US Pharm. 2017;42(8):35-38.
ABSTRACT: The management of lower back pain is relevant to the practice of community pharmacists because patients often present to community pharmacies with nonspecific back pain. In patients with acute or subacute back pain, the pharmacist may be the first healthcare professional consulted. Pharmacists should be aware of recent guidelines from the American College of Physicians that recommend nonpharmacologic options as first-line treatment. Patients who have chronic back pain may potentially come in to the pharmacy with prescriptions; therefore, community pharmacists should be aware of common medications’ considerations, dosing, and evidence supporting or discouraging their use in treating lower back pain.
The majority of Americans experience lower back pain, and one-quarter of all Americans reported back pain lasting at least 1 day within the previous 90 days.1 Patients with acute back pain who do not seek medical care typically experience improvements without treatment.2 Recent evidence suggests that a rush to perform unnecessary medical procedures, such as MRI, can lead to increased costs and poorer clinical outcomes.3 The management of lower back pain is relevant to the practice of community pharmacists because patients often present to community pharmacies with nonspecific back pain.
TREATMENT OPTIONS AT COMMUNITY PHARMACIES
In February 2017, the American College of Physicians (ACP) issued updated clinical practice guidelines for the treatment of patients with acute or subacute lower back pain. Pharmacists and other healthcare professionals are advised to reassure patients with lower back pain that their condition will typically improve regardless of the treatment options pursued.4 For patients who present to community pharmacies with back pain, the pharmacist can make a referral to a physician, suggest a course of OTC products, recommend a nonpharmacologic treatment, or advise no treatment at all.4 The ACP guidelines prioritize nonpharmacologic treatments, which include superficial heat, massage, acupuncture, and spinal manipulation.4
Transcutaneous electrical nerve stimulation (TENS) machines are often sold in community pharmacies.5 They provide an electric current to the body via adhesive pads and are purported to relieve musculoskeletal pain. However, a literature review concluded that TENS machines were no more effective than sham TENS, and this modality is not recommended for treatment of back pain in the current guidelines.6
The superficial heat wrap (e.g., Thermacare) is a particularly simple therapy that is often sold at community pharmacies. Heat wraps were shown to improve pain relief and disability compared with placebo.7 Patients who exercised and used a heat wrap had improved pain relief and Roland Morris Disability Questionnaire (RDQ) scores compared with patients who exercised and did not use a heat wrap.7 Finally, patients who used a heat wrap had improved pain relief and RDQ scores at 1 or 2 days compared with patients who used acetaminophen or ibuprofen.8
PHARMACOLOGIC THERAPY
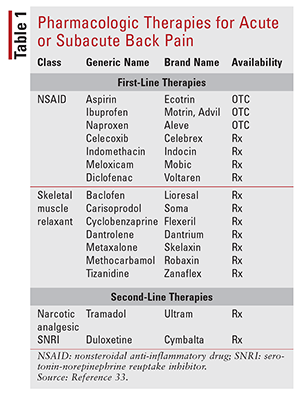
One in five patients with back pain reports a persistent, substantial limitation of activities.9 Pharmacologic therapy (TABLE 1) is likely to continue to play a role in the management of lower back pain. A recent study showed that patients with chronic lower back pain who were administered open-label placebo pills in addition to their usual treatment had less lower back pain and disability compared with patients who continued treatment as usual.10,11 The ACP guidelines do not recommend topical medications, although the recent OTC availability of lidocaine patches presents another option for patients seeking a pharmacologic treatment. In a recent double-blind, placebo-controlled study, 50% of patients treated with lidocaine patches and 50% of those treated with placebo patches reported a reduction in pain of more than 50%, and there was no difference between the groups in pain intensity or pain-related brain activity.12 These results for placebo patches were evaluated by other researchers, who speculated that simply the patient’s participation in the “rituals, symbols, and interactions” of the therapeutic encounter could lead to clinical improvement.11
The American Pain Society and the ACP jointly released a clinical guideline for the treatment of lower back pain in 2007. At that time, the guideline concluded that acetaminophen was effective for acute lower back pain.13 Evidence now supports the finding of a randomized, placebo-controlled clinical trial that acetaminophen treatment does not result in pain relief or restoration of function.14 Regarding other available OTC pharmacologic treatment, research on the use of nonsteroidal anti-inflammatory drugs (NSAIDs) for lower back pain continues to suggest that NSAIDs achieve small improvements in pain intensity and function versus placebo.4 Accordingly, recent guidelines narrow the pharmacist’s options for pharmacotherapy to just the three OTC NSAIDs: aspirin, ibuprofen, and naproxen.
