US Pharm. 2017;42(3):HS14-HS17.
ABSTRACT: Perioperative pain management is an area of focus among surgeons and anesthesiologists for the surgical patient; however, if the interventions and drugs employed do not adequately treat the underlying pain, the pain could develop into a chronic problem or worsen patient outcomes. The pharmacist can play a valuable role in the pharmacological understanding of the different medications used in the perioperative clinical setting. Various techniques are used in the management of perioperative pain, including neuraxial opioid analgesia, patient-controlled analgesia with systemic opioids, peripheral regional analgesia, and multimodal agents. Pharmacists’ knowledge of pain and appropriate strategies in the treatment of acute perioperative pain can be beneficial to their patients’ well-being.
The management of acute pain poses a unique challenge to the physician and can often lead to chronic problems for the surgical patient. Often, it is the anesthesiologist or surgeon’s role to determine the appropriate perioperative doses of drugs to help reduce pain. About 10% of patients undergoing different types of surgeries can develop chronic pain postoperatively1; thus, it is imperative for pharmacists who practice in the inpatient setting to be thoroughly familiar with the agents used, as well as approaches to prevent chronic pain in the perioperative period. The purpose of this review is to highlight the drugs used in preventive analgesia, perioperative techniques, and multimodal agents used in perioperative pain management.
Preventive Analgesia
Recently, physicians have focused on interventions performed during the perioperative period as a mechanism for modifying chronic pain in postsurgical patients. Both gabapentin and pregabalin are widely prescribed for the treatment of neuropathic pain. In a double-blind, placebo-controlled study of a 4-day regimen of gabapentin added to celecoxib, Clarke et al evaluated total knee arthroplasty (TKA) patients’ in-hospital rehabilitation and physical function on postoperative day 4 and at 6 weeks and 3 months.2 Patients, who were randomized to either gabapentin 200 mg or placebo three times daily for 4 days, received femoral and sciatic nerve blocks and spinal anesthesia followed by IV patient-controlled analgesia (PCA) for 24 hours. Patients in the gabapentin treatment arm were found to have used less morphine during the first 24 hours post surgery and to have increased range of motion in the knee; however, no differences were observed in terms of pain or physical function on postoperative day 4, at 6 weeks, or at 3 months after surgery.2
Buvanendran et al evaluated the use of pregabalin compared to placebo in 240 patients after TKA.3 Pregabalin was dosed at 300 mg preoperatively, followed by 150 mg twice daily for 10 days post surgery, and then reduced to 50 mg twice daily for 4 days. In the pregabalin group, improvement in range of motion at 30 days and neuropathic pain reduction at 3 and 6 months were observed in comparison to placebo.3 While both of these trials used lower doses, the dosing of gabapentinoids was studied by Carroll et al, who recommended giving higher doses of gabapentin (1,200 mg) or pregabalin (300 mg) 2 hours preoperatively and then continuing gabapentin 400 to 600 mg three times daily or pregabalin 150 mg twice a day for at least 14 days to reduce the risk of acute or chronic pain.4
Although antidepressants such as amitriptyline and duloxetine are widely prescribed in the management of chronic and neuropathic pain through their effects on serotonin and norepinephrine, data from clinical trials in humans are limited and/or not studied extensively in the perioperative phase.4
Ketamine is a general anesthetic that works by blocking the N-methyl-D-aspartate (NMDA) glutamate receptor. In their evaluation of ketamine used in the perioperative setting, Sano et al assigned 16 patients to receive either ketamine or placebo intraoperatively.5 Ketamine was given as a bolus and followed with a continuous infusion. In this study, which focused on acute and chronic post-thoracotomy pain, the authors found that pain was reduced even 6 weeks postoperatively in patients who had used opioids chronically.5
Lavand’homme and colleagues evaluated the timing of continuous analgesics with clonidine in patients undergoing major surgeries involving the digestive tract.6 In this randomized, controlled study, analgesics were administered via epidural or continuous IV infusion prior to incision and then continued for another 72 hours after surgery. Residual pain through patient surveys was assessed at 2 weeks, followed by 1, 6, and 12 months post surgery. Results of this study found a benefit with continuous perioperative epidural analgesia in the perioperative period versus IV administration of clonidine.6
Other agents that are administered in the perioperative period due to their mechanism of action, but require further clinical studies, include systemic steroids, vitamin C, and lidocaine.4
Perioperative Techniques for Pain Management
