US Pharm. 2023;48(4):13-20.
ABSTRACT: Asymptomatic bacteriuria (ASB) is the colonization of bacteria in the urinary tract without clinical manifestation of symptoms associated with urinary tract infection (UTI). Treatment of ASB is recommended in only a couple of specific patient populations because of the rise in antibiotic resistance and the lack of treatment benefit in most populations. Pharmacists should counsel patients about when to undergo ASB screening, when UTI screening tests should be used, and when to consult a healthcare provider. An understanding of the recommendations for ASB screening and management is necessary for all pharmacists so that they take an active role in improving health outcomes in individual patients as well as on a larger scale.
The threat of multidrug-resistant (MDR) organisms is rising globally. By 2050, an estimated 10 million people worldwide will die of infections caused by MDR organisms unless significant measures are taken to stop these pathogens from spreading.1 Given this alarming fact, all pharmacists should promote antibiotic stewardship to help reduce unnecessary antibiotic use, which contributes to the rise of MDR organisms.
Asymptomatic bacteriuria (ASB) is defined as the colonization of bacteria in the urinary tract without clinical manifestation of symptoms typically associated with urinary tract infection (UTI). This condition involves the presence of detectable levels of bacterial-species growth in the urine (>105 colony-forming units [CFU]/mL).2,3 ASB has often been treated with antibiotic therapy; however, recent data have shown that most patient populations with ASB should not be treated with antibiotic therapy because of the lack of proven benefit.2
ASB is common in many patient populations, including those with or without underlying comorbidities. The prevalence of ASB in specific populations varies based on factors such as sex, age, and comorbidities. Compared with healthy premenopausal and postmenopausal women, pregnant women with no relevant comorbidities have a higher ASB prevalence range (1.9%-9.5% vs. 1%-5% and 2.8%-8.6%, respectively).2 ASB is more commonly diagnosed in women than in men, and elderly persons are more likely than younger persons to develop ASB.4,5
Factors such as residence in a long-term care (LTC) facility and indwelling catheter use may contribute to an even greater increase in ASB prevalence. For example, ASB has been reported in 15% to 50% of LTC-facility residents, with only a slight variation between men and women.5 Notably, 100% of patients with a long-term indwelling catheter have been reported to have ASB.6 Given the prevalence of ASB among multiple populations as well as increased reports of antibiotic resistance, it is necessary for healthcare professionals, especially pharmacists, to understand the importance of following the most up-to-date, evidence-based approach to the management of ASB in their patients.2,7
Background
Frequently observed pathogens in ASB are consistent with those associated with cystitis and pyelonephritis. The most common pathogen is Escherichia coli, especially in healthy patients with no underlying comorbidities. Additional organisms that are associated with ASB and UTI include other Enterobacteriaceae, Pseudomonas aeruginosa, Enterococcus species, and group B Streptococcus. These pathogens are more often observed in patients who reside in LTC facilities or have underlying comorbidities (e.g., diabetes) or an indwelling catheter.8,9
Contributory factors of the host, bacteria, or both may be responsible for the existence of bacteriuria in the absence of a UTI. For example, a patient’s urinary tract might be colonized with uroprotective Lactobacillus species, or the urine sample might be contaminated since urine samples typically are not obtained in a sterile manner.10 Patients with E coli–colonized ASB may undergo a genetic adaptation that produces a less virulent strain of E coli than in symptomatic bacteriuria, and this may contribute to the lack of symptoms.11
No single definitive etiology of ASB has been identified, as multiple factors have been associated with its development. Anatomy, structure, and function are key factors in the development of bacteriuria. For example, because the female urethra is shorter than the male urethra, bacteria migrate a shorter distance to the bladder and more easily colonize the genitourinary tract. After sexual intercourse, women may briefly develop ASB, but the immune system usually prevents escalation to a UTI. Incomplete voiding of the bladder is another contributor to ASB in elderly persons.4
