US Pharm. 2020;45(4):5-8.
Colorectal cancer is the third leading cause of cancer-related deaths in the United States and the third most common cancer affecting both men and women.1,2 Although the rate at which people are diagnosed with colorectal cancer has been decreasing, there are still more than 1.3 million Americans currently living with colorectal cancer. In 2019, there were approximately 145,600 new cases of colorectal cancer and 51,020 deaths. In 2020, these numbers are expected to increase to 147,950 and 53,200, respectively. The overall expected 5-year survival rate is 64.4%; however, the earlier colorectal cancer is detected the better chance for survival. The 5-year survival for localized colorectal cancer is 89.9% compared with approximately 14% in patients diagnosed with distant colorectal cancer.1,3 This fact alone illustrates that early detection is very important.
Proper screening and education about colorectal cancer are vital in reducing its impact and burden. Typically, colorectal cancer originates from benign adenomatous polyps that slowly increase in size, ultimately progressing to dysplasia and cancer. This progression can take many years to occur, varying from 5 years or less to more than 20 years. Most patients will not present with any signs or symptoms of colorectal cancer; if signs and symptoms are present, this is indicative of a more advanced stage of colorectal cancer.4,5 Colorectal cancer screenings can detect these benign polyps, resulting in their removal prior to causing cancer. As the most accessible healthcare professional, pharmacists are in a unique position to help patients by increasing awareness about colorectal cancer and by promoting colorectal cancer screenings.
Risk Factors and Prevention
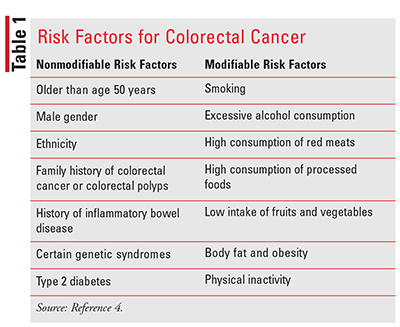
There is no single identified risk factor for the development of colorectal cancer; heredity, environmental, and lifestyle factors all play a role (TABLE 1). Male gender and increasing age have been shown to be strongly associated with increased risk. Males have approximately a 1.5-fold greater risk of developing colorectal cancer than do females. Those who are aged 65 years and older are almost three times more likely to be diagnosed with colorectal cancer than patients between the ages of 50 and 64 years and 30 times more likely compared with those between the ages of 25 and 49 years. The median age at diagnosis for colon cancer is 68 years in males and 72 years in females, while the median age for rectal cancer is 63 years in both groups. Variations in ethnicity have also displayed associations, with African Americans and Native Americans having a higher incidence of colorectal cancer.4,6,7
A positive family history and genetic syndromes also seem to influence a patient’s risk. Almost 20% of all patients with colorectal cancer have a positive family history; those with a first-degree relative have up to a four-times higher risk. Hereditary colorectal cancer accounts for approximately 10% of all cases. The most common syndromes associated with colorectal cancer include Lynch syndrome and adenomatous polyposis. In addition, individuals with comorbidities such as inflammatory bowel disease have a twofold risk of developing colorectal cancer.4,6,7
Although hereditary and genetic factors influence a person’s risk for colorectal cancer, modifiable lifestyle factors are greatly responsible for up to 71% of colorectal cancer cases. Smoking, excessive alcohol intake, increased body weight, and physical inactivity are associated with an increased risk. Moderate and heavy alcohol consumption is associated with a 20% or greater risk compared with light drinking (<1 drink/day); this risk is similar to that of prolonged heavy smoking. For every 1-point increase in BMI, a patient’s risk for colorectal cancer increases by about 3%. Diet can also influence colorectal cancer risk. A diet high in red meat and processed food is linked with an estimated 1.16-fold increase per 100 grams of daily intake. Conversely, a diet rich in milk consumption, whole grains, fresh fruits, vegetables, and tree nuts, along with at least 30 minutes of physical activity daily, may prevent the development of colorectal cancer.4,6-9
Certain vitamins and medications may also reduce a patient’s risk. Regular nonsteroidal anti-inflammatory drug (NSAID) and aspirin intake has been associated with up to a 40% risk reduction; the U.S. Preventive Services Task Force recommends the use of low-dose aspirin for the primary prevention of cardiovascular disease and colorectal cancer in adults aged 50 to 69 years. Vitamin D and calcium may also provide a preventive effect, although the data are mixed. A daily intake of 400 international units of vitamin D and calcium intake of up to 1,200 mg/day may help reduce colorectal cancer risk. However, patients should not rely solely on these treatments alone for colorectal cancer risk reduction.9,10
