US Pharm. 2016;41(5):31-34.
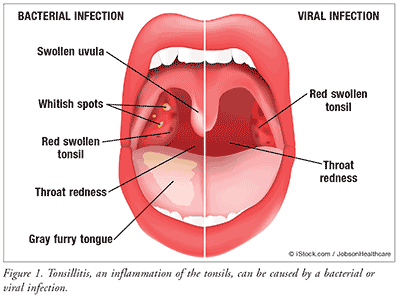
ABSTRACT: Tonsillectomy with or without adenoidectomy is the most commonly performed pediatric surgical procedure in the United States. There is controversy regarding which postsurgical analgesic agents are safe and effective. After reports of codeine-related fatalities, the FDA issued a Drug Safety Communication advising practitioners that codeine use in certain children after tonsillectomy may lead to rare but life-threatening respiratory failure and death. Post-tonsillectomy pain control recommendations changed to ensure safe and effective medication selection. Pharmacists can play an essential role in helping providers choose proper and safe analgesics after tonsillectomy.Tonsillectomy is a surgical procedure performed with or without adenoidectomy that completely removes the tonsil, including its capsule, by dissecting the peritonsillar space between the tonsil capsule and the muscular wall (FIGURE 1). Tonsillectomy with or without adenoidectomy is the most commonly performed pediatric surgery in the United States. The pain associated with this procedure is moderate-to-severe, and more than 500,000 tonsillectomies are performed on children in the U.S. every year.1,2 Reports of codeine-related fatalities have presented challenges with the choice of post-tonsillectomy analgesia.3
FDA Drug Safety Communication
Following reports of life-threatening adverse events and death in certain children who received codeine after tonsillectomy, the FDA issued a new black box warning and contraindication on use after tonsillectomy and/or adenoidectomy.3 Deaths have occurred postoperatively in children with obstructive sleep apnea (OSA) who received codeine for pain relief following surgery. These children had evidence of being ultrarapid metabolizers of codeine, which causes the liver to convert codeine into life-threatening or fatal amounts of morphine in the body. There is a need for an evidence-based noncodeine plan for children undergoing tonsillectomy.
Identifying Patients at Risk
It is very important to identify children who might be at risk of developing codeine-related adverse events and death after tonsillectomy. Some of these children had evidence of being ultrarapid metabolizers of substrates of the isoenzyme CYP2D6, including codeine. Codeine is metabolized in the liver to morphine by CYP2D6, which is highly polymorphic. These variations create four phenotypes for codeine metabolism: ultrarapid, extensive, intermediate, and poor metabolizers. Poor metabolizers (10% of the population) obtain no analgesia from codeine. These polymorphisms may result in varying analgesic results and toxicity.4,5
Respiratory comorbidities including unresolved apnea, asthma, bronchopneumonia, craniofacial disorders, obesity, and respiratory tract infections combined with swelling after surgery can further compound the respiratory effects of opioids. Children with OSA are more sensitive to opioids and require lower doses of analgesia, likely because of hypoxemia-induced changes in opioid receptors.6
Choice of Analgesia
For many years, otolaryngologists were reluctant to use nonsteroidal anti-inflammatory drugs (NSAIDs) after tonsillectomy for fear of platelet inhibition and postsurgical hemorrhage. In 2010, a Cochrane review update was published that found that NSAIDs (other than aspirin and cyclooxygenase-2 [COX-2] inhibitors) did not significantly alter postoperative bleeding compared with placebo or other analgesics.7 The updated review analyzed data from 15 randomized, controlled trials that included more than 1,000 children. Based on this evidence, the 2011 American Academy of Otolaryngology—Head and Neck Surgery (AAO-HNS) Clinical Practice Guideline on Tonsillectomy in Children states that ibuprofen can be used safely for pain control after adenotonsillar surgery.7 The usual recommended dosing for ibuprofen is 10 mg/kg by mouth every 6 hours in healthy children (no renal dysfunction) after tonsillectomy.6
A recent pediatric study by Liu and Ulualp advised that alternating doses of ibuprofen and acetaminophen provided an effective treatment for post-tonsillectomy pain in the majority of children and did not increase the rate of bleeding.8 The study included 583 patients. The acetaminophen dose was 10 mg/kg every 6 hours (not to exceed 4 g/day). The ibuprofen dose was 5 mg/kg every 6 hours (not to exceed 2.4 g/day).
