US Pharm. 2015;40(12):17-18.
Chronic Inflammatory Disease of the Colon
Ulcerative colitis is a chronic inflammatory disease of the colon (large intestine) that causes ulcerations and swelling of the intestinal lining. For most patients, ulcerative colitis symptoms begin gradually and worsen slowly, with periods of improvement between flare-ups. The cause may be genetic, immunologic, environmental, or a combination of these factors. Common symptoms include bloody diarrhea, abdominal pain, poor appetite, fever, and weight loss. Treatment includes stepwise measures, with specific drugs targeted to the severity of symptoms. The goal of therapy is to relieve symptoms and maintain a symptom-free period (remission). In severe cases that do not respond to drug therapy, a surgical cure can be accomplished by removing the colon.
Periods of Remission Alternate With Flares of Symptoms
Ulcerative colitis is a type of inflammatory bowel disease that causes swelling and ulceration of the inner lining of the large intestine and rectum. It is a chronic condition, although symptoms may improve or worsen throughout a person’s lifetime.
Causes and Symptoms
The cause of ulcerative colitis is not fully understood. It is most likely the result of an overactive immune system that causes inflammation in the lining of the colon similar to the inflammation seen in an infection. A family history of ulcerative colitis increases the risk, but an exact genetic link has not been discovered. There may also be an environmental cause or a combination of causes. People of European origin or Jewish descent are at higher risk for developing ulcerative colitis.
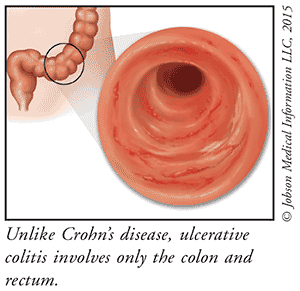
Symptoms of ulcerative colitis are diarrhea with blood, abdominal pain, cramping, a sudden urge to pass stool, poor appetite, weight loss, fatigue, and fever. The diagnosis is based on symptoms, a physical examination, and blood and stool sample testing. Endoscopy can confirm ulcerative colitis by allowing the doctor to look at the walls of the intestines and take a sample of tissue using a lighted tube inserted into the rectum.
Goals of Therapy
The goal of treatment is to control intestinal inflammation and ulceration to relieve symptoms. Avoiding foods that increase symptoms (acidic, spicy, or high-fiber) may help some people. A healthy, balanced diet of appealing foods is the goal to counteract the problem of poor appetite.
Medication can relieve symptoms completely or reduce the number or severity of flare-ups. Drug therapy reduces inflammation and helps heal ulcers in the intestinal wall. There are several classes of drugs used to treat ulcerative colitis. Often, patients will be treated with more than one class of drug to achieve the best results.
In mild cases or to keep symptoms in remission, an aminosalicylate is often chosen. Examples are sulfasalazine and mesalamine. Corticosteroids (steroids) are also used to control inflammation, either by mouth or in a rectal dosage form. Although steroids such as prednisone can be used by mouth, their long-term use has side effects, and they must be tapered slowly when discontinued. Locally applied steroids, such as budesonide in a rectal foam, have fewer systemic side effects. If other classes of medications do not eliminate symptoms, immunomodulators are another option. These medicines block the immune system from causing inflammation. Examples are azathioprine, mercaptopurine, and cyclosporine.
Recently, biologics have been developed to treat more serious cases of ulcerative colitis that do not respond to other agents. Biologics such as infliximab, adalimumab, and golimumab interfere with the body’s inflammation response, stopping the symptoms of ulcerative colitis. An IV drug recently approved for adult patients who do not respond to any other therapy is vedolizumab, a monoclonal antibody that works specifically in the intestine to block inflammation.
Complications
Complications of ulcerative colitis can be serious and include dehydration, blood loss, and perforation (hole) in the colon wall. People with ulcerative colitis are also at higher risk for colon cancer and should be monitored with regular colonoscopies.
In more than one-fourth of patients, drug therapy does not control symptoms and surgery may be indicated. Depending on the patient, the entire colon and rectum are removed, and an external opening on the abdomen is covered with a pouch to empty waste. A newer procedure removes only the colon, and an internal pouch is created and attached to the rectum to allow for more normal defecation.
To comment on this article, contact rdavidson@uspharmacist.com.





