US Pharm. 2015;40(5):HS11-HS20.
ABSTRACT: Over the last several decades, the assessment and treatment of pain in children has become a standard of pediatric care. Despite improvements in and availability of pain-assessment tools and increased awareness of pharmacotherapeutic factors, the pain reported by hospitalized children has not decreased. This suggests that these patients are still receiving inadequate analgesia. Barriers include misconceptions about pain perception, lack of knowledge about potential long-term consequences of pain in children, and perceived difficulties in assessing the presence and degree of pain in children. Additional barriers are inadequate information on appropriate treatment modalities for pain and concern about potential adverse effects. Studies are needed to identify optimal strategies for translating current knowledge into improved clinical practices in pediatric pain management.
Over the last several decades, the assessment and treatment of pain in children has become a standard of pediatric care. The prevalence of moderate-to-severe pain in hospitalized children has been reported to be between 25% and 64%.1,2 Although progress has been made in the availability of pain-assessment tools and the understanding of pain pharmacotherapy, research suggests that hospitalized children are still receiving inadequate analgesia.1-4 Fewer than 25% of hospitalized children who reported moderate-to-severe pain received an appropriate scheduled opioid, and fewer than 33% of those prescribed as-needed opioids received their medication.1,2 Despite guidelines published by the American Academy of Pediatrics and the World Health Organization (WHO), current literature indicates that barriers remain to effective analgesia in hospitalized children.3,4 Barriers include misconceptions about pain perception; lack of knowledge about potential long-term consequences of pain in children; perceived difficulties in assessing the presence and degree of pain in children; inadequate information on appropriate treatment modalities for pain; and concern about potential adverse effects (AEs), including respiratory depression and addiction.5-7
Pain Perception
Fetal neuronal connections between spinal dorsal horn cells and sensory neurons occur early in gestation and are present in the fetal skin and mucous membranes in the second trimester of pregnancy. Synapses between spinal connections and sensory neurons are developed by the beginning of the third trimester. Interconnections with the thalamus are complete by 24 weeks, and myelination of the sensory pain tracts of the central nervous system is accomplished by 30 weeks.5 The only pathways documented to be deficient in prematures are those of the descending inhibitory controllers of pain. Therefore, neonates are likely more sensitive to pain than are older infants.5,6 Although infants have more generalized responses to pain compared with older children, their ability to perceive and react to pain has been documented.8 The assumption that increased distractibility in children indicates a lack of pain may lead to the incorrect conclusion that pediatric patients do not perceive pain as noxious stimuli and therefore need minimal analgesia.
Consequences of Pain
There is a lack of knowledge about the potential long-term consequences of pain in children, but evidence is growing that children, even young prematures, experience pain and the consequences of pain in the form of metabolic, hormonal, and hemodynamic stress. The release of cortical hormones, catecholamines, glucagon, and catabolic hormones results in increases in oxygen consumption and in carbon dioxide production, hyperglycemia, and a catabolic state. The end result is a negative nitrogen balance. In postsurgical children, the degree of this stress response correlates with mortality rates. Hyperalgesia and allodynia have been reported in the literature as a result of pain in prematures and neonates, presumably a result of modification of neuronal pathways in response to painful stimuli.9 Anecdotal reports and animal data indicate that repeated exposure to pain may result in patterns of self-destructive behavior, attention-deficit/hyperactivity disorder, impaired social skills, anxiety, and stress-related disorders in older children and adolescents.10
Pain Assessment
Optimal pain management begins with an accurate and thorough assessment of pain. Self-reporting is considered the gold standard for pain assessment.11 Since self-reporting is not possible in infants and young children, a growing body of literature describes pain assessment using behavioral and physiological measures in nonverbal children. As cognitive abilities advance, children become verbal and later develop the mathematical concepts required to seriate. A number of developmentally appropriate assessment tools have been designed. As children grow into adolescents, they develop the cognitive and communication skills needed to think about pain in abstract terms and describe the quality of their pain.
Behavioral, physiological, and self-reporting tools have been modified to accommodate pediatric populations with cognitive impairments, language or speech deficits, motor impairments, or sensory impairments.11 Tools based solely on physiological measurements such as heart rate, palmar sweating, transcutaneous oxygenation, blood pressure, and respirations should be used with caution, since they are nonspecific and may not adequately reflect pain.
TABLE 1 summarizes common pain-assessment tools used in children and the appropriate developmental or age range for their use. Pain assessment should be frequent and thorough, as it is a prerequisite for effective treatment and monitoring of the child’s response to analgesic therapies.

Pain Treatment
The effort to provide pediatric patients with timely, effective, and safe analgesia requires a multidisciplinary approach and focused training and information on pain-management techniques in children. One study found that pediatric medical residents lacked basic knowledge in the use of analgesics in children.12 Specific areas in which the residents were deficient included opioid equivalency and appropriate dosing of nonopioid analgesics.
