US Pharm. 2021;46(3):17-22.
ABSTRACT: Fibromyalgia, a condition affecting the central nervous system, causes widespread pain as well as other symptoms—such as sleep disruptions, fatigue, and difficulty concentrating—that adversely affect the patient’s quality of life. There is no specific diagnostic test for fibromyalgia, but a variety of tools are used to evaluate the patient’s symptoms in order to confirm the diagnosis. Although several classes of medications, such as antidepressants, are useful for treating fibromyalgia pain and other associated symptoms, nonpharmacologic treatments such as exercise, mindfulness techniques, acupuncture, and others have been shown to be equally effective—if not more effective—options.
Fibromyalgia is a chronic, disabling condition that encompasses musculoskeletal pain, fatigue, depression, and sleep disturbances.1 It can significantly worsen the patient’s quality of life and adversely affect memory and the ability to learn and concentrate (a phenomenon known as dyscognition or “fibro fog”).1,2 In some individuals, fibromyalgia is triggered by a physical or psychological event or disorder; in others, it develops gradually with no precipitating cause. Although fibromyalgia can occur at any time of life, even in childhood, onset is usually in middle age, and the likelihood increases with age. A family history of fibromyalgia may play a part in the development of the disorder. Several pharmacologic and nonpharmacologic options exist for the treatment of fibromyalgia symptoms.
ETIOLOGY
The primary symptom of fibromyalgia is chronic, widespread pain. Additional signs and symptoms may include stiffness; fatigue; depression; anxiety; insomnia; headaches; tingling or numbness in the hands or feet; restless legs syndrome; irritable bowel syndrome; temporomandibular joint disorder; and sensitivity to light, temperature, and loud sounds. Fibromyalgia is two times more likely in women than in men.3 Other potential risk factors include age, rheumatoid arthritis, lupus, obesity, repetitive injuries, and traumatic or stressful or events.1 Some studies have suggested a genetic component. One such study that compared fibromyalgia patients with healthy controls showed a significant difference in cerebral pain processing due to polymorphisms in the mu-opioid receptor gene.4
EPIDEMIOLOGY
The CDC has reported that 4 million U.S. adults—roughly 2% of the population—have fibromyalgia.1 This condition was originally classified as an inflammatory musculoskeletal disease, but there are no inflammatory markers for fibromyalgia, and it has now been shown to primarily affect the central nervous system.5 Complications of fibromyalgia may include hospitalizations and higher rates of other rheumatic conditions, major depression, and suicide.1
DIAGNOSIS
Currently there are no specific diagnostic tests for fibromyalgia, but a review of the patient’s medical history, physical examination, x-rays, and bloodwork can help rule out other causes of widespread pain. Subjective tools, some of which are the Visual Analogue Scale, the Fibromyalgia Impact Questionnaire, and the Hospital Anxiety and Depression Scale, may be used to determine the severity of fibromyalgia symptoms.6 These tools have also been used to measure the primary outcomes of many studies involving fibromyalgia patients in order to determine the effectiveness of treatment. TABLE 1 lists the diagnostic criteria for fibromyalgia.7 One potential difficulty in fibromyalgia diagnosis is that a patient could have a condition that mimics fibromyalgia (e.g., obstructive sleep apnea, Lyme disease, arthritis) and concurrently also have fibromyalgia. However, the current consensus is that if the diagnostic criteria for fibromyalgia are met, fibromyalgia is a valid diagnosis irrespective of the presence of any signs or symptoms of other diseases.7

TREATMENT
There is no cure for fibromyalgia at present, but treatments are available that can reduce symptoms. Pain is typically the main symptom, but other symptoms may include depression, anxiety, sleep disorders, and various other conditions. Both pharmacologic and nonpharmacologic approaches to treatment are recommended depending on the patient’s signs and symptoms. Options include antidepressant use, sleep management, exercise, fibromyalgia support group participation, acupuncture, and stress-reduction activities.8
