US Pharm. 2018;43(7):HS-2-HS12.
ABSTRACT: Pulmonary embolism (PE) is a clot in the lung artery, most often due to deep vein thrombosis. It can be difficult to detect and may result in death. The severity of PE and the patient’s presentation drive treatment selection and the care plan. Massive PE is a medical emergency requiring immediate treatment with thrombolytics, anticoagulants, and/or surgery; nonmassive PE may be treated in an outpatient setting. In patients with this diagnosis, pharmacists have a major role in assessing and monitoring therapy, providing patient and caregiver education, and assisting with prior authorization and procurement in the community.
Venous thromboembolism (VTE) encompasses deep vein thrombosis (DVT) and pulmonary embolism (PE).1 Incidence of PE is difficult to determine as it is complicated to identify and diagnose.2,3 It is estimated that approximately 900,000 people per year have a VTE, up to 30% of whom will die within the first month of diagnosis. Approximately one-quarter of patients with PE will die of sudden death.4 Treatment options include nonpharmacologic or pharmacologic management.
Epidemiology
The World Health Organization (WHO) estimates a worldwide incidence of PE of 0.75 to 2.69 per 1,000 individuals per year.5 The CDC estimates a rate of 1 to 2 per 1,000 people per year in the United States alone.4 The mortality rate of acute PE is approximately 7% to 11% and is estimated to cost the United States’ healthcare system $30,000 in the first year after diagnosis.6,7
Etiology, Risk Factors, and Pathophysiology
Patient age and history of VTE are risk factors for the development of VTE, with PE commonly resulting from DVT. A clot in a deep vein can dislodge and travel, entering the right side of the heart and continuing to the pulmonary artery. If the clot blocks blood flow in the pulmonary artery or one of its branches, it is a PE, which can lead to death if not treated.1,8,9 Additional risk factors, typically referred to as Virchow’s Triad, include blood stasis, vascular injury, and hypercoagulability.1 Malignancy, heart failure, pregnancy, postpartum status, obesity, age, smoking, respiratory failure, intensive care, coagulopathy, and hormone replacement therapy/oral contraceptives are also risk factors.6,10,11
Signs and Symptoms
Over 90% of patients present with dyspnea, tachypnea, or chest pain that mimics ischemic angina.1,10 Patients may also have tachycardia.1 Others may present with coughing (20%), syncope (14%), or hemoptysis (7%). Only 5% to 7% of patients will present with “classic” symptoms of PE reported as a triad of shortness of breath, chest pain, and hemoptysis.10
Diagnosis
Diagnosis includes electrocardiogram, chest x-ray, echocardiogram, and CT pulmonary angiography (CTA).10,11 A workup may include the following to aid in confirming or excluding PE: D-dimers, biomarkers of myocardial injury and overload, blood gases, clotting tests, and ventilation-perfusion scans. Although two scoring systems, the Wells Score and the Revised Geneva Score, are available to assess the likelihood of PE, they are not commonly used in practice. Diagnosis is challenging in the presence of other pulmonary comorbidities, such as pneumonia, chronic obstructive pulmonary disease, asthma, or chronic lung disease with fibrosis.10 The complexity of PE presentation frequently results in a diagnosis of exclusion.10,11 In most cases, it is recommended to begin parenteral anticoagulation for suspicion of PE while the workup is in progress.12
Management and Classification
Management includes pharmacologic therapy with thrombolytics and anticoagulation, or nonpharmacologic management, and is stratified into initial, long-term, and extended treatments. Patient-specific treatment is guided by signs and symptoms, bleeding risk, and comorbidities.11,13,14 Goals of treatment include clot resolution and decreased risk of recurrence. Additional goals include decreased risk of consequences of PE, such as death, pulmonary hypertension, and impaired functional outcomes.13
Initial Phase: The aim in the initial phase is to reduce mortality and recurrence in the 5 to 10 days after presentation. Treatment options for initial-phase management include thrombolytics, parenteral anticoagulants, oral anticoagulants, and nonpharmacologic interventions.14
