US Pharm.
2008;33(9):19-23.
Contraceptive choices
currently available in the United States provide safe, reliable, effective,
and affordable birth control for virtually any patient. Products come in a
variety of forms--tablet, patch, injection, implant, vaginal, and intrauterine.
Current oral contraceptive products also contain novel progestins that have
altered the scope of benefits and adverse effects.
The availability of new,
effective contraceptive products in the last decade has not generated a
significant decrease in the rate of unintended pregnancy. About half of all
pregnancies in the U.S. are unintended, and more than one in five U.S.
pregnancies ends in abortion.1 A study of more than 10,000 women
who requested an abortion found that 46% had not used a contraceptive method
during the month they conceived.2
The number-one method of
contraception in the U.S. is sterilization.3 Many women who opt for
sterilization before the age of 30 later express regret and report choosing
sterilization because they didn't know that equally effective reversible
options exist.4 Combination oral contraceptives (COCs) are the most
commonly used reversible form of birth control in the U.S.3 By the
third month, the typical user misses three or more pills each cycle.5
These data suggest that the contraceptive needs of women are currently unmet (TABLE
1). Health care providers (HCPs) must be knowledgeable about recent
advances in birth control methods and able to discuss their pros and
cons--including efficacy, adverse effects, and compliance issues--with
individual patients.

Recent contraceptive advances
discussed in this review include extended-cycle COCs, drospirenone-containing
products, the chewable contraceptive pill, and emergency contraceptive
options. Concerns about the Ortho Evra transdermal patch and
desogestrel-containing products also are discussed.
Extended-Cycle Oral
Contraceptives
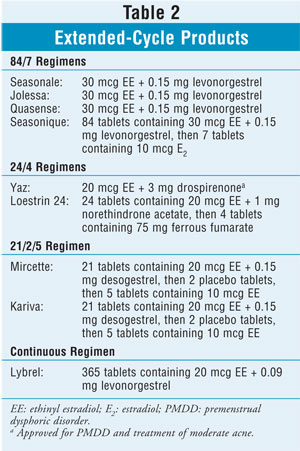
Extended-cycle
products differ from traditional 21/7 COCs by decreasing or eliminating the
hormone-free interval (HFI). A variety of dosing schedules are available (TABLE
2). Consecutive days of hormone therapy may extend to 84 or 365 days. In
add-back regimens, the HFI is shortened to zero, two, or four days instead of
the typical seven-day interval. The remaining days supply a lower dose of
hormone than that given during the rest of the cycle.
Reasons for switching to an
extended-cycle product include the typical menstrual symptoms experienced
during the HFI; improving efficacy in women who forget to restart the pill;
and patient preference to decrease the frequency of menstrual-like bleeding.
For a number of years, prescribers have utilized continuous administration of
monophasic pills to simulate an extended-cycle product. However, patients
generally incur additional financial expense with this dosing regimen because
insurance companies generally pay for only 13 cycles per year.6
Women with dysmenorrhea,
premenstrual syndrome, premenstrual dysphoric disorder, or endometriosis prior
to starting COCs typically experience exacerbations of these symptoms during
the HFI. Decreasing or discontinuing the HFI is likely to reduce or eliminate
breast tenderness, headache, bloating, cramping, hypermenorrhea, and the
psychological symptoms typical of hormone withdrawal. Patients also experience
less menstrual-blood loss with extended-cycle products, thereby decreasing the
risk of iron-deficiency anemia. An additional benefit of extended-cycle
products may be improved efficacy. A randomized clinical trial found that
continuous COC regimens were more effective at preventing follicular
development and breakthrough ovulation during the HFI.6 These
issues are a concern, particularly in patients who have difficulty adhering to
the dosing schedule, as low-dose products (20–30 mcg ethinyl estradiol) are
the norm.7
Extended-cycle products are
likely to cause unscheduled bleeding or spotting during active hormone
therapy, most commonly during the first few months of therapy. The bleeding
and spotting typically improve after several cycles, however. Patients must
weigh the convenience of having fewer cycles of scheduled bleeding per year
against the possibility of unscheduled bleeding or spotting during the initial
stage of therapy.8
Studies have compared
extended-cycle products with traditional 21/7 products to determine whether
patients are more compliant with continuous regimens of a COC. The Coraliance
study and many other trials have concluded that extended-cycle products
promote compliance and efficacy because patients don't forget to restart the
pill after a week-long HFI.9
Patients and HCPs have
expressed concern that decreasing or eliminating the HFI may be unhealthy and unnatural.