It is important to note that some prescribed medications, while effective at first, may show reduced efficacy over time. In such cases, it is recommended that the patient be weaned off the medication and then slowly initiated on a replacement. It may be necessary to attempt this multiple times until the right combination of medications is found.8
Pharmacologic
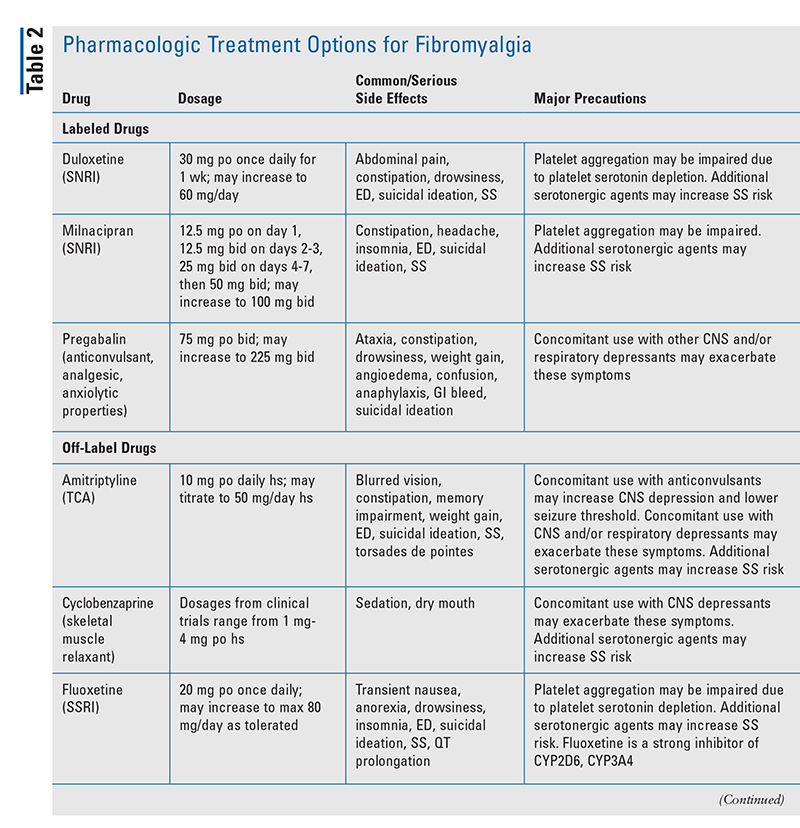
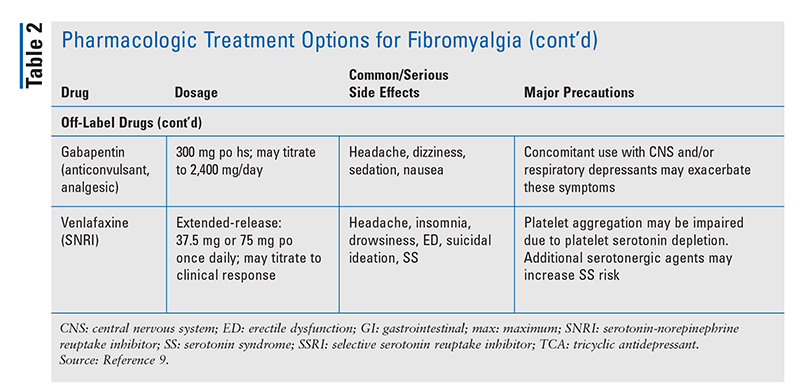
Medications currently indicated for the treatment of fibromyalgia include duloxetine, milnacipran, and pregabalin. Medications with off-label use include amitriptyline, cyclobenzaprine, gabapentin, fluoxetine, and venlafaxine. TABLE 2 summarizes the dosing, common and serious side effects, and major precautions for current pharmacologic treatment options.9
Anti-Inflammatory Medications: Patients sometimes self-medicate with nonsteroidal anti-inflammatory agents such as ibuprofen or naproxen or are prescribed corticosteroids to treat peripheral pain. However, evidence indicates that these medications are ineffective for treating fibromyalgia pain.3
Antidepressants: A meta-analysis of 18 studies was conducted to determine the efficacy of antidepressant use for fibromyalgia symptoms including pain, depression, fatigue, sleep disturbances, and health-related quality of life (HRQOL).10 As a group, antidepressants were found to decrease pain, reduce sleep disturbances, enhance mood, and increase HRQOL. Except for amitriptyline, there was little evidence of improvement in fatigue. Amitriptyline improved pain, fatigue, and sleep disturbances but did not improve depressed mood (it was speculated that the doses used were too low to have an effect). Fluoxetine and paroxetine produced a decrease in pain and a small effect on depressed mood and HRQOL, but they had no effect on fatigue or sleep. Duloxetine and milnacipran lessened pain and sleep disturbances, and duloxetine resulted in improvements in depressed mood and HRQOL. Two major limitations of the studies were 1) no measurement of serum antidepressant levels (to determine adherence) and 2) no controlling for concomitant analgesic use. The absence of long-term follow-up suggested that patient evaluation be conducted at regular intervals to determine continued treatment efficacy. Based on these findings, short-term use of amitriptyline or duloxetine was recommended.10 For patients whose chief symptoms are depression and/or anxiety, an antidepressant such as duloxetine or fluoxetine, based on current evidence, should be used. If sleep-related difficulties are a bigger problem, amitriptyline may be a better option.10
Cannabis: Data on the use of cannabis for the treatment of fibromyalgia are limited. Nabilone is a synthetic cannabinoid approved only for treating refractory nausea and vomiting in patients undergoing chemotherapy.11 Although nabilone has been shown to have some benefit for sleep improvement, anxiety reduction, and HRQOL (0.25 mg-2 mg/day), evidence is weaker compared with first-line treatments for fibromyalgia. Side effects include dizziness, poor coordination, dry mouth, and ataxia. The Canadian Rheumatology Association states that it does not endorse the use of dried cannabis and currently recommends against it unless standard treatment has failed.12
Opioids: Although opioids are used to treat many different types of pain, their use for fibromyalgia remains controversial at best. Not much data exist to support the use of opioids, and other medications are available that can effectively alleviate the symptoms of fibromyalgia without potentially causing debilitating adverse effects such as mood disturbances, constipation, sedation, mental clouding, and dependence. In as little as 1 month, regular use of opioids can produce opioid-induced hyperalgesia.13 Tramadol, which has a different mechanism of action than other opioids, has been used to treat fibromyalgia pain. In addition to binding to mu-opioid receptors, it also inhibits both serotonin and norepinephrine reuptake. Tramadol is also less likely to produce dependence.14 Hyperalgesia (enhanced sensitivity to pain) is not a reported adverse effect of tramadol. Although tramadol is not indicated for the treatment of fibromyalgia, dosages of 50 mg to 400 mg daily have been reported.14