Long-Term Treatment: Long-term treatment is given for at least 3 months with either parenteral or oral anticoagulants. In patients whose PE was provoked, either by surgery or another risk factor, treatment is recommended for 3 months. Patients with unprovoked PE should be treated for 3 months, with reevaluation at 3 months to determine the risks versus the benefits of continuing therapy. In patients with low or moderate bleeding risk, the 2016 Chest Guideline and Expert Panel Report on antithrombotic therapy for VTE recommends extended therapy at this time, whereas patients with high bleeding risk may not be candidates for continuing anticoagulation after 3 months.14
Extended Anticoagulation: Extended anticoagulation is treatment with anticoagulants beyond the first 3 to 6 months, with no anticipated discontinuation date.12,14,15 Patients in whom thrombosis was triggered by nonsurgical risk factors or who have persistent risk factors are at higher risk for recurrence than those with postoperative thrombosis. Patients with unprovoked PE with low-to-moderate bleeding risk should be considered for extended treatment and reevaluated frequently for continuation. Patients with a second unprovoked PE may require extended therapy if their bleeding risk is low or moderate. In all patients with active cancer and cancer-associated PE, extended therapy should be continued, regardless of bleeding risk.14
PE severity is classified as massive (high risk), submassive (intermediate risk), and nonmassive (low risk).10
Massive PE (high risk): Massive PE is defined as having no pulse, a heart rate less than 40 beats per minute, and signs of shock or continuous hypotension. In this case, sustained hypotension cannot be due to dysrhythmias, hypovolemia, sepsis, or left ventricular dysfunction, and is defined as systolic blood pressure (SBP) below 90 mmHg for at least 15 minutes, or SBP below 100 mmHg in a patient with a hypertension diagnosis, or at least a 40% reduction in baseline SBP.13 Patients with massive PE may require immediate resuscitation and management in an intensive-care setting.11 Initial treatment is based on the patient’s vital signs and signs of clinical shock and may include isotonic IV fluids along with other appropriate critical-care management.11,13
Initial-phase treatment with thrombolytics followed by parenteral anticoagulation is recommended for these patients, and considerations may also include catheter-directed thrombolysis or surgical embolectomy if thrombolytics are contraindicated.13,14
Submassive PE (moderate risk): Submassive PE consists of SBP at least 90 mmHg, with some signs of cardiopulmonary stress, such as right ventricular dysfunction or myocardial necrosis defined as elevation in troponin I or T.13 Submassive PE presents with end organ damage, but patients are hemodynamically stable. These patients may also present with cardiac ischemia and altered mental status.11
Thrombolytics may be considered for initial-phase treatment in this patient population if there is clinical evidence of developing hemodynamic instability or worsening prognosis. Risks of bleeding should be weighed against benefits of thrombolysis.13 Other pharmacologic options include parenteral or oral anticoagulants.12 If hypotension develops after anticoagulation, thrombolytic therapy may be revisited at that time.14
Nonmassive PE (low risk): Nonmassive PE may not show any clinical or hemodynamic signs or right ventricular dysfunction based on echocardiogram or biomarkers.13 Patients with low-risk (nonmassive) PE have no end organ damage or hemodynamic instability.11
These patients are candidates for initial-phase treatment with anticoagulants as outpatients and continued long-term therapy.12,14
Nonpharmacologic Options
Nonpharmacologic treatment is considered when there is a high risk of bleeding and thrombolytic therapy is contraindicated.14 These treatments include catheter-directed therapies, embolectomy, suction, or inferior vena cava filter (IVCF) placement.
Catheter-Directed Therapies: Catheter-directed therapies include ultrasound, use of pressurized saline injection, or catheter-led mechanical disruption of thrombi.16 Delivery of catheter-directed therapy may involve off-label use of thrombolytics, used in smaller doses than are used in systemic thrombolysis, thereby lowering the risk of bleeding. The 2016 antithrombotic guideline recommends administration of systemic thrombolytic therapy over catheter-directed therapies in patients who do not have high bleeding risk, given that this therapy has a higher level of evidence.14
Embolectomy: Embolectomy can be done either via catheter or surgically and should be considered if a patient has hemodynamic instability and if thrombolytic therapy is contraindicated.14
