US Pharm. 2022;47(11):HS-11-HS-16.
ABSTRACT: Individuals with diabetes are at a heightened risk for development of infections, including skin/soft tissue infections, urinary tract infections, and lower respiratory tract infections, as well as more complex and rare infections. Research has established that among those with diabetes, especially those with poorly controlled disease, there is a greater risk for the development of infections and related complications due to a complex interplay between various factors, which can be classified as systemic and local host factors and/or specific pathogens. Findings have revealed that infections in those with diabetes are often correlated with increased rates of hospitalization, durations of stay, and complications. Pharmacists are well poised to educate patients about the augmented risk for infection. They can also provide patients with pertinent information regarding measures to reduce or prevent these infections, including clinical guidelines that recommend eligible individuals with diabetes obtain pneumonia, influenza, and COVID-19 vaccines. Pharmacists can also emphasize the importance of adherence to therapy and nutritional plans and the impact of tight glycemic control to lessen their risks.
Diabetes continues to be a growing public health issue that is correlated with substantial morbidity and mortality. Uncontrolled diabetes is also associated with numerous health and economic burdens for affected patients and the healthcare system. As a chronic condition, diabetes is associated with both macrovascular and microvascular complications. While the precise extent is largely unknown, research has established that individuals with diabetes, particularly those with poorly controlled diabetes, are more susceptible and/or at heightened risk for development of infection when compared to the general patient population.1-4
As integral members of the healthcare team, it is imperative that pharmacists are knowledgeable about the augmented susceptibility for infections in the diabetic patient population and understand their roles as clinician and patient educator in making clinical recommendations about possible therapies. Pharmacists can also be instrumental in educating patients about the expanded risk for infections, measures to decrease or prevent infections, and the importance of maintaining tight glycemic control to decrease their risk of diabetes-related complications.
Diabetes and Increased Risk of Infections
Various publications have indicated hyperglycemia and lack of and/or poorly controlled glucose are believed to trigger dysfunction of the immune response via numerous pathways that are correlated with both chronic inflammatory processes and diabetes mellitus–related susceptibility/vulnerability to infections.1-7 In turn, these mechanisms result in an impairment or failure of the immune system to thwart and/or reduce the transmission of invading pathogens in those with diabetes, leaving diabetics more susceptible to the risk of infection.1,5 Research reveals that the elevated rates of infections among individuals with diabetes is due to impairment of the immune function, particularly of the innate immune system and dysfunction of neutrophils, as well as flaws in the adaptive immune system.5-7 Clinical evidence also indicates that waning of immune defenses comprising both congenital and secondary to metabolic disturbances, as well as to microangiopathy and neuropathy, contributes to the augmented susceptibility to certain infections in those with diabetes.5,7 Some studies indicate that in those with diabetes, immune dysfunction may be mediated via compromised migration, phagocytosis, intracellular killing, and chemotaxis.5-11 Other studies note that flaws in the innate response transpire from dysfunction of granulocytes, monocyte/macrophages, dendritic cells, natural killer cells, B cells, T cells, and cytokine signaling.5-11 Increased frequency and severity of bacterial infections in diabetes have been linked to weakened innate and adaptive immune responses within the hyperglycemic environment.10 Furthermore, those with diabetes are more likely to be hospitalized to treat and manage infections compared with those without diabetes.12 In addition, diabetes-related complications, such as neuropathy and vascular insufficiency, can also expand risk of infection.
