US Pharm. 2024;49(3):17-21.
Headaches represent a prevalent health issue experienced by individuals throughout their lives and frequently constitute a common complaint encountered by health practitioners in emergency department settings, particularly among adults aged 18 to 44 years in the United States. According to a 2021 National Health Interview Survey, 4.3% of adults reported being troubled by headaches or migraines in the past 3 months, with women exhibiting a higher percentage (6.2%) than men (2.2%). A headache is defined as a sensation of pressure in the head or face, manifesting as throbbing, constant, sharp, or dull pain, with variations in type, severity, frequency, and location.1,2
Headaches can be categorized into primary and secondary types. Primary headaches arise from issues or overactivity in pain-sensitive structures within the head, unrelated to an underlying disease. Examples include cluster headaches, migraines (with or without aura), and tension headaches. Secondary headaches result from an underlying disease activating pain-sensitive nerves in the head.3
The impact of headaches on one’s quality of life is significant, potentially leading to missed work, social events, and responsibilities, thereby incurring indirect costs on overall life experiences. Additionally, there are intangible costs associated with the physical and mental pain endured during headache episodes. Pharmacists play a crucial role in mitigating the impact of headaches by educating patients and recommending various treatment options, such as OTC products, nonpharmacologic approaches, self-care strategies, or advising patients to seek further medical attention from their healthcare provider.
DIFFERENT TYPES OF HEADACHES
Various types of headaches exist, classified into primary and secondary categories based on their underlying causes. Primary headaches, characterized by abnormal activity in pain-sensitive head structures, include cluster headaches, migraine with aura, migraine without aura, and tension headaches.
Cluster Headache
Cluster headaches are characterized by their intense pain, earning them the grim moniker “suicide headache.” This type of headache is predominantly observed in men and is known for its episodic nature, manifesting in cycles lasting 2 weeks to 3 months. Remarkably, individuals may experience up to eight episodes in a single day, each marked by severe unilateral orbital pain lasting between 15 minutes and 3 hours. These debilitating episodes are often accompanied by a distinctive set of symptoms, including increased lacrimation (tearing), nasal congestion, nasal discharge, partial Horner’s syndrome, and restlessness. Notably, the temporal pattern of cluster headaches tends to be consistent, with episodes recurring around the same time each year. The absence of remission for more than a month categorizes the condition as chronic cluster headaches. Genetic predisposition and familial gene linkage have been identified as contributing factors to cluster headaches. Research suggests that individuals with certain genetic characteristics may be more susceptible to this type of headache. Additionally, several environmental factors and lifestyle habits have been recognized as triggers that can heighten the likelihood and severity of cluster headaches. These triggers include alcohol consumption, gender (with a higher prevalence in males), and smoking.4,5
Migraine
Migraine, a complex and often debilitating neurologic condition, can manifest with or without aura and reversible nervous system symptoms that typically involve visual or sensory disturbances. The progression of a migraine unfolds through four distinct phases: prodrome, aura, headache phase, and postdrome.
The prodrome phase, present in approximately 60% of migraine patients, precedes the actual headache by hours to days. During this phase, individuals may experience various symptoms, including but not limited to depression, hyperactivity, cognitive changes, frequent urination, irritability, euphoria, neck pain, neck stiffness, fatigue, and food cravings. Recognizing these early signs is crucial for timely intervention. Following the prodrome phase, some individuals may undergo an aura, which entails fully reversible nervous system symptoms. Auras are commonly visual or sensory in nature and gradually develop before subsiding. These symptoms may include visual disturbances, such as flashing lights or zigzag lines, or sensory phenomena like tingling sensations. The aura phase is unique to certain migraine presentations. The hallmark of migraines is the headache phase, characterized by a unilateral headache with moderate to severe intensity. This phase is often accompanied by additional symptoms like nausea, vomiting, and heightened sensitivity to light and sound. The duration and intensity of the headache can vary, and its impact on daily activities can be substantial. Following the resolution of the headache, individuals may enter the postdrome phase. This stage is marked by lingering symptoms such as abnormal concentration and fatigue. It represents a period of recovery and readjustment as the individual returns to baseline neurologic function.4,6
Numerous risk factors have been identified in association with migraines. These include advanced age, lower socioeconomic status, caffeine consumption, medication overuse, stress, sleep problems, obesity, pain syndrome, and conditions characterized by proinflammatory or prothrombotic states.4,6
Tension-Type Headache
Tension-type headaches, while less severe than some other types, are the most prevalent and are defined by a distinctive set of characteristics. These headaches are typically described as a dull, bilateral pressure with mild-to-moderate intensity, centered on the forehead and temples, resulting in discomfort. To simplify, individuals often liken the sensation to having a tight band encircling their head, creating both pressure and pain.