Suctioning: Suctioning may remove a thrombus (thrombectomy) or thrombi fragments.16
IVCF Placement: IVCF placement indications vary according to different medical societies and guidelines, although there is consensus to utilize IVCF in patients with acute VTE who are not candidates for anticoagulation.17 The 2016 antithrombotic guideline recommends against the use of IVCF in acute PE patients who are treated with anticoagulants.14 Although a systematic review and meta-analysis found an association of IVCF placement and lower PE risk, these studies were of low-to-moderate quality and showed a higher DVT risk with no effect on mortality.18
Pharmacologic Options
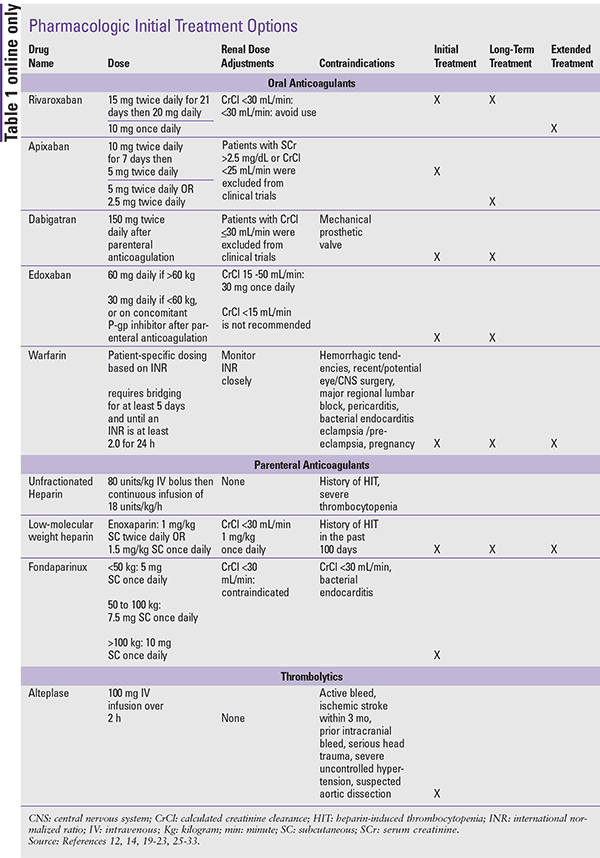
Pharmacologic treatment options, including drug dosages and contraindications, are listed in Table 1.
Thrombolytic: Patients with massive PE who are not at high risk of bleeding are candidates for systemic thrombolytic therapy with alteplase, also known as tissue plasminogen activator (tPA).14 Additionally, patients who deteriorate after receiving initial anticoagulation should be considered for alteplase. Twenty-four hours after thrombolytic therapy, studies showed lowering of pulmonary artery pressure, increasing arterial oxygenation, and resolving perfusion scan defects in patients.12 Alteplase, the only FDA-approved thrombolytic treatment for massive PE, converts plasminogen to plasmin in the coagulation cascade, which results in fibrinolysis. It is administered intravenously via a peripheral vein as a 2-hour infusion.12,19
Parenteral Anticoagulation: Parenteral anticoagulants may be used alone in patients who are not candidates for tPA, or are initiated at the end of the tPA infusion.12,19 These medications prevent further clot formation and work in the coagulation cascade to enhance the body’s ability to dissolve existing clots.11 Options include enoxaparin, dalteparin, fondaparinux, and unfractionated heparin (UFH).
Subcutaneous low molecular weight heparins (LMWH) (enoxaparin and dalteparin) and fondaparinux are effective parenteral anticoagulants for the treatment of PE with dalteparin indicated for extended treatment.12, 20-22 LMWH is preferred if the patient also presents with proximal DVT, in patients with cancer-associated PE, and in pregnancy or pregnancy risks.12,14 LMWH is administered by SC injection and does not require activated partial thromboplastin time (aPTT) laboratory monitoring. Patients treated with enoxaparin should be evaluated for appropriate kidney function because the drug is renally excreted.20 Fondaparinux is a synthetic antithrombotic agent with specific Factor Xa activity, which is also indicated for PE treatment. Like LMWH, it is a subcutaneous injection administered once daily and dosed based on patient weight.22,23 Although fondaparinux has a long half-life and no reversal agent, it is an alternative for patients with a history of heparin-induced thrombocytopenia because it does not cross-react with heparin-induced antibodies.11 Other parenteral agents may be available for off-label treatment of PE in patients with heparin-induced thrombocytopenia (HIT).
Intravenous UFH: Intravenous UFH is the treatment of choice for patients at high risk of bleeding or who are likely to undergo intervention, thrombolysis, or embolectomy, owing to its short half-life.11 It is also the preferred agent in patients with renal dysfunction, obese patients, or those with a recent bleeding history.24 UFH is administered as a continuous infusion via a peripheral vein and requires aPTT laboratory monitoring and dose titration during the infusion to ensure efficacy.25 Platelet count is monitored since UFH is associated with the highest incidence of HIT. In fact, patients treated with UFH are 8 to 10 times more likely to develop HIT than those treated with LMWH.
Noncancer patients are transitioned to oral anticoagulants for long-term treatment upon discharge.14 If a patient is to be transitioned to warfarin, overlap or “bridging” with a parenteral anticoagulant is continued for at least 5 days and until an international normalized ratio (INR) test is at least 2.0 for 24 hours.24,26
Oral Anticoagulation: The 2016 antithrombotic guidelines recommend oral anticoagulation with direct oral anticoagulants (DOACs): direct thrombin inhibitor dabigatran, or factor Xa inhibitors edoxaban, rivaroxaban, or apixaban in low-risk patients without cancer.14,27-32 These agents may be started after initial treatment with thrombolytics and parenteral anticoagulants in massive and submassive PE, or as initial treatment in nonmassive PE.
