US Pharm. 2007;32(11):26-32.
Bipolar disorder, also commonly referred to as manic depression, is a diagnosis of brain dysfunction characterized by severe alterations in mood and energy with a diminished capacity for daily functioning. It is thought to affect approximately 1% of the general population, a lifetime prevalence rate that appears consistent across many cultures. No significant differences in risk for developing the disorder have been detected based on race, ethnicity, or gender. Its key feature involves the emergence of multiple and distinct mood episodes of varying types over time. It is considered a chronic disorder with a variable course and is associated with significant morbidity and mortality; the mean rate of suicide completion approximates 10%.1
Diagnosis and Symptoms
The four different types of mood
episodes associated with bipolar disorder, based on the Diagnostic and
Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (
DSM-IV-TR), are defined as manic, major depressive, hypomanic, or mixed. A
manic episode is probably the type most commonly associated with bipolar
disorder. The formal diagnosis requires the presence of elevated--either
expansive or irritable--mood for a period of at least one week, accompanied by
at least three of the following (four if the mood is only irritable): inflated
self-esteem, decreased need for sleep, racing thoughts or flight of ideas,
pressured speech, distractibility, increased psychomotor activity, or
increased involvement in activities that are pleasurable but have a high risk
for negative consequences. Significant impairment of functioning or need for
hospitalization should also be present.1
The criteria for a major
depressive episode are identical to that required to make the diagnosis of
unipolar major depressive disorder. There should be at least a two-week period
of either a clearly depressed mood or the loss of interest or pleasure in
usual activities. In addition, other symptoms may include decreased appetite,
insomnia or hypersomnia, psychomotor retardation or agitation, feelings of
guilt or worthlessness, decreased energy, impaired concentration, and suicidal
thoughts. As with manic episodes, major depressive episodes impart
considerable disability.1
The other episode subtypes
also fall into a manic spectrum. A mixed episode is defined as a period of at
least one week in which both manic and major depressive episodes have emerged
nearly every day. A hypomanic episode is similar to mania, but the intensity
of symptoms is not as severe and there is no marked impairment in social or
occupational functioning. Another clinical phenomenon that may occur in about
10% to 20% of bipolar disorder cases is that of "rapid cycling," defined as
four or more mood episodes of any type within a one-year period.1
Four major subtypes of bipolar
disorder are defined by DSM-IV-TR.1 Bipolar I disorder is
characterized by one or more manic or mixed episodes along with major
depressive episodes. Bipolar II disorder is defined by a clinical course of
recurrent major depressive episodes, accompanied by at least one hypomanic
episode without any history of mania or mixed episodes. Cyclothymic disorder
consists of chronic fluctuations between subsyndromal depressive and hypomanic
episodes. Bipolar Disorder Not Otherwise Specified is used to denote changing
mood states that do not meet formal DSM-IV-TR diagnostic criteria for
any specific bipolar disorder.
Because most patients with
bipolar disorder will present with more depressive episodes than manic ones,
2 it is important to obtain a careful longitudinal history of episodes.
This will help distinguish the presence of unipolar major depressive disorder
from that of bipolar disorder, which requires some evidence of episodes in the
manic spectrum. It is also critical to fully characterize the clinical
presentation of the patient; i.e., whether symptoms are currently active and
causing distress or are stable and in relative remission. Emerging research
indicates that knowledge of such details can be particularly useful to
clinicians in managing bipolar disorder.
Pharmacotherapy Goals
The selection of
appropriate pharmacotherapy depends on both the history and presentation of
treatable symptoms. As medication options have increased in number, various
treatment guidelines have been developed from clinical studies and expert
consensus to facilitate evidence-based medication management. Recent sources
for these include the Texas Implementation of Medication Algorithms (TIMA)
initiative,3 the Expert Consensus Guideline Series (ECS),4
and the American Psychiatric Association (APA).5
The specific goals of drug
treatment in bipolar disorder will change depending on the stage of the
illness. In the acute phase, reduction of active target symptoms and overall
mood stabilization are the focus. Once these occur, medications are continued
to prevent future mood episodes and to enhance the chances of improved
psychosocial functioning. The actual choice of a mood stabilizer is determined
by knowledge of established efficacy and a reasonable risk-benefit evaluation
regarding the likelihood of adherence and the extent of side effects. Patient
preference should also be taken into consideration. It is important to realize
that pharmacotherapy alone will not provide the best treatment outcomes.