Clinical Presentation
The site of infection within the urinary tract contributes to the clinical presentation of patients with symptomatic UTI. Acute cystitis is a bacterial infection localized to the bladder whose typical symptoms include dysuria, increased urinary frequency or urgency, and suprapubic pain.12,13 Pyelonephritis is a bacterial infection of the kidney; its symptoms are more systemic and may include flank pain, fever, or chills in addition to the symptoms associated with cystitis.13
A key clinical feature of symptomatic UTIs in the elderly population is that these patients often present with altered mental status (AMS), or delirium. AMS is considered a UTI symptom in this population; however, before a patient with AMS who has no other typical UTI symptoms is screened and treated for UTI, other causes of the AMS should be explored.2 Some noninfectious causes of AMS in elderly patients are a medical history of dementia and medication-induced delirium. Anticholinergics, benzodiazepines, and narcotic analgesics are some of the drugs that can cause medication-induced delirium.14
If a patient is determined have a symptomatic UTI, it is imperative to initiate empiric antibiotic therapy as soon as possible and then individualize it based on urine culture and sensitivity results. On its own, the presence of bacteria in a urine sample does not indicate an infection. Therefore, in the absence of UTI signs or symptoms, ASB usually should not be treated with antibiotics, except for the specific patient populations discussed below.2
Management
Because the rates of extended-spectrum beta-lactamase–, AmpC beta-lactamase–, and carbapenemase-producing strains of Enterobacteriaceae are increasing globally, these MDR infections are becoming more common, and they are often difficult to treat; these factors must be considered in the management of patients with ASB.2,9 The Infectious Diseases Society of America (IDSA) recommends against screening for and treating ASB in most cases because the risks greatly outweigh any potential benefits, especially when the strength of the supporting evidence is considered.2 In most patient populations, ASB is a benign condition that is unlikely to escalate to a UTI.
Selected patient populations that should be screened and treated for ASB include pregnant women and persons undergoing endoscopic urologic procedures with anticipated mucosal trauma.2 In pregnant women, untreated ASB can have negative effects on the fetus, including low birthweight and preterm birth. In patients undergoing urologic procedures with anticipated mucosal trauma, operating in a contaminated field greatly increases the risk of postsurgical infection.2,15 Given insufficient evidence, the IDSA makes no recommendations for patients <1 month post kidney transplantation, patients with high-risk neutropenia (absolute neutrophil count <100 cells/mm3 and >7 days post chemotherapy), or patients undergoing removal of an indwelling catheter.
Decisions regarding screening and treatment of ASB in these populations should be based on the clinician’s expertise and patient-specific factors. Both patients and clinicians should be advised against routinely screening for UTIs in the absence of signs and symptoms unless the criteria for ASB screening are met.2 Asymptomatic patients who meet these criteria will use the dipstick test, gram-stain method, or midstream clean-catch to confirm the presence of bacteriuria.15
To screen for ASB in pregnant patients, the midstream clean-catch method is preferred.15,16 For this test, a urine sample is obtained in a healthcare facility and sent to a microbiology laboratory for culturing and sensitivity testing. To be considered positive for ASB, asymptomatic patients must have two consecutive midstream clean-catch urine specimens of an isolated bacterial species with a quantitative count of >100,000 CFU/mL. Gram stain and dipstick tests may be used to collect urine samples, but neither method gives information on specific bacteria, and they are less accurate than midstream clean-catch testing.15,16
In patients undergoing endoscopic urologic procedures with anticipated mucosal trauma, it is recommended to obtain a urine culture prior to surgery. To treat ASB in these patients, the IDSA recommends initiating a short course of targeted antimicrobial therapy rather than empiric therapy. This targeted therapy should be administered IV in one or two doses 30 to 60 minutes prior to surgery.2
