US Pharm. 2017;42(4):HS21-HS28.
ABSTRACT: Travel-related infections affect children disproportionately and may lead to more serious consequences due to unique characteristics in this population. Children traveling to visit friends and relatives have higher rates of febrile illness from greater direct exposure to pathogenic sources. Pretravel counseling is important, though seldom utilized, in helping to prevent common travel-related illnesses in this demographic. Children more often require hospitalization for travel-related illnesses. Traveler’s diarrhea is one of the most common infections in children traveling abroad, resulting from ingestion of contaminated water or food. Malaria, typhoid, and dengue infections can lead to life-threatening illness in young children. Pharmacists can provide crucial pretravel information based on region and risk profiles of young patients.
Of the more than 70 million Americans who traveled abroad in 2015 (Table 1), two million were children.1,2 Infections in the pediatric population can range from mild, self-limited symptoms to life-threatening disease. Fortunately, most of these syndromes can be prevented through an understanding of the epidemiology of infectious diseases, as well as their unique manifestations in children. As many families do not visit a physician for counseling prior to departure, pharmacists can play an important role in preventing illness.
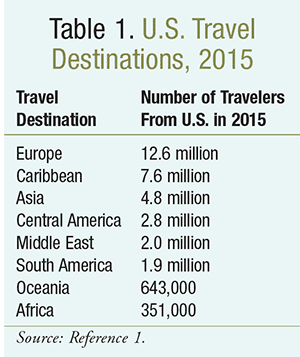
Pretravel counseling should be guided by the travel destination, pre-existing conditions, whether the trip is for visiting friends and relatives (VFR), and other specific risk factors. Although Asia and Africa make up less than 25% of all international destinations, travel-related illnesses occur more frequently within these regions. As opposed to tourism, trips for VFR are associated with a longer duration of stay, more interactions with the local community, and more exposure to local food, water, and animals. Furthermore, travelers going for VFR often do not take necessary prophylactic medications for serious infections, such as malaria, due to the mistaken belief that they are protected by virtue of originally living in that region. Because children travel with family, they are overrepresented among this population.3,4
While adults and children have the same rates of travel-related infections, there are several characteristics unique to the pediatric population that warrant special counseling. These include illnesses that specifically affect those of very young age and the differences in clinical presentations demonstrated in younger children. 5 Infants and toddlers, for instance, are at greater risk for many types of infections relative to older children because of their underdeveloped immune systems, because they often come in direct contact with contaminated objects with their mouths, and because of their limited ability to communicate symptoms.6 Overall, children present earlier in the illness course and are more likely to require hospitalization.
While there are a myriad of infectious syndromes that can affect children who travel abroad, this discussion focuses on diarrhea and fevers, as they are the most commonly encountered problems.4,5 The causes, unique manifestations, prevention, and management of some of the most common pathogens that lead to these syndromes are discussed below.