Clinical Presentation
A wide range of signs and symptoms are associated with colorectal cancer. Patient symptoms are usually nonspecific and can vary drastically; however, colorectal cancer is mainly an asymptomatic disease until it reaches advanced stages. Rectal bleeding and blood in the stool are the most common symptoms in both benign colorectal polyps and malignant cases. Patients may also present with changes in bowel habits, nausea, vomiting, and abdominal discomfort. Other symptoms include fatigue and other anemia-related symptoms such as a pale appearance, shortness of breath, and weight loss.4,8
Screening
Colorectal cancer rates have been decreasing by approximately 2% every year. Timely screening for colorectal cancer has been instrumental in decreasing incidence and colorectal cancer-related mortality. Screening helps detect colorectal cancer at an early stage when it is easier to treat and more likely to be curable. Despite this, many patients are not up-to-date with their colorectal cancer screening. In 2016, 68.8% of adults between the ages of 50 and 75 years were up-to-date with their screenings, leaving almost one-third of the population not up-to-date or having never been screened at all.2,11
Several medical organizations have provided recommendations for colorectal cancer screening. They are generally consistent in their recommendation of initiating screening at age 50 years in average-risk patients, defined as an asymptomatic individual with no personal or family history of colorectal cancer or hereditary colorectal syndrome and no personal history of inflammatory bowel disease or abdominal or pelvic radiation. The U.S. Multi-Society Task Force of Colorectal Cancer recommends beginning screenings earlier in the black population because of their higher incidence of disease and higher mortality rates. Recently the American Cancer Society (ACS) updated their recommendations to reflect the growing incidence of colorectal cancer among younger adults. They recommend initiating screening in all average-risk individuals at age 45. The decision to screen patients older than 75 years should be made on an individualized basis, taking into consideration life expectancy, health status, and prior screenings; screening after 85 years of age is not recommended. Patients who are considered to be at a higher risk for colorectal cancer have different screening recommendations and should be referred to their primary care provider.5,12-16
Screening Tests
There are generally two categories of colorectal cancer screening tests: stool-based tests and direct visualization exams. Stool-based exams are quick and noninvasive, can be done at home, and do not require bowel preparation. However, their usefulness is limited by their inability to detect nonbleeding polyps or cancers. These methods include guaiac-based fecal occult blood test (gFOBT), fecal immunochemical test (FIT), and multitargeted stool DNA test (FIT-DNA). gFOBT evaluates for the presence of blood in the stool by testing for peroxidase activity of heme or hemoglobin. gFOBT is the most commonly used stool-based exam, but it is considered to be less accurate when compared with others. Three stool samples obtained at home on different days should be submitted. Patients should also avoid ingesting certain foods and medications, including red meat, NSAIDs, iron products, or vitamin C before the test to avoid false positives. FIT uses antibodies to human hemoglobin to detect occult blood in the stool. This test has been found to be more sensitive and specific for detecting colorectal cancer when compared to gFOBT. It is more convenient compared with gFOBT because it only requires one stool sample and has no dietary restrictions. A FIT-DNA assay tries to improve the standard FIT by also testing for altered DNA biomarkers that are associated with colon neoplasia. FIT-DNA has been shown to be more sensitive compared with FIT alone, but less specific for detecting colorectal cancer. If any of these tests return a positive result, follow-up with a colonoscopy may be required. It is recommended that these exams be performed on an annual basis, with the exception of FIT-DNA which should be performed every 1-3 years.17,18
Direct visualization tests include colonoscopy, flexible sigmoidoscopy, and computed tomographic colonography. These tests have greater sensitivity compared with stool-based tests and allow for the early identification of adenomatous polyps before they progress to colorectal cancer. They do require the patient to complete a bowel preparation prior to testing; however, because of their increased sensitivity, they are recommended to be performed less often. Colonoscopy is the most widely used screening test for colorectal cancer and is considered the gold standard. This procedure allows for the examination of the entire colon and rectum. Polyps found during the colonoscopy can be removed simultaneously; polyps found utilizing other methods will require a follow-up colonoscopy. It should be performed every 10 years for most patients who are not considered high risk. Colonoscopy does require complete bowel preparation by the patient, ensuring an accurate examination. The procedure also requires sedation and has a higher risk of complications, including bowel perforation and reactions to the bowel prep.17,18