Ideally, all pharmacotherapy is accompanied by psychotherapy or other
nonpharmacologic interventions if optimal outcomes are to be achieved, and
this is supported by a significant body of literature.5 In
addition, there may be clinical presentations of bipolar disorder that do not
completely respond to a single agent, and combinations of mood stabilizers are
commonly required to bring symptoms into remission.
Acute Mania or Mixed
Episodes
There are many pharmacologic options
for treating acute manic episodes. If the presenting episode is particularly
severe, short-term adjunctive treatment with a benzodiazepine may be used as
the mood stabilizer is initiated. As with antidepressants, the full effects of
mood-stabilizing agents may not be realized until after several weeks of
continuous therapy. The primary therapeutic goal would be the remission of
symptoms, including rapid control of any agitation, aggression, or impulsivity
that may be present. Antipsychotics have also been used effectively to treat
concomitant symptoms of mania and psychosis.5
Acute Bipolar Depression
As with unipolar
major depression, the most important goal of treatment is remission of the
observed signs and symptoms consistent with the episode, with eventual return
to normal levels of psychosocial functioning.5 A risk associated
with the use of antidepressant monotherapy in bipolar depression is if the
patient suddenly switches from a depressive to a manic or hypomanic state.
Many clinicians would temper this risk by using a mood stabilizer as
adjunctive therapy. Other options that do not involve the use of
antidepressants alone include lithium, lamotrigine, olanzapine-fluoxetine, and
quetiapine.4,5
Maintenance Treatment
Once acute symptoms
have subsided, the focus shifts to the prevention of relapse, resolution of
any residual symptoms, reduction of episode frequency, minimization of suicide
risk, and optimization of overall functioning.5 To date, there is
limited empirical evidence available to inform the clinician attempting to
make the best choices of long-term pharmacotherapy. However, much current
research has been devoted to this topic, and new data should be forthcoming.
Pharmacotherapy Options for
Bipolar Disorder
Lithium
Acute Mania or Mixed Episodes:
Lithium has a long history of evidence to support its role as first-line
therapy in the treatment of acute mania. Early placebo-controlled studies have
suggested that the overall response rate of acute symptoms to lithium is about
78% and that up to two weeks of continuous therapy may be needed to optimize
effectiveness.6 Because of lithium's narrow therapeutic index, the
monitoring of steady-state serum concentrations is part of general clinical
practice, with a targeted range of 0.6 to 1.2 mEq/L.
Acute Bipolar Depression:
A review of multiple studies revealed that about 60% to 80% of patients with
bipolar disorder in the depressive phase responded to lithium monotherapy.
7 In general, the time frame for a depressive episode to resolve is
longer than that for a manic one (i.e., at least six to eight weeks). If the
clinical situation warrants a shorter onset of response, other interventions
adjunctive to lithium (adding an antidepressant, psychotherapy, or a second
mood stabilizer) may be initiated. Lithium is considered to be one of the
first-line agents for this episode subtype, although it may take six to eight
weeks of continuous treatment to control or eliminate symptoms of depression.
8
Maintenance:
Open-label studies and clinical experience have established the efficacy of
lithium in reducing the frequency, duration, and severity of both manic and
depressive episodes, although more recent data suggest greater efficacy in
preventing mania.9 The likelihood of sustained effects is enhanced
if a patient has a history of good functioning between episodes and a positive
family history of bipolar disorder with known lithium response. A significant
reduction in mortality may be achieved with long-term lithium, which has been
shown to reduce suicide risk by eight to 10-fold.10
Valproic Acid
Acute Mania
or Mixed Episodes: A
growing body of controlled clinical studies has supported the use of valproic
acid or its derivatives to treat acute mania since divalproex sodium was first
approved for this use in 1995. Some reports have suggested that valproate may
be more effective than lithium in certain subtypes of the disorder (e.g., when
rapid cycling or mixed episodes are present).5,11 While definitive
therapeutic serum concentrations have not been established for valproic acid
in bipolar disorder, based on a seminal trial,12 most clinicians
would target a range of 50 to 125 mcg/mL.