Various techniques are used in the management of perioperative pain. Some of the more common methods include neuraxial opioid analgesia, PCA with systemic opioids, and peripheral regional analgesic techniques such as intercostal blocks, plexus blocks, and local anesthetic infiltration of incisions (TABLE 1). These modalities should be considered only after assessing the risks and benefits for each individual patient.7
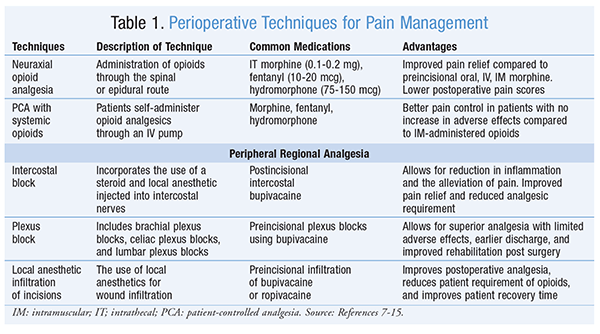
Neuraxial opioid analgesia refers to the administration of opioids through the spinal or epidural route, which includes administration as a single-injection, continuous infusion, as well as PCA.7 A commonly administered spinal anesthetic includes small doses of preservative-free intrathecal morphine (0.1-0.2 mg), fentanyl (10-20 mcg), or hydromorphone (75-150 mcg) as an alternative to morphine.8 Preincisional epidural or intrathecal morphine was found to have improved pain relief compared to preincisional oral, IV, or intramuscular (IM) morphine.7 Neuraxial opioid analgesia is associated with lower postoperative pain scores in adults and children who undergo surgery.9
According to the American Pain Society (APS), clinicians should consider the use of epidural or spinal analgesia for the management of postoperative pain in patients who undergo major surgeries, including thoracic and abdominal procedures, cesarean sections, and hip and lower-extremity surgeries; this is especially recommended for patients at risk for cardiac complications, pulmonary complications, or prolonged ileus.9
PCA allows patients to self-administer opioid analgesics such as morphine, hydromorphone, and fentanyl through an IV pump. The APS recommends the use of IV PCA when the parenteral route is needed for postoperative systemic analgesia.9 IV PCA therapy is considered appropriate for patients who require analgesia for at least a few hours who also have adequate cognitive function to operate the device.9 IV PCA allows for better pain control in patients with no increase in side effects, compared to IM-administered opioids.10 There is evidence showing greater effectiveness with PCA therapy, along with patient satisfaction; therefore, the use of IV PCA is recommended over opioid administration.9
Regional analgesic techniques include peripheral nerve blocks that can help reduce postoperative physiological stress and decrease complications associated with surgery if used properly and in combination with other forms of treatment. It has the potential to allow for adequate pain control while reducing the amount of opioid therapy needed to do so.11 Systemic adverse effects can be avoided as seen with epidural analgesia (e.g., hypotension, urinary retention) and PCA morphine (e.g., sedation).12 These techniques include intercostal blocks, plexus blocks, and local anesthetic infiltration of incisions.7
Intercostal Blocks: An intercostal nerve block incorporates the use of a steroid and a local anesthetic injected into intercostal nerves located near the ribs, allowing for a reduction in inflammation and the alleviation of pain.13 Various randomized, controlled trials report improved pain relief and reduced analgesic requirement with post-incisional intercostal bupivacaine compared to saline.7 Some patients may experience pain relief immediately after receiving the injection, although they may find the pain returning after a few hours when the anesthetic wears off.13
Plexus Blocks: Plexus block techniques include brachial plexus block and celiac plexus block, as well as lumbar plexus block.11,12 Continuous brachial plexus blocks allow for superior analgesia with limited adverse effects, as well as earlier discharge and improved rehabilitation post surgery.11 A meta-analysis of randomized, controlled trials reported equivocal pain relief and less analgesic use with preincisional plexus blocks using bupivacaine compared to saline.7 There have also been reports of lower pain scores with preincisional plexus blocks compared to no block, while postincisional intraarticular opioids showed equivocal pain scores and analgesic use compared to saline.7
Local Anesthetic Infiltration of Incisions: Wound infiltration is a postoperative analgesic technique that helps improve postoperative analgesia, reduce patient requirement of opioids, and improve patient recovery time.14 The use of local anesthetics for wound infiltration allows for effective analgesia for various surgical procedures, with limited major adverse effects.15 A meta-analysis of randomized, controlled trials reported improved pain scores and equivocal analgesic use with preincisional infiltration of bupivacaine compared to saline, as well as reports of improved pain scores and a reduction in analgesic use with the preincisional infiltration of ropivacaine compared to saline.7
Multimodal Techniques for Pain Management