Flexible sigmoidoscopy allows for the inspection of the lower half of the colon and the entire rectum. Using this method along with a stool-based test improves the sensitivity for lesions that may have been missed by sigmoidoscopy alone. This procedure should be repeated every 5 to 10 years. Sedation is not required and patients do not have to undergo a complete bowel evacuation; enemas may be enough. However, the entire colon cannot be examined, and a positive finding will require follow-up with colonoscopy.17,18
Computed tomographic colonography is an imaging procedure, often referred to as a virtual colonoscopy. It provides a less-invasive option, but follow-up with colonoscopy will be needed if any lesions are detected. A computed tomographic colonography should be performed every 5 years. A complete bowel preparation is required but sedation is not necessary.17,18
Role of the Pharmacist
Pharmacists have a tremendous opportunity to promote awareness of colorectal cancer and the importance of screening. As first-line healthcare professionals, pharmacists can educate patients on how certain lifestyle behaviors can influence colorectal cancer risk and encourage patients to incorporate a healthier diet, exercise, and stop smoking. Two common barriers to colorectal screenings are lack of knowledge and lack of provider recommendation.19 Pharmacists are able to help overcome both of these barriers. Pharmacists have the opportunity to educate patients about colorectal screenings, including the benefits associated with their use, current recommendations, and differences between the various screening tools available, as well as to address any reservations or concerns patients may have, especially with bowel preparation. Pharmacists are in a prime position to identify patients who are candidates for screening, referring them to their healthcare provider. For patients who will be undergoing a colonoscopy, pharmacists can ensure the patient’s understanding regarding the importance of the bowel preparation and promote the safe use of these products.
Conclusion
Colorectal cancer is a serious disease that is relatively common, affecting many patients. Prevention and early detection are key to reducing the incidence and mortality associated with colorectal cancer. Lifestyle modifications can help reduce a patient’s risk for developing colorectal cancer. Colorectal cancer screening is a very important tool to help identify lesions early and remove them before they progress to cancer. Pharmacists have the opportunity to educate patients about the significance of colorectal cancer, help promote lifestyle changes, and provide recommendations for colorectal cancer screenings.

Why should I be concerned about colorectal cancer?
Colorectal cancer is the third leading cause of cancer-related deaths in the United States and the third most common cancer affecting both men and women. Many cases could have been prevented with screening. Almost one-third of the population is not up-to-date with colorectal screening.
Who is at risk of getting colorectal cancer?
As you get older, your risk increases. You are at higher risk if you have a family history of colorectal cancer or polyps, if you have inflammatory bowel disease, or if you have certain genetic syndromes. Your lifestyle can also influence your risk. Limiting how much red meat and processed meat you eat and including plenty of fruits and vegetables in your diet may help. Staying active and not smoking will also help reduce your risk.
What are the symptoms of colorectal cancer?
Symptoms can include stomach pain, blood in your stool, a change in bowel movements, and weight loss. But many patients will not experience symptoms, especially at an early stage.
Do I need to be screened for colorectal cancer?
Many people do not know they have colorectal cancer. Screening is a way for doctors to check to see if there are lesions or abnormal growths in the colon and rectum. At age 50 years or older, most people should begin screening. Those who are at an increased risk (patients with a family history; history of inflammatory bowel disease) may be screened at an earlier age. Many people can stop screening at age 75 years.
Are there different screening tests?
Tests that are available include stool-based tests and direct visualization. Stool-based tests check for blood in the stool. These tests will require you to collect stool samples at home and submit them for evaluation. They are easy to use but are less likely to find polyps.