Research indicates that vascular damage causes poor tissue perfusion, and damage and loss of sensations from neuropathy often result in unnoticed injuries and infections, which can turn into skin ulcers or other infections.1,5,7,13 Moreover, microvascular complications such as neuropathy also increase vulnerability within the skin barrier, which is the first line of defense in preventing many infections.13 Poor vascular flow to sites of infection can also negatively impact immune system function and slow or halt the healing process, which can result in exacerbation of infections or manifestation of secondary infections.13
Common Infections Among the Diabetic Patient Population
Numerous studies have reported that among diabetics, there is an augmented incidence of lower respiratory tract infections such as pulmonary tuberculosis and pneumonia, urinary tract infections (UTIs), asymptomatic bacteriuria (particularly in women), pyelonephritis, lower extremity infections including skin and soft tissue infections, renal and perinephric abscesses, surgical and/or nosocomial infections, deep subcutaneous tissue infections, and postoperative sternal wound infections.1,12-17 Moreover, not only are these types of infections prevalent within the diabetes patient population, but infections often progress more swiftly and can be severe in nature.1,12-17
In 2010, with regard to those with diabetes, 2.8% of hospital discharges were due to foot ulcers, while among those without diabetes with foot ulcers, the rates of discharge was only 0.6%.16 Studies also reveal that having an HbA1c higher than 6.5% is linked with an augmented risk of community-acquired and hospital-acquired bloodstream infection and sepsis.18,19 Epidemiologic studies suggest that individuals with diabetes are at elevated risk for complications, hospitalization, and death from influenza and pneumococcal disease, and recent findings indicate comparable outcomes with the COVID-19 virus.17 Among diabetics, the prevalence of acute bacterial skin and skin structure infections (ABSSSIs) is also linked with elevated rates of morbidity, complications, and rates of mortality and is considered to be a principal cause of morbidity and mortality in this patient population.20 Skin infections in diabetics may range from cellulitis to more severe and/or complicated infections that include diabetic foot infections, which may result in amputation and deep tissue infections.20 Studies indicate that an ABSSSI in a diabetic patient may exacerbate glycemic control, which in turn may also affect the resolution of the infection and/or contribute to a negative clinical outcome.20
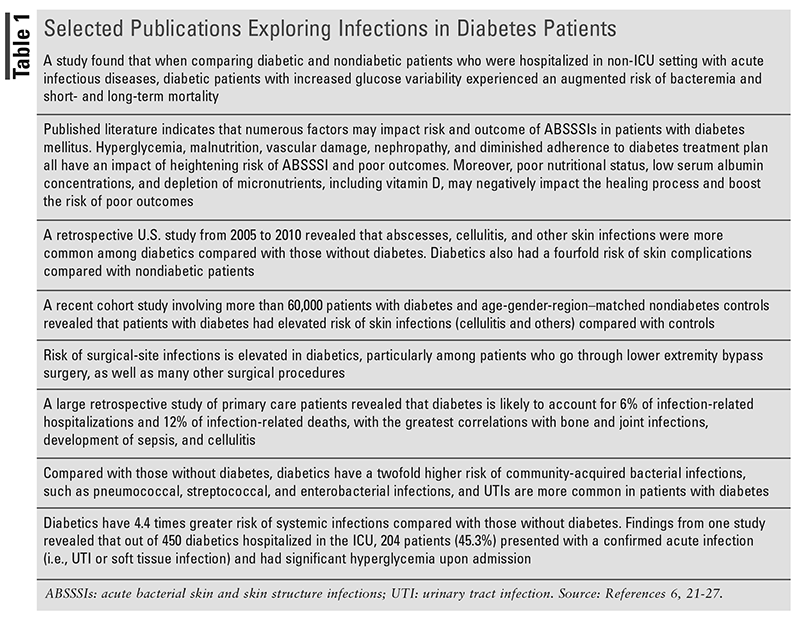
A summary of publications exploring infections and the diabetes patient population is shown in TABLE 1.6,21-27
Diabetes and COVID-19 Infections
Numerous studies have established that patients with diabetes, especially those with poorly controlled diabetes, were at augmented risk for severe COVID-19 infections, hospital admissions, and mortality.28 Studies have also revealed that uncontrolled glucose levels at admission and during hospitalization were associated with poor clinical outcomes in COVID-19 patients. Moreover, among COVID-19 patients with hyperglycemia, implementation of therapeutic strategies in conjunction with measures to achieve good glycemic control should be considered to diminish the risk of severe outcomes and mortality.29