Multimodal techniques for pain management involve using two or more analgesic drugs with different mechanisms of action working in synergy (TABLE 2). These drugs may be given by either the same or different routes of administration preoperatively, intraoperatively, and/or postoperatively.7 By targeting different pain pathways within the central and peripheral nervous systems, the use of multiple agents with different mechanisms of action allows for lower doses of individual agents, which in turn results in a lower risk of adverse effects. The lower incidence of adverse effects and improved pain management may further result in shorter hospitalization times, improved patient recovery, and rehabilitation and decreased costs of care.16

The APS and the American Society of Anesthesiologists (ASA) recommend the use of different pharmacologic agents and have developed guidelines to promote evidence-based, safe, and effective pain management.7,9 Multimodal techniques are typically initiated preoperatively to prevent postoperative pain. Studies have shown that the combined use of systemic opioids and nonsteroidal anti-inflammatory drugs (NSAIDs) relieved postoperative pain more effectively than single-drug regimens.17 Although there is not a standardized multimodal pain-management regimen, guidelines recommend the use of combinations of systemic opioid and nonopioid analgesics, in addition to central regional analgesics.7,9
Systemic Analgesics: Nonopioid systemic analgesics, such as acetaminophen, selective cyclooxygenase-2 inhibitors (COXIBs), nonselective NSAIDs, and calcium channel alpha2-delta antagonists (gabapentin and pregabalin), should be considered as part of a postoperative multimodal pain-management regimen. Moreover, implementing around-the-clock COXIBs, NSAIDs, or acetaminophen is recommended, unless contraindicated.7 NSAIDs are commonly included in many order sets in an effort to reduce opioid consumption, especially during the immediate postoperative stage.
Systemic opioids commonly used for multimodal analgesia include morphine, fentanyl, hydromorphone, and sufentanil. Most systemic opioids can be administered via parenteral, oral, transdermal, neuraxial, and rectal routes or via a PCA pump.7,9
According to the APS, oral administration of opioids for postoperative pain management is recommended over IV administration in patients who can tolerate oral medications.9 Studies have shown that the concurrent use of acetaminophen or NSAIDs with opioids is associated with decreased opioid usage and less postoperative pain when compared with opioids alone.9
Central Regional Analgesics: Central regional analgesic techniques refer to the use of intrathecal or epidural opioids, such as morphine, fentanyl, and sufentanil; epidural opioids plus local anesthetics, such as bupivacaine and ropivacaine; or epidural opioids plus clonidine.9 Epidural opioids combined with local anesthetics have been found to have improved pain scores when compared with either epidural opioids or local anesthetics alone, as reported in the meta-analyses of randomized, controlled trials.7 Based upon multiple trials that have showed the effectiveness of local anesthetics combined with systemic analgesics, the APS recommends the use of local anesthetic-based regional anesthesia techniques for surgical procedures of the extremities, abdomen, and thorax.9
In a prospective randomized, controlled trial, Lamplot et al compared TKA patients with intraoperative periarticular injections containing bupivacaine, morphine, and ketorolac versus a control group without the intraoperative intervention.18 The researchers found that patients receiving periarticular injections reported overall lower pain scores, decreased narcotic usage, and significantly fewer adverse reactions.18
Multimodal pain-management therapy should be used whenever possible, and each plan, including the medication, dose, route, and duration of therapy, should be individualized.7 Pharmacists can also help optimize drug regimens by verifying doses of individual agents and screening for adverse effects. Tailoring pain-management plans to patients’ needs has many associated benefits, such as effective pain management, reduced postoperative opioid usage, and reduced length of hospital stay.9
Lee and colleagues conducted a prospective study in 61 patients who underwent upper-extremity surgery.19 Patients were randomized to receive either multimodal analgesia (ibuprofen, celecoxib, and pregabalin) or PCA, and all patients received scheduled oxycodone 10 mg every 12 hours and acetaminophen 650 mg three times daily postoperatively. Outcomes evaluated included the use of rescue medication, complications related to opioid use, and patient satisfaction. The use of rescue pain medications was higher in the PCA group once the PCA was removed, as were complications related to opioids on the day of surgery and at postoperative day one. Patient satisfaction was recorded as higher in the multimodal-analgesic group.19
Conclusion
The management of postoperative pain involves a unique multifaceted approach that entails treatment prior to incision, as well as techniques during the perioperative phase, in an effort to prevent the development of acute to chronic pain. The safe and effective use of multimodal agents from different therapeutic classes working synergistically seems to be a promising facet in the treatment of pain that requires further studies in this patient population.