Direct visualization tests allow the doctor to look at your colon and rectum. The most common procedure is a colonoscopy. You will need to clean out your colon before this procedure by using medicines called bowel prep. It is very important to follow the directions carefully. If the bowels are not clear, your provider will not be able to accurately inspect your colon. Other tests include a sigmoidoscopy and computed tomographic colonography, also known as a virtual colonoscopy.
Where can I learn more about colorectal cancer?
You can visit the American Cancer Society: www.cancer.org/cancer/colon-rectal-cancer.html and the CDC: www.cdc.gov/cancer/colorectal/index.htm for further information.
REFERENCES
1. American Cancer Society. Key statistics for colorectal cancer. www.cancer.org/cancer/colon-rectal-cancer/about/key-statistics.html. Accessed February 6, 2020.
2. CDC. Colorectal cancer statistics. Published October 4, 2019. www.cdc.gov/cancer/colorectal/statistics/index.htm. Accessed February 6, 2020.
3. American Cancer Society. Cancer facts & statistics. http://cancerstatisticscenter.cancer.org/. Accessed February 6, 2020.
4. Dekker E, Tanis PJ, Vleugels JLA, et al. Colorectal cancer. Lancet. 2019;394(10207):1467-1480.
5. Qaseem A, Crandall CJ, Mustafa RA, et al. Clinical Guidelines Committee of the American College of Physicians. Screening for colorectal cancer in asymptomatic average-risk adults: a guidance statement from the American College of Physicians. Ann Intern Med. 2019;171(9):643-654.
6. Rawla P, Sunkara T, Barsouk A. Epidemiology of colorectal cancer: incidence, mortality, survival, and risk factors. Prz Gastroenterol. 2019;14(2):89-103.
7. American Cancer Society. Colorectal cancer facts & figures 2017-2019. Atlanta, GA: American Cancer Society; 2017.
8. Kuipers EJ, Grady WM, Lieberman D, et al. Colorectal cancer. Nat Rev Dis Primers. 2015;1:15065.
9. Crosara Teixeira M, Braghiroli MI, Sabbaga J, Hoff PM. Primary prevention of colorectal cancer: myth or reality? World J Gastroenterol. 2014;20(41):15060-15069.
10. U.S. Preventive Services Task Force. Final recommendation statement: aspirin use to prevent cardiovascular disease and colorectal cancer: preventive medication. Published September 2017. www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/aspirin-to-prevent-cardiovascular-disease-and-cancer. Accessed February 6, 2020.
11. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70(1):7-30.
12. Rex DK, Boland CR, Dominitz JA, et al. Colorectal cancer screening: recommendations for physicians and patients from the U.S. Multi-Society Task Force on Colorectal Cancer. Gastroenterology. 2017;153(1):307-323.
13. US Preventive Services Task Force. Screening for colorectal cancer: US Preventive Services Task Force Recommendation Statement. JAMA. 2016;315(23):2564-2575.
14. Wolf AMD, Fontham ETH, Church TR et al. Colorectal cancer screening for average-risk adults: 2018 guideline update from the American Cancer Society. CA Cancer J Clin. 2018;68(4):250-281.
15. Siegel RL, Fedewa SA, Anderson WF, et al. Colorectal cancer incidence patterns in the United States, 1974-2013. J Natl Cancer Inst. 2017;109(8).
16. Meester RGS, Mannalithara A, Lansdorp-Vogelaar I, Ladabaum U. Trends in incidence and stage at diagnosis of colorectal cancer in adults aged 40 through 49 years, 1975-2015. JAMA. 2019;321(19):1933-1934.
17. Wilkins T, McMechan D, Talukder A. Colorectal cancer screening and prevention. Am Fam Physician. 2018;97(10):658-665.
18. Lieberman D, Ladabaum U, Cruz-Correa M, et al. Screening for colorectal cancer and evolving issues for physicians and patients: a review. JAMA. 2016;316(20):2135-2145.
19. Schmidtknecht HL. Increasing colorectal cancer screening uptake in patients: provider-initiated discussion at every primary care patient encounter. J Health Comm. 2017;2(4).
To comment on this article, contact rdavidson@uspharmacist.com.