First-Line Pharmacologic Therapy
NSAIDs: Evidence suggests that pain relief does not differ between traditional OTC NSAIDs and prescription NSAIDs. For this reason, pharmacists have reason to be optimistic when patients present with prescriptions for agents such as meloxicam, celecoxib, or diclofenac. In one study, pain from acute sciatica improved with the use of meloxicam 7.5 mg or 15 mg daily, and the effect was comparable to that with the use of diclofenac 150 mg.15 For patients with lower back pain and a history of gastrointestinal (GI) distress, the selective cyclooxygenase-2 inhibitor celecoxib may be the best choice of therapy. In short-term trials, celecoxib was associated with a lower rate of discontinuation owing to GI distress compared with nonselective NSAIDs.16 Among the contraindications to NSAID use are patient factors likely to increase bleeding risk, including current use of anticoagulants (warfarin, dabigatran, rivaroxaban, or apixaban), esophageal varices, chronic alcohol abuse or cigarette use, chronic liver disease, or a previous bleed.17 History of the use of any antidepressants, phenytoin, or carbamazepine is also associated with an elevated risk of a future bleed.17
Skeletal Muscle Relaxants (SMRs): SMRs are divided into two categories: antispastics and antispasmodics. Little evidence supports the use of antispastic agents, such as baclofen and dantrolene, for lower back pain. Antispasmodic agents, which include carisoprodol, cyclobenzaprine, metaxalone, methocarbamol, and tizanidine, are used for musculoskeletal conditions. Cyclobenzaprine is the most-studied SMR in published trials; however, data do not support one muscle relaxant over the others. In multiple trials, SMRs were preferred over placebo for short-term use (<1 week) in patients with acute low back pain. Evidence of the efficacy of SMRs for chronic back pain or sciatica is insufficient. SMRs may increase overall adverse effects, such as dizziness and drowsiness.13,18
Second-Line Pharmacologic Therapy
Tramadol: In patients with chronic lower back pain, tramadol was more effective than placebo for short-term pain relief and improved functional status.19,20 Evidence is sparse for tramadol in the treatment of acute or subacute lower back pain, but one study from 2010 found tramadol plus acetaminophen to be superior to acetaminophen alone in relieving subacute lower back pain.21 Pharmacists should be aware that tramadol, being an opioid, has addictive properties.22
Duloxetine: The FDA recently approved duloxetine for lower back pain because it is a safer alternative than tricyclic antidepressants (TCAs).23 In patients with chronic lower back pain, duloxetine had a moderate association with an analgesic effect versus placebo.13 Duloxetine use was associated with improvements in sleep, physical functioning, interference of pain with life and mood, and pain severity.24 No differences in serious adverse effects between duloxetine and placebo were reported in trials; however, patients receiving duloxetine versus placebo were more likely to experience withdrawal.24 No trials have evaluated the efficacy of antidepressants versus placebo for acute lower back pain.
Pharmacotherapy Not Currently Recommended
Apart from the therapies previously mentioned, pharmacists will encounter prescriptions for gabapentin, pregabalin, benzodiazepines, TCAs, systemic corticosteroids and opioids, and other drugs to treat lower back pain. In the latest ACP guidelines, the evidence was considered insufficient to support recommending the use of these agents.4 However, the community pharmacist should be aware of the patient’s therapeutic process and weigh the benefits against the adverse effects that are possible with therapy not currently recommended by the ACP.
TCAs: Current guidelines have concluded that TCAs are not effective for treating lower back pain compared with placebo. Members of the TCA class include amitriptyline, desipramine, imipramine, and nortriptyline. TCAs typically cause anticholinergic effects that pharmacists should be aware of, including dry mouth, urinary retention, constipation, blurry vision, and memory impairment. Desipramine tends to be less sedating and to have fewer anticholinergic effects than other TCAs, but evidence for relief of neuropathic pain is slim.25,26 Guidelines published by the International Association for the Study of Pain recommend nortriptyline as a first-line medication for neuropathic pain27; therefore, pharmacists may see TCAs such as nortriptyline prescribed if a neuropathic etiology is suspected or other agents have failed. Other antidepressants, such as paroxetine and trazodone, are ineffective in patients with chronic back pain and are not recommended.4
Opioids: Based on the high risk of addiction, the ACP guidelines recommend that physicians avoid prescribing opioids for relief of back pain except as a last resort. In short-term trials, patients with noncancer pain found opioids moderately superior to placebo for pain relief. However, data on long-term effects and/or abuse of opioids are sparse. Pharmacists should be aware that nausea, constipation, and somnolence are the most common side effects of opioids.4
SPINAL FRACTURES
Pharmacists who are questioned about back pain should be aware of red flags for spinal fracture, such as prolonged corticosteroid use or a history of physical trauma.28 Risk factors for a vertebral compression fracture include older age, female sex, previous history of bone fracture, current use of medications to treat osteoporosis, and acetaminophen use being insufficient to relieve the patient’s current level of pain.29 These patients are likely to require medical attention beyond pharmacotherapy and should be referred to a physician.