Continuous regimens expose women to two additional months of hormone each year
and increase lifetime exposure to estrogen and progestin. Concerns raised by
HCPs and patients include unforeseen adverse effects and long-term health
problems like endometrial hyperplasia, thrombosis, breast cancer, and future
fertility.10 A definitive answer will not be available until
long-term studies of extended-cycle products are completed. To date, no
studies supporting these concerns have been published.
The Association of
Reproductive Health Professionals (ARHP) commissioned a survey to determine
women's views about menstrual cycling and the use of hormonal contraceptives.
Almost one-half of survey participants said that they would choose to never
have a period, and approximately one-quarter said that they would choose to
continue to have monthly cycles.6 Another ARHP study found that
women would choose extended-cycle products if they were safe, did not affect
future fertility, and did not increase adverse effects; cost was also a factor.10
In the same study, 44% of HCPs believed that menstrual suppression is a good
idea and 52% prescribed oral contraceptives for that reason.10
Among patients and HCPs (7%) who believed that menstruation is physiologically
necessary, reasons cited included the importance of confirming that pregnancy
did not occur during the previous cycle and the beliefs that menstruation is a
natural state and withdrawal bleeding is necessary to cleanse the system.10
Proponents of extended-cycle
contraception note that modern women experience about 450 cycles in their
lifetime, compared with only 160 cycles for the pre–Industrial Revolution
woman.11 The increased number of cycles for modern women is due to
multiple factors, including earlier menarche, later menopause, fewer
pregnancies, and less breast-feeding.11 Economically speaking,
eliminating menstrual disorders may improve women's work productivity and
decrease health care costs. Data collected from 1984 through 1992 found that
menstrual disorders were the most commonly reported gynecologic condition.12
More than 75% of women studied had consulted a doctor about this
condition, and nearly 30% had spent one or more days in bed in the previous
year.12 A 2002 study concluded that menstrual bleeding has a
significant economic impact for working women, with an estimated annual cost
of $1,692 per woman in the workplace.13
Desogestrel-Containing Oral
Contraceptives
Desogestrel is a
third-generation progestin that is found in a number of COCs, including
Cyclessa, Ortho-Cept, Mircette, and Desogen. The third-generation products
were developed during the 1980s to decrease the androgenic effects, including
hirsutism and acne, commonly seen with earlier generations of oral
contraceptives. Two meta-analyses published in 2001 concluded that
desogestrel-containing oral contraceptives increase the risk of
thromboembolism by a factor of 1.7 over products that contain levonorgestrel.14,15
The FDA requires manufacturers
of desogestrel-containing products to include a statement in the Warnings
section of COC labeling that these products are associated with a two-fold
increase in the risk of venous thromboembolism. According to the FDA, patients
at increased risk for thromboembolism should consider switching to a
second-generation product.16 The Public Citizen's Health Research
Group (PCHRG) filed a petition with the FDA in February 2007 to remove
desogestrel because of the increased risk of developing blood clots.17
The petition claims that the third-generation products confer no clear
advantage over older oral contraceptives that is sufficient to warrant the
risks.17
Drospirenone-Containing
Oral Contraceptives
COCs that contain
the antimineralocorticoid drospirenone (Yasmin, Yaz; 3 mg drospirenone) as the
progestin component may decrease the bloating and water retention that
commonly occur with COC use. Drospirenone may cause potassium retention,
however, leading to hyperkalemia. While this is not likely to be a problem in
most patients, those who are concurrently taking potassium-sparing drugs,
including nonsteroidal anti-inflammatory drugs, diuretics,
angiotensin-converting enzyme inhibitors, angiotensin II agonists, and
potassium chloride, are at increased risk for hyperkalemia.18 A
2007 study found that 17.6% of women taking a drospirenone-containing product
were concurrently taking another potassium-sparing drug; 40% of those aged 35
years and older were taking an interacting combination.18 In a
related study, only 40% of patients who received an interacting combination of
drospirenone with a potassium-sparing drug were monitored for hyperkalemia as
recommended by product labeling; reasons for noncompliance included physician
disagreement with the recommendation, patient factors, and health-plan
barriers to testing.19 Pharmacists can monitor for this interaction
and educate patients to help them overcome barriers to having their potassium
levels monitored.