Acute Bipolar Depression:
In contrast to the
literature that has confirmed the use of valproate in acute mania, there are
no analogous controlled clinical trials investigating its efficacy in treating
acute bipolar depression. The lack of supportive evidence for this indication
has led to the relative exclusion of valproate from current practice
guidelines for bipolar depression, except in combination with other mood
stabilizers and antidepressants in treatment-resistant patients.3
Maintenance:
A randomized, placebo-controlled trial compared the effects of lithium,
valproate, and placebo in prolonging the time to recurrence of any mood
episode over a 52-week study period.9 No significant differences
were found among the three treatment arms, an outcme that diverges from the
known maintenance efficacy of lithium, rendering this trial a "failed study."
However, valproate was found to be superior to lithium on the secondary
outcome measure of time to recurrence of mania in the study. Other definitive
trials using valproate in long-term therapy are lacking.
Carbamazepine
Acute Mania or Mixed Episodes:
Carbamazepine has been used for several years off-label for treating acute
manic episodes, but only its beaded extended-release formulation has been
approved for this indication and for mixed episodes. Historically, it has also
been used as an alternative for rapid-cycling patients who evinced minimal
responses to lithium. Its known hematologic side-effect profile and propensity
for significant drug interactions make it potentially challenging to use. The
results from clinical trials with designs of varying credibility generally
support the use of carbamazepine for acute mania. In some studies, it was
demonstrated to be as effective as valproate and lithium.13
Acute Bipolar Depression:
Archival double-blind, placebo-controlled studies enrolling depressed
patients diagnosed with different subtypes of bipolar disorder demonstrated a
good or partial response to carbamazepine.14,15 More robust
responses were found in another trial in which carbamazepine therapy was
augmented with lithium.16
Maintenance:
Evidence for the use of long-term carbamazepine in the prevention of mood
episodes is limited. One six-month open-label study using the beaded
extended-release formulation demonstrated prophylactic activity in patients
with recently manic or mixed episodes.17
Second-Generation or Atypical Antipsychotics
Acute Mania or Mixed Episodes: Much of the recent drug trial research in bipolar disorder has focused on this class of medications, and the collective results of several studies suggest that there may be an antimanic "class effect."18 Randomized, double-blind, placebo-controlled or comparator studies19 have established the efficacy of risperidone, quetiapine, ziprasidone, and aripiprazole in the treatment of acute manic or mixed episodes, with some suggesting that the adjunctive use of second-generation antipsychotics (SGAs) with mood stabilizers may be helpful. A complete understanding of the risks associated with long-term use of SGAs is not fully known. However, the growing evidence for emerging metabolic syndrome with this class of drugs has prompted specific guidelines for scheduled laboratory and physical examination assessments in continuing SGA treatment to prevent relapse of psychiatric symptoms.20,21
Acute Bipolar Depression: Two SGAs that are associated with apparent efficacy in treating acute depressive episodes are quetiapine and olanzapine. In a series of multicenter trials,22 quetiapine monotherapy at dosages of 300 and 600 mg/day was found to be superior to placebo when depressive symptoms in patients with bipolar disorder were assessed. In another study that compared the effects of olanzapine, fluoxetine, and a combination product of olanzapine-fluoxetine in treating bipolar depressive symptoms, olanzapine monotherapy elicited a response that was not as robust as the response associated with the combination.23
Maintenance: The literature supporting the use of SGAs in preventing recurrence of bipolar disorder symptoms is small but growing. Published studies to date have focused on olanzapine and aripiprazole. Olanzapine has been investigated for its efficacy against placebo and comparator drugs. Olanzapine was found to be superior to placebo24 and comparable to lithium25 and divalproex26 in the time to relapse into mania or depression. Aripiprazole has also demonstrated efficacy in delaying the time to relapse compared with placebo.27
Other Drugs and Combinations
Lamotrigine: Per APA and TIMA guidelines4,5 and controlled trials,28,29 the niche for this anticonvulsant agent as monotherapy in bipolar disorder appears to be for both treatment of acute depressive episodes and maintenance treatment in patients without a history of frequent or recent episodes of mania. Lamotrigine has received specific approval by the FDA for use in delaying the time to recurrence of mood episodes. Since its effects on resolving manic spectrum symptoms have not been found to be as robust as for treating depressive ones, lamotrigine has often been used successfully in combination with other mood stabilizers to prevent relapse.30 As lamotrigine has been associated with serious rashes, including Stevens-Johnson syndrome, careful monitoring for dermatologic changes is essential.37
Oxcarbazepine: A chemical analog of carbamazepine, oxcarbazepine has positive but limited evidence for its use in the treatment of bipolar disorder. A series of two-week trials in patients with acute mania showed that oxcarbazepine was more effective than placebo and similar in efficacy to lithium or haloperidol. 31 A larger 10-week trial demonstrated equal efficacy between valproate and oxcarbazepine.32 Overall, compared to the literature for carbamazepine, there are fewer well-controlled studies of oxcarbazepine in patients with bipolar disorder.