Oxycodone and hydrocodone are commonly used oral opioids and, like codeine, are metabolized by CYP2D6. The clinical study of these drugs has been less extensive than that of codeine, but the use of hydrocodone in combination with acetaminophen (e.g., Vicodin) has been advocated as an effective alternative opioid for managing pediatric post-tonsillectomy pain.9
Unlike codeine, a relatively weak mu agonist whose analgesic action depends significantly on metabolic conversion to morphine, hydrocodone is believed to be primarily responsible for its observed analgesic effects (i.e., active metabolites play a minor role in its analgesic action). It is not known whether slow metabolizers will have reduced analgesia when treated with hydrocodone or if ultrarapid metabolizers may risk toxicity with normal doses.10
Although both hydrocodone and oxycodone are used to manage pain in adult patients following tonsillectomy and adenoidectomy, there is limited evidence to support their use in the management of post-tonsillectomy pain in children. If oral opioids are prescribed for post-tonsillectomy pain, provider awareness and parental education are critical to ensure that early signs of overdose are immediately reported to the prescribing practitioner.11 However, because hydrocodone is metabolized, in part, by the same CYP2D6 pathway as codeine, it may not be a good substitute. Oxycodone is a choice that has a favorable profile for efficacy, side effects, and metabolism, and only a small percentage of the drug is metabolized via CYP2D6.4
Best Practices
Recommendations for preventing and treating tonsillectomy pain in children involve both pharmacologic and nonpharmacologic therapy (TABLE 1).7 The 2011 AAO-HNS guideline suggests that it is important to educate caregivers about communicating with the child regarding severity of pain, pain medications, adequate hydration, giving pain medication on a regular schedule, the normal increase of pain in the mornings, and possible rectal administration of acetaminophen when oral medication is refused.7 Careful evaluation is also important to avoid overdosing. Scheduled acetaminophen, rather than taken as needed, is highly recommended as the first-line medication in children after adenotonsillectomy.

Statistically significant yet limited existing evidence suggests that ibuprofen is safe to use concomitantly or as a second-line medication.5 There should be education about avoiding the use of ibuprofen with dehydration owing to possible renal toxicity. Opioids including hydrocodone and oxycodone may be administered with caution in children with sleep-disordered breathing following tonsillectomy.5
The lowest possible dose should be chosen because children with sleep-disordered breathing are known to be particularly susceptible to respiratory depression from opioids. Following adenotonsillectomy, opioids should not be administered to any child who is excessively sleepy, lethargic, unarousable, or incoherent.5
In addition, any child who is having trouble breathing, including respiratory pauses while sleeping, should not receive opioids. A single intraoperative dose of IV dexamethasone (0.5 mg/kg, maximum dose 20 mg) is effective for the reduction of postoperative nausea, vomiting, and pain—and leads to an earlier return to a normal diet—but it may also lead to an increased need for operative reintervention for bleeding, and thus should be used with caution.12
Inpatient and emergency room monitoring for IV hydration and monitored pain control are safe options for selected patients. Ongoing monitoring of postoperative calls from families and review of possible increases in dehydration or bleeding are recommended to determine if adjustments to this guideline are needed.5 Large, long-term studies of the safety and efficacy of ibuprofen, the different opioids, and corticosteroids in this setting are still needed.
Supportive Care
Nonpharmacologic therapy to treat postoperative pain is an important adjunct therapy that nurses can initiate and control without medical orders. Common nonpharmacologic measures to assist in pain relief are having parents present, using effective distraction techniques, and offering cold foods.13 Although an educational intervention (i.e., preparatory information, comforting/reassurance, comfortable environment, distraction, and positioning) had a positive effect on nurses’ use of these therapies, many obstacles, such as language barriers or ongoing knowledge deficits, can prohibit consistent use of them.14 Therefore, an understanding of nonpharmacologic interventions by both nurses and caregivers is an important step in pain management after tonsillectomy.
In pediatrics, the focus is on family-centered care. Traditionally, parents were not allowed into the post-anesthesia care unit (PACU) because of patient sensitivity, quick turnover, and possible adverse effects of anesthesia. However, through education and promotion of the practice, an increase in visitation and earlier reunion of parent and child can take place. As anxiety contributes to pain intensity, promoting the presence of parents may help decrease anxiety and consequently reduce pain.15 Parental presence is valuable, although preparation is necessary so that it can be a positive experience for both parent and child.