Combination Therapy: A meta-analysis of 16 studies that used various two-drug combinations for treatment of fibromyalgia pain reported that three combinations (melatonin-amitriptyline, fluoxetine-amitriptyline, and pregabalin-duloxetine) produced a greater reduction in pain compared with monotherapy alone.15 Given the paucity of large and high-quality studies, however, the authors concluded that evidence on the use of combination pharmacotherapy to treat fibromyalgia symptoms was limited.15 In a recent study comparing pregabalin as monotherapy versus combined pregabalin and milnacipran, it was concluded that combination therapy demonstrated no significant improvement over pregabalin alone.16 However, it has been suggested that patients who exhibit polygenic chronic illnesses may be treated with combinations of medications based on their different mechanisms of action.3
Nonpharmacologic
Mindfulness Plus Amygdala and Insula Retraining: An 8-week parallel pilot study compared mindfulness techniques plus amygdala and insula retraining (MAIR) with relaxation therapy (RT) for fibromyalgia treatment in women. MAIR or RT was added to treatment as usual (TAU) in two groups of subjects with diagnosed fibromyalgia.17 The RT group participated in four techniques: visualizations, autogenic relaxation, progressive relaxation, and breathing. The MAIR group focused on improving coping skills by using techniques—such as breathing, meditation, and neurolinguistic programming—theorized to interrupt the amygdala’s conditioned responses of anxiety and fear. The MAIR group was superior to the RT group in the primary outcome of reduced symptoms at cessation of treatment and 3-month follow-up. That group also demonstrated a significant decrease in brain-derived neurotrophic factor, which is thought to play a key role in a variety of neuroplastic processes, including pain modulation/transduction, nociception, and hyperalgesia.
Exercise: A prospective, longitudinal (5-year) study observed the effectiveness of moderate-intensity continuous training and high-intensity interval training in improving fibromyalgia symptoms, including pain, anxiety, depression, and HRQOL, in women.6 The 89 subjects were retrospectively categorized as active (moderate-intensity training), semiactive (low-intensity training), or passive (training noncompletion). The active group showed the most improvement, with significantly decreased pain, anxiety, and depression and increased sleep quality and HRQOL. Most subjects in the active group experienced alleviation of all symptoms by the end of the study. By contrast, the passive group experienced a significant increase in pain after year 1 and year 5.6 A different study compared the effectiveness of TAU versus TAU plus nature-activity therapy for fibromyalgia.18 TAU was defined as basic education on fibromyalgia, advice on aerobic exercise, and pharmacotherapy (duloxetine, amitriptyline, pregabalin, and low-dose tramadol as monotherapy or in combination). Nature activities included hiking, yoga, photography, Nordic walking, and shinrin-yoku. The primary outcome was symptom improvement. TAU plus nature-activity therapy showed significant improvements over TAU alone in pain, depression, anxiety, and fatigue.
Acupuncture: Approximately 10 million acupuncture treatments are administered annually in the U.S., and this technique has been shown to relieve pain and improve HRQOL.19,20 A meta-analysis of nine studies revealed that real acupuncture (placing needles along specific meridian points) was significantly superior to sham acupuncture (placing needles at nonmeridian points) in decreasing pain and increasing HRQOL in fibromyalgia patients.21 In a different study, real acupuncture resulted in significant improvements in fibromyalgia symptoms, increased serum serotonin, and decreased substance P compared with sham and simulated acupuncture in 75 female patients.22
CONCLUSION
Fibromyalgia is a chronic condition that can cause widespread pain, depression, anxiety, and a host of other symptoms. The goals of therapy should be to lessen the severity of symptoms and to improve HRQOL; focusing solely on pain management is a recipe for failure. Pharmacists should discuss with patients not only the prescribed medications but also the various nonpharmacologic options, and they should encourage patients to find the best avenue for their care. For many patients, nonpharmacologic options often provide the greatest symptom relief. Exercise has demonstrated the biggest improvement in fibromyalgia symptoms including pain, depression, anxiety, and sleep problems. Patients who are fully informed about their condition and the available treatment options can take charge and learn to live with fibromyalgia the best way possible.
