US Pharm. 2015;40(9):33-37.
ABSTRACT: Hormone replacement therapy is an important element of managing symptoms experienced by menopausal women. Both synthetic and compounded hormone replacement products are widely used to manage decreased sexual function and unwanted vasomotor symptoms, including hot flashes and night sweats. Given the vast number of hormone combinations and delivery methods available, selection of the proper product is dependent on symptoms, adverse events, and patient-specific factors. Pharmacists can play a large part in helping patients and prescribers with product selection and symptom management. In order to do this, it is important for pharmacists to understand the role of hormones in the female body and the symptoms associated with hormone excess and deficiency.
Hormone replacement therapy (HRT) is a key element of managing the symptoms experienced by menopausal women. The objective of this article is to discuss the general role of hormones in the female body, symptoms caused by hormone excess and deficiency, and options for replacement therapy. The reader will become familiar with products currently on the market and with the role pharmacists can play in the management of HRT in female patients going through menopause.
Hormone Basics
HRT is a topic most women will discuss with their friends, physician, and possibly their pharmacist as they approach menopause. With so many options available, including rings, patches, creams, tablets, and capsules, how does the pharmacist conduct this challenging conversation? Most pharmacists can clearly and concisely explain diabetes, hypertension, and asthma, but what about the balance between estrogen and progesterone? How does the pharmacist explain to a patient why her doctor is recommending testosterone replacement, or why the HRT that is effective for her friend may not be the best option for her?
HRT was developed to reduce (and, hopefully, eliminate) the undesirable symptoms of menopause. Menopausal symptoms are experienced when the hormones typically produced by the ovaries during the reproductive years begin to decline. Symptoms of hormone imbalance include weight gain, hot flashes, dry skin, vaginal dryness, headaches, irritability, mood swings, insomnia, decreased sex drive, and fatigue. Symptoms of specific hormone excesses and deficiencies are listed in TABLE 1. By supplementing or replacing these hormones with manufactured or specially compounded HRT, many women are able to correct the hormone imbalances contributing to menopausal symptoms. The first step to understanding hormone imbalances is to become familiar with the roles of the individual hormones and the body’s natural hormonal cascade (FIGURE 1).1

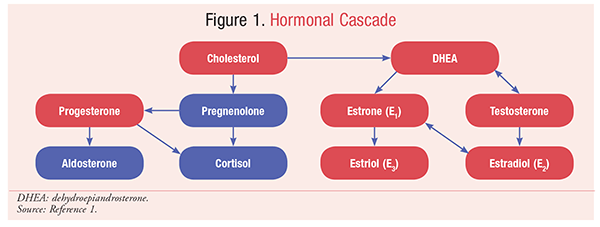
The adrenal glands and ovaries produce a series of hormones that are derived from LDL cholesterol. After being converted to pregnenolone, the hormone cascade separates into two chains; one chain forms progesterone, aldosterone, and cortisol, and the other forms dehydroepiandrosterone (DHEA), testosterone, and estrogen.1
Estrogen: Often thought of as a single female sex hormone, estrogen actually encompasses to a group of female hormones produced by the ovaries. Estrogen travels throughout the body, enabling hundreds of crucial functions, including temperature regulation, muscle maintenance, blood pressure regulation, decreased plaque accumulation, and many others. Estrogen deficiency may be caused by menopause, whereas excess estrogen may be due to impaired estrogen elimination, lack of exercise, or a diet low in grains or fiber.1
There are three different types of estrogen: estrone (E1), estradiol (E2), and estriol (E3). Estradiol, the strongest form of estrogen, has often been referred to as the “estrogen of youth” since it is most abundant in females in their teens and 20s. Estrone, the main form of estrogen produced after menopause, is derived from estradiol and functions similarly, only more weakly. Currently, the only known function of estrone is to serve as a reservoir of estrogen. Estriol is the least active form of estrogen, but it has been found beneficial for vaginal symptoms of menopause (including painful intercourse and vaginal dryness and thinning) and urinary incontinence.1