Dabigatran and edoxaban are approved for long-term VTE treatment after 5 to 10 days of parenteral anticoagulation.14,29,30 Dabigatran, rivaroxaban, and apixaban have been studied in extended treatment and are as efficacious as warfarin with less bleeding.14 Apixaban and rivaroxaban doses are decreased for extended therapy.31-34
Warfarin may be considered in patients with renal disease, coronary artery disease, poor adherence, history of gastrointestinal bleeding, or noncancer patients who are not candidates for DOACs.14 With bridging from other anticoagulants, warfarin is dosed once daily, and the dose is adjusted based on INR results, with a goal INR of 2.0 to 3.0.12,14,26
Aspirin: Three studies evaluated the use of aspirin for extended treatment. The authors concluded that aspirin reduced the overall risk of recurrence of unprovoked PE without increased risk of bleeding when compared with placebo.35 Aspirin may be considered for extended treatment in patients who are stopping anticoagulation and have no contraindications to aspirin.14
Pharmacist’s Role
Pharmacists play an important role in the management of PE. Patient-specific drug selection and dosing are important to maximize therapy and minimize adverse events. Patient risk factors, comorbidities, and organ function are factors in selecting the appropriate agent at the appropriate dose for the appropriate duration. Drug-drug and drug-nutrient interactions are also important in selecting medications and doses. Owing to the risk of bleeding and other drug misadventures, patient and caregiver education that stresses correct administration, storage, adherence, and when to call a healthcare provider are crucial to preventing complications and identifying recurrences. The community or ambulatory pharmacist may be first-line in triaging these occurrences.
In addition to counseling and patient selection, instruction in injection technique may be necessary. Disease-state education focuses on risk reduction, including medication therapy reviews to identify medications that may increase the risk of PE. Pharmacists also have a role in facilitating third-party payment, such as prior authorizations or suggesting alternative therapies while payment approval is pending. Many institutions possess an anticoagulation clinic to manage and monitor this patient population. Pharmacists have also been involved in evaluating cost-effectiveness of these therapies for managed care and other organizations.36,37
Conclusion
PE is the result of a clot in the pulmonary artery or one of its branches. If untreated, PE can result in death. Goals of initial treatment include clot resolution; long-term and extended treatment aim to decrease the risk of recurrence. Additional goals include decreased risk of consequences of PE, such as death, pulmonary hypertension, and impaired functional outcomes. Treatment selection is patient-specific and depends on symptoms, bleeding risk, and comorbidities. Treatment options include nonpharmacologic therapies and pharmacologic therapy with thrombolytics and anticoagulants.
REFERENCES
1. Witt DM, Clark NP, Vazquez SR. Venous thromboembolism. In DiPiro JT, Talbert RL, Yee GC, Matzke GR, et al, eds. Pharmacotherapy: A Pathophysiologic Approach, 10th ed. New York, NY: McGraw-Hill; 2017: Chapter 19.
2. Anderson T, Soderberg S. Incidence of acute pulmonary embolism, related comorbidities and survival; analysis of a Swedish national cohort. BMC Cardiovasc Disord. 2017;17:155.
3. Hendriksen JMT, Koster-van Ree M, Morgenstern MJ, et al. Clinical characteristics associated with diagnostic delay of pulmonary embolism in primary care: a retrospective observational study. BMJ Open 2017;7e012789.
4. CDC. Venous thromboembolism. www.cdc.gov/ncbddd/dvt/data.html. Accessed March 26, 2018.
5. World Health Organization. Cardiovascular diseases. www.who.int/en/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds). Accessed March 26, 2018.
6. Ryan J. Pulmonary embolism: new treatments for an old problem. Open Access Emerg Med. 2016;8:87-95.
7. Geske JB, Smith SB, Morgenthaler TI, Mankad SV. Care of patients with acute pulmonary emboli: a clinical review with cardiovascular focus. Expert Rev Cardiovasc Ther. 2012;10(2):235-250.
8. Cleveland Clinic. Deep vein thrombosis. https://my.clevelandclinic.org/health/diseases/16911-deep-vein-thrombosis-dvt. Accessed March 26, 2018.
9. National Blood Clot Alliance. What is pulmonary embolism (PE)? www.stoptheclot.org/diagnosis_symptoms/what_is_pe.htm. Accessed March 26, 2018.