Olanzapine-Fluoxetine: This combination product shares the distinction with quetiapine of being one of the few agents with an FDA indication for the acute treatment of depressive episodes in bipolar disorder. In a double-blind, placebo-controlled study that included a parallel arm testing olanzapine monotherapy, olanzapine-fluoxetine was found to be superior to both placebo and olanzapine alone in effectively reducing the core mood symptoms of depression.23
Benzodiazepines: Short-term use of longer-acting benzodiazepines--e.g., clonazepam and lorazepam--is appropriate in the management of acute mania, significant agitation or anxiety, or severe insomnia during a mood episode. These agents are often used as adjunctive therapy to mood stabilizers but are generally discontinued as these acute symptoms subside.5,33
Antidepressants: Prior to the discovery that SGAs demonstrate efficacy against bipolar depression, both tricyclic and SSRI antidepressants were used to treat the debilitating target symptoms associated with this condition. Such use had been a choice made with caution, since antidepressant monotherapy had been linked to a risk of "switching" into mania in individuals with undiagnosed bipolar disorder. Current guidelines recommend the concurrent use of antidepressant and mood stabilizer pharmacotherapy if agents from those therapeutic classes are chosen.3-5
Third-Generation
Anticonvulsants:
Earlier reports of the therapeutic efficacy of gabapentin in treating acute
mania through open-label trials have been countered by more recent controlled,
double-blind studies that have shown no difference between gabapentin and
placebo.29,34 The lack of well-designed controlled trials involving
the use of topiramate in the management of acute bipolar mania or depression
indicates that its role has yet to be defined, although open-label trials have
suggested some efficacy as adjunctive treatment with other mood stabilizers.
35
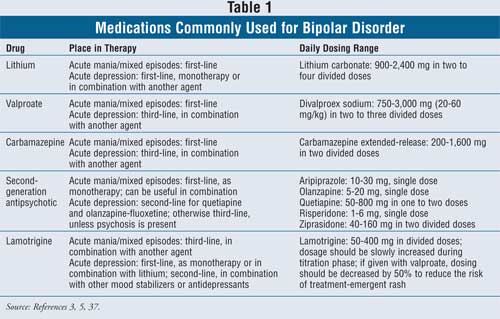
Dosing information for the
most commonly used medications in the treatment of bipolar disorder is listed
in Table 1.
The Role of the Pharmacist
Pharmacists have a key role in the
drug therapy management of bipolar disorder. In addition to the usual
counseling of patients about the common side effects and potential drug
interactions associated with their prescribed medications, education regarding
the nature of the disease state and expected medication responses can be
extremely helpful to patients and their supportive caregivers. Many of the
agents now used in treating bipolar disorder were originally approved for
other indications. Patients may need to be reassured that a drug that they
perceive as being used to treat primarily seizures or psychosis can be also
appropriate for their mood symptoms. Pharmacists can direct patients to
community resources; e.g., the National Alliance for the Mentally Ill,
consumer links on the National Institute of Mental Health (NIMH) Web site, or
community or Internet-based support groups for individuals with bipolar
disorder. In order to optimize medication response, other useful advice may
include maintaining regular patterns of sleep and daily activities, avoiding
alcohol or street drugs, and engaging in relaxation or stress-reduction
techniques.