When the criteria for ASB treatment are met, antibiotic therapy is warranted, with variations based on patient-specific factors. Treatment of ASB in these selected populations is similar to that for uncomplicated cystitis. Agents of choice include amoxicillin, amoxicillin-clavulanate, cephalexin, cefpodoxime, trimethoprim-sulfamethoxazole, nitrofurantoin, and fosfomycin.2,17 Fluoroquinolones may be an option in patients who are undergoing procedures involving the prostate because of their ability to penetrate the prostate tissue. However, the increase in fluoroquinolone-resistant E coli should be taken into consideration in the selection of empiric antibiotic therapy, especially if local resistance rates for E coli exceed 20%.18 Antibiotic therapy should be guided by patient-specific factors as well as urine culture and sensitivity results, if available.2
The Pharmacist’s Role
Pharmacists play a vital role in promoting antimicrobial stewardship and effectively counseling patients on UTI self-testing with home kits. Several UTI dipstick tests are available OTC. Pharmacists should thoroughly counsel patients on the criteria for their use before recommending self-testing, and they should provide appropriate instructions. Home tests are best used if a patient has UTI signs and symptoms (e.g., dysuria, increased urinary frequency/urgency, suprapubic pain) or still has symptoms after completing a full course of antibiotics for a UTI.19 In both circumstances, a positive result or a negative result despite the existence of UTI symptoms warrants a visit to a healthcare provider. Using a home test is not a substitute for visiting a healthcare provider, as symptomatic UTIs must be treated with antibiotics. Patients often take OTC phenazopyridine for UTI symptoms, so it is important to counsel that this medication should be used only for symptomatic relief and does not treat active infection. It is not necessary for patients with UTI signs and symptoms to perform a home test before visiting a healthcare provider, but they can self-test if wished. Home testing is inappropriate in patients who do not have UTI signs and symptoms, so they should be discouraged from self-testing.2,8,13,19
UTI home tests, which involve collecting a urine sample with a dipstick, are designed to detect the presence of nitrite and leukocyte esterase in the urine. Based on the findings, the dipstick will change colors to indicate whether nitrites and/or leukocytes are present in the urine sample. Nitrates in the urine are reduced to nitrites in the presence of gram-negative bacteria, which are the most common causative organisms in UTIs. Leukocyte esterase may also be detected in the urine when an infection is present. Leukocyte esterase is included in these home kits to increase the test’s overall sensitivity by detecting infections from gram-positive bacteria that would not be identified with a nitrite test alone. However, leukocyte esterase and nitrite in the urine are not definitive indicators of a UTI, and they should not be used as primary diagnostic markers to confirm or rule out an active infection without consideration of other signs and symptoms of UTI. Leukocytes are commonly found in patients with ASB, most notably in those who have diabetes. In the absence of UTI symptoms, pyuria does not warrant antibiotic therapy.20
A few factors can interfere with the accuracy of UTI home tests. A strict vegetarian or vegan diet can cause a false-negative result because the lack of meat consumption leads to insufficient urinary nitrate production; without sufficient urinary nitrate, gram-negative bacteria will not produce detectable nitrite. Excessive vitamin C (>500 mg/24 hours) and tetracycline antibiotics also can interfere with the home test and produce a false-negative result by blocking the color reaction for leukocyte esterase. Because a positive result is indicated by the test strip turning pink, the consumption of products or medications that contain large amounts of similarly colored dyes (e.g., phenazopyridine) can interfere with the color reaction, producing a false-positive result.19 In addition to these factors, patients may collect the urine sample inappropriately. If a urine sample is contaminated, normal flora or other bacteria present on the body may cause a false-positive result.17
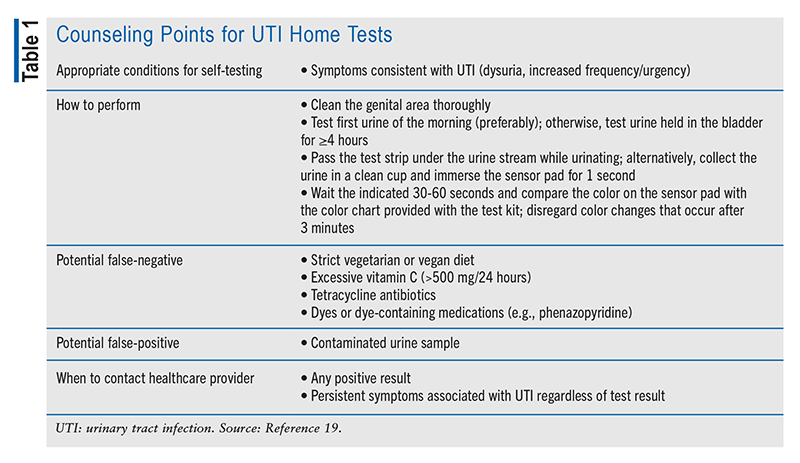
If a UTI home test is being used, the patient should be appropriately counseled on the correct way to perform the test, potential causes of inaccurate results, and factors that warrant a visit to a healthcare provider.19 TABLE 1 lists a summary of important counseling points for UTI home tests.