The WHO, recognizing that pharmacists play an important role in the translation of research data into clinical practice, has extracted and published relevant information in a format specifically designed for pharmacists.13 The WHO guidelines recommend a two-step approach to pain management in children, beginning with the categorization of pain as mild (step 1) or moderate-to-severe (step 2). Potential analgesics for mild pain are nonopioid analgesics at fixed maximal doses, which can provide limited analgesia. For moderate-to-severe pain, strong opioids in weight-appropriate starting doses are indicated and may be increased in steps of no more than 50% per 24 hours. Multiple therapies with nonopioids may be required.14 Appropriate analgesics should be dosed at regular intervals, using the least invasive administration route indicated. Therapy should be individualized and should include appropriate baseline analgesia given at regular prescribed intervals, as well as intermittent as-needed therapy for breakthrough pain.
Appropriate starting doses of nonopioid analgesics are listed in TABLE 2, and those for opioid analgesics in opiate-naïve children are given in TABLE 3. These dosages are intended to be suggestions. Clinical factors such as age, pain chronicity, drug tolerance, and anxiety level can have profound effects on the ultimate dose required to produce analgesia. All opioid doses should be titrated upward until satisfactory analgesia is obtained.
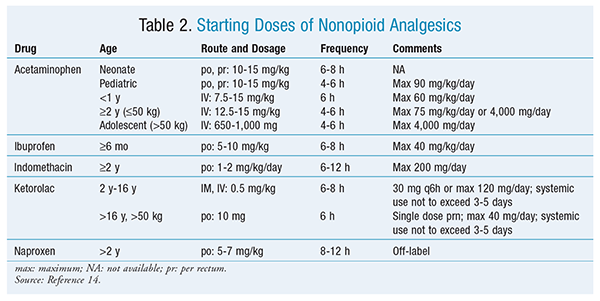
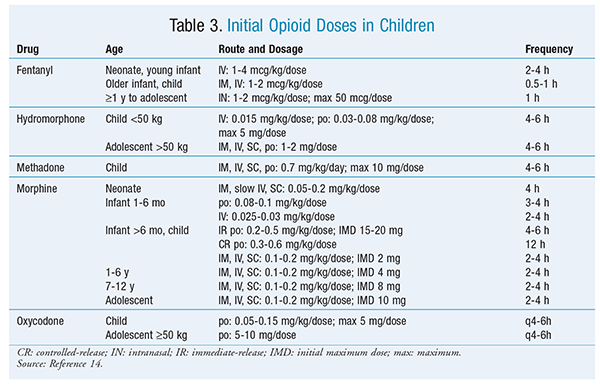
Of note is the omission of codeine from TABLE 3. A neonatal death caused by respiratory depression secondary to codeine administration to a lactating mother has been reported.15 Other studies have reported codeine’s unreliability as an analgesic in children secondary to phenotypic differences in metabolism of codeine to morphine.16,17 In 2012, the WHO excluded codeine from its recommended medications for pain management in children.4 In 2013, following a series of deaths reported since 1969 in children undergoing tonsillectomy and/or adenoidectomy for obstructive apnea, the FDA eliminated this indication for codeine. Despite these events, recent studies have found continued high use of codeine by both emergency department and inpatient prescribers.18,19 Counseling directed at prescribers that identifies more appropriate analgesics appears to be needed.
Adverse Effects
The common AEs of opioids and nonopioid analgesics are similar in children and adults. Sedation, constipation, nausea, and vomiting are commonly reported in children taking opioids, and renal impairment and gastrointestinal (GI) upset have been reported with nonopiate use. Neonates, however, have maturational differences in the metabolism and renal excretion of drugs. Significant pharmacokinetic differences have been identified in prematures and neonates for nonsteroidal anti-inflammatory drugs, acetaminophen, morphine, and fentanyl.20,21 Neonates appear to be less susceptible to the respiratory depressive effects of morphine, owing to metabolic pathways that result in increased levels of morphine 3-glucuronide and lower levels of morphine 6-glucuronide.20 AEs uncommon in older children and adults, such as chest-wall rigidity and laryngospasm, have been identified in prematures on ventilators who are receiving fentanyl.20,21
Patient-Controlled Analgesia
For more than two decades, patient-controlled analgesia (PCA) has been used clinically in children and has been well tolerated in children aged 5 years and older. PCA has been studied in children with cancer, sickle-cell disease, and burns.22-24 It has been used in children with acute postoperative pain and in those with chronic pain who are receiving palliative care.25 For children unable or unwilling to participate in their own analgesia, nurses and parents have served as surrogates to assist the child in the PCA process.26 Advantages of PCA include decreased need for painful IM injections; ability to provide a baseline individualized opioid blood level; rapid effective analgesia with less patient anxiety; reduced sleep disruption; decreased overall dose of opioids; and greater patient satisfaction.27
Morphine and fentanyl are the most frequently used opioids for analgesia using PCA, based on their safety record for pediatrics, rapid onset of action, short half-lives with resultant short durations of action, and relative ease of titration and weaning. Initial morphine dosing includes a basal rate of 10 to 30 mcg/kg/h with 10 to 30 mcg/kg bolus doses every 4 to 6 hours. The suggested maximum initial dose is 100 to 150 mcg/kg/h. Fentanyl has a 0.5 to 1 mcg/kg/h initial basal rate, with 0.5 to 10 mcg/kg bolus doses every 2 to 3 hours and a maximum initial dose of 2 to 4 mcg/kg/h. The lockout period for both medications is 6 to 10 minutes.14 Hydromorphone has also been recommended, for similar reasons.