A recent major NIMH-sponsored
research initiative exploring various interventions in more naturalistic
settings has been the Systematic Treatment Enhancement Program for Bipolar
Disorder (STEP-BD).36 Unlike controlled trials, this study enrolled
subjects with a more heterogeneous spectrum of symptoms typically found in
clinical settings where patients with bipolar disorder are managed. The intent
was to identify best practices in "real world" pharmacotherapy, with
particular interest in areas for which clinical drug trials are relatively
lacking (i.e., bipolar depression and relapse prevention). While the core
study has been completed, the entire analysis of the data has not yet been
fully reported or published. Pharmacists may access an updated bibliography of
studies at www.stepbd.org/referencelist.html.
Summary
Advances in the medication management of bipolar disorder beyond the traditional mood stabilizers include use of the second-generation or atypical antipsychotics, lamotrigine, and combination therapies for acute manic and mixed episodes. Bipolar depression may require specific treatment modalities that differ from those used for unipolar major depressive disorder. Optimizing long-term pharmacotherapy with the intention of preventing relapse is now a significant focus of research. Overall quality of life improvement is now recognized as a critical therapeutic outcome and may involve nonpharmacologic approaches in concert with medications. Because of pharmacists' knowledge of bipolar disorder and the medications used for treatment, they can serve as an invaluable resource in their role as educators and providers of pharmaceutical care.
References
1. American
Psychiatric Association. Diagnostic and Statistical Manual of Mental
Disorders, Fourth Edition, Text Revision. Washington, DC: American
Psychiatric Association; 2000:345-401.
2. Judd LL, Akiskal HS,
et al. The long-term natural history of the weekly symptomatic status of
bipolar I disorder. Arch Gen Psychiatry. 2002;59:530-537.
3. Suppes T, Dennehy E,
et al. The Texas Implementation of Medication Algorithms: update to the
algorithms for the treatment of bipolar disorder. J Clin Psychiatry.
2005;66:870-886.
4. Keck PE, Perlis RH,
et al. The Expert Consensus Guideline Series: treatment of bipolar disorder.
Postgrad Med Special Report. 2004:1-120.
5. American Psychiatric
Association. Practice guidelines for the treatment of patients with bipolar
disorder (revision). Am J Psychiatry. 2002;159(4 suppl):1-50.
6. Goodwin FK, Zis AP.
Lithium in the treatment of mania: comparisons with neuroleptics. Arch Gen
Psychiatry. 1979;36:840-844.
7. Price LH, Heninger
GR. Lithium in the treatment of mood disorders. N Engl J Med.
1994;331:591-598.
8. Zornberg GL, Pope HG
Jr. Treatment of depression in bipolar disorder: new directions for research.
J Clin Psychopharmacol. 1993;13:397-408.
9. Bowden CL, Calabrese
JR, et al. A randomized, placebo-controlled 12-month trial of divalproex and
lithium in treatment of outpatients with bipolar I disorder. Arch Gen
Psychiatry. 2000;57:481-489.
10. Goodwin FK.
Rationale for long-term treatment of bipolar disorder and evidence for
long-term lithium treatment. J Clin Psychiatry. 2002;63(suppl 10):5-12.
11. Calabrese JR,
Shelton MD, et al. Current research on rapid cycling bipolar disorder and its
treatment. J Affect Disord. 2001;67:241-255.
12. Bowden CL, Brugger
AM, et al. Efficacy of divalproex vs. lithium and placebo in the treatment of
mania. JAMA. 1994;271:918-924.
13. Emillen G,
Maloteaux JM, et al. Lithium compared to valproic acid and carbamazepine in
the treatment of mania: a statistical meta-analysis. Eur
Neuropsychopharmacol. 1996;245-252.
14. Ballenger JC, Post
RM. Carbamazepine in manic-depressive illness: a new treatment. Am J
Psychiatry. 1980;137:782-790.
15. Post RM, Uhde TW,
et al. Prophylactic efficacy of carbamazepine in manic-depressive illness.
Am J Psychiatry. 1983;140:1602-1604.
16. Kramlinger KG, Post
RM. The addition of lithium to carbamazepine: antidepressant efficacy in
treatment-resistant depression. Arch Gen Psychiatry. 1989;46:794-800.
17. Ketter RA, Kalali
AH, et al. A 6-month, multicenter, open-label evaluation of beaded,
extended-release carbamazepine capsule monotherapy in bipolar disorder
patients with manic or mixed episodes. J Clin Psychiatry.
2004;65:668-673.
