US Pharm. 2014;39(11):HS18-HS25.
ABSTRACT: As the population ages, so increases the percentage of individuals challenged by dementia. Dementia is a progressively degenerative neurologic condition associated with Alzheimer’s disease as well as other conditions including vascular and Lewy body dementia. Since there is no cure for dementia, clinicians must look for clinical opportunities to slow the progression of the disease while maintaining the highest quality of life and independence for the patient. It is often the behavioral symptoms associated with the progression of dementia that lead to inpatient hospitalization and institutionalization and thus should be an additional clinical priority.
With the age and life expectancy of the overall population increasing, so too are the number of people diagnosed with dementia. By 2050, the number of Americans aged >65 years is projected to be 88.5 million, more than double the number in 2010.1
Dementia Background
While dementia results from a number of neurologic conditions, Alzheimer’s disease (AD) is responsible for the greatest number of dementia cases.2 Dementia diagnosis and treatment are based on the severity of illness. The patient’s disease severity and degree of behavioral symptoms have significant impact on both informal and formal caregivers. It is behavioral symptoms that are often the catalyst for earlier institutionalization of patients, resulting in increased overall healthcare costs and unnecessary displacement of patients from their home.3 For this reason, special consideration must be given to the associated behavioral symptoms of dementia along with a focus on slowing the disease’s progression and severity.
Other causes of dementia include vascular and other neurodegenerative diseases such as Lewy body dementia and Parkinson’s disease. HIV, head trauma, Huntington disease and other general medical conditions can also cause dementia. Symptoms of dementia can mimic those of other conditions; therefore, the healthcare team must rule out other potential causes such as untreated HIV, syphilis, endocrine disorders (hypothyroidism, hypercalcemia, hypoglycemia), vitamin deficiency (thiamin, niacin), immune disorders (lupus), and other neurologic conditions in order to avoid confusing or delaying appropriate treatment.4
The newly released Diagnostic Statistical Manual of Mental Disorders, Fifth Edition (DSM-5 ) categorizes dementia and other neurocognitive disorders as either major or mild.5 Major neurocognitive disorder is evidenced by profound cognitive decline in one or more areas including, but not limited to, memory, attention, language, and executive function. Cognitive decline should be supported by clinical assessments and neuropsychological testing, and the decline should represent impairment in one’s ability to perform activities of daily living. Memory impairment is a prominent early symptom and is required to make a diagnosis of dementia. Another symptom is a decreased ability to learn new information and/or forgetting previously learned material. Deterioration in language function (aphasia) is often seen when the patient has difficulty in providing names of items and people. Late stages of dementia are often characterized by echolalia (echoing what is heard).6
Behavioral Disturbances
While dementia is well recognized as a disorder that progressively deteriorates, the associated behavioral disturbances may unnecessarily hasten a patient’s loss of quality of life as well as lead to inpatient hospitalization and institutionalization (placement in a long-term care facility). These behavioral manifestations in dementia include agitation, aggression, psychosis, and purposeless wandering. Delusions and disruptive behaviors including aggression and screaming are reported to be among the most disturbing to caregivers. Despite an overlap of symptoms between dementia types, studies comparing vascular dementia and AD have demonstrated greater incidence and severity of depression in patients with vascular dementia.7 Often these behaviors worsen at night and have been termed sundowning, linking the worsening behaviors with the time the sun sets in the evening. Disinhibition also can be seen in this population, which can be worsened by drug therapy such as antihistamines and benzodiazepines. For patients experiencing early signs of dementia, mood changes and increased anxiety may actually be more prominent than memory loss, so healthcare providers and family members should be alerted to report and document such changes.
Pharmacists can play a significant role in both the recognition of these behaviors and the provision of therapeutic recommendations to mitigate these disturbances. When considering treatment options, it is important to focus on a specific symptom or behavior that is responsive to drug therapy.
Treatment for the behavioral disturbances in institutionalized patients with dementia is challenging. The FDA has not approved any medication specifically for the treatment of behavioral symptoms in dementia. This lack of FDA-approved medication, along with the limitations imposed by the Omnibus Budget Reconciliation Act of 1987 (OBRA) and the American Geriatric Society BEERS Criteria for Potentially Inappropriate Medication Use in Older Adults, prescribers may find themselves without viable, flexible alternatives for patients with severe refractory symptomatic illness.8-10 These restrictions have encouraged many to explore off-label prescribing, including the use of polypharmacy in an effort to reduce behavioral symptoms. The use of polypharmacy in older adults can greatly increase the risk of drug-drug interactions and adverse drug reactions. Acute symptoms of increased confusion, psychosis, and psychomotor retardation (withdrawal) can be signs of delirium, which is a common co-occurring condition in patients with dementia.
