US Pharm. 2022;47(12):20-24.
ABSTRACT: Electronic prescribing, touted as a cure-all for poorly written prescriptions and their increased risk to patients, frequently adds unique difficulties to the prescription-filling process due to defects in the data transmitted to a pharmacy. We have found that in electronic prescriptions received by a long-term care pharmacy, technical errors do occur and may require pharmacist intervention to correct to dispense a medication accurately and consistent with legal requirements.
Electronic prescribing (e-prescribing) has been defined as the use of healthcare technology to improve prescription accuracy, increase patient safety, and reduce costs as well as enable secure, real-time, bidirectional, electronic connectivity between clinicians and pharmacies.1 E-prescribing allows prescribers to directly transmit electronic prescriptions (e-scripts) to pharmacies and minimize the use of potentially illegible handwritten prescriptions. Misinterpretation of illegible handwritten prescriptions was associated with numerous errors, and the consequences could cause patient harm.2,3
The e-prescribing process decreases medication errors and clarification calls to and from the pharmacy due to illegible handwriting, potentially improving workflow efficiency and decreasing patient wait times.4,5 However, the use of e-prescribing does not fully eliminate prescribing errors. E-scripts are still vulnerable to order entry system–related errors from the prescriber side, such as selection of the wrong drug name, dosage, unit, and drop-down menu selection or other information table access errors as well as the prescriber or the prescriber’s agent forgetting to change or edit a mistake.6 Other errors include incorrect or conflicting directions, conflicting information, wrong quantity, and refill errors.
There are different levels of healthcare providers and professionals who are able to prescribe medications. Agents of prescribers, such as medical assistants (MAs) and nurses (RNs), are also able to prepare the order-entry details before the prescriber electronically signs it. Notably, pharmacists are increasingly prescribing medications with their prescriptive authority under collaboration drug therapy agreements (CDTAs/CPAs). As pharmacists’ roles are becoming more integrated with patient care, there is increasing evidence that their contributions to the healthcare team have improved patient health outcomes.7,8 However, there has been little insight into the comparison of frequency of errors between the different prescriber types, especially with pharmacists as prescribers.
Objective
The goal of this article is to present recent quantifiable data on order-entry e-script errors and the rate of errors associated with different degrees of prescribers to contribute to the existing discussion of e-script error rates.
Methods
E-scripts received by AXIS Pharmacy NW (Mountlake Terrace, Washington) for nonscheduled legend drugs (dates of service, 2/11/22-2/ 24/22); schedule II drugs (4/9/21-6/7/21); and Schedule III-V drugs (10/6/21-12/20/21) were reviewed for prescription errors in the following areas: drug name, quantity prescribed, day supply, sig instructions, dosage form, and additional notes or messages from the prescriber. The errors were organized into the following categories: drug name, missing sig components (dose, dosage form, administration route, frequency, duration), dosage form discrepancy, competing instructions/quantity/day supply, and competing sig and messages/notes. In addition, the type of prescriber who made the error was noted. The types of prescribers were organized into the following categories: MD/DO, mid-level (NP/ARNP, PA-C), RN agent, MA agent, and RPh/PharmD. Other modes of prescription transmission (handwritten, verbal, and facsimile) were excluded from this report.=
Results
A total of 2,000 e-scripts comprising 1,000 nonscheduled legend drug e-scripts, 500 schedule II drug e-scripts, and 500 schedule III-V drug e-scripts were reviewed. TABLE 1 shows the number and frequency of various types of e-script errors. Drug name errors included the selection of drugs that are not commercially available in the United States and wrong drug formulation. Competing instructions errors included quantity/day supply discrepancies and conflicting instructions. Schedule III to V drug e-scripts had the most errors at 7%, while legend drug e-scripts had the fewest errors at 4%.