REFERENCES
1. CDC. Fibromyalgia. www.cdc.gov/arthritis/basics/fibromyalgia.htm. Accessed November 4, 2020.
2. Mease P, Arnold LM, Bennett R, et al. Fibromyalgia syndrome. J Rheumatol. 2007;34(6):1415-1425.
3. Clauw DJ. Fibromyalgia: a clinical review. JAMA. 2014;311(15):1547-1555.
4. Ellerbrock I, Sandström A, Tour J, et al. Polymorphisms of the mu-opioid receptor gene influence cerebral pain processing in fibromyalgia. Eur J Pain. 2020;25(2):398-414.
5. Understanding fibromyalgia and its related disorders. Prim Care Companion J Clin Psychiatry. 2008;10(2):133-144.
6. Bodéré C, Cabon M, Woda A, et al. A training program for fibromyalgia management: a 5-year pilot study. SAGE Open Med. 2020;8:2050312120943072.
7. Wolfe F, Clauw DJ, Fitzcharles MA, et al. 2016 revisions to the 2010/2011 fibromyalgia diagnostic criteria. Semin Arthritis Rheum. 2016;46(3):319-329.
8. IIiades C. When fibromyalgia painkillers stop working. www.everydayhealth.com/fibromyalgia/fibromyalgia-and-painkillers.aspx. Accessed December 20, 2020.
9. Clinical Pharmacology [Internet]. Tampa, FL: Elsevier; 2020. www.clinicalpharmacology.com. Accessed October 28, 2020.
10. Häuser W, Bernardy K, Üçeyler N, Sommer C. Treatment of fibromyalgia syndrome with antidepressants: a meta-analysis. JAMA. 2009;301(2):198-209.
11. Canadian Agency for Drugs and Technologies in Health. Long-term nabilone use: a review of the clinical effectiveness and safety. www.ncbi.nlm.nih.gov/books/NBK326830/pdf/Bookshelf_NBK326830.pdf. Accessed November 4, 2020.
12. College of Family Physicians of Canada. Authorizing Dried Cannabis for Chronic Pain or Anxiety: Preliminary Guidance from the College of Family Physicians of Canada. Mississauga, ON: College of Family Physicians of Canada; 2014.
13. Ngian GS, Guymer EK, Littlejohn GO. The use of opioids in fibromyalgia. Int J Rheum Dis. 2011;14(1):6-11.
14. Barakat A. Revisiting tramadol: a multi‑modal agent for pain management. CNS Drugs. 2019;33(5):481-501.
15. Thorpe J, Shum B, Moore RA, et al. Combination pharmacotherapy for the treatment of fibromyalgia in adults. Cochrane Database Syst Rev. 2018;2(2):CD010585.
16. Abdel Fattah YH, Elnemr R. Efficacy of pregabalin as a monotherapy versus combined pregabalin and milnacipran in the management of fibromyalgia. Int J Rheum Dis. 2020;23(11):1474-1480.
17. Sanabria-Mazo JP, Montero-Marin J, Feliu-Soler A, et al. Mindfulness-based program plus amygdala and insula retraining (MAIR) for the treatment of women with fibromyalgia: a pilot randomized controlled trial. J Clin Med. 2020;9(10):3246.
18. Serrat M, Almirall M, Muste M, et al. Effectiveness of a multicomponent treatment for fibromyalgia based on pain neuroscience education, exercise therapy, psychological support, and nature exposure (NAT-FM): a pragmatic randomized controlled trial. J Clin Med. 2020;9(10):3348.
19. Mayo Clinic. Acupuncture. www.mayoclinic.org/tests-procedures/acupuncture/about/pac-20392763. Accessed November 4, 2020.
20. Hao JJ, Mittelman M. Acupuncture: past, present, and future. Glob Adv Health Med. 2014;3(4):6-8.
21. Zhang XC, Chen H, Xu WT, et al. Acupuncture therapy for fibromyalgia: a systematic review and meta-analysis of randomized controlled trials. J Pain Res. 2019;12:527-542.
22. Karatay S, Okur SC, Uzkeser H, et al. Effects of acupuncture treatment on fibromyalgia symptoms, serotonin, and substance P levels: a randomized sham and placebo-controlled clinical trial. Pain Med. 2018;19(3):615-628.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