Chewable Oral Contraceptive
Femcon Fe contains
35 mcg ethinyl estradiol and 0.4 mg norethindrone in a spearmint-flavored pill
that can be swallowed or chewed. The tablet should be followed immediately by
a full 8 oz. of liquid. The proposed advantage of this product is ease of
administration.20 The seven brown tablets in the HFI contain 75 mg
ferrous fumarate.
Use of COCs in Older Women
Perimenopausal women commonly
experience hot flashes and dysfunctional uterine bleeding. Hormone replacement
therapy can treat vasomotor and menstrual symptoms, but does not prevent
ovulation. A patient taking COCs who experiences hot flashes during the HFI
may be switched to an extended-cycle product. The use of COCs in older women
confers both effective birth control and noncontraceptive benefits like
increased bone mineral density and reduced risk of ovarian and endometrial
cancer.21
Despite the benefits of COC
use in older women, significant risks are associated with hormone use. Women
over the age of 39 who take COCs have four times the risk of venous
thromboembolism (VTE) compared with adolescents. The incidence in these women
is 100 cases per 100,000 woman-years; obesity increases the risk.21
COC users with a history of hypertension may have an increased risk of heart
attack and stroke, and hypertension and smoking act synergistically to
increase the risk of stroke and heart attack in COC users.22
Therefore, women over 35 years of age should not take estrogen-containing
contraceptives if they smoke or have diabetes, migraines, or hypertension. COC
use does not appear to increase the risk of stroke or heart attack in healthy
nonsmokers over age 35; oral contraceptives can be continued in these women
until age 55.22 Depot medroxyprogesterone acetate or the
levonorgestrel intrauterine device (IUD) may be appropriate for women in whom
COCs are contraindicated.
Transdermal Contraceptive
Patch
The Ortho Evra
contraceptive patch, a matrix system containing 6 mg norelgestromin and 0.75
mg ethinyl estradiol, was approved in 2001. Proposed advantages include
improved adherence to the regimen and better efficacy if errors of up to two
days are made in dosing. This dosing method avoids first-pass metabolism of
hormones, gastrointestinal enzymatic degradation, and peaks and troughs in
drug levels. It is easy to confirm the presence of the patch, which reassures
the user of continued protection. Disadvantages are application-site reactions
and decreased efficacy in patients weighing more than 198 lb.23
The FDA revised the labeling
for Ortho Evra in September 2006 and again in January 2008, based on results
of an epidemiologic study that found that users of the birth control patch
were exposed to 60% more estrogen than users of a typical COC containing 35
mcg estrogen and were twice as likely to develop blood clots.24,25
A 2007 postmarketing study of women aged 15 to 44 years confirmed earlier
studies that women in this age group were at greater risk for VTE.26
Despite the increased overall exposure to estrogen, the peak concentration of
estrogen to which women are exposed is about 25% less with Ortho Evra than
with typical COCs.24
The FDA recommends that women
with risk factors for VTE (TABLE 3) discuss the use of the Ortho Evra
patch with their HCP and consider using nonhormonal contraceptive methods
instead. Women who are immobilized due to surgery or injury should discontinue
the patch while they are recovering from the event.27

PCHRG filed a petition with
the FDA in May 2008, requesting withdrawal of Ortho Evra from the market due
to safety concerns based on the abovementioned studies.28 PCHRG
suggested that the FDA phase out sale of the patch over six months, allowing
existing users to obtain refills while switching to another contraceptive.28
Use of the patch has decreased in recent years, most likely due to the reports
of risk of thromboembolism. Last year, about 2.7 million prescriptions were
written for the patch, down from more than 9.9 million prescriptions in 2004,
according to data cited by the petition.28
Emergency Contraception
In August 2006,
Plan B was approved for OTC sale to women aged 18 years and older. Plan B
contains two tablets of 0.75 mg levonorgestrel. The product labeling states
that the tablets are to be taken 12 hours apart starting within 72 hours of
unprotected sex. Recent findings suggest that the regimen is equally effective
if the tablets are taken as one dose.29 Additional evidence
suggests that Plan B may be effective taken up to five days after intercourse;
however, this use is not approved.30 Women may purchase Plan B to
keep for future use; this concept, called advance provision, is recommended by
many HCPs because it eliminates delays in starting therapy. Concerns that
widespread availability of Plan B would increase sexual risk-taking behavior
have not been borne out in clinical studies.27
COCs may be used for emergency
contraception also. Two to five tablets of a COC that contains levonorgestrel
as the progestin are used in the Yuzpe regimen, which comprises 100 mcg to 120
mcg ethinyl estradiol combined with 0.5 mg to 0.6 mg levonorgestrel. Plan B is
preferred to the Yuzpe regimen because it has fewer adverse effects,
particularly nausea and vomiting, that may decrease the regimen's
effectiveness.32
The copper IUD can be used in
women who want emergency as well as regular contraception. The proposed
mechanism of action is to impair fertilization, alter sperm motility, and
impede implantation.32 The IUD may be inserted up to five days
after unprotected sex. IUD use is contraindicated in cases of sexual assault
where there is a high risk of sexually transmitted disease.32
Mifepristone, used in the U.S.