Other Infections
Diabetics often have an increased risk for mucocutaneous fungal infections (e.g., oral and vaginal candidiasis) and bacterial foot infections (including osteomyelitis). Characteristically, these infections are worsened by diabetic neuropathy and lower extremity vascular insufficiency, and hyperglycemia is a well-documented risk factor for surgical-site infections.30
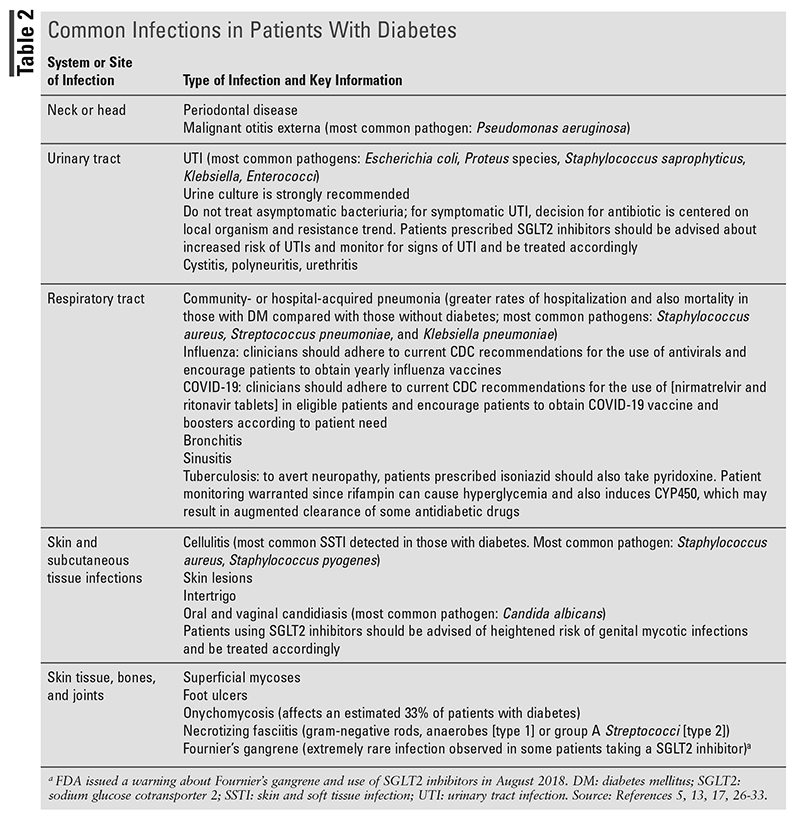
The literature also indicates that some serious infections that are rare and transpire almost entirely in the diabetic patient population include emphysematous pyelonephritis and emphysematous cholecystitis, malignant otitis externa, and rhinocerebral mucormycosis.17,31 These are sometimes referred to as signal infections.31 TABLE 2 describes examples of common infections in patients with diabetes.5,13,17,26-33
Treatment and Prevention Examples
According to the 2022 American Diabetes Association (ADA) Standards of Medical Care, the majority of diabetic foot infections are polymicrobial, with aerobic gram-positive cocci, Staphylococci, and Streptococci the most frequent causative pathogens.34 The ADA also notes that wounds without evidence of soft tissue or bone infection do not require antibiotic therapy.34 Empiric antibiotic therapy can be narrowly targeted at gram-positive cocci in many patients with acute infections. However, those at risk for infection with antibiotic-resistant organisms or with chronic, previously treated, or severe infections may warrant broader spectrum regimens and should be referred to specialized care centers. Additionally, the ADA notes that foot ulcers and wound care may necessitate medical care by a podiatrist, an orthopedic or vascular surgeon, or a rehabilitation specialist experienced in the management of individuals with diabetes.34
Since vaccinations have been proven safe and effective in thwarting the incidence and/or severity of certain infections, such as pneumonia, influenza, and COVID-19 infections, the ADA Standards of Medical Care also recommend and stress the significance of routine vaccinations according to age-appropriate recommendations, particularly in those with diabetes. These vaccines are effective in reducing and preventing morbidity, but they also diminish hospitalization rates.34
In 2019, the International Working Group on the Diabetic Foot published an update to its evidence-based guidelines on diabetic foot disease prevention and management.35 The updated guidelines indicate the following with regard to treatment: A diabetic foot infection should be treated with an antibiotic agent whose efficacy has been confirmed in a published randomized, controlled trial and that is tailored to patient need based on medical history and allergy history. Suggestions for the agents to consider when no contraindications are present include penicillins, cephalosporins, carbapenems, metronidazole (in combination with one or more other antibiotics), clindamycin, linezolid, daptomycin, fluoroquinolones, and vancomycin; tigecycline should not be considered.35
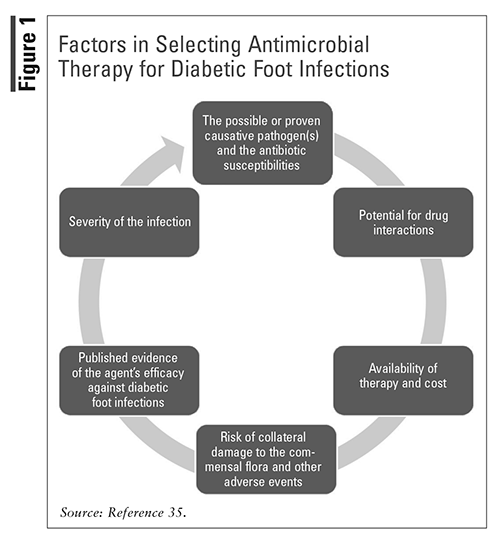
Factors that should be considered in the selection of antimicrobial therapy for the treatment of a diabetic foot infection are shown in FIGURE 1.35
