US Pharm. 2011;36(11):72-76.
Depression affects an estimated 121 million people worldwide.1 To offer a different, perhaps more personal, perspective, a national survey indicated that more than 16% of Americans will experience major depressive disorder in their lifetime.2 The survey also revealed that individual episodes of major depressive disorder last an average of 16 weeks—or longer, when rated as “very severe” according to the Quick Inventory of Depressive Symptomatology Self-Report—despite 57.3% of individuals reporting that they have received some type of treatment for their depression. In addition, only about 20% of cases in a given year are considered adequately treated.2 Furthermore, the time to remission in the landmark STAR*D (Sequenced Treatment Alternatives to Relieve Depression) trial was a mean of 6.7 weeks, leading to a remission rate of just 28%.3 Given these statistics, it is easy to understand why depression is one of the chief causes of disability globally.2 These facts highlight the positive effect personalized drug therapy would have on the management of this devastating illness. Individualized therapy for depression would revolutionize treatment and allow optimization of drug efficacy while minimizing toxicity. This article will discuss whether individualized treatment of depression remains a dream or is being actualized.
Relationship Between Depression and Genetics
The terms pharmacogenetics and pharmacogenomics have been used to describe how gene variation—in single genes or whole genomes—influences drug response and side effects.4 (See ADDITIONAL RESOURCES box for more information.) With regard to medication use, genetic factors play a large role in response and side-effect rates.4 However, one meta-analysis found that the heritability of liability for major depression is 37%, with the remaining 63% accounted for by individual specific factors related to the environment.5 Heritability of drug response also has been described, although this is affected by the environment as well.4 The complicated relationship between genes and the environment in major depression and drug response offers challenges that are perhaps best summarized by Lohoff and Ferraro: “The field of psychiatric genetics has been historically disappointing given that the initial hope to find common gene variants of large effect in the pathogenesis of mental illness have been unsuccessful.”6 One study suggests that pharmacogenetic testing may be particularly useful in individuals with treatment-resistant depression or those who experience medication intolerance, but that additional guidance is needed and the harms of genetic testing should be further explored.7 With these limitations in mind, this article will summarize some of the current research that may enhance our understanding of depression and assist in the development of more effective treatments that are better tolerated.

Possible Candidate Genes
The ability to detect specific genes in patients will allow clinicians to predict how patients will metabolize certain medicines and will guide effective therapy choices while reducing the side-effect burden. Pharmacogenetic influences on drug response have been divided predominately into pharmacokinetic (absorption, distribution, metabolism, and elimination) and pharmacodynamic (processes on the receptor level influencing drug concentration and resultant effect) outcomes.4
Genetics influences individual treatment response to antidepressant medications.8 Specific gene markers have been evaluated in various studies to determine their impact on treatment outcomes, including their ability to predict specific adverse effects. STAR*D is largely cited when pharmacogenetic data are discussed, owing to its capturing of DNA samples from 1,914 diverse, real-world individuals living with major depressive disorder.3,8 STAR*D, which was supported by the National Institute of Mental Health, is the largest prospective study of unipolar depression.3 In this trial, four levels of treatment were investigated in patients at 41 different sites. Although STAR*D was not designed to assess pharmacogenetic characteristics, it changed pharmacogenetic research by expanding current knowledge about antidepressant response and tolerability. A summary of markers explored in STAR*D and other studies may be found in TABLE 1.3,6,8-11
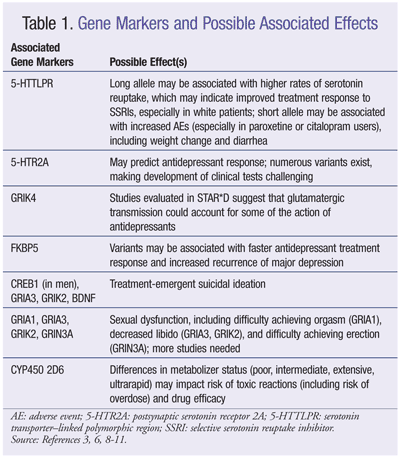
It is important to note that several studies have evaluated genes from various biological pathways listed in TABLE 1. In many cases, a combination of genes from the systems listed are better predictors of antidepressant response than any single gene candidate, further complicating the clinical utility of these data.10 Despite the tremendous value the ability to identify these genetic predictors would have—including elucidation of the role of these adverse effects on adherence—current studies require replication, and additional data on various ethnic groups are needed.3,8
Currently Available Genetic Testing
The FDA approved the Roche AmpliChip CYP450 genotyping test in January 2005. AmpliChip CYP450, which is the first FDA-approved pharmacogenetic test for variants in CYP2D6 and CYP2C19, permits the individualization of therapy.12
According to the manufacturer, the AmpliChip CYP450 test “provides comprehensive detection of gene variations—including deletions and duplications—for the CYP2D6 and CYP2C19 genes, which play a major role in the metabolism of an estimated 25% of all prescription drugs.”13 The test helps clinicians determine appropriate treatment plans, including dosing, for medications metabolized by CYP2D6 or CYP2C19. Since CYP2D6 is involved in the metabolism of many psychotropic drugs, the test could be particularly useful for patients taking these agents.
