US Pharm. 2015;40(2):HS3-HS7.
ABSTRACT: Oral anticoagulants are commonly prescribed for the prevention and treatment of thromboembolic disorders. Coagulopathy is an inherent risk for all anticoagulants, and data regarding reversal of newer agents are sparse. Unlike warfarin, limited options currently exist for rapid reversal of novel oral anticoagulants (direct thrombin inhibitors, factor Xa inhibitors) and include fresh frozen plasma and prothrombin complex concentrates. While no true antidote is yet available, several promising agents are in development. As a result, healthcare providers, principally pharmacists, must be prepared to appropriately monitor and manage patients requiring reversal.
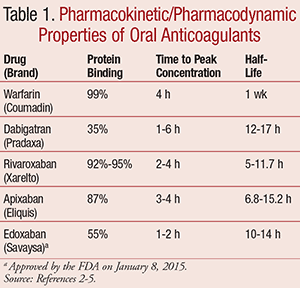
The widespread use of oral anticoagulants for various conditions has resulted in the necessity to have rapid-acting reversal agents in critical situations such as life-threatening bleeds or urgent surgical procedures. Warfarin, which inhibits vitamin K epoxide reductase, preventing the formation of vitamin K–dependent clotting factors (II, VII, IX, X), had previously been the only oral anticoagulant available.1 Newer agents, such as the direct thrombin inhibitor dabigatran and the factor Xa inhibitors (rivaroxaban, apixaban, edoxaban) have recently been introduced. These drugs work by interrupting the coagulation cascade and show similar efficacy to warfarin.1 As novel oral anticoagulants (NOACs) become increasingly popular, pharmacists should be cognizant of both monitoring and reversal strategies for them, which primarily stem from the pharmacokinetic and pharmacodynamic properties of each agent as outlined in TABLE 1.2-5
Nonemergent Management
In nonurgent cases, including planned procedures, reversal of anticoagulant agents can be achieved by withholding the medication.1 Anticoagulant interruption may suffice if reversal is desired in a few days to within a week.
With warfarin, the gradual diminishing effect on coagulation is dependent on hepatic function. If rapid reversal is necessary, interventions may be warranted. Phytonadione, exogenous vitamin K, is commonly used for rapid reversal of warfarin, with normalization of international normalized ratio (INR) typically seen within 24 hours.6 Phytonadione may be necessary for elevated INR or for patients exhibiting signs or symptoms of bleeding. Current guidelines state that no intervention is necessary for patients with an INR up to 10 and no evidence of bleeding. If INR is >10 with no evidence of bleeding, administering 2 to 2.5 mg of phytona-dione orally would be sufficient to reverse the effects of warfarin. If INR is >10 with clinically significant bleeding, IV phytonadione dosed at 5 to 10 mg is indicated, as it provides a quicker INR reduction compared to oral administration.6 Cautions to note with phytonadione use include anaphylaxis with IV administration and the potential for refractoriness to warfarin when warfarin is restarted.6
Withholding NOACs allows for a reversal that relies predominantly on renal clearance, as these newer agents lack specific antidotes. Current guidelines suggest the use of activated charcoal and dialysis for reversal of the NOACs.1 Activated charcoal may be administered to decrease the absorption of dabigatran, rivaroxaban, and apixaban. Manufacturers suggest activated charcoal be used up to 2, 8, and 6 hours, respectively.7 Hemodialysis is cited as an option for dabigatran.8
Monitoring
Newer anticoagulants promote the advantage of not requiring routine therapeutic level measurement. However, as with warfarin, pharmacists should continue to counsel and monitor patients regarding signs and symptoms of bleeding. In certain instances, quantifying the degree of anticoagulation would be beneficial to guide reversal. Laboratory options that have been evaluated in clinical trials are summarized in TABLE 2.7,9 A discussion of the practical utility of these coagulation assays follows.
