaire available from the pharmacy.8 Minors still have to present a physician-supplied prescription. The purpose behind the new law is to increase access to self-administered hormonal birth control while addressing safety concerns, resulting in a decrease in unwanted pregnancies. Only self-administered oral or trans-dermal products are included in this program.6
The “Hormonal Contraceptive Self-Screening Questionnaire” asks the patient to state her name, healthcare provider, date of birth (age must be verified with valid photo ID), health insurance status, date of last women’s health clinic visit, and any allergies to medications. It also asks if the patient has a preferred method of birth control (i.e., daily pill, weekly patch, or other [ring, injectable, implant, IUD]). There are also five questions related to background information and 15 questions concerning medical history. The Background Information questions include8:
1. Do you think you might be pregnant now?
2. What was the first day of your last menstrual period?
3. Have you ever taken or are currently using birth control pills or a birth control patch, ring, or shot/injection? Did you ever experience a bad reaction to using hormonal birth control?
4. Have you ever been told by a medical professional not to take hormones?
5. Do you smoke cigarettes?
The Medical History portion of the form is quite detailed. Questions include8:
6. Do you think you might be pregnant now?
7. Are you currently breastfeeding?
8. Do you have diabetes?
9. Do you get migraine headaches?
10. Do you have high blood pressure, hypertension, or high cholesterol?
11. Have you ever had a heart attack or stroke, or been told you had any heart disease?
12. Have you ever had a blood clot?
13. Have you ever been told by a medical professional that you are at risk of developing a blood clot?
14. Have you had recent major surgery or are you planning to have surgery in the next 4 weeks?
15. Have you had bariatric surgery or stomach reduction surgery?
16. Do you have or have you ever had breast cancer?
17. Do you have or have you ever had hepatitis, liver disease, liver cancer, or gall bladder disease, or do you have jaundice (yellow skin or eyes)?
18. Do you have lupus, rheumatoid arthritis, or any blood disorders?
19. Do you take medication for seizures, tuberculosis, fungal infections, or HIV?
20. Do you have any other medical problems or take any medications, including herbs or supplements?
Following the prescribing and dispensing of contraceptives, the pharmacist is to give the patient a “Pharmacist Referral and Visit Summary” form.9 This template can be customized to the particular pharmacy, but it must retain all elements. When the patient is approved, it will state “Today you were prescribed the following hormonal contraceptive” and name the product. It will also inquire if the patient has any questions and include a space for the prescribing pharmacist’s name. If the patient was declined, it will state that “I am not able to prescribe hormonal contraception to you today,” and list four possible reasons. These reasons include that pregnancy cannot be ruled out, the patient has a health condition that requires further evaluation, the patient takes medications or supplements that may interfere with patches or pills, and the patient’s blood pressure reading is >140/90 mmHg. Each requires additional evaluation by another healthcare provider.9
Pharmacists wishing to participate in this new program must attend state-approved educational training seminars lasting 5 hours and learn how to prescribe the best hormonal therapy based on the health questionnaire assessment.10 All pharmacists have the capacity and opportunity to participate. Some pharmacists may decline to take part. This is allowed in Oregon rules, but there is a professional responsibility to refer the patient to an alternative pharmacy service provider.11 There is concern that some pharmacists may refuse to fill prescriptions for birth control on moral grounds, as such reports have surfaced in at least 25 states, according to the National Women’s Law Center.4
State-based insurance plans that pay for birth control must cover a 12-month supply of the medication at one time. Federal laws are comparable. The idea for this requirement springs from a study showing that patients who have a 1-year supply of the drugs have a lower rate of unintended pregnancies and abortions compared to women who have access to only a 1- or 3-month supply.12
Response to the Legislation
As might be expected, some physicians have expressed concern that too many women will skip the annual checkup, where they heretofore obtained their prescription for birth control. However, annual checkups might not be needed for some women. For example, the CDC recommends that women between 21 and 65 years of age get a Pap test for cervical cancer every 3 years. If they cotest, i.e., get a Pap smear and a human papillomavirus (HPV) test at the same time, it is enough to be screened every 5 years.13 Nevertheless, women are still encouraged to see a trusted gynecologist. This is because a minority of women develop blood clots after using birth control hormones, although the risk of developing one is less than getting a clot from pregnancy.14 Having an established relationship with a gynecologist for this type of concern could be lifesaving.
