US Pharm. 2018;(43):6-10.
The common cold is a condition that is prevalent in the community and is associated with a variety of symptoms. Typically, it is an acute, self-limiting viral infection of the upper respiratory tract that is most frequently caused by rhinoviruses.1 Symptoms commonly associated with the common cold include coughing, nasal congestion, low-grade fever, and fatigue, usually presenting 1 to 2 days after exposure. Generally, most symptoms subside within 7 to 10 days, although some symptoms can persist for up to 3 weeks.2 The incidence of the common cold declines with increasing age. Data indicate that children experience colds about six to eight times a year, adults younger than age 60 years tend to have two to four colds per year, and adults older than age 60 years usually have only one cold a year.2 In addition to age, factors such as stress and lack of sleep may increase the risk of the common cold.3 While the cold does not cause serious illness or complications in most cases, patients with comorbidities may be at a higher risk for complexities such as exacerbations of asthma, chronic obstructive pulmonary disease, and pneumonia.
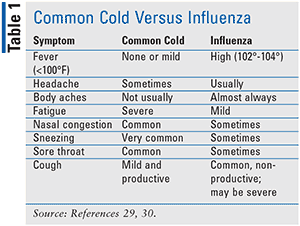
The common cold is often mistaken for the flu. The flu is caused by the influenza virus, classified as type A, B, or C. Types A and B affect humans, with type A generating more severe symptoms. The influenza virus can be dangerous in older people and in those patients who are immunocompromised. Nevertheless, people with influenza are sicker than those experiencing common cold symptoms and commonly manifest such signs and symptoms as temperatures greater than 102°F, chills, headaches, myalgia, and malaise (Table 1).3
The common cold is the leading cause of missed work and school days during the winter months. There is no known cure. Many patients seek out nonprescription medications for symptom relief, leading to expenditures in excess of $8 billion annually on cough and cold products.4
Because the common cold is a viral infection, antibiotics should be avoided. Treatment is limited to symptom relief and patients will often visit the pharmacy to inquire about OTC remedies. It is important to note that giving OTC medications to children less than 2 years of age may be dangerous; in 2008, the FDA recommended that OTC cough and cold medications be avoided in children younger than 2 years.5 Since then, manufacturers have changed the labeling of cough and cold products to state, “Do not use in children under 4 years of age.”6 For children between the ages of 4 and 6 years, there is limited evidence of clinically significant benefit regarding OTC products for treatment of the common cold.7,8
There are a multitude of products available to help provide relief from the symptoms of the common cold. Before the pharmacist makes a recommendation, the patient should be assessed to determine if he or she is a candidate for self-treatment (Table 2). Therapies available for symptom relief include antihistamines, decongestants, expectorants, antitussives, and analgesics/antipyretics used as monotherapy or in combination.
PHARMACOLOGIC AGENTS
Decongestants
If patients are suffering from nasal congestion, a systemic or topical decongestant may be appropriate. Decongestants are adrenergic agonists; they cause vasoconstriction, resulting in a decrease in sinusoid engorgement and mucosal edema.9 Phenylephrine and pseudoephedrine are two systemic decongestants often found in OTC preparations. Topical decongestants in the form of nasal sprays include the short-acting products ephedrine, na-phazoline, and phenylephrine and the longer-acting product oxymetazoline.
Multiple doses of nasal decongestants seem to provide some relief in patients suffering from nasal congestion due to the common cold.9 Oral pseudoephedrine appears to relieve congestion more effetively than phenylephrine.10,11 One study evaluated the nasal-decongestant effects of phenylephrine and pseudoephedrine compared with placebo. Phenylephrine’s effect was not significantly different from that of placebo; pseudoephedrine was found to be significantly more effective than both placebo and phenylephrine.12 This lack of efficacy may, in part, be due to phenylephrine’s extensive systemic metabolism leading to low bioavailabilty.12,13 Although pseudoephedrine is available without a prescription, state and federal regulations have moved this product behind pharmacy counters because of its role in the illegal production of methamphetamine.14 There are new formulations of pseudoephedrine available that help deter this activity and do not adversely affect the product’s decongestant properties.