RADICULAR LOWER BACK PAIN
Radicular pain is pain that radiates along a nerve because of an injury to the nerve root.30 It is unlikely that patients who visit the pharmacist regarding their first complaint of back pain will be aware of a radicular cause. Patients who present to the community pharmacy with lower back pain that has a radicular cause have already undergone evaluation, likely because of pain or associated numbness.
Minimal evidence exists that supports the use of pharmacologic agents to treat radicular back pain. A previous study suggested that a large bolus dose of methylprednisolone may produce an immediate but small effect on pain relief in patients with radicular leg pain, although the effect was no longer seen after 3 days, however.30 Other studies have failed to show a benefit from corticosteroids, and current ACP guidelines recommend against the use of systemic corticosteroids, even in patients who have a radicular etiology.4
In two small trials, gabapentin was found to be slightly superior to placebo for short-term pain relief in patients with radicular back pain, although the study results varied. In one trial, patients who were titrated up to a dose of 1,200 mg did not achieve better results than placebo for back pain at rest; however, back pain during movement and leg pain improved versus placebo upon assessment.31 In the other study, in which patients received up to 3,600 mg of gabapentin, patients had greater improvements in pain relief than placebo patients.32 These results suggest that gabapentin may be used for short-term pain relief and that the effect on pain may be dose dependent; however, further studies are required.
CONCLUSION
The future treatment of lower back pain is likely to be influenced by recent guidelines developed by the ACP, which recognizes that most acute episodes of back pain are self-limiting and recommends that nonpharmacologic treatments should be used in preference to pharmacologic treatments. Pharmacists who encounter patients in the community setting may continue to recommend nonpharmacologic items, such as heat wraps, but may also recommend OTC NSAIDs, such as aspirin, ibuprofen, or naproxen. Prescription options include NSAIDs and antispasmodic SMRs. Duloxetine, tramadol, TCAs, selective serotonin reuptake inhibitors, pregabalin, and gabapentin do not have sufficient supporting evidence, but their use should be evaluated on a case-by-case basis. Opioids are considered a last-line option for treatment because improvements have been modest and the risk of addiction and adverse events is high.
REFERENCES
1. Deyo RA, Mirza SK, Martin BI. Back pain prevalence and visit rates: estimates from U.S. national surveys, 2002. Spine (Phila Pa 1976). 2006;31:2724-2727.
2. Carey TS, Evans AT, Hadler NM, et al. Acute severe low back pain. A population-based study of prevalence and care-seeking. Spine (Phila Pa 1976). 1996;21:339-344.
3. Webster BS, Bauer AZ, Choi Y, et al. Iatrogenic consequences of early magnetic resonance imaging in acute, work-related, disabling low back pain. Spine (Phila Pa 1976). 2013;38:1939-1946.
4. Qaseem A, Wilt TJ, McLean RM, Forciea MA. Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2017;166:514-530.
5. Manheimer E, White A, Berman B, et al. Meta-analysis: acupuncture for low back pain. Ann Intern Med. 2005;142:651-663.
6. van Middelkoop M, Rubinstein SM, Kuijpers T, et al. A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain. Eur Spine J. 2011;20:19-39.
7. Mayer JM, Ralph L, Look M, et al. Treating acute low back pain with continuous low-level heat wrap therapy and/or exercise: a randomized controlled trial. Spine J. 2005;5:395-403.
8. Nadler SF, Steiner DJ, Erasala GN, et al. Continuous low-level heat wrap therapy provides more efficacy than ibuprofen and acetaminophen for acute low back pain. Spine (Phila Pa 1976). 2002;27:1012-1017.
9. Von Korff M, Saunders K. The course of back pain in primary care. Spine (Phila Pa 1976). 1996;21:2833-2837.
10. Carvalho C, Caetano JM, Cunha L, et al. Open-label placebo treatment in chronic low back pain: a randomized controlled trial. Pain. 2016;157:2766-2772.