GASTROINTESTINAL ILLNESS
Traveler’s diarrhea (TD) is the most common form of gastrointestinal illness among children traveling outside the United States.4 Children aged 2 years and those visiting for longer durations are more vulnerable to developing a gastrointestinal illness.7 The GeoSentinel report documenting travel-related illness between 2007 and 2011 found gastrointestinal ailments to be the most prevalent type of sickness among returning travelers in any age group, with Salmonella, Campylobacter, and Shigella the predominant bacterial causative agents and Giardia the primary parasitic agent responsible.8 Travel to Asia, Africa, Mexico, the Middle East, and Central and South America is associated with higher incidences of TD.9
Traveler’s Diarrhea
Causes: The most common causes of TD are bacterial in origin, followed by viral and protozoan etiologies.10 The bacteria most often associated with TD are enterotoxigenic Escherichia coli (ETEC), Shigella spp., Campylobacter jejuni, and Salmonella spp. Viruses that lead to TD include norovirus (usually in outbreak settings such as on a cruise ship), astrovirus, and rotavirus. Giardia intestinalis is the most common protozoan pathogen.9 Sources of infection are usually improperly cooked or stored food and undertreated water, both of which can result in heavy contamination. Entry points include drinking water directly from the tap or from natural sources, using ice in drinks, brushing teeth, and showering with tap water. Similarly, ingesting foods that are raw or undercooked (particularly from street vendors), consumption of unpasteurized milk or dairy products, fruits washed in untreated water, and juice or fruit drinks are all risk factors for TD in children.11
Presentation: TD is defined by the presence of three or more unformed stools and at least one other associated symptom, such as abdominal pain.12 Gross blood usually suggests the presence of Salmonella, Shigella, or Campylobacter, whereas watery stools are usually due to ETEC, viruses, or Giardia. Most of the pathogens result in fever, whereas viral gastroenteritis is usually associated with concomitant vomiting. Time to onset of diarrhea can offer diagnostic clues to the type of pathogen. TD of viral origin has a short incubation period (usually 12-24 hours) and lasts 2 to 3 days. Bacterial TD incubates for 1 to 3 days, and symptoms last up to a week. TD of protozoan origin can incubate for weeks, and symptoms may last weeks or even months if left untreated.9 Dehydration is the biggest challenge associated with TD in children.4
Prevention (Food and Water Safety): Prevention of TD in children requires parental vigilance regarding food and water intake. For example, eating at well-regarded restaurants rather than eating street food can reduce risk. When travelers are staying with family, it is important that food be well cooked. Preventing the ingestion of contaminated water can be challenging; however, avoiding ice, cut fruits and vegetables, and lettuce can help reduce the risk of TD. Furthermore, it is important that all water for drinking, brushing teeth, reconstituting formula, and washing baby products be disinfected. This can be done either by boiling water for at least 1 minute or by using purifiers, ultraviolet light, or chemical disinfection with chlorine or iodine.13 An abundance of caution must be observed for infants and toddlers, as they are at greater risk for complications from severe diarrhea due to their lack of preexisting immunity. Frequent hand washing with an alcohol-based hand sanitizer that contains 60% alcohol is critical to breaking transmission cycles.9
Treatment and Management: For most children, TD is a self-limiting illness that resolves over the course of a week and requires only careful monitoring by caregivers to ensure adequate oral intake. For the minority who become dehydrated, the mainstay of management is oral rehydration therapy (ORT).14 ORT is a simple, inexpensive, rapid-acting, and highly effective OTC remedy that has saved millions of lives.15 Salt packets are reconstituted in disinfected water and taken orally over several hours. Early resumption of breastfeeding or bottle-feeding of infants within 6 to 12 hours of initiating ORT is encouraged, even if the baby is continuing to have diarrhea.9 Antidiarrheals and antiemetics are generally not recommended for use in children.16
Brief courses of antibiotics have a limited role for use shortly after symptom onset and must be tailored to the region of the world. Prophylactic antibiotics should be prescribed only after pretravel consultation with a physician.9
FEVER
The GeoSentinel report on travel-related illness (2007-2011) found that febrile syndromes accounted for 23% of all travel-related illness.8 Of the many causes of fevers in a child returning from recent travel, malaria, dengue, and typhoid fever cannot be overlooked because they are relatively common and can be life-threatening.17 Other infectious causes of fevers that are outside the scope of this review include Chikungunya, Zika, and Ebola viruses, and other uncommon but serious bacterial infections, such as those from Neisseria meningitidis and Leptospirosis.16
Malaria