In a recent systematic review and meta-analysis, researchers revealed that those with type 2 diabetes are more prone to experience resistant urinary tract and respiratory infections; however, more research is warranted.36 Health experts indicate that asymptomatic bacteriuria does not warrant the use of antimicrobial therapy, and if patient is symptomatic (uncomplicated cystitis/lower UTI), those with diabetes may warrant a longer course of antibiotic treatment.30,36
The Role of the Pharmacist
Due to their drug expertise, pharmacists can be instrumental in making clinical recommendations tailored to patient need, ensuring that antimicrobials are prescribed appropriately, and reminding patients to adhere to prescribed therapy to improve clinical outcomes. Findings from a recent study published in JAMA Network Open indicated that implementation of a pharmacist-led, multidisciplinary review of discharge planning for patients during transition of care from hospital to home setting with an antimicrobial prescription for an uncomplicated infection was linked with noticeably enhanced antimicrobial prescribing.37 In addition, following employment of the antimicrobial stewardship program, there was also a decrease in antimicrobial-associated harms (i.e., inappropriate, suboptimal, and/or unnecessary antimicrobial prescribing at hospital discharge).37 The authors of the study noted that their findings emphasize the vital role of pharmacists in enhancing the proper usage of antimicrobial therapy. They concluded that in their study, pharmacists were able to diminish superfluous and prolonged use of antibiotics in patients without infections and avoid the usage of antimicrobials that are excessively broad or targeted toward pathogens that are not susceptible to the antimicrobial, and pharmacists’ interventions resulted in easy conversion from IV to oral therapies for patients.37
During patient counseling, pharmacists can remind patients about the importance of adhering to the recommended treatment protocol, maintaining tight glycemic control to diminish diabetes-related complications, and the warning signs of an infection such as fever, wounds that will not heal, swelling or erythematous appearance around cuts, scrapes and scratches, etc. Pharmacists can also advise about when to contact their primary healthcare provider and suggest measures to decrease and/or prevent infections, such as daily skin care including cleansing, moisturizing, and meticulous diabetic foot care including inspection and toenail trimming; implementing measures for urinary hygiene to reduce or prevent UTIs; routine monitoring of blood glucose levels; and adherence to a diet plan and regular follow-up with primary healthcare providers.
It is also an excellent opportunity to remind patients about the value of routine immunizations, such as COVID-19, influenza, and pneumonia vaccines to eligible patients and their value in decreasing risk of serious infections and rates of mortality from these types of infections.
Conclusion
Since the risk of infection is often heightened in those with diabetes, especially in those undiagnosed or in those with poorly controlled diabetes, pharmacists are well positioned to provide patient education. This integral component of diabetes care can foster improved clinical outcomes and possibly prevent and/or reduce the incidence and complications often associated with infections.