The AmpliChip CYP450 test analyzes the patient’s DNA to predict the phenotype. Blood serum or a buccal swab may be used for the DNA sample. The patient is classified according to four phenotypes for CYP2D6 gene activity: the ultrarapid metabolizer, who has more difficulty reaching therapeutic concentrations; the extensive (normal) metabolizer; the intermediate metabolizer, who experiences more adverse effects; and the poor metabolizer, who is at highest risk for overdose. Although genetic testing may aid in clinical choices, insurance companies do not cover the cost (approximately $400 per AmpliChip) because genetic testing is not the standard of care for medication management during psychotropic therapy.12 See the ADDITIONAL RESOURCES box for more information.
FDA Guidance on Pharmacogenetic Testing
The FDA issued its document Guidance for Industry and FDA Staff: Pharmacogenetic Tests and Genetic Tests for Heritable Markers on June 19, 2007.14 The guidance document outlines analytical studies and labeling considerations for pharmacogenetic tests. According to the guidance document, clinical studies need defined protocols prior to data collection. The protocol should clearly define the sample size, subject inclusion and exclusion criteria, variations between sampling sites, and data evaluation that will justify and represent the population in which the device is intended to be used. The lack of prospective clinical trials, however, is a limitation for the field of pharmacogenetics. Labeling should include clear instructions describing the features of the test; the quality-control measures incorporated to ensure that the device is performing as intended; a key for interpreting the results; test limitations; and procedures for the handling and collection of samples to minimize false results. The analytical data supporting the test’s performance should demonstrate the ability of the test to “accurately and reproducibly differentiate genotypes, alleles, or mutations using both the lowest and highest” DNA concentrations with adequate precision and specificity.14
Despite the issuance of this guidance document, warning letters from the FDA have recently been distributed to certain manufacturers or marketers of direct-to-consumer genetic tests who failed to obtain premarket approval for these medical devices. FDA enforcement of premarket approval is essential to help minimize the impact of being “misled by incorrect test results or unsupported clinical interpretations.”15
Conclusion
The ability to detect gene variations may influence how clinicians approach treatment choices for antidepressant therapy, but data currently are not robust. Public interest in pharmacogenetic testing has been indicated, but no prospective study has proven a clinical superior outcome or reduced side-effect burden when drug and dosing choices are based upon CYP2D6 genetic information.10,16 Furthermore, there is a lack of cost-effectiveness data and an absence of clinical recommendations on which populations are most likely to benefit from genetic testing.6 Because of societal demands and public interest, pharmacists must be prepared to provide patient education regarding the clinical utility of direct-to-consumer genetic testing for depression. With research in this area expanding and the FDA supporting pharmacogenomic initiatives, the current dream of personalized medicine for depression may soon become a reality.
The content of this article does not reflect the views or policies of the Department of Health and Human Services, nor does mention of trade names, commercial products, or organizations imply endorsement by the U.S. government.
REFERENCES
1. World Health Organization. Depression.
www.who.int/mental_health/
2. Kessler RC, Berglund P, Demler O, et al. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289:3095-3105.
3. Trivedi MH, Rush AJ, Wisniewski SR, et al. Evaluation of outcomes with citalopram for depression using measurement-based care in STAR*D: implications for clinical practice. Am J Psychiatry. 2006;163:28-40.
4. Schosser A, Kasper S. The role of pharmacogenetics in the treatment of depression and anxiety disorders. Int Clin Psychopharmacol. 2009;24:277-288.
5. Sullivan PF, Neale MC, Kendler KS. Genetic epidemiology of major depression: review and meta-analysis. Am J Psychiatry. 2000;157:1552-1562.
6. Lohoff FW, Ferraro TN. Pharmacogenetic considerations in the treatment of psychiatric disorders. Expert Opin Pharmacother. 2010;11:423-439.
7. Hoop JG, Lapid MI, Paulson RM, Roberts LW. Clinical and ethical considerations in pharmacogenetic testing: views of physicians in 3 “early adopting” departments of psychiatry. J Clin Psychiatry. 2010;71:745-753.
8. Laje G, Perlis RH, Rush AJ, McMahon FJ. Pharmacogenetics studies in STAR*D: strengths, limitations, and results. Psychiatr Serv. 2009;60:1446-1457.
9. Kato M, Serretti A. Review and meta-analysis of antidepressant pharmacogenetic findings in major depressive disorder. Mol Psychiatry. 2010;15:473-500.
10. Hortsmann S, Binder EB. Pharmacogenomics of antidepressant drugs. Pharmacol Ther. 2009;124:57-73.
11. Binder EB, Salyakina D, Lichtner P, et al. Polymorphisms in FKBP5 are associated with increased recurrence of depressive episodes and rapid response to antidepressant treatment. Nat Genet. 2004;36:1319-1325.
12. de Leon J, Susce MT, Murray-Carmichael E. The AmpliChip CYP450 genotyping test: integrating a new clinical tool. Mol Diagn Ther. 2006;10:135-151.
13. AmpliChip CYP450 test.
www.roche.com/products/
14. FDA. Guidance for Industry and FDA Staff: Pharmacogenetic Tests and Genetic Tests for Heritable Markers.
www.fda.gov/downloads/
15. Kuehn BM. FDA: gene tests need premarket approval. JAMA. 2010;304:145.
16. Herbild L, Bech M, Gyrd-Hansen D. Estimating the Danish populations’ preferences for pharmacogenetic testing using a discrete choice experiment. The case of treating depression.
Value Health.
2009;12:560-567.
To comment on this article, contact rdavidson@uspharmacist.com.