Several risk factors have been associated with the development of tension-type headaches, emphasizing the importance of recognizing and addressing these contributors. Individuals with a perception of poor overall health may be more susceptible to tension-type headaches. Factors such as psychological well-being and self-assessment of health play a role in the onset and frequency of these headaches. Inadequate or poor-quality sleep is a recognized risk factor for tension-type headaches. Sleep plays a crucial role in overall health and well-being, and disruptions in sleep patterns can contribute to the development and exacerbation of these headaches. High levels of stress and the inability to unwind after work have been linked to tension-type headaches. Prolonged periods of stress and tension can contribute to the development of chronic headaches, underscoring the importance of effective stress-management strategies.4,7
Secondary Headache
Secondary headaches result from an underlying condition causing traction or inflammation of pain-sensitive structures in the head. Although less common than primary headaches, recognizing secondary headaches is crucial, as they may signal life-threatening conditions such as trauma, infection, dehydration, homeostatic disorders, vascular disease, sinus-related issues, medication overuse, and drug withdrawal. A headache is considered secondary if it correlates with the underlying condition’s development and improves with its recovery.8
ROLE OF THE PHARMACIST IN SELF-CARE MANAGEMENT
Pharmacists play a pivotal role in ensuring that patients receive safe and informed treatment, extending beyond prescription medications to encompass comprehensive healthcare guidance. Despite common misconceptions, pharmacists are integral in advising and educating individuals on selecting appropriate OTC products, ensuring proper medication usage, identifying potential interactions, providing self-care advice, suggesting nonpharmacologic approaches, and determining the need for physician referral. When recommending OTC products, pharmacists consider various factors, such as medication allergies, concurrent medications, underlying conditions, pregnancy or breastfeeding status, age, budget considerations, and other relevant factors, to make personalized and safe recommendations.
Headaches can typically be addressed using OTC products and nonpharmacologic interventions, guided by the assessment and advice provided by pharmacists. When a patient approaches the pharmacist with a headache complaint, an evaluation is conducted, encompassing an exploration of the pain’s severity, gathering additional information on medical and medication history, and determining any prior attempted treatments. Exclusions for self-treatment are considered, especially if the headache presents specific characteristics that warrant attention, helping the pharmacist discern whether the patient is suitable for self-treatment.
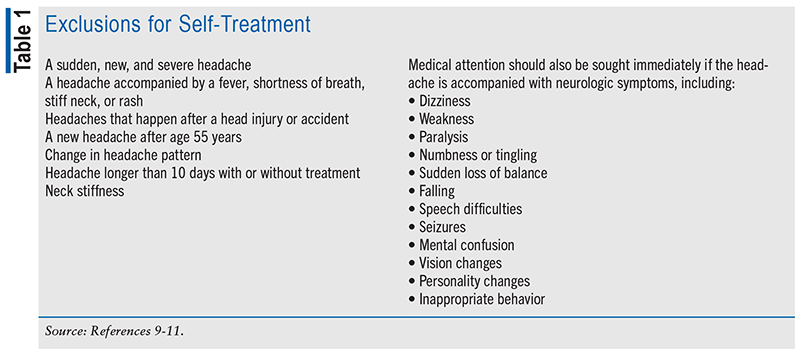
Distinctive features of headaches that necessitate immediate medical care are outlined in TABLE 1. Additional exclusions for self-treatment encompass individuals aged younger than 8 years, women in their last trimester of pregnancy, those with a new headache during pregnancy, secondary headaches associated with underlying pathology (except for minor sinus headache, cluster headaches, and symptoms consistent with migraines lacking a formal diagnosis), those with a history of liver disease or daily consumption of three or more alcoholic drinks, and individuals with high-risk comorbid conditions (such as cancer or HIV). Patients meeting these criteria are advised to seek further medical attention from their doctor. Additionally, considerations for special populations are essential in the pharmacist’s assessment and product recommendations, including the patient’s age (especially those aged younger than 18 years or older than 65 years), pregnancy/breastfeeding status, current medications (especially anticoagulants), alcohol use, and medical history involving conditions like asthma, nasal polyps, gastrointestinal ulcers, gout, recent surgery, coagulation disorders, congestive heart failure, kidney disease, and aspirin allergy.9-11