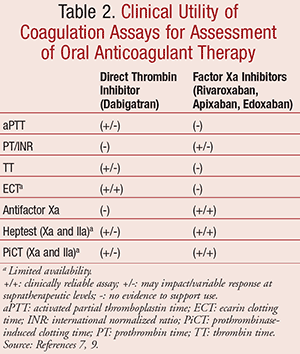
Direct Thrombin Inhibitors (DTIs): Although the presence of dabigatran impacts activated partial thromboplastin time (aPTT) as well as prothrombin time (PT)/INR, the dose response with each of these assays varies, particularly at higher concentrations.10 Therefore, aPTT, PT, and INR may be tools for determining compliance with therapy or for initial detection of dabigatran during an emergent evaluation instead of quantifying a patient’s coagulopathy. Similarly, although thrombin time (TT) increases in the presence of a DTI, it becomes inaccurate at supratherapeutic concentrations. The ecarin clotting time (ECT) provides a reliable, concentration-dependent, linear response to DTIs, including at higher concentrations.11 Chromogenic assays, which have the ability to measure antifactors Xa and IIa, have demonstrated correlation with DTIs including lepirudin and argatroban; however, limited data are available with use of these assays for patients on dabigatran.12
Factor Xa Inhibitors: Although analysis of PT/INR provides a linear dose response with use of factor Xa inhibitors, clinicians should be aware that patients receiving therapeutic doses of factor Xa inhibitors may present with a normal PT/INR value. Use of aPTT yields a nonlinear dose response, and thus is not ideal for measurement purposes. Assays that allow for quantification of factor Xa activity, such as antifactor Xa, Heptest, and prothrombinase-induced clotting time (PiCT), offer highly reproducible and precise, dose-dependent linear response.7
While the utility of these assays has been established in the investigational setting, lack of availability at most institutions along with cost-related limitations creates a challenge when selecting the appropriate assay for urgent evaluation of a critically ill patient. Assays including ECT, Heptest, and PiCT, which seem to provide the most promising utility in this patient population, are currently not widely available. The use and significance of these nonstandardized biomarkers as surrogate endpoints for desired clinical outcomes remain to be seen.
Options for Urgent Reversal
Limited options exist currently for rapid reversal of oral anticoagulants and include blood derivatives such as fresh frozen plasma (FFP) and prothrombin complex concentrates (PCCs), including coagulation factor VIIa (recombinant), in conjunction with treatment for nonemergent reversal.1 These products may aid in the reversal of anticoagulants, but are not true antidotes.
FFP is frequently used for urgent reversal of elevated INR. This product is composed of plasma from whole blood containing both coagulation and anticoagulant factors in normal physiological concentrations. Standard weight-based dosing of 10 to 20 mL/kg, which is commonly 2 units of FFP, provides a 20% to 30% increase in the levels of plasma clotting factors.9 Disadvantages of using FFP include the administration of a large volume of fluids and the risk of transmitting infective agents. Other adverse effects associated with FFP include urticaria, transfusion-associated cardiac overload, and acute lung injury, although anaphylaxis is not as common compared to phytonadione.9
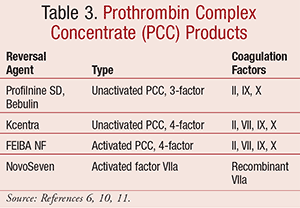
Several PCCs are available in activated and inactivated forms in the United States (TABLE 3).6,10,11 Current guidelines favor use of PCCs over FFP for reversal of warfarin-associated coagulopathy, although use for NOACs is not addressed.1 Composition of each PCC varies, as concentrations of each individual clotting factor depend on the product, manufacturer, and lot. Dosages are expressed as units of factor IX component. When compared to FFP, advantages of using PCC include reduced risk of volume overload and shorter infusion time of 15 to 30 minutes. Disadvantages consist of an increased risk for thrombosis due to the prothrombotic nature of factor products, particularly those containing activated factors. Furthermore, the shortened half-life of activated factor VIIa may deem repeated administrations necessary. Inclusion of heparin in some PCC formulations (Bebulin, Kcentra) reduces the risk of thrombosis due to the presence of factors with long half-lives, although it limits use in patients with contraindications to heparin therapy.3
Inconsistent dosing is noted in studies evaluating PCC for urgent reversal of NOACs. The suggested approach to dosing factor products ranges from fixed-dose to weight-based or INR-specific.9 The need for repeat dosing has similarly not been elucidated.13 Recommendations seen in literature are largely derived from findings in the investigational setting and are not currently approved by the FDA. The efficacy of 25 to 50 U/kg of four-factor PCC (Kcentra) for reversal of elevated INR in warfarin patients has recently received FDA approval.11 While dabigatran targets thrombin, it is hypothesized that administration of factors may overcome dabigatran’s effects on the coagulation cascade, allowing for PCC to play a role in its reversal.14 In fact, emergent reversal of dabigatran with activated PCC (aPCC) has shown efficacy in trials with animal models and healthy volunteers, with doses ranging from 12 to 160 U/kg.15,16 Trials evaluating rivaroxaban reversal with four-factor PCC have employed dosing strategies similar to those of warfarin and have demonstrated reversal, although potential efficacy of lower doses cannot be ruled out. Dosing employed in available literature is 50 units/kg.14
These results may potentially apply to reversal of other Xa inhibitors due to a shared mechanism of action.14-16 While promising, it should be noted that this evidence is primarily derived from healthy volunteers and animal models, and assessed with varying measurement assays in place of outcome data from coagulopathic patients requiring emergent reversal.