as an abortifacient since 2000, has been examined for emergency contraception.
It has multiple mechanisms of action, depending on when in the menstrual cycle
it is administered. A single dose of 10 mg to 50 mg has been shown to be
highly effective for preventing pregnancy.32 The dose is effective
up to five days after unprotected sex. Impediments to the drug's use are that
the only dose available in the U.S. is a 200-mg tablet; prescriber
availability is limited to physicians who have registered with the FDA to
obtain access; and the drug is likely to delay the onset of menstrual bleeding
versus other methods of emergency contraception.29
Summary
A number of new
contraceptive methods have been introduced in the U.S. These methods are safe
and effective for contraception. They also decrease adverse effects and confer
some noncontraceptive benefits.
REFERENCES
1. Finer LB,
Henshaw SK. Disparities in rates of unintended pregnancy in the United States,
1994 and 2001. Perspect Sex Reprod Health. 2006;38:90-96.
2. Jones RK, Darroch
JE, Henshaw SK. Contraceptive use among U.S. women having abortions in
2000-2001. Perspect Sex Reprod Health. 2002;34:294-303.
3. Chandra A, Martinez
GM, Mosher WD, et al. Fertility, family planning, and reproductive health of
U.S. women:data from the 2002 National Survey of Family Growth. Vital
Health Stat 23. 2005;25:1-160.
4. Hillis SD,
Marchbanks PA, Tylor LR, Peterson HB. Poststerilization regret: findings from
the United States Collaborative Review of Sterilization. Obstet Gynecol.
1999;93:889-895.
5. Potter L, Oakley D,
de Leon-Wong E, Cañamar R. Measuring compliance among oral contraceptive
users. Fam Plann Perspect. 1996;28:154-158.
6. AHRPClinical
Proceedings. Extended and Continuous Use of Contraceptives to Reduce
Menstruation. Washington, DC: Association of Reproductive Health
Professionals; 2004.
7. Birtch RL,
Olatunbosun OA, Pierson RA. Ovarian follicular dynamics during conventional
vs. continuous oral contraceptive use. Contraception. 2006;73:235-243.
8. Portman D. Altering
the hormone-free interval with extend ed-cycle contraception. Female
Patient. 2006 (suppl):1-4.
9. Aubeny E, Buhler M,
Colau JC, et al. The Coraliance study: non-compliant behavior. Results after a
6-month follow-up of patients on oral contraceptives. Eur J Contracept
Reprod Health Care. 2004;9:267-277.
10. Andrist LC, Arias
RD, Nucatola D, et al. Women's and providers' attitudes toward menstrual
suppression with extend ed use of oral contraceptives. Contraception.
2004;70:359-363.
11. Eaton SB, Pike MC,
Short RV, et al. Women's reproductive cancers in evolutionary context. Q
Rev Biol.1994;69:353-367.
12. Kjerulff KH,
Erickson BA, Langenberg PW. Chronic gynecological conditions reported by US
women: findings from the National Health Interview Survey, 1984 to 1992. Am
J Public Health. 1996;86:195-199.