Special Considerations for the Cholinesterase or AChE Inhibitors
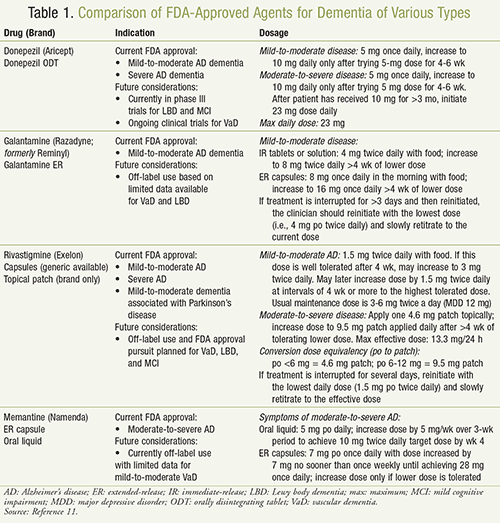
FDA-approved agents for the treatment of dementia target the cholinergic deficit that causes this disorder. The cholinergic system is responsible for modulating excitatory amino acid transmission and processing. The progressive loss of cholinergic neurons and cholinergic function results in memory deficits as well as a decreased ability to engage in activities of daily living. This decreased acetylcholinesterase (AChE) activity is believed to be the core cause of dementia, thus making the cholinesterase or AChE inhibitors the first-line agents approved by the FDA for use in dementia. Rivastigmine and galantamine are approved for use in mild-to-moderate AD, and donepezil is approved for use in mild-to-moderate and moderate-to-severe disease (TABLE 1).11
These drugs inhibit the enzyme responsible for the destruction of acetylcholine (ACh), thus increasing its availability. ACh stimulates gastric acid secretion and therefore represents class-related adverse effects, including nausea, vomiting, and aggravation of preexisting conditions such as peptic ulcer disease. Caution is recommended for patients on nonsteroidal anti-inflammatory drug (NSAID) therapy due to an increased risk of gastrointestinal (GI) bleeding. Additional class warnings encompass use in patients with chronic obstructive pulmonary disease (COPD) and asthma. Peripheral ACh activity includes increased bronchial secretion and spasm; thus, the drug-induced cholinergic enhancement increases the risk of complications in patients with underlying pulmonary disorders. Increased risk of seizures is possible as a result of the decreased seizure threshold caused by dementia. Bradycardia due to increased vagal tone and bladder outflow constriction are additional clinical concerns when ACh activity is increased through the use of AChE inhibitors. Drug interactions are specific to the agent prescribed; however, any medication that has “anticholinergic” qualities will decrease the beneficial effect of the AChE inhibitors.11
Anticholinergic medications may include traditional histamine-1 (H1) antagonists, but also include antipsychotic agents used to address behavioral symptoms of dementia. Caution must be taken to address treatment interruptions so that both the patient and the prescriber are aware of the need to reintroduce therapy at the initial starting dose to avoid severe gastric reactions and potential gastric rupture.7 Slow-dose escalation is recommended to achieve the maximum clinical benefit seen at the lowest effective doses of these agents. In order to prevent intolerable adverse GI side effects, patients must be encouraged to maintain adequate hydration and fluid intake throughout the course of cholinesterase therapy. For inpatients, the goal of ensuring adequate fluid intake must be a priority of the treatment team.
NMDA Receptor Antagonist
Another therapeutic mechanism is antagonizing the excitatory effects of glutamate and slowing the influx and accumulation of intracellular calcium. Memory and learning are thought to be associated with glutamate activation at the N-methyl-d-aspartate (NMDA) receptor; however, chronic excessive excitation may lead to the neuronal damage responsible for AD and other related neurologic disorders. Memantine is an NMDA receptor antagonist that may be used as monotherapy in moderate-to-severe AD or in combination with cholinesterase inhibitors (see TABLE 1 for full description).11 There have been no robust findings in favor of using combined treatment of NMDA antagonist and AChE inhibitors for mild-to-moderate disease; however, in severe dementia the combination has shown some additional benefit over either agent alone.11 Switching drugs within the AChE inhibitor class can also prove to be an additional option that may provide benefit to patients who either cannot tolerate a drug or find that there is no benefit to the current agent they are taking.