Monitoring parameters in children on PCA are the same as those for other opioid analgesics. Most AEs have been minor. GI effects and pruritus can be attenuated by using concurrent opioid-sparing analgesia. Rarely, respiratory depression has been associated with the administration of baseline infusions of morphine, in addition to boluses.
Alternative Management Strategies
Adjunctive therapies like benzodiazepines and anticonvulsants have been used to supplement analgesics in the treatment of muscular spasm, anxiety, and neurogenic pain. Sucrose is considered safe and effective for reducing procedural pain in neonates.28 Complementary therapies reported in the literature as effective include acupuncture, guided imagery, thermal therapy, distraction, relaxation techniques, hypnosis, and art therapies.29 Some of these modalities require learning and are more suited for the treatment of chronic rather than acute pain.
System Approach to Improvement
The provision of knowledge to a single discipline has not produced consistent pain management in hospitalized children.12,30 An interprofessional health team focus on the management of pediatric pain is required. Translational approaches are needed to ensure that pharmacotherapeutic research and advances in technology result in improvements in clinical pain management. Multidisciplinary approaches to the assessment and treatment of pain in hospitalized children have been effective in translating knowledge into clinical practice, with resulting improvements in pain prevalence and pain intensity as measured by clinical outcomes.31,32
Conclusion
More interdisciplinary research is required to identify optimal strategies for improving pediatric pain management. A multidisciplinary approach is needed to provide essential information on the assessment and management of pain in children and to promote safe and effective analgesia as a primary treatment goal. The pharmacist has knowledge relevant to the goal of developing a safe and effective pain treatment plan for hospitalized children and can be an important advocate within the interdisciplinary team.
REFERENCES
1. Kozlowski LJ, Kost-Byerly S, Colantuoni E, et al. Pain prevalence, intensity, assessment and management in a hospitalized pediatric population. Pain Manag Nurs. 2014;15:22-35.
2. Taylor EM, Boyer K, Campbell FA. Pain in hospitalized children: a prospective cross-sectional survey of pain prevalence, intensity, assessment and management in a Canadian pediatric teaching hospital. Pain Res Manag. 2008;13:25-32.
3. Fein JA, Zempsky WT, Cravero JP, et al. Relief of pain and anxiety in pediatric patients in emergency medical systems. Pediatrics. 2012;130:e1391-e1405.
4. World Health Organization. WHO Guidelines on the Pharmacological Treatment of Persisting Pain in Children With Medical Illnesses. Geneva, Switzerland: World Health Organization; 2012.
5. Gerik SM. Pain management in children: developmental considerations and mind-body therapies. South Med J. 2005;98:295-302.
6. Ghai B, Makkar JK, Wig J. Postoperative pain assessment in preverbal children and children with cognitive impairment. Paediatr Anaesth. 2008;18:462-477.
7. American Academy of Pediatrics Committee on Psychosocial Aspects of Child and Family Health, Task Force on Pain in Infants, Children, and Adolescents. The assessment and management of acute pain in infants, children, and adolescents. Pediatrics. 2001;108:793-797.
8. Walker SM. Pain in children: recent advances and ongoing challenges. Br J Anaesth. 2008;101:101-110.
9. Taddio A, Katz J, Ilersich AL, Koren G. Effect of neonatal circumcision on pain response during subsequent routine vaccination. Lancet. 1997;349:599-603.
10. Buskila D, Neumann L, Zmora E, et al. Pain sensitivity in prematurely born adolescents. Arch Pediatr Adolesc Med. 2003;157:1079-1082.
11. Valkenburg AJ, van Dijk M, de Klein A, et al. Pain management in intellectually disabled children: assessment, treatment, and translational research. Dev Disabil Res Rev. 2010;16:248-257.
