US Pharm. 2017;42(8):29-34.
ABSTRACT: In the United States, only two genera of spiders are venomous enough to be considered medically relevant. These are the widow spiders (Latrodectus) and the recluse spiders (Loxosceles). While these venomous exposures are rarely fatal, bites can often lead to extremely painful muscle spasms or even skin necrosis. Nonpharmacologic and pharmacologic treatment options are available, including an antivenin for widow bites and opioids and benzodiazepines for symptom relief. Pharmacist involvement includes giving advice about prevention and treatment and providing appropriate patient counseling on prescribed or administered medications.
Spiders are found all around the world and are a great source of fear for many people, whether venomous or not. The United States has only two genera of spiders that are venomous enough to be considered medically relevant. These are the widow spiders (Latrodectus) and the recluse spiders (Loxosceles).1,2
Types of Venomous Spiders
Widow Spider: This spider, aptly named for the propensity of the female to eat the male after mating, is found worldwide, and five different species are present in the U.S.3 TABLE 1 shows the common locations of widow spiders. This spider can often be identified by a characteristic red or orange hourglass mark on the ventral abdomen.1 Widow spiders are commonly found outdoors, often in yard debris. Their bites usually result from a defensive action by the spider after it has been disturbed.1,4

Some differences between the male and female widow spiders include size and color. Male widow spiders tend to be smaller and lighter in color than females.4 Females tend to have a shiny black body (Latrodectus mactans, Latrodectus hesperus, Latrodectus variolus), brown body (Latrodectus geometricus), or black abdomen with bright red legs (Latrodectus bishopi). More important, it is the female widow spider that is venomous to humans; the male widow spider lacks the ability to envenomate humans.4,5
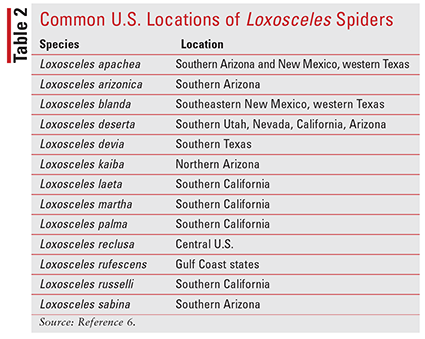
Recluse Spider: Thirteen different species of recluse spider are located in the U.S.1,6 The most widespread species in this genus is the brown recluse spider (Loxosceles reclusa), which is found in most central and southern Midwestern states. Other species are less widespread and often are contained within one to several states.6 The locations of the different recluse spider species are listed in TABLE 2.
The spiders in this genus are brown and contain no unique identifying features, with the exception of L reclusa, which has unique brown markings in the shape of a violin, fiddle, or cello on its dorsal thorax.1,7 Recluse spiders are commonly found indoors and in abundant numbers, usually hiding in dark places, such as behind furniture or in piles of clothes.1,8 As with widow spiders, female recluse spiders tend to be more venomous, darker, and larger than their male counterparts.7
Pathophysiology
Widow spider venom contains several different neurotoxins, known as latrotoxins, that act to impair or destroy nerve tissue. Of particular note is that latrotoxins seem to target specific types of animals. For example, some latrotoxins exert their effects only on insects; another type affects only crustaceans; and yet another targets only vertebrates. For vertebrates, the selective latrotoxin in widow spider venom is alpha-latrotoxin, which exerts its effects by two different mechanisms.9,10 After binding to a neuronal receptor, alpha-latrotoxin can enter the plasma membrane to form a pore or it can activate the receptor, leading to intracellular signaling. Both mechanisms result in a sizable release of presynaptic neurotransmitters, including acetylcholine, dopamine, glutamate, and norepinephrine.9 The release of these neurotransmitters can cause severe, painful muscle contractions.