Topical decongestants also relieve nasal congestion.9 These agents provide a local effect at the nasal mucosa with limited systemic absorption, leading to fewer adverse effects. One study evaluated the effect of a single-dose trial of oxymetazoline. The drug reduced nasal airway resistance and symptoms of nasal blockage within 1 hour, with the effect lasting for up to 7 hours.15 The use of topical decongestants should be limited to 3 to 5 days to avoid rebound congestion, otherwise known as rhinitis medicamentosa.16
Decongestants are relatively safe if used appropriately, but their use is associated with many adverse effects resulting from their direct action on adrenergic receptors and stimulation of the central nervous system (CNS). Common adverse effects include insomnia, increased blood pressure, restlessness, anxiety, tachycardia, palpitations, arrhythmias, hallucinations, and urinary dysfunction.17 These agents should be avoided in patients with heart disease, hypertension, thyroid disease, diabetes, and benign prostatic hyperplasia (BPH).17 Decongestants should not be used in patients who are concurrently taking monoamine oxidase inhibitors; this combination can result in a life-threatening rise in blood pressure.17
Antihistamines
To help relieve a runny nose, itchy and watery eyes, and sneezing associated with the common cold, antihistamines may be considered. First-generation antihistamines including brompheniramine, chlorpheniramine, and clemastine, are preferred over the second-generation antihistamines in the management of these symptoms. Second-generation antihistamines such as cetirizine, fexofenadine, and loratadine do not cross the blood-brain barrier; effectiveness of the first-generation agents appears to be due to their actions on histaminic and muscarinic receptors in the medulla.18 First-generation antihistamines have been shown to provide some short-term benefit against rhinorrhea, nasal congestion, and sneezing when used as monotherapy, but appear to be more beneficial when used in combination with other agents, such as decongestants and analgesics.19,20
First-generation antihistamines are associated with a variety of adverse effects because of their ability to interfere with CNS histamine receptors. These agents may cause drowsiness, sedation, somnolence, and fatigue; they should be used with caution in patients who require mental alertness. They may also potentially impair cognitive function, memory, and psychomotor performance.17,21 In addition, first-generation antihistamines are associated with undesired anticholinergic effects including dry eye, urinary retention, constipation, and mydriasis.17 Antihistamines should be not be used in patients with narrow-angle glaucoma or BPH.21
Antitussives
Many OTC cold preparations contain dextromethorphan, an antitussive, to suppress the cough that is often associated with the common cold and other respiratory infections. Although available as a single-agent preparation, dextromethorphan is also commonly available in combination with other agents in multisymptom cold and flu products. Multiple studies evaluating the efficacy of these products have been conducted but are limited by small sample size, poor study design, or variability in dosing and frequency of medication use.22 Although some reviews suggest that dextromethorphan may be effective in treating acute cough based upon cough-counting studies, others conclude that there is no strong evidence for or against the use of these agents in managing cough.22,23
When consumed in excessive doses, dextromethorphan is capable of producing hallucinogenic effects similar to those of phencyclidine and ketamine; this has resulted in the drug being abused by some individuals in the community setting.24 Surveillance data suggest that the peak prevalence of dextromethorphan abuse occurred in 2006, with an estimated 17.6 cases per million.25 Potential physiologic effects of excessively high doses of dextromethorphan include, but are not limited to, tachycardia, mental-status changes, hypertension, seizures, coma, and both respiratory and cardiac arrest.24 The abuse potential of this agent has resulted in numerous states enacting legislation prohibiting the sale of dextromethorphan to minors.24
Expectorants
Expectorants are agents that are generally employed to reduce the viscosity and volume of sputum produced by patients suffering from a variety of respiratory conditions. Guaifenesin is the only FDA-approved expectorant and is found in a variety of remedies for the symptomatic relief of acute, ineffective, productive cough. Although guaifenesin has been available in OTC preparations for decades, its efficacy as an expectorant in cold and flu preparations continues to be questioned. A 2014 Cochrane review of cough and cold products failed to find any clinical evidence supporting the clinical efficacy of the drug either alone or in combination.22
Despite the lack of trials demonstrating clinical benefit, guaifenesin continues to be promoted as an effective expectorant in OTC products. The drug is considered relatively safe and is not associated with any clinically significant drug interactions. When used at recommended doses, the drug is relatively well tolerated, with the most common side effect reported to be gastrointestinal intolerance.22
Analgesics
OTC analgesics and antipyretics such as aspirin, acetaminophen, ibuprofen, and naproxen are often employed in the management of the generalized pain, headache, and fever associated with the common cold and other viral illnesses.13,26 Although these agents are generally considered to be equally effective in the management of the above symptoms, they should be used judiciously because they are associated with several adverse effects.13 Patients with aspirin allergy and those with active ulcers may not be candidates for aspirin or related nonsteroidal anti-inflammatory drugs (NSAIDs). In addition, a recent study suggested that patients who used NSAIDs during an acute respiratory infection tripled their risk of an acute myocardial infarction.27
Prevention
Preventing the spread of common cold viruses is the primary method for reducing the risk of getting a cold. Pharmacists should educate patients on the various methods used to help reduce the risk of getting a cold. Good hygiene practices include washing the hands often with soap and water for at least 20 seconds; avoiding touching the face, eyes, nose, and mouth with unwashed hands; and avoiding contact with infected people.28
CONCLUSION
Patients affected by the common cold often rely on OTC products to help manage their symptoms. Pharmacists are an invaluable resource, providing education and recommendations to ensure safe and appropriate use of OTC medications. It is important to properly assess patients to determine whether they are candidates for self-treatment. It is also important to counsel patients to make sure that they understand potential adverse effects, drug interactions, and warnings associated with any medication.