REFERENCES
1. Berbudi A, Rahmadika N, Tjahjadi AI, Ruslami R. Type 2 diabetes and its impact on the immune system. Curr Diabetes Rev. 2020;16(5):442-449.
2. Abu-Ashour W, Twells LK, Valcour JE, Gamble JM. Diabetes and the occurrence of infection in primary care: a matched cohort study. BMC Infect Dis. 2018;18(1):67.
3. Korbel L, Spencer JD. Diabetes mellitus and infection: an evaluation of hospital utilization and management costs in the United States. J Diabetes Complications. 2015;29:192-195.
4. Mor A, Berencsi K, Nielsen JS, et al. Rates of community-based antibiotic prescriptions and hospital-treated infections in individuals with and without type 2 diabetes: a Danish nationwide cohort study, 2004-2012. Clin Infect Dis. 2016;63(4):501-511.
5. Toniolo A, Cassani G, Puggioni A, et al. The diabetes pandemic and associated infections: suggestions for clinical microbiology. Rev Med Microbiol. 2019;30(1):1-17.
6. Atamna A, Ayada G, Akirov A, et al. High blood glucose variability is associated with bacteremia and mortality in patients hospitalized with acute infection. QJM. 2019;112(2):101-106.
7. Lu ZH, Yu WL, Sun Y. Multiple immune function impairments in diabetic patients and their effects on COVID-19. World J Clin Cases. 2021 Aug 26;9(24):6969-6978.
8. Abu-Ashour W, Twells L, Valcour J, et al. The association between diabetes mellitus and incident infections: a systematic review and meta-analysis of observational studies. BMJ Open Diabetes Res Care. 2017;5(1):e000336.
9. Hodgson K, Morris J, Bridson T, et al. Immunological mechanisms contributing to the double burden of diabetes and intracellular bacterial infections. Immunology. 2015;144(2):171-85.
10. Frydrych LM, Bian G, O’Lone DE, et al. Obesity and type 2 diabetes mellitus drive immune dysfunction, infection development, and sepsis mortality. J Leukoc Biol. 2018;104(3):525-534.
11. Martins M, Boavida JM, Raposo et al. Diabetes hinders community-acquired pneumonia outcomes in hospitalized patients. BMJ Open Diabetes Res Care. 2016;4(1):e000181.
12. Shah BR, Hux JE. Quantifying the risk of infectious diseases for people with diabetes. Diabetes Care. 2003;26:510-513.
13. Zhou K, Lansang MC. Diabetes mellitus and Infections. In: Feingold KR, Anawalt B, Boyce A, et al, eds. South Dartmouth, MA: MDText.com, Inc.; 2021. www.ncbi.nlm.nih.gov/books/NBK569326/.
14. Nitzan O, Elias M, Chazan B, Saliba W. Urinary tract infections in patients with type 2 diabetes mellitus: review of prevalence, diagnosis, and management. Diabetes Metab Syndr Obes. 2015;8:129-136.
15. Jenkins TC, Knepper BC, Jason Moore S, et al. Comparison of the microbiology and antibiotic treatment among diabetic and nondiabetic patients hospitalized for cellulitis or cutaneous abscess. J Hosp Med. 2014;9(12):788-794.
16. Dryden M, Baguneid M, Eckmann C, et al. Pathophysiology and burden of infection in patients with diabetes mellitus and peripheral vascular disease: focus on skin and soft-tissue infections. Clin Microbiol Infect. 2015;21(Suppl 2:S27-S32).
17. Egede LE, Hull BJ, Williams JS. Infections associated with diabetes. In: Cowie CC, Casagrande SS, Menke A, et al, eds. Diabetes in America. 3rd ed. chap 30. Bethesda, MD: National Institute of Diabetes and Digestive and Kidney Diseases (US); 2018 Aug. www.ncbi.nlm.nih.gov/books/NBK567992/.
18. McKane CK, Marmarelis M, Mendu ML, et al. Diabetes mellitus and community-acquired bloodstream infections in the critically ill. J Crit Care. 2014;29:70-76.
19. Trevelin SC, Carlos D, Beretta M, et al. Diabetes mellitus and sepsis: a challenging association. Shock. 2017;47:276-287.
