US Pharm. 32(11):63-70.
Despite the increased prevalence of
obesity, there is still a population of patients who suffer from eating
disorders such as anorexia nervosa (anorexia), bulimia nervosa (bulimia), or a
combination. Due to secretive behaviors and the time frame before the clinical
picture of an eating disorder can be identified, the true number of affected
individuals is unknown. Individuals from all demographics can develop eating
disorders, which affect more than 3% of the general female population between
ages 18 and 30.1 The median age of onset is 17, with rare cases
occurring after age 40.2 Although more than 90% of patients
diagnosed with anorexia are females, eating disorders occur in males as well.
Eating disorders among athletes and models have a 10% and 20% incidence for
males and females, respectively, with bulimia occurring more frequently in
this population.1,3
The etiology for anorexia is
not fully understood; however, biological, genetic, psychological, and
sociocultural factors may play a role. Higher rates of anorexia have been
documented among first-degree biological relatives, with an even higher
association for monozygotic twins.4 Coexisting psychiatric
illnesses such as bipolar disorder, depression, dysthymia,
obsessive-compulsive disorder (OCD), and anxiety are higher among this
population. Many cultural factors can add specific pressures with regard to a
patient's weight or shape perception. In today's world, with an abundance of
media and peer pressures, patients with anorexia have a desire to be thin and
accepted.
The diagnostic criteria for
anorexia are set forth by the American Psychiatric Association (APA)and are
published in the Diagnostic and Statistical Manual of Mental Disorders
(DSM-IV-TR).5 The current diagnostic criteria for anorexia in
the DSM-IV-TR are refusal to maintain a minimally normal body weight,
extreme concern about gaining weight, a major aggravation in the perception of
shape or size of the body, and (in a female) missing three consecutive menses.
5 A person is considered below minimal normal body weight if he or she
weighs less than 85% of normal weight for their height and age or has a body
mass index (BMI) of 17.5 kg/m2 or lower.5
Patients with anorexia may
exhibit an array of symptoms. Most notable is their low body weight, which
they are embarrassed about even though they are thin. Obsessive fears about
being overweight and gaining weight along with dissatisfaction over their body
image may exist.6
Many patients with anorexia
are depressed and socially withdrawn and may have obsessive-compulsive
characteristics.5 Common traits include counting calories, weighing
food, hoarding food, lying about food consumption, fasting, and examining
diets excessively.7,8 Odd eating behaviors may develop, such as
taking very small bites, chewing food excessively, and pushing food around on
the plate. Female patients can experience menstrual irregularities due to the
extreme weight loss from not eating and/or from excessive exercise.5-7
Patients with anorexia may use
several aids to attain lower body weight. Those with diabetes may not use
their insulin regimens properly due to the fear of gaining weight; therefore,
many patients will omit their insulin to minimize weight gain. Some patients
suffering from anorexia may also present with bulimia characteristics of binge
eating or food purging. Self-induced vomiting, as well as vomiting with the
use of ipecac syrup, is common. Other ways used by patients with anorexia to
attain weight loss include abusive use of diuretics, laxatives, stimulants,
legend or OTC diet or metabolism-enhancing products, and excessive exercise
routines.
Anorexia is a very serious
condition with many potential life-threatening consequences. Two of the most
alarming concerns are the high relapse rates and the fact that of all
psychiatric illnesses, anorexia is associated with the highest mortality rate.
9,10 Of the patients who seek treatment, only half make a full recovery,
20% to 30% show residual symptoms, 10% to 20% continue to be severely ill, and
5% to 10% die from end organ damage and complications (TABLE 1).10
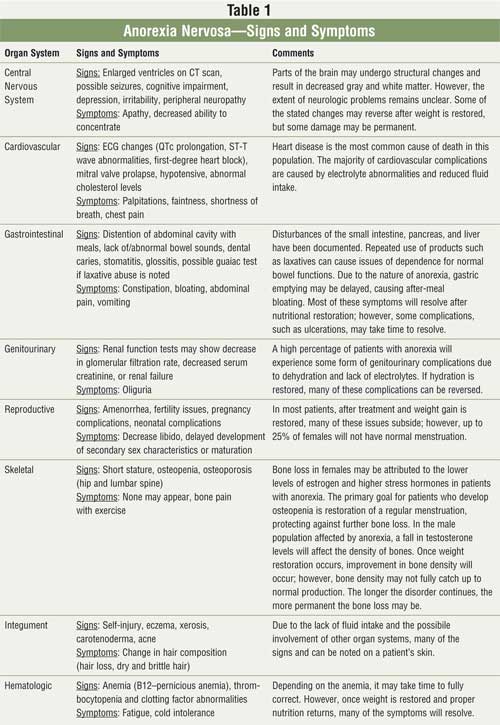
Anorexia is a complex disease
involving many pathways, making it difficult to evaluate medications for
treatment. There have been few randomized, double-blind, placebo-controlled
trials. The difficulty of getting a well-designed trial under way is due to
the low incidence of anorexia and the high drop-out rate in attempted trials;
therefore, the results should be considered cautiously. Most studies involve
adult women; however, young adolescent women make up the greatest population
of anorexic patients. Additionally, the many comorbidities that occur with
anorexia complicate treatment and patient compliance. Drug treatment alone is
not enough; some form of counseling also needs to be in place for anorexic
patients.