Recluse spider venom contains several toxic enzymes, the most damaging one being sphingomyelinase D.1,7,11 Sphingomyelinases exert their effects on the body via multiple mechanisms. First, they can activate the complement system and the membrane attack complex by recruiting inflammatory cells to the site of the bite. The membrane attack complex and complement system, which are part of the body’s immune system, work together to clear cells of invading organisms and damaged host cells. The activation of the complement system from recluse spider venom induces dermonecrosis. Sphingomyelinase D also activates neutrophils, which can cause a breakdown of collagen fibers in the skin. There is an increase in the expression of gelatinase, which may lead to the development of skin breakdown.12 This process is also known as necrotic arachnidism.1
Signs and Symptoms of Common Exposures
A bite from a widow spider feels similar to a pinprick and may be moderately to severely painful.1,7 After exposure, there is often little to no sign of inflammation around the bite site.7 However, after a period of about 30 minutes to 1 hour, systemic toxicity begins, and muscle spasms and rigidity occur at and around the area of the bite.1,7 Depending on the location of the bite, the spasms and rigidity could then spread to the abdomen (if bite is on a lower extremity) or chest (if bite is on an upper extremity).1,7 In addition to muscular effects, other symptoms, such as generalized diaphoresis, fever, hypertension, nausea, and vomiting, may occur.1,7
The initial bite of a recluse spider is often minimally painful or not painful at all.1,7 Soon afterward, the skin around the bite site becomes tender and red.1 Unlike widow spider envenomation, systemic toxicity is delayed in recluse spider bites, with an incubation period of approximately 3 to 7 days.7 Common signs of systemic toxicity include joint pain, fever, chills, and maculopapular rash.7 Skin necrosis and severe ulceration are a result of the toxic enzymes of recluse spider bites mentioned earlier.12,13 One study showed that about 40% of recluse bites result in skin necrosis and that approximately 13% of these cause scarring.13
Treatment of Venomous Exposures
Although bites from widows or recluses can be alarming and appear quite serious, they often resolve without causing serious injury or death.7 The envenomation from a widow spider typically resolves within 2 to 3 days,1,7 but that from a recluse spider takes longer to resolve. Necrotic wounds caused by recluse bites take about 1 to 8 weeks to heal with proper wound care.7,12 Treatment options include nonpharmacologic and pharmacologic modalities.
Nonpharmacologic Therapies: Nonpharmacologic treatment options for widow spider bites are rather minimal. The first suggested treatment is to cleanse the wound at the site of the bite.7 Since the goal is to prevent infection, soap and water are sufficient to cleanse the wound. The next step is to apply an ice pack or other cold substance to the affected area to help reduce local pain and inflammation.7 Because spider bites have also been known to put patients at increased risk for contracting tetanus, a tetanus booster is recommended if the affected individual is not up-to-date on tetanus immunization.1,7
Nonpharmacologic treatment for recluse spider bites is similar to that for widow bites. The wound should first be cleansed to prevent infection. Then, a cold compress is applied to the affected area. The bite site should be immobilized and elevated if the bite occurred on an extremity. Lastly, tetanus prophylaxis should be given in the form of a tetanus booster.7 Overtreatment of a bite can potentially lead to more skin damage, and early excision of the bite site to prevent skin necrosis is contraindicated.1,7,14
Pharmacologic Therapies: Initial pharmacologic therapy for widow bites is aimed at relieving the associated muscle pain and cramping. Formerly, calcium gluconate was a first-line option to treat the symptoms associated with widow spider envenomation. However, reviews of widow spider exposure cases have shown that this treatment is not as effective as the use of IV benzodiazepines and opioids such as morphine (mean dose 15 mg) or meperidine (mean dose 88 mg).15 When the drugs were used as combination therapy, the mean doses of morphine and meperidine were 20 mg and 50 mg, respectively.15 Benzodiazepines, especially diazepam (mean dose 15 mg) or lorazepam (mean dose 4 mg), usually relieve the symptoms of muscle rigidity and spasms, and opioids are used to lessen the pain that accompanies envenomation.15 This therapy usually suffices to maintain the patient until symptoms resolve.1,7