The World Health Organization (WHO) reported that malaria was responsible for over 400,000 deaths in 2015; 90% of these occurred in sub-Saharan Africa. Seventy percent of deaths were among children aged <5 years.18 Malaria is transmitted via the bite of Anopheles mosquitoes carrying parasites of the genus Plasmodium.18 The different species of Plasmodium have unique manifestations, but in general, severe infection is usually due to Plasmodium falciparum, while a milder illness is usually due to infection with Plasmodium vivax.19 P falciparum is the predominant form of malaria infection in Africa, and P vivax is responsible for malaria in other endemic regions of the world.18 Clinicians and pharmacists must carry a high suspicion for this disease as a cause of fever when a child has been in an endemic area. Children going for VFR, those traveling to Africa, and children who may not have received preventive antimalarial prophylaxis are at highest risk for contracting this disease.16
Symptoms and Sequence: It is well known that children are at greater risk for complications from malaria, such as severe anemia, acute respiratory distress syndrome, cerebral malaria, and multiorgan involvement.18 There are 1,500 cases of malaria diagnosed in the U.S. annually, primarily in travelers to endemic areas.20 The typical incubation period is between 7 and 30 days for infections by P falciparum, but symptoms may appear as late as a year after infection with P vivax. The most common manifestations include fever, chills, body aches, headache, nausea/vomiting, and sweating.21 Infants and very young children may present only with fever and vomiting.4
Prevention: Malaria can be effectively prevented in children through chemoprophylaxis and by avoiding mosquitoes. The former is achieved through a variety of agents that are chosen based on a child’s age, the target destination, the side-effect profile, and ease of dosing (see Table 2). Mosquitoes can be avoided by using protective clothing to cover exposed skin areas, using treated bed netting, eliminating standing water near buildings, and using repellents with DEET (diethyltoluamide). Products with <30% DEET are recommended for children aged >2 months. DEET is not recommended for infants aged <2 months.22 Many families who are traveling for VFR mistakenly believe that they are immune to malaria because they grew up in an endemic area.4 This represents an important opportunity for counseling by a pharmacist, who may be the only provider to see the family prior to departure.
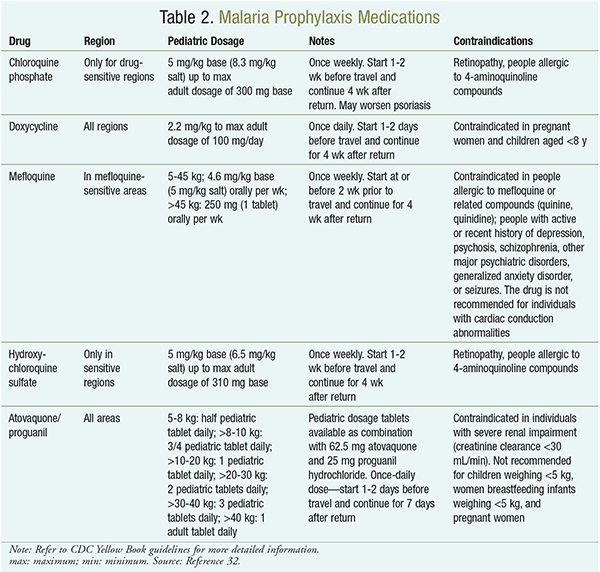
Treatment and Management: Treatment varies depending on the type of malaria, disease complexity, and area of travel, as well as special considerations such as pregnancy, age, weight of the patient, and the possibility of drug resistance.23
Dengue
Dengue fever is a virus caused predominantly by the bite of Aedes aegypti or Aedes albopictus mosquitoes. There are four viral serotypes known to cause disease in humans. Dengue is the second most common cause of nonspecific fever after malaria.24 Reports indicate up to 390 million people may be infected with dengue annually.25 In 2015, over two million cases of dengue were reported in the Americas, with 1,181 deaths.24 Dengue is primarily associated with tropical and subtropical regions of the world, and the most severe cases occur in Asia and Latin America.24 It is possible to be immune to one serotype but susceptible to other serotypes of the virus; additionally, progression to complicated infection is higher upon subsequent exposure.26
Symptoms and Sequence: Patients typically present with fever and two or more additional symptoms, such as headache, body aches, nausea/vomiting, swollen glands, and rash.24 In the Caribbean, infection with dengue is often referred to as “break-bone” fever because of the intense pain in the bones. The incubation period of the virus is generally between 4 and 10 days, and symptoms can last up to 7 days.24 If a patient’s symptoms begin >10 days after return from an endemic location, the illness is highly unlikely to be due to dengue. In cases of severe dengue, signs of serious complications include leukopenia, severe abdominal pain, acute bleeding, respiratory distress, and other organ damage.24 Approximately 5% to 10% of patients develop dengue hemorrhagic fever, which is a potentially deadly complication with rapid onset of multiorgan failure; a percentage of these patients go on to dengue shock syndrome, which can be fatal if volume replacement is not initiated promptly.24
Prevention: Families with children traveling to endemic areas should be advised that primary prevention is accomplished by avoiding mosquitoes and, as with malaria, involves the use of repellents, treated bed netting, and protective clothing. Several vaccine trials are currently under way.27 A recently developed vaccine, Dengvaxia (CYD-TDV), has been approved for use in individual countries and in patients aged 9 to 45 years. The WHO currently recommends limiting use of the vaccine to affected geographic areas with an elevated virus burden.24
Treatment and Management: Treatment for dengue involves accurate diagnosis and early symptom management. There is no targeted antiviral medication that can cure infection.