As with measurement assays, availability of blood derivatives varies among institutions. In instances where four-factor products are not available, clinicians may elect to administer a three-factor PCC and activated factor VIIa together to provide the same clotting factors as a four-factor PCC product.6 The nuances of each product, potential for thromboembolic complications, and cost must be considered when developing an institution-specific approach towards anticoagulant management and reversal.
Reversal Products in the Pipeline
Presently, there is no true antidote for the NOACs. Two agents in the drug development pipeline show promise in filling this void, andexanet alfa and idarucizumab.15,17 Both are designated as breakthrough therapy by the FDA, which may hasten approval.16,18 Andexanet alfa, also known as r-antidote or PRT064445, is an inactive human recombinant factor Xa inhibitor antidote. The modifications to the structure render the recombinant protein catalytically inactive.15 The mechanism of action is through competing with circulating levels of factor Xa to bind directly with factor Xa inhibitors, as well as heparin-antithrombin complexes. Therefore, andexanet alfa inhibits both direct and indirect factor Xa inhibitor–mediated anticoagulation.16 In animal models, IV administration of andexanet alfa 2 hours after rivaroxaban resulted in up to 85% reduction in blood loss.16
In phase I evaluation, the results demonstrated dose-dependent reduction of antifactor Xa activity of rivaroxaban and also demonstrated no interference with tissue factor initiation of thrombin production in plasma of those patients receiving andexanet alfa.19 An ongoing phase II study is evaluating the anticoagulant reversal effects, pharmacokinetics, and safety of andexanet alfa with the NOACs. The study is a randomized, double-blind, placebo-controlled trial in which each factor Xa inhibitor will be evaluated with up to four different andexanet alpha doses or placebo.19 Participants receiving apixaban 5 mg twice daily for 6 days were randomized into six different cohorts to receive IV andexanet alfa. Three cohorts received a single IV bolus of 90 mg, 210 mg, or 420 mg. The remaining three cohorts received a bolus combined with an infusion; the initial bolus was 420 mg IV plus one of the following: 45-minute infusion, 2-hour infusion, or repeat bolus at 45 minutes. Preliminary results demonstrated that 2 minutes following administration of the 420-mg andexanet alfa bolus, the anticoagulant activity of apixaban, measured by antifactor Xa activity, was reduced by approximately 92% compared with placebo.19
The safety follow-up for this study is ongoing, and no serious adverse events or premature discontinuations of andexanet alfa have been reported to date. Thus far, one case of pneumonia was observed, though no thrombotic events or development of antibodies against andexanet alfa has been reported.19,20
Idarucizumab, a fully humanized antibody fragment, is an investigational antidote for dabigatran with a mechanism analogous to agents for digoxin toxicity. Idarucizumab has been shown in animal models to bind and neutralize dabigatran to allow normalization of clotting parameters.17,21 Phase I trial data showed that idarucizumab administered to healthy participants produces immediate, complete, and sustained reversal of dabigatran-induced anticoagulation.21 The RE-VERSE AD trial is under way in patients taking dabigatran who have developed uncontrolled bleeding or require emergent surgery or procedures (NCT02104947).22 The primary outcome of the study is to evaluate the maximum reversal of the anticoagulant effect of dabigatran at any time from the end of the infusing of 0.5 g idarucizumab up to 4 hours following the last infusion.22
Last, another potential antidote, PER977 (aripazine), is currently undergoing clinical trials for reversal of multiple anticoagulants.23 Aripazine exhibits its effect by directly binding with anticoagulants. In animal models, rats treated with NOACs demonstrated a 90% rate of bleeding reversal following aripazine administration. Although there are limited clinical data at this time, this potential antidote has shown promise in both in vivo and in vitro studies.24
Conclusion
With increased use of NOACs, development of antidotes and management strategies remains vital to ensure patient safety. Limited data currently advocate for withholding NOACs for nonemergent reversal, and using PCCs for urgent reversal. Clinicians should be keenly aware of available options, forthcoming antidotes, and supporting clinical evidence in order to improve outcomes in management of coagulopathic patients who are taking NOACs.
REFERENCES
1. Ageno W, Gallus AS, Wittkowsky A, et al. Oral antico-agulant therapy: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest. 2012; 141(2 suppl):e44S-e88S.
2. Tsu LV, Dienes JE, Dager WE. Vitamin K dosing to reverse warfarin based on INR, route of administration, and home warfarin dose in the acute/critical care setting. Ann Pharmacother. 2012;46:1617-1626.