TREATMENT
When anorexia is
identified and diagnosed, treatment should begin as soon as possible to
minimize the detrimental effects of the condition itself and the complications
that often coexist.4 Early diagnosis and treatment may reduce the
chance of a relapse.4,6,8,10 According to the American Psychiatric
Association, treatment goals include the following: return to and sustain a
normal weight; eliminate binge eating and purging of food; motivate patients
to be proactive with their heath care regimen; change negative thoughts about
eating; improve self-image; address physical problems; treat psychiatric
problems that may exist; administer counseling; and prevent relapse.4
Weight gain is the primary focus of treatment because this is a key factor in
success with other treatments.4,9,11 High relapse rates are a
challenge when treating anorexic patients, and patients should be monitored
regularly for relapse. In addition, patients must be educated on healthy
nutrition and exercise patterns. It is essential that patients be willing to
fully cooperate and have the support to follow the necessary treatment.
However, getting patients to comply fully has often proved difficult for
clinicians.6
Nonpharmacologic Strategies
Nonpharmacologic therapy for
anorexia includes weight gain, nutritional rehabilitation, and counseling. The
first form of treatment that many practitioners suggest is weight restoration.
4,6 Some patients may require inpatient treatment to achieve normal
weight.4 It has been shown that patients who regain weight to a
normal BMI at inpatient treatment facilities have better long-term outcomes.
4 There appears to be a higher relapse rate associated with patients who
leave treatment facilities before their target weight is obtained; therefore,
patients should remain hospitalized until the target weight is achieved.4
It is strongly recommended
that patients receive some form of counseling. Individual, group, or family
sessions are commonly utilized.4,10 The type of counseling that a
patient undergoes depends on his or her personal needs. Family counseling
appears to be the most commonly used form of psychotherapy for adolescents
with anorexia, and results from studies appear promising.4,10 It is
suspected that this form of therapy is beneficial because parents may
sometimes play a role in the child's development of anorexia, through either
environmental or genetic aspects.4 Individual therapy has also
shown positive results.10 Cognitive behavioral therapy (CBT), a
form of individual therapy, is the most commonly used method.10
Group therapy offers a different dynamic that some patients find supportive.
Group therapy can provide acceptance and camaraderie and help patients realize
they are not alone.6 Unfortunately, there is little evidence
indicating the best type of counseling. This may be attributed to the high
relapse rate and patients' reluctance to comply with either initial treatment
or follow-up examinations.
Pharmacologic
Direct
pharmacologic treatment for anorexia currently does not exist due to the
varied symptoms and range of other psychological problems that often coexist
with this disorder. There are currently no FDA-approved agents for the
treatment of anorexia. However, clinicians often use medications in anorexic
patients to treat comorbidities and to help patients feel more comfortable
with themselves. The literature is varied on the best time to begin
pharmacologic treatment, and studies have not shown consistent results.9
It has been suggested to not begin pharmacologic treatment until weight gain
has been established and instead to rely on counseling and the other
nonpharmacologic treatments mentioned earlier.6,8,12 One common
problem facing patients is that they are often not willing to begin treatments
or take medications.6 Conversely, patients may be more willing to
regain weight if associated conditions are first alleviated with medication.
The following sections discuss the most frequently used classes of medicines
for patients with anorexia.
Antidepressant Agents
Two common
comorbidities that exist in patients with anorexia are depression and
obsessive-compulsive tendencies. Antidepressant medications have been used to
alleviate these conditions in the hope that patients' psychological
functioning will improve, resulting in weight gain.
The selective serotonin
reuptake inhibitors (SSRIs) seem to be favored over the tricyclic
antidepressants (TCAs) because of their side-effect profile, lower chance of
overdose, and higher tolerability.4,13
Studies have been conducted
evaluating tricyclic antidepressants in the treatment of anorexia.
Clomipramine was studied for anorexia in eight patients and found to have no
benefits over placebo on the rate of weight gain.14 The patients on
clomipramine did not gain weight faster than the control group or exhibit any
long-term benefits.14 Amitriptyline was studied for change in mood,
weight gain, and body perception in a double-blind, placebo-controlled trial
with 25 patients. This agent showed no benefits versus placebo.15
Additionally, the patients experienced anticholinergic side effects associated
with amitriptyline. Independent of side effects, TCAs should be avoided in
this population if the risk for suicide is high.