Typhoid and Paratyphoid Fever
Typhoid and paratyphoid infections are caused by Salmonella enterica subsp. enterica, serovar Typhi, and serovar Paratyphi.4 Typhoid fever is one of the most common vaccine-preventable illnesses among traveling children,8 and it is acquired primarily through contaminated food and water sources. More than 400 cases of typhoid and paratyphoid fever are diagnosed in the U.S. each year, with a majority (>80%) of cases in persons who have traveled to Southern Asia.28
Symptoms and Sequence: Typhoid and paratyphoid fever have similar clinical presentations. Symptoms tend to build up gradually over 7 to 14 days and are characterized by fever, headaches, body aches, anorexia, and constipation, rather than diarrhea, in children.4 Blood cultures, as well as a detailed clinical history of exposures and symptoms, are crucial for diagnosis. It may be necessary to obtain multiple blood and bone marrow cultures to differentiate from other causes of infection.28
Prevention: As the mechanism of transmission is identical for TD, typhoid, and paratyphoid fever, the food and water safety precautions mentioned previously are equally applicable here. These include vigilance in food preparation, use of bottled or disinfected water only, and strict hand hygiene. Although not 100% effective, the typhoid fever vaccine is an important adjunctive preventive measure, particularly given the rise of antibiotic resistance. An intramuscular polysaccharide vaccine (Typhim Vi, Sanofi Pasteur) given as a single dose at least 2 weeks before exposure provides up to 2 years of protection and is approved for children 2 years of age; an oral live attenuated vaccine (Vivotif, PaxVax) provides 5 years of protection and is approved for children 6 years old. Use of Vivotif is contraindicated in those with a yeast allergy, immunocompromised patients, or those on immunosuppressive therapies. Vivotif is also contraindicated in people with acute febrile illness and acute gastrointestinal symptoms such as diarrhea or vomiting. It is classified as Pregnancy Category C. There are no vaccines for paratyphoid infection.28
Treatment and Management: Treatment has become complicated due to the emergence of multidrug-resistant strains in several countries. Azithromycin, ciprofloxacin, and ceftriaxone are recommended based on region and resistance patterns. Fluoroquinolones may be contraindicated for use in children in some countries; however WHO guidelines indicate that the benefits of use outweigh the risks in locations where suitable alternatives may not be available. Long-term studies indicate they are safe to use for short durations in children. Diagnostic testing to isolate the organism and ascertain drug resistance is key to successful treatment.29
ROLE OF THE PHARMACIST
Children are at increased risk for acquiring travel-related infections when going for VFR.4 Furthermore, U.S.-born children of immigrant parents, when traveling for VFR, have a higher chance of certain illnesses.30 Pretravel consultation that encompasses specific information for children is important; however, specific and relevant information for children traveling for VFR is seldom utilized or offered.31 Pharmacists can play a key role in providing travel-related information (see Resources for Pharmacists) and can administer preventive vaccines, if certified. Travel advice based on region, duration, age-related aspects of prevention, and coordination of information with other relevant health practitioners are important factors to consider in pharmacist counseling.