What are the symptoms?
The common cold usually causes nasal congestion, runny nose, and sneezing. You may also have a scratchy throat, headaches, and muscle aches; you may feel tired; and you may have a low-grade fever. If a cough occurs, it usually happens on the fourth or fifth day.
What can I do if I have a cold?
• Drink plenty of fluids
• Get plenty of rest
• Humidify the air
Are there any treatments for the cold?
There is no cure for the common cold, but there are medications that might help relieve some of the symptoms. Before you use any product, you should speak with a healthcare provider, especially if you have high blood pressure, heart disease, diabetes, glaucoma, an enlarged prostate, or are allergic to aspirin.
Nasal congestion: Oral decongestants such as pseudoephedrine and phenylephrine may provide relief from a stuffy nose. If you use a decongestant nasal spray it is very important that you do not use it for more than 3 days.
Runny nose: Antihistamines may provide some relief.
Fever, sore throat/headache/body aches: Use a mild pain reliever such as acetaminophen or a nonsteroidal anti-inflammatory agent such as ibuprofen or naproxen.
Cough: Common ingredients include guaifenesin and dextromethorphan.
How can I prevent a cold?
Preventing the spread of cold viruses is the best way to prevent the spread of colds.
• Avoid contact with infected people if possible
• Practice good hand-washing habits and techniques, such as washing your hands for at least 20 seconds after touching surfaces, before preparing food and eating, and before touching your face, eyes, nose, or mouth
• Use hand sanitizers when hand-washing is not possible
• Do not share drinks or eating utensils
• Sneeze or cough into your crooked elbow and use tissues. Wash your hands afterwards
• Avoid touching the face with the hands and touching contaminated surfaces
• Have infected individuals use only one bathroom in homes with multiple bathrooms
REFERENCES
1. Mäkelä MJ, Puhakka T, Ruuskanen O, et al. Viruses and bacteria in the etiology of the common cold. J Clin Microbiol. 1998;36(2):539-542.
2. Heikkinen T, Järvinen A. The common cold. Lancet. 2003;361(9351):51-59.
3. Allan GM, Arroll B. Prevention and treatment of the common cold: making sense of the evidence. CMAJ. 2014;186(3):190-199.
4. Consumer Healthcare Products Association. OTC sales by category 2012-2016. www.chpa.org/OTCsCategory.aspx. Accessed December 27, 2017.
5. FDA. For consumers. Consumer update. Using over-the-counter cough and cold products in children. October 22, 2008. https://wayback.archive-it.org/7993/20170722060133/https://www.fda.gov/ForConsumers/ConsumerUpdates/ucm048515.htm. Accessed December 21, 2017.
6. FDA. Drugs. Special features. Use caution when giving cough and cold products to kids. November 4, 2016. www.fda.gov/Drugs/ResourcesForYou/SpecialFeatures/ucm263948.htm. Accessed December 21, 2017.
7. Briars LA. The latest update on over-the-counter cough and cold product use in children. J Pediatr Pharmacol Ther JPPT. 2009;14(3):127-131.
8. Bell EA, Tunkel DE. Over-the-counter cough and cold medications in children: are they helpful? Otolaryngol Head Neck Surg. 2010;142(5):647-650.
9. Deckx L, De Sutter AI, Guo L, et al. Nasal decongestants in monotherapy for the common cold. Cochrane Database Syst Rev. 2016;(10):CD009612.
10. Meltzer EO, Bukstein DA. The economic impact of allergic rhinitis and current guidelines for treatment. Ann Allergy Asthma Immunol. 2011;106(2 suppl):S12-S16.
11. Hatton RC, Winterstein AG, McKelvey RP, et al. Efficacy and safety of oral phenylephrine: systematic review and meta-analysis. Ann Pharmacother. 2007;41(3):381-390.