3. Miyares MA, Davis K. Newer anticoagulants: a review of laboratory monitoring options and reversal agents in the hemorrhagic patients. Am J Health Syst Pharm. 2012;69:1473-1484.
4. Pradaxa (dabigatran) package insert. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals, Inc; 2014.
5. Savaysa (edoxaban) package insert. Parsippany, NJ: Daiichi Sankyo, Inc; January 2015.
6. Kalus JS. Pharmacologic interventions for reversing the effects of oral anticoagulants. Am J Health Syst Pharm. 2013;70(10 suppl 1):S12-S21.
7. Lindahl TL, Baghaei F, Blixter IF, et al. Effects of the oral, direct thrombin inhibitor dabigatran on five common coagulation essays. Thromb Haemost. 2011;105:371-378.
8. Stangier J, Rathgen K, Stahle H, et al. The pharmacokinetics, pharmacodynamics and tolerability of dabigatran etexilate, a new oral direct thrombin inhibitor, in healthy male subjects. Br J Clin Pharmacol. 2007;64:292-303.
9. Amiral JJ, Vissac AM, Peyrafitte M. New assays for measuring direct thrombin inhibitors in plasma [abstract]. Thromb Haemost. 2009;7:2.
10. NovoSeven RT (coagulation factor VIIa [recombinant]) package insert. Plainsboro, NJ: Novo Nordisk, Inc; 2014.
11. Kcentra (prothrombin complex concentrate [human]) package insert. Kankakee, IL: CSL Behring, LLC; 2014.
12. Wong PC, Crain EJ, Xin B, et al. Apixaban, an oral, direct and highly selective factor Xa inhibitor: in vitro, antithrombotic and antihemostatic studies. J Thromb Haemost. 2008;6:820-829.
13. Samama MM, Guinet C. Laboratory assessment of new anticoagulants. Clin Chem Lab Med. 2011;49:761-772.
14. Eerenberg ES, Kamphuisen PW, Sijpkens MK, et al. Reversal of rivaroxaban and dabigatran by prothrombin complex concentrate. Circulation. 2011;124:1573-1579.
15. Lu G, DeGuzman FR, Hollenbach SJ, et al. A specific antidote for reversal of anticoagulation by direct and indirect inhibitors of coagulation factor Xa. Nat Med. 2013;19:446-451.
16. Ebright J, Mousa SA. Oral anticoagulants and status of antidotes for the reversal of bleeding risk. Clin Appl Thromb Hemost. 2014 Aug 12 [Epub ahead of print].
17. Schiele F, van Ryn J, Canada K, et al. A specific antidote for dabigatran: functional and structural characterization. Blood. 2013;121:3554.
18. O’Riordan M. Positive results for factor Xa inhibitor antidote: ANNEXA-A. Medscape. www.medscape.com/viewarticle/832648. Accessed January 29, 2015.
19. Crowther M, Kitt M, Lorenz T, et al. A phase 2 randomized, double-blind, placebo-controlled trial of PRT064445, a novel, universal antidote for direct and indirect factor Xa inhibitors. Presented at: XXIV Congress of the International Society on Thrombosis and Haemostasis; June 29-July 4, 2013; Amsterdam, the Netherlands.
20. Portola Pharmaceuticals announces first phase 2 results demonstrating extended duration infusion with andexanet alfa (PRT4445) provides prolonged reversal of anticoagulation activity of factor Xa inhibitor Eliquis. Portola Pharmaceuticals, Inc. July 2, 2013. http://investors.portola.com/phoenix.zhtml?c=198136&p=irol-newsArticle&ID=1834683. Accessed October 21, 2014.
21. Glund S, Stangier J, Schmohl M, et al. A specific antidote for dabigatran: immediate, complete and sustained reversal of dabigatran induced anticoagulation in healthy male volunteers. Presented at: American Heart Association Scientific Sessions, Dallas, Texas; November 16-20, 2013; Abstract 17765.22. Reversal of dabigatran anticoagulant effect with idarucizumab. NCT02104947. ClinicalTrials.gov. https://clinicaltrials.gov/ct2/show/NCT02104947?term=idarucizumab&rank=1. Accessed June 25, 2014.
23. PER977. ClinicalTrials.gov. http://clinicaltrials.gov/ct2/results?term=PER977&Search=Search. Accessed October 29, 2014.
24. PER977. An oral anticoagulant reversal agent. Perosphere Inc. http://perosphere.com/content/research/per977.htm. Accessed October 28, 2014.
To comment on this article, contact rdavidson@uspharmacist.com.