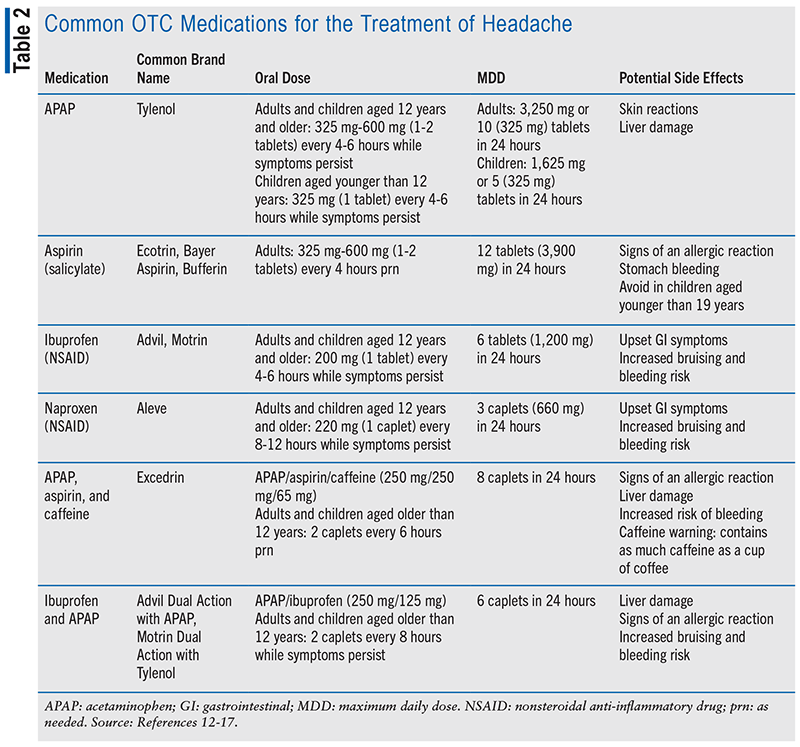
In managing headaches, patients often achieve satisfactory relief through nonprescription medication and/or nonpharmacologic interventions. However, for some patients with severe or chronic headaches and those with a history of inadequate response to previous treatments, prescription options may be considered, necessitating referral to a physician. The available nonprescription medications commonly used for the self-treatment of headaches include acetaminophen and nonsteroidal anti-inflammatory drugs, such as ibuprofen, naproxen, and salicylates. Pharmacists conduct a thorough review of the patient’s profile, including medical and medication histories, to guide them in selecting the most suitable nonprescription analgesic. TABLE 2 outlines common OTC treatment options for headaches, detailing their recommended dosing, frequency, duration, side effects, and special considerations. Patients should be advised to use these OTC products intermittently, up to three times a week.9-11
It is noteworthy that not every headache necessitates medication. Nonpharmacologic treatments can be initial or supplementary options for patients experiencing headaches. Self-care strategies include resting in a dark and quiet room, stretching, taking a walk, applying heat or cooling pads, and massaging the head, neck, or back. Individualized approaches to occasional headache management are crucial, as triggers vary between individuals. Identifying and avoiding triggers can potentially prevent headaches altogether. Maintaining a headache journal, recording instances, frequency, duration, related symptoms, precipitating factors, medications used, and menstrual schedule, is a valuable tool. Common triggers include stress, specific scents, certain foods, inadequate sleep, dehydration, alcohol, nicotine, skipped meals, and poor posture, emphasizing the importance of recording when headaches tend to occur.9-11
CONCLUSION
Headaches present a widespread health concern, particularly among adults aged 18 to 44 years in the U.S. The impact of headaches on daily life is substantial, encompassing missed work, social events, and responsibilities. The role of pharmacists in self-care management is pivotal, as they assess the severity of the headache, gather medical and medication history, and determine the suitability of self-treatment. Pharmacists provide patient education on OTC products and offer valuable self-care advice for the management of headaches. The pharmacist’s role in self-care management is highlighted as a crucial component, involving careful evaluation of headache severity, medical history, and exclusions for self-treatment.
What Are the Risk Factors of Headaches?
There are several risk factors that are possibly associated with causing a primary headache. These include family history, alcohol, smoking, advanced age, caffeine, medications, sleep problems, obesity, pain syndrome, poor self-related health, stress, and inability to relax.
What Are the Different Types of Headaches?
The most common types of primary headaches include migraine, tension-type headaches, and cluster headaches. They all range in differences of frequency, severity, length, and location. Tension-type headaches can be recurrent, lasting from a minute to weeks, have mild-to-moderate intensity, and are bilateral in location. Migraines are episodic headaches that have features associated with them, such as sensitivity to light, sound, or movement; they can occur with or without aura. Lastly, there are cluster headaches, which are rare but more severe and are even referred to as “suicide headache.” They cause a severe unilateral headache that lasts from 15 minutes to 2 hours and can occur up to eight times daily.
How Are Headaches Treated?