High estrogen levels are believed to be associated with an increased risk of developing breast or uterine cancer. This view is supported by several studies, including the Women’s Health Initiative (WHI), that compared estrogen-progestin therapy with placebo in more than 16,000 women. High levels of estrone and estradiol are associated with increased activity in breast and uterine tissue, which is thought to increase the risk of breast and uterine cancer.2 Estriol is much less active in breast and uterine tissues, and it may actually help protect against cancer.1
Progesterone: Progesterone is a sex hormone involved in menstruation and pregnancy. Progesterone is produced mostly in the ovaries, with a small amount continuing to be made in the adrenal glands after menopause. Other roles of progesterone include balancing estrogen, building bone, regulating moods, and aiding in proper bladder function. Women with low levels of progesterone may experience anger, irritability, and anxiety.1
Androgens: DHEA and testosterone belong to a group of hormones known as androgens. DHEA, a sex hormone made by the adrenal glands, is one of the first steps in the cascade toward testosterone and estrogen. DHEA serves many purposes, including protecting against cancer, diabetes, obesity, hyperlipidemia, and several other conditions.1,3 Although testosterone is typically thought of as a male hormone, it is also present in females. Most of the testosterone in the female body is bound to sex hormone-binding globulin, which keeps it from exhibiting an effect on the body. The remaining testosterone helps prevent excess body fat, avoid bone breakdown, improve muscle tone, and increase sexual interest.1
Although it is far less common than estrogen deficiency, androgen deficiency is another hormonal imbalance that can occur in females. Androgen deficiency can imply a decrease in any of the major androgens: DHEA sulfate, DHEA, testosterone, and dihydrotestosterone (DHT). DHEA sulfate and DHEA are prohormones, which means that they require activation to testosterone and DHT to exert their effects on sexual function and prevent bone loss. Unlike excess-androgen syndromes such as polycystic ovarian syndrome, there is currently no androgen-deficiency syndrome defined in females, nor are there strict biochemical criteria to diagnose androgen deficiency.4
Therapeutic Options
There are many products for HRT, including synthetically manufactured hormones available commercially and bioidentical hormone products compounded specifically to meet the patient’s needs. Both come in a variety of dosage forms, including tablets, patches, and vaginal creams and rings. Compounded products may come in additional dosage forms, such as transdermal creams, troches (small lozenges), and capsules. Topical creams are applied to the wrist or behind the knee, where the skin is thin with high blood perfusion. Troches are dissolved in the mouth, allowing the hormone to be absorbed without being altered by digestion.5 In compounding HRT, the compounder can alter the concentration of each hormone to target the patient’s specific symptoms while avoiding the side effects of some commercial preparations.
The first step in choosing an HRT product is to identify which hormone or hormones need to be supplemented or replaced. Age is another factor to consider with HRT, as most adverse effects seen in the WHI trials occurred in women older than 60 years. Most women experience menopause in their 40s or 50s, however, so this is when HRT would be most beneficial. Young, healthy patients going through menopause should be reassured that the risk is very low when using HRT for a duration of 5 years.6 In clinical practice, patients have been known to use HRT for up to 10 years. The HRT product is then gradually titrated to the lowest effective dosage possible while avoiding symptoms of hormone deficiency.
Common symptoms in patients with declining estrogen include hot flashes, dry skin and hair, night sweats, vaginal dryness, and incontinence. Since estrogen therapy is not without its risks, it is important to start with the lowest dosage and slowly titrate to an effective dosage.7 Options for estrogen-only products include Estrace oral tablets (estradiol), Vivelle-Dot patches (estradiol), and Premarin tablets (conjugated estrogen). For more localized vaginal symptoms, Premarin cream is an effective option that avoids other symptoms of increased estrogen, such as weight gain, mood swings, and breast tenderness.