HELPFUL TIPS
• Vaccines should be up-to-date prior to travel, including influenza and pneumonia
• To find local doctors abroad: https://travel.state.gov/content/passports/en/go/health/doctors.html.
• To find accredited hospitals abroad: www.jointcommissioninternational.org/about-jci/jci-accredited-organizations.
• Travelers should be warned to acquire medications only from pharmacies that are regulated to prevent acquisition of adulterated, expired, misbranded, or counterfeit medications and, for medication integrity, to avoid medications that may not have been stored in a temperature-controlled environment.
REFERENCES
1. National Travel and Tourism Office. U.S. citizen international outbound travel up eight percent in 2015. March 21 2016. http://travel.trade.gov/tinews/archive/tinews2016/20160321.asp. Accessed November 20, 2016.
2. CDC. Traveling with children. Updated April 26, 2013. wwwnc.cdc.gov/travel/page/children. Accessed November 20, 2016.
3. United States Department of Commerce. International Trade Administration. U.S. resident travel to international destinations increased nine percent in 2015. http://travel.trade.gov/outreachpages/download_data_table/2015_Outbound_Analysis.pdf. Accessed November 20, 2016.
4. Flores MS, Hickey P, Fields J, Ottolini M. A “syndromic” approach for diagnosing and managing travel-related infectious diseases in children. Curr Probl Pediatr Adolesc Health Care. 2015;45(8):231-243.
5. Hagmann S, Neugebauer R, Schwartz E, et al. Illness in children after international travel: analysis from the GeoSentinel Surveillance Network. Pediatrics. 2010;125(5):e1072-e1080.
6. Tucker R. Managing risks of travel abroad with children. Nurs Times. 2015;111(26):22-24.
7. Soriano-Arandes A, Garcia-Carrasco E, Serre-Delcor N, et al. Travelers’ diarrhea in children at risk: an observational study from a Spanish Database. Pediatr Infect Dis J. 2016;35(4):392-395.
8. Leder K, Torresi J, Libman MD, et al. GeoSentinel surveillance of illness in returned travelers, 2007–2011. Ann Intern Med. 2013;158(6):456-468.
9. Connor B. Travelers’ diarrhea. In: CDC. Traveler’s Health—Yellow Book. Chapter 2. The pre-travel consultation. Updated July 10, 2015. wwwnc.cdc.gov/travel/yellowbook/2016/the-pre-travel-consultation/travelers-diarrhea. Accessed November 21, 2016.
10. Freedman D, Chen LH, Kozarsky PE. Medical considerations before international travel. N Engl J Med. 2016;375(3):247-260.
11. Dupont H. In: CDC. Traveler’s Health—Yellow Book. Chapter 2. Pre-travel consultation. Self-treatable conditions. For the record: a history of the definition & management of travelers’ diarrhea. Updated July 10, 2015. wwwnc.cdc.gov/travel/yellowbook/2016/the-pre-travel-consultation/for-the-record-a-history-of-the-definition-management-of-travelers-diarrhea. Accessed November 22, 2016.
12. Watson J, Hlavsa M, Griffin P. In: CDC. Traveler’s Health—Yellow Book. Chapter 2. Pre-travel consultation. Counseling and advice for travelers. Food and water precautions. Updated July 10, 2015. wwwnc.cdc.gov/travel/yellowbook/2016/the-pre-travel-consultation/food-water-precautions. November 22, 2016.
13. Backer H. In: CDC. Traveler’s Health—Yellow Book. Chapter 2. Pre-travel consultation. Counseling and advice for travelers. Water disinfection for travelers. Updated July 10, 2015. wwwnc.cdc.gov/travel/yellowbook/2016/the-pre-travel-consultation/water-disinfection-for-travelers. Accessed November 22, 2016.