11. Hashmi JA, Baliki MN, Huang L, et al. Lidocaine patch (5%) is no more potent than placebo in treating chronic back pain when tested in a randomised double blind placebo controlled brain imaging study. Mol Pain. 2012;8:29.
12. Kaptchuk TJ, Miller FG. Placebo effects in medicine. N Engl J Med. 2015;373:8-9.
13. Chou R, Huffman LH. Clinical guideline for the evaluation and management of low back pain. American Pain Society. http://americanpainsociety.org/uploads/education/guidelines/evaluation-management-lowback-pain. Accessed June 1, 2016.
14. Williams CM, Maher CG, Latimer J, et al. Efficacy of paracetamol for acute low-back pain: a double-blind, randomised controlled trial. Lancet. 2014;384:1586-1596.
15. Dreiser RL, Le Parc JM, Vélicitat P, Lleu PL. Oral meloxicam is effective in acute sciatica: two randomised, double-blind trials versus placebo or diclofenac. Inflamm Res. 2001;50(suppl 1):S17-S23.
16. Moodley I. Review of the cardiovascular safety of COXIBs compared to NSAIDS. Cardiovasc J Afr. 2008;19:102-107.
17. Hippisley-Cox J, Coupland C. Predicting risk of upper gastrointestinal bleed and intracranial bleed with anticoagulants: cohort study to derive and validate the QBleed scores. BMJ. 2014;349:g4606.
18. See S, Ginzburg R. Choosing a skeletal muscle relaxant. Am Fam Physician. 2008;78:365-370.
19. Beaulieu AD, Peloso P, Bensen W, et al. A randomized, double-blind, 8-week crossover study of once-daily controlled-release tramadol versus immediate-release tramadol taken as needed for chronic noncancer pain. Clin Ther. 2007;29:49-60.
20. Lee JH, Lee CS. A randomized, double-blind, placebo-controlled, parallel-group study to evaluate the efficacy and safety of the extended-release tramadol hydrochloride/acetaminophen fixed-dose combination tablet for the treatment of chronic low back pain. Clin Ther. 2013;35:1830-1840.
21. Dhillon S. Tramadol/paracetamol fixed-dose combination: a review of its use in the management of moderate to severe pain. Clin Drug Investig. 2010;30:711-738.
22. Drug Enforcement Administration. Schedule of controlled substances: placement of tramadol into schedule IV. Final rule. Fed Regist. 2014;79:37623-37630.
23. Chou R, Deyo R, Friedly J, et al. Systemic pharmacologic therapies for low back pain: a systematic review for an American College of Physicians clinical practice guideline. Ann Intern Med. 2017;166:480-492.
24. Skljarevski V, Ossanna M, Liu-Seifert H, et al. A double-blind, randomized trial of duloxetine versus placebo in the management of chronic low back pain. Eur J Neurol. 2009;16:1041-1048.
25. Desipramine hydrochloride. In: Brayfield A, ed. Martindale: The Complete Drug Reference. 38th ed. London, England: Pharmaceutical Press; 2014.
26. Hearn L, Moore RA, Derry S, et al. Desipramine for neuropathic pain in adults. Cochrane Database Syst Rev. 2014;(9):CD011003.
27. Dworkin RH, O’Connor AB, Audette J, et al. Recommendations for the pharmacological management of neuropathic pain: an overview and literature update. Mayo Clin Proc. 2010;85(suppl 3):S3-S14.
28. Downie A, Williams CM, Henschke N, et al. Red flags to screen for malignancy and fracture in patients with low back pain: systematic review. BMJ. 2013;347:f7095.
29. Abdel Shaheed C, McFarlane B, Maher CG, et al. Investigating the primary care management of low back pain: a simulated patient study. J Pain. 2016;17:27-35.
30. Finckh A, Zufferey P, Schurch MA, et al. Short-term efficacy of intravenous pulse glucocorticoids in acute discogenic sciatica. A randomized controlled trial. Spine (Phila Pa 1976). 2006;31:377-381.
31. McCleane GJ. Does gabapentin have an analgesic effect on background, movement and referred pain? A randomised, double-blind, placebo controlled study. Pain Clinic. 2001;13:103-107.
32. Yildirim K, Sisecioglu M, Karatay S, et al. The effectiveness of gabapentin in patients with chronic radiculopathy. Pain Clinic. 2003;15:213-218.
33. Micromedex 2.0 [online database]. Greenwood Village, CO: Truven Health Analytics, Inc. www.micromedexsolutions.com. Accessed March 3, 2017.
To comment on this article, contact rdavidson@uspharmacist.com.