13. Côté I, Jacobs P,
Cumming D. Work loss associated with increased menstrual loss in the United
States. Obstet Gynecol. 2002;100:683-687.
14. Hennessy S, Berlin
JA, Kinman JL, et al. Risk of venous thromboembolism from oral contraceptives
containing gestodene and desogestrel versus levonorgestrel: a meta-analysis
and formal sensitivity analysis. Contraception. 2001;64:125-133.
15. Kemmeren JM, Algra
A, Grobbee DE. Third generation oral contraceptives and risk of venous
thrombosis: meta-analysis. BMJ. 2001;323:131-134.
16. Desogen
(desogestrel and ethinyl estradiol) package insert. Roseland, NJ: Organon USA
Inc; August 2007.
17. Public Citizen
Health Research Group. Petition to the FDA to Ban Third Generation Oral
Contraceptives Containing Desogestrel due to Increased Risk of Venous
Thrombosis (HRG Publication #1799).
www.citizen.org/publications/release.cfm?ID=7503. Accessed May 20, 2008.
18. McAdams M, Staffa
JA, Dal Pan GJ. The concomitant prescribing of ethinyl estradiol/drospirenone
and potentially interacting drugs. Contraception. 2007;76:278-281.
19. Mona Eng P, Seeger
JD, Loughlin J, et al. Serum potassium monitoring for users of ethinyl
estradiol/drospirenone taking medications predisposing to hyperkalemia:
physician compliance and survey of knowledge and attitudes. Contraception.
2007;75:101-107.
20. Femcon Fe site.
More to chew on. www.femconfe.com/more.jsp. Accessed May 15, 2008.
21. Kaunitz AM.
Clinical practice. Hormonal contraception in women of older reproductive age. NEJM.
2008;358:1262-1270.
22. ACOG practice
bulletin. No. 73: use of hormonal contraception in women with coexisting
medical conditions. Obstet Gynecol. 2006;107:1453-1472.
23. Zieman M,
Guillebaud J, Weisberg E, et al. Contraceptive efficacy and cycle control with
the Ortho Evra/Evra transdermal system: the analysis of pooled data. Fertil
Steril. 2002;77(suppl 2):S13-S18.
24. Ortho Evra
(norelgestromin/ethinyl estradiol transdermal system) package insert. Raritan,
NJ: Ortho-McNeil-Janssen Pharmaceuticals, Inc; March 2008.
25. Cole JA, Norman H,
Doherty M, Walker AM. Venous thromboembolism, myocardial infarction, and
stroke among transdermal contraceptive system users. Obstet Gynecol.
2007;109:339-346.
26. ClinicalTrials.gov.
Relative risks for non-fatal venous thromboembolism, ischemic stroke and
myocardial infarction in users of ORTHO EVRA (norelgestromin and ethinyl
estradiol contraceptive patch) compared to levonorgestrel-containing oral
contraceptives. www.clinicaltrials.gov/ct2/show/NCT00511784. Accessed July 31,
2008.
27. FDA News. FDA
approves update to label on birth control patch.
www.fda.gov/bbs/topics/NEWS/2008/NEW01781.html. Accessed May 15, 2008.
28. Public Citizen
Health Research Group. Petition to the FDA to Ban Ortho-Evra (HRG Publication
#1840). www.citizen.org/publications/release.cfm?ID=7582. Accessed May 15,
2008.
29. von Hertzen H,
Piaggio G, Ding J, et al. Low dose mifepristone and two regimens of
levonorgestrel for emergency contraception: a WHO multicentre randomised
trial. Lancet. 2002;360:1803-1810.
30. Rodrigues I, Grou
F, Joly J. Effectiveness of emergency contraceptive pills between 72 and 120
hours after unprotected sexual intercourse. Am J Obstet Gynecol.
2001;184:531-537.
31. Walsh TL, Frezieres
RG. Patterns of emergency contraception use by age and ethnicity from a
randomized trial comparing advance provision and information only. Contraception.
2006;74:110-117.
32. LaValleur J.
Emergency contraception. Obstet Gynecol Clin North Am. 2000;27:817-839.
33. Jain J, Jakimiuk
AJ, Bode FR, et al. Contraceptive efficacy and safety of DMPA-SC. Contraception.
2004;70:269-275.
To comment on this article, contact
rdavidson@jobson.com.