As with the AChE inhibitors, memantine should also be used cautiously in patients with underlying seizure disorders, as data are lacking for the potential confounding effects with underlying worsening dementia syndromes. Patients who have conditions of the urinary system that can increase urine pH, such as infection, obstruction, and/or chronic renal failure, will be subject to increased serum concentrations of memantine.11
Other Agents Used for Behavioral Symptoms Associated With Dementia
Antipsychotics: Both first- and second-generation antipsychotic agents have been used to address the behavioral symptoms experienced by patients with dementia. This class of medication has been subject to FDA scrutiny, and subsequent black box warnings have been issued to address the increased risk of cerebrovascular adverse events such as stroke and transient ischemic attacks. While the first black box warning was issued in 2003 related to studies involving risperidone, the FDA has issued additional warnings, and in 2005 expanded the black box to all atypical agents specific to increased all-cause mortality for patients diagnosed with dementia.12 This black box warning, in addition to the warnings issued on the metabolic complications attributed to the use of second-generation agents (SGAs), has fostered renewed interest in using the first-generation agents (FGAs) for behavioral disturbances in institutionalized patients with dementia; however, studies examining the safety of FGAs used in dementia populations demonstrated even higher mortality rates versus those for SGAs.12 The use of higher doses of the SGAs was associated with increased mortality and more commonly occurred in the early period of initiation.
Based on the data on studies done by Wang et al and others, the FDA expanded the all-cause mortality black box warning to all antipsychotic agents in 2008.13 The FDA has also evaluated specific agents as to their risk of causing cerebrovascular accidents and, subsequently, required risperidone, aripiprazole, and olanzapine to have an agent-specific warning in the package insert.11
With such risk, where is the benefit in using these agents? It is well recognized that while behavioral disturbances can have a significantly negative impact on the quality of life of patients and families, many people are willing to accept the risks. There are a number of studies that show inconsistent benefit with a variety of different agents; however, the Clinical Antipsychotic Trials in Intervention Effectiveness–Alzheimer’s Disease (CATIE-AD) showed limited efficacy and overall poor tolerability of second-generation antipsychotic agents in patients diagnosed with dementia.14 Based on CATIE-AD, limits have been established on the use of these agents through agencies such as the Centers for Medicare and Medicaid Services (CMS) to avoid inappropriate prescribing, reserving use only for patients who would be expected to show improvement and experience minimal adverse effects with these agents.
Antidepressants: Antidepressants are effective and well-tolerated alternative agents to antipsychotic agents for patients with behavioral and psychological symptoms in dementia, including anxiety and agitation. The selective serotonin reuptake inhibitors (SSRIs) are recommended as first-line treatment options for depression in the elderly because they have an improved tolerability profile, causing fewer anticholinergic and cardiovascular adverse effects than the TCAs, and they are not usually associated with significant weight gain.15 Some studies have demonstrated benefit with citalopram in treating disinhibition and irritability in addition to depression in this population; however, the QTc prolonging effects of citalopram in the elderly have resulted in FDA recommendations to reduce the dosage to £20 mg/day in patients >60 years of age.11 All SSRIs, when combined with aspirin and NSAIDs, increase the risk of GI bleeding, so prescribers must manage this risk but not discourage the use of antidepressants in this population, which is at increased risk of suicide and other significant complications of untreated depression.11
Benzodiazepines: These agents (e.g., alprazolam, diazepam, lorazepam), despite the risks of cognitive impairment, inclusion on the Beers list, and dependence and paradoxical inhibition, have been used regularly to address the behavioral symptoms in those diagnosed with dementia.16 The benzodiazepines decrease sleep latency, decrease anxiety, and provide muscle relaxant effects. There is some evidence that benzodiazepines may also be effective in reversing catatonia, which is a condition that can resemble dementia and may complicate behavioral disturbances in patients diagnosed with dementia.17 Benzodiazepines are associated with increased risk of falls and respiratory depression in older adults, so these agents should be used with caution if considered for use at all.
Mood Stabilizers: Mood-stabilizing antiepileptic drugs (AEDs) have been available for use for a number of FDA-approved (and off-label) medical and psychiatric indications.11 The use of these AEDs in treating the behavioral symptoms of dementia has a less clear documented benefit. Divalproex and valproic acid derivatives have been studied in patients exhibiting aggression, agitation, and disinhibition with variable results in those with dementia. One specific meta-analysis evaluated the use of valproic acid in patients in long-term care institutions and found that the low doses needed to avoid the adverse effects of the drug were not effective in managing behavioral disturbances.18 Other mood stabilizers such carbamazepine and lithium were limited by severe adverse effects seen when used in older patients.19 Treatment regimens that have included AEDs have shown some promise for a subset of dementia patients, often allowing a reduction of dose for antipsychotics; however, due to the inconsistent results in drug studies, they are not recommended for routine use.