18. Perlis RH, Welge
JA, et al. Atypical antipsychotics in the treatment of mania: a meta-analysis
of randomized, placebo-controlled trials. J Clin Psychiatry.
2006;67:509-516.
19. Scherk H, Pajonk
FG, et al. Second-generation antipsychotic agents in the treatment of acute
mania: a systematic review and meta-analysis of randomized controlled trials.
Arch Gen Psychiatry. 2007;64:442-455.
20. American Diabetes
Association, American Psychiatric Association, American Association of
Clinical Endocrinologists, North American Association for the Study of
Obesity. Consensus development and conference on antipsychotic drugs and
obesity and diabetes. Diabetes Care. 2004;27:596-601.
21. Marder SR, Essock
SM, et al. Physical health monitoring of patients with schizophrenia. Am J
Psychiatry. 2004;161:1334-1349.
22. Calabrese JR, Keck
PE Jr., et al. A randomized, double-blind, placebo-controlled trial of
quetiapine in the treatment of bipolar I or II depression. Am J Psychiatry
. 2005;162:1351-1360.
23. Tohen M, Vieta E,
et al. Efficacy of olanzapine and olanzapine-fluoxetine combination in the
treatment of bipolar I depression. Arch Gen Psychiatry.
2003;60:1079-1088.
24. Tohen M, Calabrese
JR, et al. Randomized, placebo-controlled trial of olanzapine as maintenance
therapy in patients with bipolar I disorder responding to acute treatment with
olanzapine. Am J Psychiatry. 2006;163:247-256.
25. Tohen M, Greil W,
et al. Olanzapine versus lithium in the maintenance treatment of bipolar
disorder: a 12-month, randomized, double-blind, controlled clinical trial.
Am J Psychiatry. 2005;162:1281-1290.
26. Tohen M, Ketter TA,
et al. Olanzapine versus divalproex sodium for the treatment of acute mania
and maintenance of remission: a 47-week study.Am J Psychiatry.
2003;160:1263-1271.
27. Keck PE Jr.,
Calabrese JR, et al. A randomized, double-blind, placebo-controlled 26-week
trial of aripiprazole in recently manic patients with bipolar I disorder. J
Clin Psychiatry. 2006;67:626-637.
28. Calabrese JR,
Bowden CL, et al. A double-blind placebo-controlled study of lamotrigine
monotherapy in outpatients with bipolar I depression. J Clin Psychiatry
. 1999;60:79-88.
29. Frye MA, Ketter TA,
et al. A placebo-controlled study of lamotrigine and gabapentin monotherapy in
refractory mood disorders. J Clin Psychopharmacol. 2000;20:607-614.
30. Calabrese JR,
Bowden CL, et al. Spectrum of activity of lamotrigine in treatment-refractory
bipolar disorder. Am J Psychiatry. 1999;156:1019-1023.
31. Keck PE Jr.,
McElroy SL, Nemeroff CL. Anticonvulsants in the treatment of bipolar disorder.
J Neuropsychiatry Clin Neurosci. 1992;4:395-405.
32. Reinstein MJ,
Sonnenberg JG, et al. Oxcarbazepine versus divalproex sodium for the
continuing treatment of mania. Clin Drug Investig.2003;23:671-677.
33. Alderfer BS, Allen
MH. Treatment of agitation in bipolar disorder across the life cycle. J
Clin Psychiatry. 2003;64(suppl 4):3-9.
34. Pande AC, Crockatt
JG, et al. Gabapentin in bipolar disorder: a placebo-controlled trial of
adjunctive therapy. Bipolar Disord. 2000;2:249-255.
35. Yatham LN,
Kusumakar V, et al. Third generation anticonvulsants in bipolar disorder: a
review of efficacy and summary of clinical recommendations. J Clin
Psychiatry. 2002;63:275-283.
36. Sachs GS, Thase ME,
et al. Rationale, design, and methods of the Systematic Treatment Enhancement
Program for Bipolar Disorder (STEP-BD). Biol Psychiatry. 2003;53:1028
1042.
37. DiPiro JT, Talbert
RL et al., eds. Pharmacotherapy: A Pathophysiologic Approach. 6th ed.
New York, NY: McGraw-Hill; 2005:1257-1284.
To comment on this article, contact editor@uspharmacist.com.






