US Pharm. 2009;34(12):12.
At the end of the 20th century, there were changes in the incidence, prevalence, and overall impact of digestive diseases, as evidenced by the 2008 update to the National Institutes of Health publication on digestive diseases.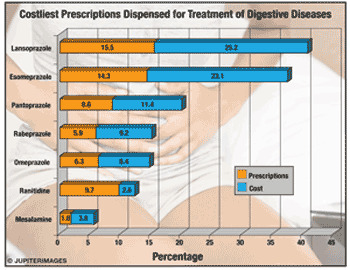
Hospital and Ambulatory-Care Visits: Between 1983 and 1988, rates of hospitalization for digestive diseases fell, a trend that occurred for all causes of hospitalization. Hospitalization rates were stable for the next 10 years and rose by 2004 to a rate equal to the previous peak rate in 1982. Between 1998 and 2004, the hospitalization rate for all diseases increased to 35%. The largest contributions to the increase were made by gastroesophageal reflux disease (GERD), with an increase of 376 per 100,000; viral hepatitis C (79/100,000); chronic constipation (62/100,000); and intestinal infection (41/100,000). Although overnight hospitalizations with a diagnosis of digestive disease decreased notably for peptic ulcer disease (PUD) and gallstones owing to a shift to same-day surgery, 25% of all hospital discharges in 1998 had a diagnosis of digestive disease; this increased to 30% in 2004.
In 2004, there were 35,684 ambulatory-care visits related to digestive diseases per 100,000 population. Visits were common for all age groups, with the highest rate in individuals aged 65 years and older. Rates were comparable between black patients and white patients and were 20% higher for females than for males.
Costs: Total ambulatory-care costs (excluding ambulatory surgery) in 2004 were $16 billion. Outpatient procedures constituted 50% of this amount. Abdominal-wall hernia (AWH), GERD, chronic constipation, gallstones, and diverticular disease were the biggest contributors to ambulatory costs. Diseases costing more than $1 billion were (in descending order) gallstones, AWH, diverticular disease, pancreatitis, colorectal cancer, appendicitis, liver disease, GERD, and PUD. The total cost of prescription drugs written during office visits was $12.3 billion, and more than half of this cost ($7.7 billion) was associated with drugs prescribed for GERD. PUD, hepatitis C virus (HCV), and irritable bowel syndrome (IBS) were major contributors to the remaining drug cost.The chart shows the seven costliest prescription drugs for digestive diseases from retail pharmacies. The five proton pump inhibitors (prescribed for GERD) constituted 51% of the total number of prescriptions, amounting to 77% of total cost; mesalamine (inflammatory bowel disease) and ranitidine were the other top contributors. Other drugs adding to the cost were tegaserod (IBS, constipation), ribavirin, and peginterferon alpha 2a (HCV). The Consumer Healthcare Products Association estimates expenditures for OTC drugs for GERD, constipation, and diarrhea at $2.1 billion, excluding complementary and alternative medicines.
In 2004, the costliest prescriptions (n = 938,000) filled at retail pharmacies were for gastrointestinal (GI) infections; most were antimicrobials or GI-motility agents (e.g., promethazine). The next costliest prescriptions were for viral hepatitis (n = 637,000), but these were represented by a few drugs.
Continued progress in improving the health of the population requires continued investment in digestive disease research, public-health initiatives, the health care system, and education of the public.
To comment on this article, contact rdavidson@jobson.com.