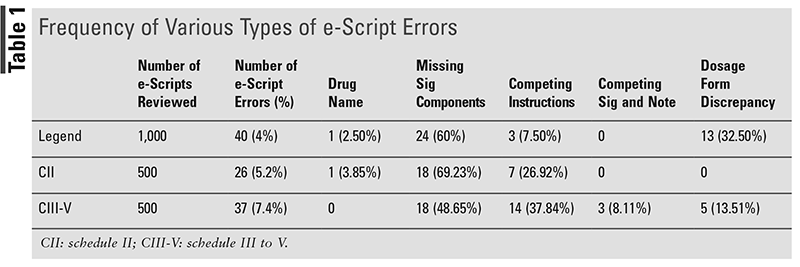
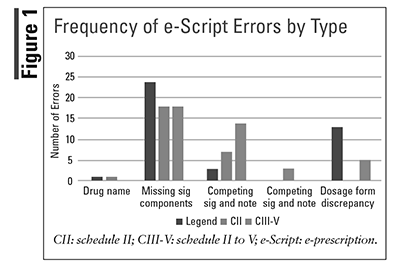
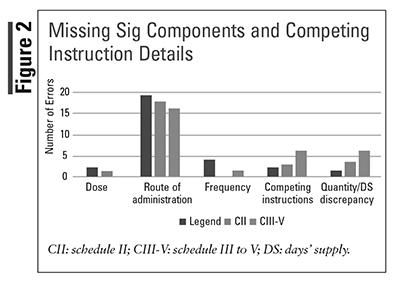
FIGURE 1 depicts the frequency of errors based on the types of e-script errors, and FIGURE 2 shows the missing sig component and competing instruction subcategories. The most common type of error was missing sig components, predominantly the omission of the administration route for all classes medications. A greater number of quantity/day supply discrepancy was identified in the controlled substance e-scripts than the legend e-scripts.
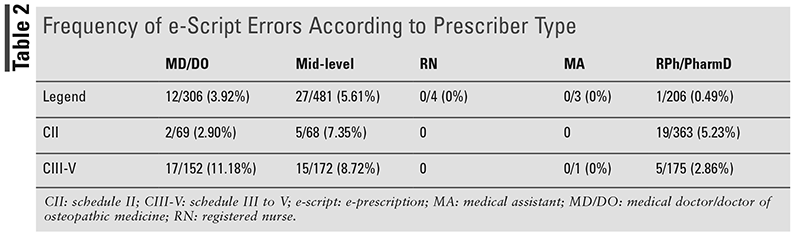
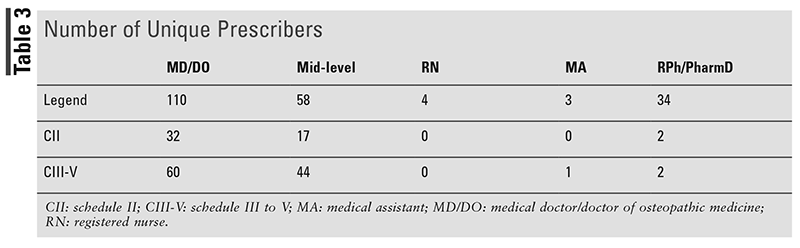
The frequency of e-script errors according to the prescriber type is listed in TABLE 2. The prescriber percentages were calculated by the number of errors the prescriber had out of the total number of errors. TABLE 3 shows the number of unique prescribers for each class of medication.
Discussion
Missing sig components was the type of error that occurred the most, particularly the omission of the route of administration. Although this may seem like a small detail, it is important for optimal absorption, efficacy, and adherence to the medication. For example, hospice patients may have difficulty swallowing, and the intention may be to take tablets sublingually or rectally rather than the conventional oral route. A similar logic can be applied to the dosage-form discrepancies. Dosage forms can affect adherence, and they are not always interchangeable (e.g., extended-release vs. sustained-release formulations). A common pattern observed was that all the information of the e-script was identical to the previous refill e-script, including the errors. The individual prescriber (or the agent) may have a tendency to make the same mistake, possibly due to the nature of the order-entry process for prescription refills. The information may be autopopulated based on the previous e-script and may include the previous errors or create incorrect directions or conflicting information errors (all of which require a contact by the pharmacy for clarification).9
There are many factors that can contribute to order-entry errors in a community pharmacy, such as flaws in the computerized order-entry system, training deficiencies, and human errors, e.g., typing errors.6,10 Work complexity, workload, and system alerts can lead to alert fatigue and potentially increase the risk for errors to be overlooked by prescribers.11 Interestingly, the frequency of errors made by the prescriber type did not show a trend and was inconsistent between the different classes of medications. This may be due to the individual prescriber making the same mistakes in multiple prescriptions, causing an inflation of errors due to that particular prescriber type.