14. Diemert DJ. Prevention and self-treatment of traveler’s diarrhea. Clin Microbiol Rev. 2006;19(3):583-594. 15. Fontaine O, Garner P, Bhan MK. Oral rehydration therapy: the simple solution for saving lives. BMJ. 2007;334:s14.
16. Weinberg N, Weinberg M, Maloney S. Traveling safely with infants and children. In: CDC. Traveler’s Health—Yellow Book. Chapter 7. International travel with infants and children. Updated July 10, 2015. wwwnc.cdc.gov/travel/yellowbook/2016/international-travel-with-infants-children/traveling-safely-with-infants-children. Accessed November 26, 2016.
17. Halbert J, Shingadia D, Zuckerman J. Fever in the returning child traveller: approach to diagnosis and management. Arch Dis Child. 2014;99(10):938-943.
18. World Health Organization. Malaria. Updated December 2016. www.who.int/mediacentre/factsheets/fs094/en/. Accessed November 24, 2016.
19. Tolle M. Evaluating a sick child after travel to developing countries. J Am Board Fam Med. 2010;23(6):704-713.
20. World Health Organization. 10 facts on malaria. Updated December 2016. www.who.int/features/factfiles/malaria/en/. Accessed November 27, 2016.
21. CDC. Malaria and travelers. Updated October 4, 2016. www.cdc.gov/malaria/travelers/index.html. Accessed November 26, 2016.
22. Fischer P, Bialek R. Prevention of malaria in children. Travel medicine. Clin Infect Dis. 2002;34(4):493-498.
23. CDC. Malaria disease. Updated October 7, 2015. www.cdc.gov/Malaria/about/disease.html. Accessed November 26, 2016.
24. CDC. Malaria diagnosis and treatment in the United States. Updated September 22, 2016. www.cdc.gov/malaria/diagnosis_treatment/index.html. Accessed November 26, 2016.
25. Bhatt S, Gething PW, Brady OJ, et al. The global distribution and burden of dengue. Nature. 2013;496(7446):504-507.
26. World Health Organization. Global alert and response. WHO report on global surveillance of epidemic-prone infectious diseases—dengue and dengue haemorrhagic fever. www.who.int/csr/resources/publications/dengue/CSR_ISR_2000_1/en/. Accessed November 27, 2016.
27. Lim S-K, Lee YS, Namkung S, et al. Prospects for dengue vaccines for travelers. Clin Exp Vaccine Res. 2016;5(2):89-100.
28. Newton A, Routh J, Mahon B. In: CDC. Traveler’s Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated July 10, 2015. Typhoid and paratyphoid fever. wwwnc.cdc.gov/travel/yellowbook/2016/infectious-diseases-related-to-travel/typhoid-paratyphoid-fever. Accessed November 30, 2016.
29. World Health Organization. Dengue treatment and management section: dengue and severe dengue. Fact sheet. Updated July 2016. www.who.int/mediacentre/factsheets/fs117/en/. November 27, 2016.
30. Han P, Yanni E, Jentes ES, et al. Health challenges of young travelers visiting friends and relatives compared with those traveling for other purposes. Pediatr Infect Dis J. 2012;31(9):915-919.
31. Hagmann S, Benavides V, Neugebauer R, Purswani M. Travel health care for immigrant children visiting friends and relatives abroad: retrospective analysis of a hospital-based travel health service in a US urban underserved area. J Travel Med. 2009;16(6):407-412.
32. Arguin P, Tan K. In: CDC. Traveler’s Health—Yellow Book. Chapter 3. Infectious diseases related to travel. wwwnc.cdc.gov/travel/yellowbook/2016/infectious-diseases-related-to-travel/malaria#4661. Accessed January 10, 2017.
To comment on this article, contact rdavidson@uspharmacist.com.