20. Falcone M, Meier JJ, Marini MG, et al. Diabetes and acute bacterial skin and skin structure infections. Diabetes Res Clin Pract. 2021;174:108732.
21. Zhang SS, Tang ZY, Fang P, et al. Nutritional status deteriorates as the severity of diabetic foot ulcers increases and independently associates with prognosis. Exp Ther Med. 2013;5(1):215-222.
22. Suaya JA, Eisenberg DF, Fang C, Miller LG. Skin and soft tissue infections and associated complications among commercially insured patients aged 0-64 years with and without diabetes in the U.S. PLoS One. 2013;8(4):e60057.
23. Kim EJ, Ha KH, Kim DJ, Choi YH. Diabetes and the risk of infection: a national cohort study. Diabetes Metab J. 2019;43(6):804-814.
24. Martin ET, Kaye KS, Knott C. Diabetes and risk of surgical site infection: a systematic review and meta-analysis. Infect Control Hosp Epidemiol. 2016;37(1):88-99.
25. Carey IM, Critchley JA, DeWilde S, et al. Risk of infection in type 1 and type 2 diabetes compared with the general population: a matched cohort study. Diabetes Care. 2018;41(3):513-521.
26. Nagendra L, Boro H, Mannar V. Bacterial Infections in Diabetes. In: Feingold KR, Anawalt B, Boyce A, et al, eds. South Dartmouth, MA: MDText.com, Inc. www.ncbi.nlm.nih.gov/books/NBK579762/.
27. Burekovic A, Dizdarevic-Bostandzic A, Godinjak A. Poorly regulated blood glucose in diabetic patients-predictor of acute infections. Med Arch. 2014;68(3):163-166.
28. Czupryniak L, Dicker D, Lehmann R, et al. The management of type 2 diabetes before, during and after Covid-19 infection: what is the evidence? Cardiovasc Diabetol. 2021;20:198. https://doi.org/10.1186/s12933-021-01389-1.
29. Jin S, Hu W. Severity of COVID-19 and treatment strategy for patient with diabetes. Front Endocrinol (Lausanne). 2021;12:602735.
|30. Brutsaert E. Complications of diabetes mellitus. Merck Manual for Health Care Professionals. Updated September 2020. www.merckmanuals.com/professional/endocrine-and-metabolic-disorders/diabetes-mellitus-and-disorders-of-carbohydrate-metabolism/complications-of-diabetes-mellitus#v29299409
31. Cooke F. Infections in people with diabetes. Complications of Diabetes. 2018. https://doi.org/10.1016/j.mpmed.2018.11.002.
32. Chávez-Reyes J, Escárcega-González CE, Chavira-Suárez E, et al. Susceptibility for some infectious diseases in patients with diabetes: the key role of glycemia. Front Public Health. 2021;9:559595.
|33. Casqueiro J, Casqueiro J, Alves C. Infections in patients with diabetes mellitus: a review of pathogenesis. Indian J Endocrinol Metab. 2012;16(Suppl 1):S27-S36.
34. American Diabetes Association Professional Practice Committee. Draznin B, Aroda VR, et al. Chap 12. Retinopathy, Neuropathy, and Foot Care: Standards of Medical Care in Diabetes-2022. Diabetes Care. 2022;45(Suppl 1):S185-S194.
35. Lipsky BA, Senneville E, Abbas ZG, et al. IWGDF guideline on the diagnosis and treatment of foot infection in persons with diabetes. International Working Group on the Diabetic Foot. https://iwgdfguidelines.org/wp-content/uploads/2019/05/05-IWGDF-infection-guideline-2019.pdf.
36. Carrillo-Larco RM, Anza-Ramírez C, Saal-Zapata G, et al. Type 2 diabetes mellitus and antibiotic-resistant infections: a systematic review and meta-analysis. J Epidemiol Community Health. 2022;76(1):75-84.
37. Mercuro NJ, Medler CJ, Kenney RM, et al. Pharmacist-driven transitions of care practice model for prescribing oral antimicrobials at hospital discharge. JAMA Netw Open. 2022;5(5):e2211331.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