12. Saroyan JM, Schechter WS, Tresgallo ME, et al. Assessing resident knowledge of acute pain management in hospitalized children: a pilot study. J Pain Symptom Manage. 2008;36:628-638.
13. World Health Organization. Persisting Pain in Children: Highlights for Pharmacists Extracted From the WHO Guidelines on the Pharmacological Treatment of Persisting Pain in Children With Medical Illnesses. Geneva, Switzerland: World Health Organization; 2012.
14. Engorn B, Flerlage J. The Harriet Lane Handbook: A Manual for Pediatric Health Officers. 20th ed. Philadelphia, PA: Saunders; 2015:111-118.
15. Koren G, Cairns J, Chitayat D, et al. Pharmacogenetics of morphine poisoning in a breastfed neonate of a codeine-prescribed mother. Lancet. 2006;368:704.
16. Williams DG, Patel A, Howard RF. Pharmacogenetics of codeine metabolism in an urban population of children and its implications for analgesic reliability. Br J Anaesth. 2002;89:839-845.
17. Niesters M, Overdyk F, Smith T, et al. Opioid-induced respiratory depression in paediatrics: a review of case reports. Br J Anaesth. 2013;110:175-182.
18. Kaiser SV, Asteria-Penaloza R, Vittinghoff E, et al. National patterns of codeine prescriptions for children in the emergency department. Pediatrics. 2014;133:e1139-e1147.
19. Cartabuke RS, Tobias JD, Taghon T, Rice J. Current practices regarding codeine administration among pediatricians and pediatric subspecialists. Clin Pediatr (Phila). 2014;53:26-30.
20. Ancora G, Garetti E, Pirelli A, et al. Analgesic and sedative drugs in newborns requiring respiratory support. J Matern Fetal Neonatal Med. 2012;25(suppl 4):88-90.
21. Bouwmeester NJ, Hop WC, van Dijk M, et al. Postoperative pain in the neonate: age-related differences in morphine requirements and metabolism. Intensive Care Med. 2003;29:2009-2015.
22. Bayat A, Ramaiah R, Bhananker SM. Analgesia and sedation for children undergoing burn wound care. Expert Rev Neurother. 2010;10:1747-1759.
23. Stinson J, Naser B. Pain management in children with sickle cell disease. Paediatr Drugs. 2003;5:229-241.
24. Mercadante S. Cancer pain management in children. Palliat Med. 2004;18:654-662.
25. McDonald AJ, Cooper MG. Patient-controlled analgesia: an appropriate method of pain control in children. Paediatr Drugs. 2001;3:273-284.
26. Birmingham PK, Suresh S, Ambrosy A, Porfyris S. Parent-assisted or nurse-assisted epidural analgesia: is this feasible in pediatric patients? Paediatr Anaesth. 2009;19:1084-1089.
27. Franson HE. Postoperative patient-controlled analgesia in the pediatric population: a literature review. AANA J. 2010;78:374-378.
28. Stevens B, Yamada, J, Lee GY, Ohlsson A. Sucrose for analgesia in newborn infants undergoing painful procedures. Cochrane Database Syst Rev. 2013(1):CD001069.
29. Lassetter JH. The effectiveness of complementary therapies on the pain experience of hospitalized children. J Holist Nurs. 2006;24:196-208.
30. Bice AA, Gunther M, Wyatt T. Increasing nursing treatment for pediatric procedural pain. Pain Manag Nurs. 2014;15:365-379.
31. Zhu LM, Stinson J, Palozzi L, et al. Improvements in pain outcomes in a Canadian pediatric teaching hospital following implementation of a multifaceted, knowledge translation initiative. Pain Res Manag. 2012;17:173-179.
32. Stevens BJ, Yamada J, Estabrooks CA, et al. Pain in hospitalized children: effect of a multidimensional knowledge translation strategy on pain process and clinical outcomes. Pain. 2014;155:60-68.
33. Crellin D, Sullivan TP, Babl FE, et al. Analysis of the validation of existing behavioral pain and distress scales for use in the procedural setting. Paediatr Anaesth. 2007;17:720-733.
34. Drendel AL, Kelly BT, Ali S. Pain assessment for children: overcoming challenges and optimizing care. Pediatr Emerg Care. 2011;27;773-781.
35. Chiaretti A, Pierri F, Valentini P, et al. Current practice and recent advances in pediatric pain management. Eur Rev Med Pharmacol Sci. 2013;17(suppl 1):112-126.
36. Schultz AA, Murphy E, Morton J, et al. Preverbal, Early Verbal Pediatric Pain Scale (PEPPS): development and early psychometric testing. J Pediatr Nurs. 1999;14:19-27.
To comment on this article, contact rdavidson@uspharmacist.com.