Fluoxetine has been the most
widely studied of the SSRIs because of its low cardiovascular and
anticholinergic side effects and absence of dietary restrictions.16
Unfortunately, the results from these studies have varied. An early,
open-label case series with six patients showed fluoxetine to be safe for use
in underweight patients with anorexia.16 A subsequent randomized,
placebo-controlled, double-blind, seven-week study with 31 patients showed
fluoxetine had no benefit on weight gain or psychological state in anorexic
patients.12
Another randomized,
double-blind, placebo-controlled, year-long trial with 35 patients showed that
fluoxetine was useful in the weight maintenance phase of anorexia.17
After patients had already regained weight, fluoxetine helped them retain the
weight and reduce the chance of relapse. This may be attributed to the
patients having a higher level of serotonin when fluoxetine was initiated.
However, a recent randomized, double-blind, placebo-controlled, year-long
study with 93 patients showed fluoxetine to have no benefit for weight
maintenance in anorexic patients.18
Citalopram was used in a pilot
study with 52 patients for three months. No difference from placebo was
noticed in weight gain. However, the citalopram group did see improvements in
depression, OCD symptoms, and anger.19 Sertraline was also studied
in an open, controlled trial with 11 patients for 64 weeks. At a 14-week
follow-up, the sertraline group showed improvements in depression,
ineffectiveness, and perfectionism. Both the sertraline and control groups
gained weight.20
The speculated reason SSRIs,
including fluoxetine, do not show consistent results is that SSRIs need some
serotonin available in the brain to work, and in a malnourished anorexic
patient the serotonin level is low.6,11,17 The amino acid
tryptophan is the precursor to serotonin and can only be acquired from dietary
sources. Hence, a person who is not eating will not synthesize serotonin, and
SSRIs will have little to no effect.
Obsessive-compulsive
tendencies may occur in patients with anorexia, along with anxiety in
recovering patients as they begin to see weight gain. The APA suggests the use
of SSRIs for these patients.4 Benzodiazepines should be used
cautiously in anxiety patients due to the likelihood of addiction in this
population.
Antipsychotic Agents
Anorexic patients
are also likely to have high rates of psychiatric conditions, including
personality disorders, delusional thoughts about their body, and mood
disturbances.13 Alterations in dopamine secretion by patients with
anorexia have been reported, but the exact mechanism is still unknown.21
The antipsychotic agents impact dopamine levels, which may alleviate the
psychiatric conditions and reduce the patient's resistance to gaining weight.
The atypical antipsychotics are associated with reducing severe agitation and
promoting mood stability, and weight gain, which may help anorexics with
psychiatric comorbidities.22 Specifically, olanzapine and
quetiapine have been used in small studies; however, larger clinical trials
are lacking.
Olanzapine has been the most
studied of the atypical antipsychotics for anorexia. A six-week, open-label
trial with 17 patients showed that olanzapine reduced depression, anxiety, and
core eating-disorder symptoms and significantly increased weight gain.22
The results from this study indicate that olanzapine may make anorexic
patients less resistant to treatment and help with compliance. Another
randomized, double-blind, placebo-controlled study with 30 patients supported
these findings but also suggested that olanzapine does not directly cause
weight gain; however, patients taking olanzapine were more willing to eat,
resulting in weight gain.21 Additionally, many case reports have
stated the positive results of weight gain during olanzapine therapy.9
Quetiapine can also lead to
weight gain and has recently been studied for its effect on psychiatric
comorbidities and weight gain in patients with anorexia.23 An
eight-week, open-label study with eight participants reported clinical
improvement in depression, OCD, and BMI after eight weeks of inpatient therapy.
23
The Role of the Pharmacist
A pharmacist
counseling a patient with anorexia is in an excellent position to try to make
the patient feel as comfortable with himself or herself as possible.
Counseling should be done carefully and tactfully, because many recovering
patients may have low self-esteem.
Many recovering patients may
be adolescents and therefore may need to be properly informed and educated
about the black box warning on antidepressants for increased risk of suicidal
thoughts and behavior in their population. A pharmacist can explain the
controversy behind this black box warning to the patient and may also need to
educate the physician and caregiver of the warning. A pharmacist may also need
to contact the practitioner and caregiver(s) if suicidality is noticed.
Additional counseling may be performed regarding the adverse effects
associated with the prescribed medications. Additionally, the antidepressant
bupropion should not be used in patients with eating disorders because of the
increased risk of seizures. Pharmacists should ensure that patients with
eating disorders are not on this drug.