REFERENCES
1. Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: risk factors and prevention. Lancet. 2006;367(9522):1618-1625.
2. Clarke HA, Katz J, McCartney CJ, et al. Perioperative gabapentin reduces 24 h opioid consumption and improves in-hospital rehabilitation but not post-discharge outcomes after total knee arthroplasty with peripheral nerve block. Br J Anaesth. 2014;113(5):855-864.
3. Buvanendran A, Kroin JS, Della Valle CJ, et al. Perioperative oral pregabalin reduces chronic pain after total knee arthroplasty: a prospective, randomized, controlled trial. Anesth Analg. 2010;110(1):199-207.
4. Carroll I, Hah J, Mackey S, et al. Perioperative interventions to reduce chronic postsurgical pain. J Reconstr Microsurg. 2013;29(4):213-222.
5. Sano M, Inaba S, Yamamoto T, Nishino T. Intraoperative ketamine administration reduced the level of post-thoracotomy pain. Masui. 2005;54(1):19-24.
6. Lavand’homme P, De Kock M, Waterloos H. Intraoperative epidural analgesia combined with ketamine provides effective preventive analgesia in patients undergoing major digestive surgery. Anesthesiology. 2005;103(4):813-820.
7. American Society of Anesthesiologists Task Force on Acute Pain Management. Practice guidelines for acute pain management in the perioperative setting: an updated report by the American Society of Anesthesiologists Task Force on Acute Pain Management. Anesthesiology. 2012;116(2):248-273.
8. Sviggum HP, Arendt KW, Jacob AK, et al. Intrathecal hydromorphone and morphine for postcesarean delivery analgesia: determination of the ED90 using a sequential allocation biased-coin method. Anesth Analg. 2016;123(3):690-697.
9. Chou R, Gordon DB, de Leon-Casasola OA, et al. Management of post-operative pain: a clinical practice guideline from the American Pain Society, the American Society of Regional Anesthesia and Pain Medicine, and the American Society of Anesthesiologists’ Committee on Regional Anesthesia, Executive Committee, and Administrative Council. J Pain. 2016;17(2):131-157.
10. Garimella V, Cellini C. Postoperative pain control. Clin Colon Rectal Surg. 2013;26(3):191-196.
11. De Pinto M, Dagal A, O’Donnell B, et al. Regional anesthesia for management of acute pain in the intensive care unit. Int J Crit Illn Inj Sci. 2015;5(3):138-143.
12. Grant CRK, Checketts MR. Analgesia for primary hip and knee arthroplasty: the role of regional anaesthesia. Contin Educ Anaesth Crit Care Pain. 2008;8(2):56-61.
13. Cleveland Clinic. Intercostal nerve block. http://my.clevelandclinic.org/services/anesthesiology/pain-management/treatments-procedures/intercostal-nerve-block. Accessed November 30, 2016.
14. Kvolik S, Kristek J, Sakic´ K, et al. A wound infiltration as a method of postoperative analgesia. Periodicum Biologorum. 2009;111(2):241-246.
15. Scott NB. Wound infiltration for surgery. Anaesthesia. 2010;65(suppl 1):67-75.
16. Buvanendran A, Kroin JS. Multimodal analgesia for controlling acute postoperative pain. Curr Opin Anaesthesiol. 2009;22(5):588-593.
17. Jin F, Chung F. Multimodal analgesia for postoperative pain control. J Clin Anesth. 2001;13(7):524-539.
18. Lamplot JD, Wagner ER, Manning DW. Multimodal pain management in total knee arthroplasty: a prospective randomized controlled trial. J Arthroplasty. 2014;29(2):329-334.
19. Lee SK, Lee JW, Choy WS. Is multimodal analgesia as effective as post-operative patient controlled analgesia following upper extremity surgery? Orthop Traumatol Surg Res. 2013;99(8):895-901.
To comment on this article, contact rdavidson@uspharmacist.com.