Many of the aforementioned nonpharmacologic interventions implemented in the PACU are also useful at home. Additionally, cognitive behavioral pain management techniques such as music, imagery, and computer/video games assist with distraction.16 Post surgery, children have reported several therapies as being helpful, including eating soft or cold foods (e.g., popsicles), drinking plenty of fluids, not talking too much, applying cold packs, receiving comfort from their parents, being distracted, relaxing or resting, sleeping, and being positioned favorably.13,16
A Cochrane review suggests additional research is necessary to confirm if there are any effective pain relief outcomes from the use of either nonpharmacologic or pharmacologic oral rinses, mouthwashes, and sprays.17
Role of the Pharmacist
Healthcare professionals should prescribe an alternate analgesic for postoperative pain control in children who are undergoing tonsillectomy and/or adenoidectomy. Codeine should not be used for pain in children following these procedures. For management of other types of pain in children, codeine should only be used if the benefits are anticipated to outweigh the risks.3
Pharmacists can play essential role in helping providers choose proper and safe analgesics after tonsillectomy. Moreover, pharmacists can educate caregivers and parents who are involved in monitoring children postoperatively. Parents and caregivers who observe unusual sleepiness, confusion, or difficult or noisy breathing in their child should stop giving codeine or similar opioid analgesics and seek medical attention immediately, as these are signs of overdose.
REFERENCES
1. Baugh RF, Archer SM, Mitchell RB, et al; American Academy of Otolaryngology—Head and Neck Surgery Foundation. Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg. 2011;144(1 suppl):S1-S30.
2. Cullen KA, Hall MJ, Golosinskiy A. Ambulatory surgery in the United States, 2006. Natl Health Stat Rep. 2009;(11):1-25.
3. FDA Drug Safety Communication: safety review update of codeine use in children; new boxed warning and contra-indication on use after tonsillectomy and/or adenoidectomy. February 20, 2013. www.fda.gov/Drugs/DrugSafety/ucm339112.htm. Accessed January 7, 2016.
4. Smith HS. The metabolism of opioid agents and the clinical impact of their metabolites. Clin J Pain. 2011;27:824-838.
5. Yellon R, Kenna MA, Cladis FP, et al. What is the best non‐codeine postadenotonsillectomy pain management for children? Laryngoscope. 2014;124:1737-1738.
6. Kelly LE, Sommer DD, Ramakrishna J, et al. Morphine or ibuprofen for post-tonsillectomy analgesia: a randomized trial. Pediatrics. 2015;135:307.
7. Baugh R, Archer S, Mitchell R, et al; American Academy of Otolaryngology—Head and Neck Surgery Foundation. Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg. 2011;144(suppl 1):S1-S30.
8. Liu C, Ulualp SO. Outcomes of an alternating ibuprofen and acetaminophen regimen for pain relief after tonsillec-tomy in children. Ann Otol Rhinol Laryngol. 2015;124(10):777-781.
9. Bean-Lijewski J, Kruitbosch S, Hutchinson L, Browne B. Post-tonsillectomy pain management in children: can we do better? Otolaryngol Head Neck Surg. 2007;137(4):545-551.
10. Crews KR, Gaedigk A, Dunnenberger H, et al. Clinical Pharmacogenetics Implementation Consortium (CPIC) guidelines for codeine therapy in the context of cytochrome P450 2D6 (CYP2D6) genotype. Clin Pharmacol Ther. 2012;91(2):321-326.
11. Sutters K, Isaacson G. Posttonsillectomy pain in children. Am J Nurs. 2014;114(2):36-42.
12. Plante J, Turgeon AF, Zarychanski R, et al. Effect of systemic steroids on post-tonsillectomy bleeding and reinterventions: systematic review and meta-analysis of randomized controlled trials. BMJ. 2012;345:e5389.
13. Idvall E, Holm C, Runeson I. Pain experiences and non-pharmacological strategies for pain management after tonsillectomy: a qualitative interview study of children and parents. J Child Health Care. 2005;9(3):196-207.
14. He HG, Jahja R, Lee TL, et al. Nurses’ use of non-pharmacological methods in children’s post-operative pain management: educational intervention study. J Adv Nurs. 2010:66(11):2398-2409.
15. Crandall M, Lammers C, Senders C, Braun JV. Children’s tonsillectomy experiences: influencing factors. J Child Health Care. 2009;13(4):308-321.
16. Wiggins SA, Foster RL. Pain after tonsillectomy and adenoidectomy: “Ouch it did hurt bad.” Pain Manag Nurs. 2007;8(4):156-165.
17. Fedorowicz Z, Al-Muharraqi MA, Nasser M, et al. Oral rinses, mouthwashes and sprays for improving recovery following tonsillectomy. Cochrane Database Syst Rev. 2011;(7):CD007806.
To comment on this article, contact rdavidson@uspharmacist.com.