Many pharmacists are in a
position within their stores to help identify abusive trends in the usage of
OTC agents that can modify weight, such as herbal stimulants, diet- and
metabolism-enhancing products, laxatives, enemas, and ipecac. During a drug
utilization review, pharmacists can also identify inappropriate use of legend
medication that can modify a person's weight. The quality of life for
recovering anorexics can improve as pharmacists incorporate their knowledge of
medications and compassion with patients' requirements.
Conclusion
Anorexia nervosa is
an eating disorder that can affect any patient population and displays widely
varying comorbidities. It is important to promote more research in this area
to improve outcomes in relapse and in symptoms associated with this eating
disorder. Health care providers, including pharmacists, need to be aware of
the signs of anorexia nervosa so that they can identify this disorder and
recommend early and appropriate treatment.
References
1. Henry BW, Ozier AD. Position of the American Dietetic Association: nutrition intervention in the treatment for anorexia nervosa, bulimia nervosa and other eating disorders. J Am Diet Assoc. 2006;106:2073-2082.
2. Marken PA, Sommi RW. Eating disorders. In: DiPiro JT, Talbert RL, Yee GC, et al., eds. Pharmacotherapy: A Pathophysiologic Approach. New York, NY: McGraw-Hill; 2005:1147-1156.
3. Sundgot-Borgen J. Eating disorders among male and female elite athletes. Br J Sports Med. 1999;33:434.
4. American Psychiatric Association. Treatment of patients with eating disorders. Am J Psychiatry. 2006;163(suppl 7):4-54.
5. American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Text Revision. Washington, DC: American Psychiatric Association; 2000.
6. Costin C. A Comprehensive Guide to the Causes, Treatments, and Prevention of Eating Disorders. 3rd ed. New York, NY: McGraw-Hill; 2007.
7. The Merck Manual On-line Medical Library. Available at: www.merck.com/mmpe/index.html. Accessed June 20, 2007.
8. National Institute of Mental Health. Eating Disorders--Facts About Eating Disorders and the Search for Solutions. Bethesda, MD: National Institute of Mental Health, National Institutes of Health, US Department of Health and Human Services; 2001. NIH Publication No. 01-4901.
9. Dunican KC, DelDotto D. The role of olanzapine in the treatment of anorexia nervosa. Ann Pharmacother. 2007;41:111-115.
10. Wilson TG, Grilo CM, Vitousek KM. Psychological treatment of eating disorders. Am Psychol. 2007;62:199-216.
11. Powers PS, Santana C. Available pharmacological treatments for anorexia nervosa. Expert Opin Pharmacother. 2004;5:2287-2292.
12. Attia E, Haiman C, Walsh BT, Flater SR. Does fluoxetine augment the inpatient treatment of anorexia nervosa? Am J Psychiatry. 1998;155:548-551.
13. Pederson KJ, Roerig JL, Mitchell JE. Towards the pharmacotherapy of eating disorders. Expert Opin Pharmacother. 2003;4:1659-1678.
14. Attia E, Mayer L, Killory E. Medication response in the treatment of patients with anorexia nervosa. J Psychiatr Pract. 2001;7:157-162.
15. Biederman J, Herzog DB, Rivinus TM, et al. Amitriptyline in the treatment of anorexia nervosa: a double-blind, placebo-controlled study. J Clin Psychopharmacol. 1985;5:10-6.
16. Gwirtsman HE, Guze BH, Yager J, Gainsley B. Fluoxetine treatment of anorexia nervosa: an open clinical trial. J Clin Psychiatry. 1990;51:378-382.
17. Kaye WH, Nagata T, Weltzin TE. Double-blind placebo-controlled administration of fluoxetine in restricting- and restricting-purging-type anorexia nervosa. Biol Psychiatry. 2001;49:644-652.
18. Walsh TB, Kaplan AS, Attia E, et al. Fluoxetine after weight restoration in anorexia nervosa: a randomized controlled trial. JAMA. 2006;295:2605-2612.
19. Fassino S, Leombruni P, Daga G, et al. Efficacy of citalopram in anorexia nervosa: a pilot study. Eur Neuropsychopharmacol. 2002;12:453-459.
20. Santonastaso P, Friederici S, Favaro A. Sertraline in the treatment of restricting anorexia nervosa: an open controlled trial. J Child Adolesc Psychopharmacol. 2001;11:143-1450.
21. Brambilla F, Garcia CS, Fassino S, et al. Olanzapine therapy in anorexia nervosa: psychobiological effects. Int Clin Psychopharmacol. 2007;22:197-204.
22. Barbarich NC, McConaha CW,
Gaskil J, et al. An open trial of olanzapine in anorexia nervosa. J Clin
Psychiatry. 2004;65:1480-1482.
23. Bosanac P,
Kurlender S, Norman T, et al. An open-label study of quetiapine in anorexia
nervosa. Hum Psychopharmacol. 2007;22:223-230.
To comment on this article, contact
editor@uspharmacist.com.