Conclusion
As one of the most accessible healthcare professionals, the pharmacist can play a key role in ASB education and management not only with patients but with other healthcare providers as well. Pharmacists can educate healthcare providers on the criteria for appropriate ASB screening and treatment, and they can counsel patients on how and when to use UTI home tests. Most importantly, pharmacists can help prevent unnecessary use of antibiotics, thereby reducing the risk of antibiotic resistance while also improving outcomes in patients who have symptomatic UTIs or meet criteria for ASB screening and treatment.
REFERENCES
1. Review on Antimicrobial Resistance. Antimicrobial Resistance: Tackling a Crisis for the Health and Wealth of Nations. London, England: Review on Antimicrobial Resistance; 2014.
2. Nicolle LE, Gupta K, Bradley SF, et al. Clinical practice guideline for the management of asymptomatic bacteriuria: 2019 update by the Infectious Diseases Society of America. Clin Infect Dis. 2019;68(10):e83-e110.
3. Nicolle LE. Asymptomatic bacteriuria: when to screen and when to treat. Infect Dis Clin North Am. 2003;17(2):367-394.
4. Givler DN, Givler A. Asymptomatic bacteriuria. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2022 Jan-.
5. Nicolle LE. Urinary tract infections in the older adult. Clin Geriatr Med. 2016;32(3):523-538.
6. Warren JW, Tenney JH, Hoopes JM, et al. A prospective microbiologic study of bacteriuria in patients with chronic indwelling urethral catheters. J Infect Dis. 1982;146(6):719-723.
7. Trautner BW. Asymptomatic bacteriuria: when the treatment is worse than the disease. Nat Rev Urol. 2011;9(2):85-93.
8. Colgan R, Nicolle LE, McGlone A, Hooton TM. Asymptomatic bacteriuria in adults. Am Fam Physician. 2006;74(6):985-990.
9. Bader MS, Loeb M, Brooks AA. An update on the management of urinary tract infections in the era of antimicrobial resistance. Postgrad Med. 2017;129(2):242-258.
10. Thomas-White K, Forster SC, Kumar N, et al. Culturing of female bladder bacteria reveals an interconnected urogenital microbiota. Nat Commun. 2018;9(1):1557.
11. Salvador E, Wagenlehner F, Köhler CD, et al. Comparison of asymptomatic bacteriuria Escherichia coli isolates from healthy individuals versus those from hospital patients shows that long-term bladder colonization selects for attenuated virulence phenotypes. Infect Immun. 2012;80(2):668-678.
12. Bent S, Nallamothu BK, Simel DL, et al. Does this woman have an acute uncomplicated urinary tract infection? JAMA. 2002;287(20):2701-2710.
13. Fairley KF, Carson NE, Gutch RC, et al. Site of infection in acute urinary-tract infection in general practice. Lancet. 1971;2(7725):615-618.
14. Alagiakrishnan K, Wiens CA. An approach to drug induced delirium in the elderly. Postgrad Med J. 2004;80(945):388-393.
15. WHO Reproductive Health Library. WHO Recommendation on the Method for Diagnosing Asymptomatic Bacteriuria in Pregnancy. Geneva, Switzerland: World Health Organization; December 2016.
16. Henderson JT, Webber EM, Bean SI. Chapter 1: introduction. Screening for Asymptomatic Bacteriuria in Adults: An Updated Systematic Review for the U.S. Preventive Services Task Force. Evidence Synthesis, No. 183. Rockville, MD: Agency for Healthcare Research and Quality; 2019.
17. Wiley Z, Jacob JT, Burd EM. Targeting asymptomatic bacteriuria in antimicrobial stewardship: the role of the microbiology laboratory. J Clin Microbiol. 2020;58(5):e00518-18.
18. Liss MA, Ehdaie B, Loeb S, et al. An update of the American Urological Association white paper on the prevention and treatment of the more common complications related to prostate biopsy. J Urol. 2017;198(2):329-334.
19. Krinsky DL. Home testing and monitoring devices. In: Krinsky DL, Ferreri SP, Hemstreet BA, et al, eds. Handbook of Nonprescription Drugs: An Interactive Approach to Self-Care. 20th ed. Washington, DC: American Pharmacists Association; 2021.
20. Zhanel GG, Nicolle LE, Harding GK. Prevalence of asymptomatic bacteriuria and associated host factors in women with diabetes mellitus. The Manitoba Diabetic Urinary Infection Study Group. Clin Infect Dis. 1995;21(2):316-322.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