The presence or absence of the uterus is another important factor to consider when an HRT product is being selected. Unopposed estrogen—estrogen therapy alone without progesterone—has been shown to increase the risk of endometrial hyperplasia and endometrial cancer, so women with a uterus should avoid receiving estrogen without progesterone to prevent the risk of uterine hyperplasia.7,8 The presence of a uterus should not be considered an absolute contraindication to HRT, although therapy should be limited to 5 years based on the increased risk of breast cancer.7 Another risk associated with prolonged estrogen therapy is the development of blood clots leading to pulmonary embolism and stroke. As with all prescriptions, the risks versus benefits of HRT should be discussed with the patient before initiation. Many women using HRT report improvements in sleep, sexual functioning, and vasomotor symptoms and experience an overall improvement in quality of life.9,10 In the WHI trials, the risk-versus-benefit ratio was more favorable in younger patients receiving conjugated estrogens who had a previous hysterectomy, compared with patients receiving conjugated estrogen and medroxyprogesterone acetate.11
Progestins: Progestin, a synthetic progesterone, is often administered together with estrogen to negate the effects of long-term estrogen therapy. Medroxyprogesterone acetate, a common progestin, was used in the WHI trials.8 Commercially available combination estrogen and progestin products include Prempro (conjugated estrogens and medroxyprogesterone) and Femhrt (ethinyl estradiol and norethindrone). Medroxyprogesterone alone as a separate tablet in addition to estrogen-only tablets is also an appropriate option to prevent the risks associated with unopposed estrogen.
Testosterone Supplementation: Supplementation of testosterone is usually limited to the improvement of sexual function in menopausal women.11 However, many women with low levels of testosterone experience depression, headaches, and fatigue, in addition to the typical symptoms of decreased sex drive and trouble reaching climax. In clinical practice, testosterone supplementation is often used to eliminate these symptoms, and it should be considered a part of the overall hormone balance. In addition, a study of 51 women using testosterone replacement for androgen deficiency caused by hypopituitarism reported free testosterone levels that reached the upper limit of normal, increased bone mineral density of the hip and radius, greater fat-free mass, and increased thigh muscle, but there was also an increase in acne.12
DHEA Replacement: DHEA replacement is another consideration, as DHEA is converted to testosterone. However, based on available data, the Endocrine Society recommends against the use of DHEA in women for improvement of sexual function. Some experts suggest a trial of DHEA in menopausal and postmenopausal women with significantly impaired mood or sense of well-being despite treatment with optimal glucocorticoid and mineralocorticoid replacement therapy.13 Since DHEA is available OTC, pharmacists can provide education on symptoms and replacement therapy to women interested in purchasing this product.
The Pharmacist’s Role
With so many options for HRT, what role should the pharmacist play in the management of HRT in menopausal women? In addition to providing therapy-optimization recommendations and patient counseling to ensure safe and effective HRT use, pharmacists are also being asked by third-party insurance plans to discourage the initiation of, or discontinue the use of, high-risk medications such as estradiol when performing medication therapy management. The pharmacist should review the patient’s profile and discuss the risks and benefits of starting or continuing therapy. If the patient wants to discontinue the hormone therapy, possible options for symptom control include local estrogen (e.g., Estring or Premarin Vaginal Cream) for vaginal symptoms; venlafaxine, fluoxetine, sertraline, or paroxetine for vasomotor symptoms; and alendronate, calcium plus vitamin D, or raloxifene for osteoporosis prevention.13
Raloxifene (Evista), a selective estrogen receptor modulator, is an option for menopausal and postmenopausal patients who cannot tolerate bisphosphonate therapy for osteoporosis prevention. Raloxifene inhibits bone resorption, reduces the risk of vertebral fracture, and decreases the risk of invasive breast cancer, but it increases the risk of blood clot formation. Some clinicians prefer to limit raloxifene therapy for osteoporosis prevention to a maximum of 8 years, based on insufficient evidence regarding longer use.14
In addition to verifying the appropriate hormone product, dosage, frequency, and therapy duration, pharmacists are becoming more involved in therapy selection by collaborating with providers. This is a growing specialty for pharmacists in the arena of compounded products. Pharmacists, as the most trusted healthcare provider, often receive detailed information from female patients about their HRT. Pharmacists are highly accessible to the public, enabling many patients to discuss their symptom improvement—or lack thereof—with a simple phone call as often as necessary. A patient may report improved vasomotor symptoms or a side effect to her pharmacist when she picks up her monthly refill, before she returns to her physician for a follow-up appointment.
Whereas manufactured HRT is available in a specific number of dosages and dosage forms, compounded therapies can be individualized for each patient. Compounded hormone medications can be altered in small increments to alleviate menopausal symptoms while minimizing risks. The bioidentical hormones used in prescription compounding have the exact chemical structure of the body’s natural hormones. This allows the product to be recognized by the body and to mimic the function of the hormones the patient produces on her own. Specialty compounding pharmacists gain extensive knowledge, training, and experience in their field, allowing many providers to consider them hormone therapy experts. Many compounding pharmacists work alongside providers to prescribe appropriate HRT for their patients.