Limitations of this report include the number of sites and the specific selection of possible errors that could occur on an e-script. This report only looked at a specific number of prescriptions at one pharmacy, where a similar pool of prescribers is seen. Errors in the drug name, sig, and dosage forms were the focus of this report. Other errors in patient name, date of birth, address, and dosing could also occur but were not addressed. For the future, the inclusion of other possible errors in dosing, indication, and drug interactions of the medications, in addition to order-entry errors, would greatly contribute to current conversations about e-scripts and mitigate medication errors and patient harm.
Conclusion
Due to legal and third-party requirements, e-prescribing is becoming the predominant method of transmission of prescriptions to community pharmacies. Although e-prescribing may be beneficial in reducing handwriting errors, it may introduce new types of errors. This report looked at just order-entry errors of a technical, not clinical, nature, of which route of administration was one frequently missing feature. E-scripts produced as a result of simply reinstating a previously generated order without reviewing may replicate the error if not corrected. Errors seem to be independent of prescriber type, as we observed errors produced by all prescriber types. It is important that community pharmacists remain vigilant in verifying prescriptions for possible errors to ensure that patients are safely receiving the right medication, dose, and instructions, as well as ensuring that e-scripts contain the legally required information to be valid.
REFERENCES
1. AMCP. Electronic prescribing. 2019. www.amcp.org/about/managed-care-pharmacy-101/concepts-managed-care-pharmacy/electronic-prescribing. Accessed June 6, 2022.
2. Hartel MJ, Staub LP, Roder C, Eggli S. High incidence of medication documentation errors in a Swiss university hospital due to the handwritten prescription process. BMC Health Serv Res. 2011;11:199.
3. Al Shahaibi NM, Al Said LS, Kini TG, Chitme HR. Identifying errors in handwritten outpatient prescriptions in Oman. J Young Pharm. 2012;4(4):267-272.
4. Thomas CP, Kim M, McDonald A, et al. Prescribers’ expectations and barriers to electronic prescribing of controlled substances. J Am Med Inform Assoc. 2012;19(3):375-381.
5. Porterfield A, Engelbert K, Coustasse A. Electronic prescribing: improving the efficiency and accuracy of prescribing in the ambulatory care setting. Perspect Health Inf Manag. 2014;11:1g.
6. Korb-Savoldelli V, Boussadi A, Durieux P, Sabatier B. Prevalence of computerized physician order entry systems-related medication prescription errors: a systematic review. Int J Med Inform. 2018;111:112-122.
7. Strand MA, DiPietro Mager NA, Hall L, et al. Pharmacy contributions to improved population health: expanding the public health roundtable. Prev Chronic Dis. 2020;17:E113.
8. Giberson S, Yoder S, Lee MP. Improving patient and health system outcomes through advanced pharmacy practice. A report to the U.S. Surgeon General. Office of the Chief Pharmacist. U.S. Public Health Service December 2011. www.accp.com/docs/positions/misc/improving_patient_and_health_system_outcomes.pdf. Accessed June 9, 2022.
9. Abramson EL. Causes and consequences of e-prescribing errors in community pharmacies. Integr Pharm Res Pract. 2015;5:31-38.
10. Zhan C, Hicks RW, Blanchette CM, et al. Potential benefits and problems with computerized prescriber order entry: analysis of a voluntary medication error-reporting database. Am J Health Syst Pharm. 2006;63:353-358.
11. Ancker JS, Edwards A, Nosal S, et al. Effects of workload, work complexity, and repeated alerts on alert fatigue in a clinical decision support system. BMC Med Inform Decis Mak. 2017;17(1):36.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