Not all headaches require a physician’s attention. Some can be treated at home using OTC products and nonpharmacologic treatments. Some products that have been found to be beneficial in treating a headache can be found OTC at your local pharmacy, including acetaminophen, ibuprofen, naproxen, and aspirin. Some nonpharmacologic treatments that have been found to be helpful in getting rid of a headache include resting in a dark and quiet room, taking a walk, doing stretches, applying hot or cold packs to your forehead, and massaging your head and neck. It is recommended to speak to your local pharmacist to seek advice on how to treat a headache because he or she can determine what OTC product to select, identify any potential interactions, give self-care advice, and share nonpharmacologic approaches and preventive measures, and he or she is able to distinguish whether you should be referred to a healthcare provider for further evaluation.
What Can I Do to Prevent a Headache?
The key to preventing a headache is to figure out what triggers it. If you are prone to experiencing headaches, having a headache journal to record frequency, duration, precipitating factors, and other symptoms can help in identifying patterns and potential triggers. Once a trigger is identified, you can ultimately avoid or minimize your headaches. Triggers can be due to lifestyle factors or situations such as certain foods, alcohol, nicotine, lack of sleep, changes in sleep, posture, lack of water, skipping meals, certain scents, motion sickness, loud or sudden noises, depression/anxiety, hormonal changes, lights, and stress. Being able to manage or avoid triggers can overall aid in the prevention of a headache.
Where Can I Go to Learn More?
American Headache Society: https://americanheadachesociety.org/resources/infographics/
National Headache Foundation: https://headaches.org/resources/
National Institute of Neurological Disorders and Stroke: https://www.ninds.nih.gov/health-information/disorders/headache
REFERENCES
1. Cleveland Clinic. Headaches. https://my.clevelandclinic.org/health/diseases/9639-headaches. Accessed February 2, 2024.
2. QuickStats: percentage of adults aged ≥18 years who have been bothered a lot by headache or migraine in the past 3 months, by sex and age group—National Health Interview Survey, 2021. MMWR Morb Mortal Wkly Rep. 2023;72:611.
3. Mayo Clinic. Headache. June 3, 2020. www.mayoclinic.org/symptoms/headache/basics/definition/sym-20050800. Accessed February 2, 2024.
4. Rizzoli P, Mullally WJ. Headache. Am J Med. 2018;131(1):17-24.
5. Elbadawi ASA, Albalawi AFA, Alghannami AK, et al. Cluster headache and associated risk factors: a systemic review and meta-analysis. Cureus. 2021;13(11):e19294.
6. Amiri P, Kazeminasab S, Nejadghaderi SA, et al. Migraine: a review on its history, global epidemiology, risk factors, and comorbidities. Front Neurol. 2022;12:800605.
7. Chowdhury D. Tension type headache. Ann Indian Acad Neurol. 2012;15(Suppl 1):S83-S88.
8. Ahmed F. Headache disorders: differentiating and managing the common subtypes. Br J Pain. 2012;6(3):124-132.
9. Beithon J, Gallenberg M, Johnson K, et al. Diagnosis and treatment of headache. January 2013. Institute for Clinical Systems Improvement. https://www.icsi.org/wp-content/uploads/2019/01/Headache.pdf. Accessed February 16, 2024.
10. Hainer BL, Matheson EM. Approach to acute headache in adults. Am Fam Physician. 2013;87(10):682-687.
11. Becker WJ. Acute migraine treatment in adults. Headache. 2015;55(6):778-793.
12. DailyMed. TYLENOL REGULAR STRENGTH- acetaminophen tablet, film coated. www.dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=01f41fae-4abb-4b96-ab09-a7d3dfc286cd. Accessed February 5, 2024.
13. DailyMed. ASPIRIN 325MG- aspirin tablet. www.dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=73e74c1c-a556-4d2b-a15e-fd2786ea057d. Accessed February 5, 2024.
14. DailyMed. IBUPROFEN 200MG- ibuprofen tablet. www.dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=f3f12b86-89dc-427e-a26f-728be6f73e7b. Accessed February 5, 2024.
15. DailyMed. BASIC CARE NAPROXEN SODIUM- naproxen sodium tablet, film coated. www.dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=d5c185d9-0bea-4970-b1e7-201a51106ad6. Accessed February 5, 2024.
16. DailyMed. EXCEDRIN EXTRA STRENGTH AND EXCEDRIN TENSION HEADACHE (acetaminophen, aspirin- nsaid, and caffeine kit). www.dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=2c8df1c7-7864-48df-939c-d9ae22e0f52c. Accessed February 5, 2024.
17. DailyMed. ADVIL DUAL ACTION WITH ACETAMINOPHEN- ibuprofen, acetaminophen tablet, film coated. www.dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=f5ea858e-76d9-4777-b3dc-5d614f66d485. Accessed February 5, 2024.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