While physicians have rallied against pharmacist prescribing of birth control, some organizations have claimed that removing the physician from the prescribing scheme does not go far enough.1 The American College of Obstetricians and Gynecologists (ACOG) notes that having to go to the pharmacist for birth control is still an obstacle for some women. “Pharmacist prescribing laws are not the same thing as over-the-counter access,” ACOG said. “Requiring a pharmacist to prescribe and dispense oral contraceptives only replaces one barrier—a physician’s prescription —with another. This is not going to allow us to reach women who remained underserved by the current prescribing requirements.”1 Advocacy groups noted that men can access OTC birth control (i.e., condoms) without any restrictions.2
As of this writing, Oregon is the only state to actually permit pharmacist prescribing of birth control products. California passed legislation in 2013, and the law is expected to go into effect later in 2016.2 The California law will also require pharmacists to provide a health screening to women and take their blood pressure, but unlike Oregon’s law, it will have no age restrictions on patients. Colorado and Washington have introduced versions of the law in their state legislatures.1
Analysis
The Oregon laws should be viewed as a first-step in independent prescriptive authority for pharmacists. Obviously, other categories of medications could lend themselves to pharmacist prescribing. Since 1986, Florida pharmacists have had the right to prescribe Rx-only drugs on a state-approved formulary.15 Unfortunately, the “pharmacist prescribing law” has been dormant for a variety of reasons.16 Hopefully, the same will not happen in Oregon and in the other states with pending legislation.
REFERENCES
1. Geggel L. New Oregon law allows pharmacists to prescribe birth control pills. Live Science. January 4, 2016. www.livescience.com/53256-oregon-birth-control.html. Accessed January 12, 2016.
2. Ostrov BF. Pharmacists can prescribe ‘the pill’ in these states. CNN Health. July 14, 2015. www.cnn.com/2015/07/14/health/pharmacist-prescribe-hormonal-contraceptives/. Accessed January 12, 2016.
3. FDA approves Plan B One-Step emergency contraceptive for use without a prescription for all women of child-bearing potential. FDA news release. June 20, 2013. www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm358082.htm. Accessed January 21, 2016.
4. HB 2879 (2015). 78th Oregon Legislative Assembly. https://olis.leg.state.or.us/liz/2015R1/Downloads/Measure Document/HB2879/Enrolled. Accessed January 14, 2016.
5. Whitman E. Pharmacists prescribing birth control: Oregon becomes first state to offer pills, patches over the counter. International Business Times. January 4, 2016. www.ibtimes.com/pharmacists-prescribing-birth-control-oregon-becomes-first-state-offer-pills-patches-2247827. Accessed January 14, 2016.
6. OAR 855-019-0400 through 855-019-0435. Oregon Administrative Rules. Effective January 1, 2016. www.oregon.gov/pharmacy/Imports/Rules/November15/Div019ContraceptiveTemp Rules11.6.15.pdf. Accessed January 12, 2016.
7. Standard procedures algorithm for Oregon RPh prescribing of contraceptives. Oregon Administrative Rules. www.oregon.gov/pharmacy/Imports/ContraceptivePrescribing/ORStandardProceduresAlgorithmForRPHPrescribingOfHormonalContraceptives11_2015.pdf. Accessed January 14, 2016.
8. Hormonal contraceptive self-screening questionnaire. Oregon Administrative Rules. www.oregon.gov/pharmacy/Imports/ContraceptivePrescribing/ORSelf-ScreeningRiskAssessmentQuestionnaire11.2015.pdf. Accessed January 14, 2016.
9. Pharmacist referral and visit summary. Oregon Administrative Rules. www.oregon.gov/pharmacy/Imports/ContraceptivePrescribing/VisitSummaryTemplate.pdf. Accessed January 14, 2016.
10. Comprehensive contraceptive education and training for the prescribing pharmacist. Oregon State University Professional and Continuing Education. https://pace.oregonstate.edu/catalog/comprehensive-contraceptive-education-and-training-prescribing-pharmacist. Accessed January 14, 2016.
11. Oregon pharmacists tasked to improve access to hormonal birth control. Frequently asked questions. Oregon State Pharmacy Association. www.oregonpharmacy.org/hb2879---hormonal-birth-control-faqs#WhatIsLaw. Accessed January 12, 2016.
12. Foster DG, Hulett D, Bradsberry M, et al. Number of oral contraceptive pill packages dispensed and subsequent unintended pregnancies. Obstet Gynecol. 2011;117(3):566-572. http://journals.lww.com/greenjournal/Abstract/2011/03000/Number_of_Oral_Contraceptive_Pill_Packages.8.aspx. Accessed January 12, 2016.
13. Cervical cancer. What should I know about screening? CDC. www.cdc.gov/cancer/cervical/basic_info/screening.htm. Accessed January 12, 2016.
14. Committee on Gynecologic Practice. Over-the-counter access to oral contraceptives. December 2012. www.acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-Gynecologic-Practice/Over-the-Counter-Access-to-Oral-Contraceptives. Accessed January 12, 2016.
15. Savino TA. Legal authority for a pharmacist’s order for prescription drugs. WebRx Pharmacy Palace. www.rxpalace.com/laws.htm. Accessed January 12, 2016.
16. Pharmacist prescribing formulary in Florida. SDN Pharmacy Forum. http://forums.studentdoctor.net/threads/pharmacist-prescribing-formulary-in-fl.824738/. Accessed January 12, 2016.
To comment on this article, contact rdavidson@uspharmacist.com.





