US Pharm. 2022;47(5):15-16.
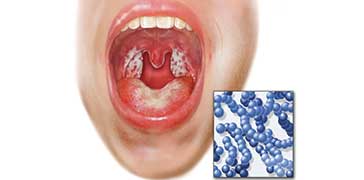
Bacterial Throat Infection
Pharyngitis is an inflammation of the pharynx, the area in the back of the throat. This inflammation causes the symptom of a sore throat. Although most infectious causes of sore throat are due to viruses, about 5% to 10% of pharyngitis cases result from a bacterial infection. Strep throat describes these throat infections since the bacteria most often responsible for bacterial pharyngitis are a strain of Streptococcus bacteria. Strep throat is most common in children aged 3 to 15 years, but it can occur at any age. Strep throat spreads easily and quickly from person to person in close-contact settings, such as schools, households, or day-care centers.
Testing Confirms Presence of Bacteria
Classic symptoms of strep throat include a painful sore throat, difficulty swallowing, fever, swollen neck glands, nausea, and headache. Upon examination, the throat appears red, often with white or yellow dots or streaks, tiny red dots on the upper palate, and swollen tonsils. Sore throats accompanied by cold or flu-like symptoms, such as nasal congestion and cough, are typically caused by a virus, and antibiotics are not effective to kill viruses. To avoid the unnecessary use of antibiotics and development of resistance, the diagnosis of a bacterial infection is essential before prescribing antibiotics. Since symptoms alone cannot definitively diagnose strep throat caused by bacteria, a rapid strep test detects the presence of a bacterial infection using a swab of the throat, followed by a culture if the rapid test is negative.
Most Infections Respond Quickly to Antibiotics
Antibiotics are the appropriate treatment for strep throat since they stop the further spread of bacteria, reduce the risk of spreading the infection to other areas of the body, and help prevent serious complications. There are many antibiotics used in the treatment of strep throat. Most commonly used are penicillin or amoxicillin (Amoxil). Other antibiotics used to treat are azithromycin (Zithromax, Z-Pak), cephalosporins, clarithromycin, and clindamycin. Side effects from antibiotics are generally mild and include stomachache, nausea, vomiting, and diarrhea. Factors to consider in the choice of antibiotic include the sensitivity of the bacteria to the antibiotic, patient allergies, dosing, taste, and cost. Seek emergency care immediately if wheezing, trouble breathing, rash, or fast heartbeat develops after antibiotic use. These symptoms can indicate an allergic reaction.
Acetaminophen or ibuprofen is appropriate to treat a fever, but aspirin should not be used in children and teens due to the risk of Reye’s syndrome. Nonprescription lozenges and sprays may help soothe a sore throat, and saltwater gargles are effective in reducing sore throat pain.
Although unusual, an untreated strep throat can lead to a sinus or ear infection, abscess of the tonsils, scarlet fever, or more serious complications, such as kidney disease (glomerulonephritis) or heart disease (rheumatic fever). After 24 hours of antibiotic therapy, patients with strep throat are no longer considered contagious and can return to school or work if they have no fever. Most cases of strep throat respond quickly to antibiotic therapy, but patients must finish the entire course of medication to avoid the bacteria from returning. If a strep throat returns after appropriate treatment, the source of Streptococcus may be a close contact (who may or may not have symptoms) or an ineffective antibiotic.
Stopping the Spread of Strep Infection
Since Streptococcus bacteria are highly contagious through saliva and nasal secretions, prevention of the spread of strep is similar to measures used against viral cold or influenza. This includes hand washing and covering the mouth and nose when coughing or sneezing. Patients should not return to school, day care, or work until they are no longer contagious and have no fever, usually 24 to 48 hours after beginning antibiotics. Streptococcus bacteria can also remain alive on objects such as a toothbrush for several days, so replacing a toothbrush after 24 to 48 hours of antibiotic therapy and thoroughly cleaning orthodontic retainers every day can prevent patients from reinfecting themselves.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