In the case of severe toxicity associated with widow spider envenomation, a Latrodectus antivenin is available. Indications for antivenin use include uncontrolled hypertension, seizures, and respiratory arrest following envenomation.7 Antivenin use is usually considered up to 48 hours after a widow bite, but case reports have shown effectiveness for as long as 90 hours following exposure.1,4 Each vial of antivenin comes as a dry powder with a 2.5-mL vial of sterile diluent. The dosage for adults and children is the entire contents of the reconstituted vial, with administration either IM (anterolateral thigh) or via IV infusion in 10 to 50 mL of normal saline over a 15-minute time span.16 One dose is usually sufficient, and symptoms typically resolve in 1 to 3 hours. However, sometimes a second dose of antivenin may be necessary. Because the antivenin is made from horse serum, anaphylaxis precautions, such as the ready availability of a tourniquet and epinephrine, should be taken. The antivenin comes with a vial of horse serum to allow for sensitivity testing before administration. Serum sickness has been reported up to 12 days after antivenin administration.16
Pharmacologic therapy for recluse bites is less clear owing to the scarcity of clinical trials on the subject.1 Therapies such as hyperbaric oxygen, dapsone, and cyproheptadine have been thought to show a benefit in treating recluse bites. However, a randomized, controlled trial in rabbits, which display reactions similar to those of human beings, showed no additional benefit compared with the control group.17 Topical nitroglycerin was another proposed therapy to treat recluse envenomation, but it was also shown to be ineffective and may actually lead to increased systemic toxicity.18 Currently, an antivenom for recluse bites is not available in the U.S., and the usual therapy consists solely of supportive measures.19 Oral antihistamines such as diphenhydramine may be used to relieve itching and help heal necrotic wounds, and oral or parenteral analgesics may be used for pain relief.7,20
Methods of Preventing Bites
Wearing protective clothing such as gloves, long-sleeved shirts, and long pants tucked into socks when outdoors can help prevent widow bites. Applying insect repellent containing diethyltoluamide (DEET) to skin and clothing can provide extra protection.7 Clearing the area of yard debris and tall grass is a good way to prevent widow spiders from making their homes nearby. It is also a good idea to inspect and shake out gloves, shoes, or any other items that may come in contact with the body, in case widow spiders are residing in them.
Since recluse bites commonly take place indoors, measures can be taken in the home to lessen the chance of an exposure. First, the home should be adequately sealed to prevent spiders from entering. This includes adequate insulation and sealing around doors, windows, attics, and crawl spaces. Vacuuming under furniture and clearing spider webs with a broom or vacuum is also helpful. Household insecticides may be used to kill and repel household spiders.7
In the case of physical contact with either type of spider, it is recommended that no attempt be made to smash it while it sits on a person’s body. This could cause a reflex injection of venom by the spider’s fangs. Instead, the spider should be removed by a quick flick of the finger.7
Pharmacist Involvement
Pharmacists who practice in areas where these types of spiders are found should become familiar with prevention and treatment recommendations. Pharmacists can give advice about prevention and treatment and reassure patients that bites rarely result in serious injury. Pharmacists can also advise patients to check with their physicians as to the date of their last tetanus booster. Finally, if a patient is being treated after an exposure, pharmacists can provide appropriate counseling on prescribed or administered medications such as antihistamines (e.g., drowsiness, dizziness, avoidance of alcohol) and analgesics (e.g., sedation, dizziness, constipation).
Conclusion
Despite being a source of fear for many people, the only clinically relevant spider bites in the U.S. are from two genera of spiders: widow spiders and recluse spiders. While these bites are rarely fatal, both types contain venom that can lead to local and systemic effects. Widow spider venom acts on neurons to cause a sizable neurotransmitter release, resulting in powerful and painful muscle cramping. Recluse spiders cause an increase in immune-system signaling, resulting in necrosis and ulceration of the skin.
Spider bites can be managed nonpharmacologically and/or pharmacologically. Early wound care, such as applying ice and cleansing the wound, can help relieve pain and prevent infection. Pharmacologic therapy is aimed mainly at symptom relief. Oral and parenteral analgesics may be used to relieve severe pain, antihistamines may be used to relieve itching, and benzodiazepines may be used to relieve muscles spasms from widow bites. Currently, an antivenin is available for widow spider envenomation, but no such drug is approved for recluse spider envenomation.
Preventive measures are primarily aimed at putting physical barriers between the spider and a potential bite victim. Wearing long-sleeved clothing and clearing yard debris can help prevent widow bites, and properly insulating homes and sealing doors and windows can prevent household recluse spider bites. Chemical barriers such as insecticides and insect repellents containing DEET can also deter spider bites. Ultimately, currently available prevention and treatment measures can render these potentially clinically significant spider bites insignificant.