10. Belohlavek J, Dytrych V, Linhart A. Pulmonary embolism, part 1: epidemiology, risk factors, risk stratification, pathophysiology, clinical presentation, diagnosis and nonthrombotic pulmonary embolism. Exp Clin Cardiol. 2013;18(2):129-138.
11. Corrigan D, Prucnal C, Kabrhel C. Pulmonary embolism: the diagnosis, risk-stratification, treatment and disposition of emergency department patients. Clin Exp Emerg Med. 2016;3(3):117-125.
12. Kearon C, Alk EA, Comerota AJ, et al. Antithrombotic therapy for VTE disease: antithrombotic therapy and prevention of thrombosis. 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;142(6):1698-1704.
13. Long B, Koyfman A. Current controversies in thrombolytic use in acute pulmonary embolism. J Emerg Med. 2016;51(1):37-44.
14. Kearon C, Alk EA, Ornelas J, et al. Antithrombotic therapy for VTE disease. CHEST Guideline and Expert Panel Report. Chest 2016;149(2):315-352.
15. Agnelli G, Becattini C. Acute pulmonary embolism. N Engl J Med 2010;363(3):266-274.
16. Condliffe R, Elliot CA, Hughes RJ, et al. Management dilemmas in acute pulmonary embolism. Thorax. 2014;69:174-180.
17. Weinberg I. Appropriate use of inferior vena cava filters. American College of Cardiology. www.acc.org/latest-in-cardiology/articles/2016/10/31/09/28/appropriate-use-of-inferior-vena-cava-filters. Accessed April 1, 2018.
18. Bikdeli B, Chatterjee S, Desai NR, et al. Inferior vena cava filters to prevent pulmonary embolism. J Am Coll Cardiol. 2017;70(13):1587-1597.
19. Activase (alteplase) package insert. South San Francisco, CA: Genentech, Inc; 2018.
20. Lovenox (enoxaparin sodium) package insert. Bridgewater, NJ: Sanofi-Aventis; 2017.
21. Fragmin (dalteparin) package insert. Woodcliff Lake, NJ: Eisai Inc; 2007.
22. Arixtra (fondaparinux) package insert. Rockford, IL: Mylan Institutional LLC; 2017.
23. The Matisse Investigators. Subcutaneous fondaparinux versus intravenous unfractionated heparin in the initial treatment of pulmonary embolism. N Engl J Med. 2003;349:1695-1702.
24. Streiff MB, Agnelli G, Connors JM, et al. Guidance for the treatment of deep vein thrombosis and pulmonary embolism. J Thromb Thrombolysis. 2016;41:32-67.
25. Heparin package insert. New York, NY: Pfizer Pharmacia & Upjohn Company; 2006.
26. Coumadin package insert. Princeton, NJ: Bristol-Myers Squibb Pharma Company; 2017.
27. The EINSTEIN-PE Investigators. Oral rivaroxaban for the treatment of symptomatic pulmonary embolism. N Engl J Med. 2012;366:1287-1297.
28. Agnelli G, Buller HR, Cohen A, et al. Oral apixaban for the treatment of acute venous thromboembolism. N Engl J Med. 2013;369(9):799-808.
29. Pradaxa (dabigatran) package insert. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals, Inc; 2018.
30. Savaysa (edoxaban) package insert. Basking Ridge, NJ: Daiichi Sankyo Co., LTD; 2017.
31. Xarelto (rivaroxiban) package insert. Titusville, NJ: Janssen Pharmaceuticals, Inc.; 2011.
32. Eliquis (apixaban) package insert. Princeton, NJ: Bristol-Myers Squibb Company; 2017.
33. Agnelli G, Buller HR, Cohen A, et al. Apixaban for extended treatment of venous thromboembolism. N Engl J Med. 2013;368(8):699-708.
34. Weitz JI, Lensing AWA, Prins MH, et al. Rivaroxaban or aspirin for extended treatment of venous thromboembolism. N Engl J Med. 2017;376(13):1211-1222.
35. Simes J, Becattini C, Agnelli G, et al. Aspirin for the prevention of recurrent venous thromboembolism (The INSPIRE Collaboration). Circulation. 2014;130:1062-1071.
36. Dobesh PP, Trujillo TC, Finks SW. Role of the pharmacist in achieving performance measures to improve the prevention and treatment of venous thromboembolism. Pharmacotherapy. 2013;33(6):650-664.
37. Horner T, Mahan CE. Venous thromboembolism: role of the pharmacists and managed care considerations. Am J Manag Care. 2017;23(20 suppl):S391-S398.
To comment on this article, contact rdavidson@uspharmacist.com.