Conclusion
What is on the horizon? While we wait for novel therapeutic compounds to be released, research to evaluate the outcomes of combination therapy with current agents and guidelines can be focused on providing a clearer picture of when treatment interventions are no longer truly clinically effective. As we explore future treatments for dementia, we must recognize the impact on current patients and caregivers and how, as pharmacists, we can provide support with education about the medications used for dementia (TABLE 2).11

REFERENCES
1. Vincent GK, Velkoff, VA. The Next Four Decades: The Older Population in the United States: 2010 to 2050. Washington, DC: U.S. Census Bureau; May 2010. www.census.gov/prod/2010pubs/p25-1138.pdf. Accessed September 1, 2014.
2. Group Health Cooperative. Dementia and cognitive impairment: diagnosis and treatment guideline. December 2012. www.ghc.org/all-sites/guidelines/dementia.pdf. Accessed October 14, 2014.
3. Chan DC, Kasper JD, Black BS, Rabins PV. Presence of behavioral and psychological symptoms predicts nursing home placement in community dwelling elders with cognitive impairment in univariate but not multivariate analysis. J Gerontol A Biol Sci Med Sci. 2003;58:548-554.
4. McCormick E, Ripp J. Dementia. Philadelphia, PA: American College of Physicians; 2013.
5. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Arlington, VA: American Psychiatric Publishing; 2013.
6. Herrmann N, Lanctôt KL, Sambrook R, et al. The contribution of neuropsychiatric symptoms to the cost of dementia care. Int J Geriatr Psychiatry. 2006;21:972-976.
7. Staekenborg SS, Su T, van Straaten EC, et al. Behavioural and psychological symptoms in vascular dementia; differences between small and large vessel disease. J Neurol Neurosurg Psychiatr. 2010;81:547-551.
8. Omnibus Budget Reconciliation Act of 1987 (OBRA). Subtitle C, nursing home reform. PL100-203. Washington, DC: National Coalition for Nursing Home Reform; 1987.
9. Health Care Financing Administration. Survey Procedures and Interpretive Guidelines for Skilled Nursing Facilities and Intermediate Care Facilities. Baltimore, MD: U.S. Department of Health and Human Services; 1990.
10. AGS Beers criteria for potentially inappropriate medication use in older adults. American Geriatric Society; 2012. www.americangeriatrics.org/files/documents/beers/PrintableBeersPocketCard.pdf. Accessed August 26, 2014.
11. Clinical Pharmacology [online database]. Tampa, FL: Gold Standard, Inc; 2013. www.clinicalpharmacology.com. Accessed August 1, 2014.
12. Casey DA. Pharmacological management of behavioral disturbance in dementia. P T. 2007;32(10):560-566.
13. Wang PS, Schneeweiss S, Avorn J, et al. Risk of death in elderly users of conventional vs. atypical antipsychotic medications. N Engl J Med. 2005;353(22):2335-2341.
14. Schneider LS, Tariot PN, Dagerman KS, et al. The CATIE-AD Study Group. Effectiveness of atypical antipsychotic drugs in patients with Alzheimer’s disease. N Engl J Med. 2006;355(15):1525-1538.
15. DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Patho-physiologic Approach. 8th ed. New York, NY: McGraw-Hill; 2011:539-541.
16. Cerejeira J, Lagarto L, Mukaetova-Ladinska EB. Behavioral and psychological symptoms of dementia. Front Neurol. 2012;3(73):10-20.
17. Alisky JM. Lorazepam-reversible catatonia in the elderly can mimic dementia, coma and stroke. Age Ageing. 2007;36(2):229.
18. Longergan ET, Cameron M, Luxenberg J. Valproic acid for agitation in dementia. Cochrane Database Syst Rev. 2004;(2):CD003945.
19. Cummings JL, McRae T, Zhang R; Donepezil-Sertraline Study Group. Effects of donepezil on neuropsychiatric symptoms patients with dementia and severe behavioral disorders. Am J Geriatric Psychiatry. 2006;14:605-612.
To comment on this article, contact rdavidson@uspharmacist.com.