REFERENCES
1. Juckett G. Anthropod bites. Am Fam Physician. 2013;88:841-847.
2. CDC. Venomous spiders. www.cdc.gov/niosh/topics/spiders/. Accessed June 10, 2016.
3. Muslimin M, Wilson JJ, Ghazali AR, et al. First report of brown widow spider sightings in Peninsular Malaysia and notes on its global distribution. J Venom Anim Toxins Incl Trop Dis. 2015;21:11.
4. Offerman SR, Daubert GP, Clark RF. The treatment of black widow spider envenomation with antivenin Latrodectus mactans: a case series. Perm J. 2011;15:76-81.
5. Antoniou GN, Iliopoulos D, Kalkouni R, et al. Latrodectus envenomation in Greece. Perm J. 2014;18:e155-e158.
6. Gertsch WJ, Ennik F. The spider genus Loxosceles in North America, Central America, and the West Indies (Araneae, Loxoscelidae). Bull AMNH. 1983;175:article 3. http://digitallibrary.amnh.org/handle/2246/981. Accessed June 26, 2017.
7. Diaz JH, LeBlanc KE. Common spider bites. Am Fam Physician. 2007;75:869-873.
8. Vetter RS, Cushing PE, Crawford RL, Royce LA. Diagnoses of brown recluse spider bites (loxoscelism) greatly outnumber actual verifications of the spider in four western American states. Toxicon. 2003;42:413-418.
9. Ushkaryov YA, Volynski KE, Ashton AC. The multiple actions of black widow spider toxins and their selective use in neurosecretion studies. Toxicon. 2004;43:527-542.
10. Khvotchev M, Südhof TC. Alpha-latrotoxin triggers transmitter release via direct insertion into the presynaptic plasma membrane. EMBO J. 2000;19:3250-3262.
11. Corrèa MA, Okamoto CK, Gonçalves de Andrade RM, et al. Sphingomyelinase D from Loxosceles laeta venom induces the expression of MMP7 in human keratinocytes: contribution to dermonecrosis. PLoS One. 2016;11:e0153090.
12. Tambourgi DV, Paixão-Cavalcante D, Gonçalves de Andrade RM, et al. Loxosceles sphingomyelinase induces complement-dependent dermonecrosis, neutrophil infiltration, and endogenous gelatinase expression. J Invest Dermatol. 2005;124:725-731.
13. Cacy J, Mold JW. The clinical characteristics of brown recluse spider bites treated by family physicians: an OKPRN study. Oklahoma Physicians Research Network. J Fam Pract. 1999;48:536-542.
14. Rees RS, Altenbern DP, Lynch JB, King LE Jr. Brown recluse spider bites. A comparison of early surgical excision versus dapsone and delayed surgical excision. Ann Surg. 1985;202:659-663.
15. Clark RF, Wethern-Kestner S, Vance MV, Gerkin R. Clinical presentation and treatment of black widow spider envenomation: a review of 163 cases. Ann Emerg Med. 1992;21:782-787.
16. Antivenin (Latrodectus mactans). Clinical Pharmacology [subscription database]. Tampa, FL: Elsevier Gold Standard; 2017.
17. Phillips S, Kohn M, Baker D, et al. Therapy of brown spider envenomation: a controlled trial of hyperbaric oxygen, dapsone, and cyproheptadine. Ann Emerg Med. 1995;5:363-368.
18. Lowry BP, Bradfield JF, Carroll RG, et al. A controlled trial of topical nitroglycerin in a New Zealand white rabbit model of brown recluse spider envenomation. Ann Emerg Med. 2001;7:161-165.
19. Gehrie EA, Nian H, Young PP. Brown recluse spider bite mediated hemolysis: clinical features, a possible role for complement inhibitor therapy, and reduced RBC surface glycophorin A as a potential biomarker of venom exposure. PLoS One. 2013;8:e76558.
20. Carlton PK Jr. Brown recluse spider bite? Consider this uniquely conservative treatment. J Fam Pract. 2009;58:e1-e6.
21. Carrel JE. Population dynamics of the red widow spider (Araneae: Theridiidae). Fla Entomol. 2001;84:385-390.
To comment on this article, contact rdavidson@uspharmacist.com.