12. Horak F, Zieglmayer P, Zieglmayer R, et al. A placebo-controlled study of the nasal decongestant effect of phenylephrine and pseudoephedrine in the Vienna Challenge Chamber. Ann Allergy Asthma Immunol. 2009;102(2):116-120.
13. Eccles R, Jawad MS, Jawad SS, et al. Efficacy and safety of single and multiple doses of pseudoephedrine in the treatment of nasal congestion associated with common cold. Am J Rhinol. 2005;19(1):25-31.
14. Drug Enforcement Agency. Rules—2006. Retail sales of scheduled listed chemical products; self-certification of regulated sellers of scheduled listed chemical products. www.deadiversion.usdoj.gov/fed_regs/rules/2006/fr0926.htm. Accessed December 13, 2017.
15. Akerlund A, Klint T, Olén L, Rundcrantz H. Nasal decongestant effect of oxymetazoline in the common cold: an objective dose-response study in 106 patients. J Laryngol Otol. 1989;103(8):743-746.
16. Mortuaire G, de Gabory L, François M, et al. Rebound congestion and rhinitis medicamentosa: nasal decongestants in clinical practice. Critical review of the literature by a medical panel. Eur Ann Otorhinolaryngol Head Neck Dis. 2013;130(3):137-144.
17. Malone M. Review: side effects of some commonly used allergy medications (decongestants, anti-leukotriene agents, antihistamines, steroids, and zinc) and their safety in pregnancy. https://clinmedjournals.org/articles/ijam/international-journal-of-allergy-medications-ijam-3-024.php?jid=ijam.
18. Muether PS, Gwaltney JM. Variant effect of first- and second-generation antihistamines as clues to their mechanism of action on the sneeze reflex in the common cold. Clin Infect Dis. 2001;33(9):1483-1488.
19. De Sutter AIM, Saraswat A, van Driel ML. Antihistamines for the common cold. Cochrane Database Syst Rev. 2015;(11): CD009345.
20. De Sutter AIM, van Driel ML, Kumar AA, et al. Oral antihistamine-decongestant-analgesic combinations for the common cold. Cochrane Database Syst Rev. 2012;(2):CD004976.
21. Simon FER, Simons KJ. H1 antihistamines: current status and future directions. World Allergy Organ J. 2008;1(9):145-155.
22. Smith SM, Schroeder K, Fahey T. Over-the-counter (OTC) medications for acute cough in children and adults in community settings. Cochrane Database Syst Rev. 2014;(11):CD001831.
23. Morice A, Kardos P. Comprehensive evidence-based review on European antitussives. BMJ Open Respir Res. 2016;3(1):e000137.
24. Gershman JA, Fass AD. Dextromethorphan abuse: a literature review. J Pharm Technol. 2013;29(2):66-71.
25. Wilson MD, Ferguson RW, Mazer ME, et al. Monitoring trends in dextromethorphan abuse using the National Poison Data System: 2000–2010. Clin Toxicol. 2011;49(5):409-415.
26. Kim SY, Chang Y-J, Cho HM, et al. Non-steroidal anti-inflammatory drugs for the common cold. Cochrane Database Syst Rev. 2015;(9):CD006362.
27. Wen Y-C, Hsiao F-Y, Chan KA, et al. Acute respiratory infection and use of nonsteroidal anti-inflammatory drugs on risk of acute myocardial infarction: a nationwide case-crossover study. J Infect Dis. 2017;215(4):503-509.
28. CDC. Prevent the common cold. Published February 6, 2017. www.cdc.gov/features/rhinoviruses/index.html. Accessed December 16, 2017.
29. Cleveland Clinic. Influenza. How often symptoms occur in a cold or the flu. https://my.clevelandclinic.org/health/diseases/17146-influenza. Accessed December 21, 2017.
30. CDC. Cold versus flu. Seasonal influenza (flu). www.cdc.gov/flu/about/qa/coldflu.htm. Accessed December 21, 2017.
31. Fashner J, Ericson K, Werner S. Treatment of the common cold in children and adults. Am Fam Physician. 2012;86(2):153-159.
32. Scolaro KL. Colds and allergy. In: Kinski DL, Ferreri SP, Hemstreet B, et al, eds. Handbook of Nonprescription Drugs: An Interactive Approach to Self-Care, 18th ed. Washington, DC: American Pharmacists Association; 2015.
To comment on this article, contact rdavidson@uspharmacist.com.