In this model, the patient is referred to a pharmacist by a prescriber for an HRT consultation. The patient is asked to give a background history containing pertinent health information and to describe her current menopausal symptoms. This information is combined with the patient’s laboratory values, and the pharmacist recommends an appropriate therapy to the prescriber to be approved. Once the therapy is approved, the patient, prescriber, and compounding pharmacist work as a team to adjust the dosage until symptom improvement is seen. Many patients have found relief from menopausal symptoms and improvement in their health and quality of life through this route. As with many compounded medications, there are not many large studies on their efficacy, but compounding pharmacists continue to be a valuable resource for many patients.
Conclusion
In summary, many HRT products are available to alleviate symptoms associated with menopause. Several medications are available commercially, whereas others are compounded in accordance with the needs of the individual patient. Commercial products are available in a variety of dosage forms, including tablets, patches, vaginal creams, and vaginal rings. The majority of compounded HRT products are in the form of creams, troches, or capsules. Medications are chosen based on the patient’s level of deficiency of natural hormones, including estrogen, progesterone, and testosterone. Although there are risks associated with HRT, there are several clinically significant benefits in terms of alleviating unwanted menopausal symptoms.
Pharmacists should continue to assist with HRT management, as their extensive knowledge of prescription products and the role of hormones in the female body qualifies them to identify the most appropriate products based on symptoms and laboratory values. Pharmacists also are capable of recommending and compounding HRT at the request of a prescriber. By collaborating with patients and providers, pharmacists may be the key to therapy optimization in women experiencing menopausal symptoms.
REFERENCES
1. Smith PW. What You Must Know About Women’s Hormones. Garden City Park, NY: Square One Publishers; 2010.
2. Manson JE, Chlebowski RT, Stefanick ML, et al. Menopausal hormone therapy and health outcomes during the intervention and extended poststopping phases of the Women’s Health Initiative randomized trials. JAMA. 2013;310:1353-1368.
3. Hutchinson KA. Androgens and sexuality. Am J Med. 1995;98:111S-115S.
4. Rosner W, Auchus RJ, Azziz R, et al. Position statement: utility, limitations, and pitfalls in measuring testosterone: an Endocrine Society position statement. J Clin Endocrinol Metab. 2007;92:405-413.
5. Pencol Compounding Pharmacy. Alternate delivery methods.
http://pencolrx.com/alternate_delivery_methods.html. Accessed May 15, 2015.
6. Santen RJ, Allred DC, Ardoin SP, et al. Postmenopausal hormone therapy: an Endocrine Society scientific statement. J Clin Endocrinol Metab. 2010; 95:S1-S66.
7. Roussouw JE, Anderson GL, Prentice RL, et al. Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results from the Women’s Health Initiative randomized controlled trial. JAMA. 2002;288:321-333.
8. Anderson GL, Judd HL, Kaunitz AM, et al. Effects of estrogen plus progestin on gynecologic cancers and associated diagnostic procedures: the Women’s Health Initiative randomized trial. JAMA. 2003;290:1739-1748.
9. Zethraeus N, Johannesson M, Henriksson P, Strand RT. The impact of hormone replacement therapy on quality of life and willingness to pay. Br J Obstet Gynaecol. 1997;104:1191-1195.
10. Welton AJ, Vickers MR, Kim J, et al. Health related quality of life after combined hormone replacement therapy: randomised controlled trial. BMJ. 2008;337:a1190.
11. Miller KK, Biller BM, Beauregard C, et al. Effects of testosterone replacement in androgen-deficient women with hypopituitarism: a randomized, double-blind, placebo-controlled study. J Clin Endocrinol Metab. 2006;91:1683-1690.
12. Alkatib AA, Cosma M, Elamin MB, et al. A systematic review and meta-analysis of randomized placebo-controlled trials of DHEA treatment effects on quality of life in women with adrenal insufficiency. J Clin Endocrinol Metab. 2009;94:3676-3681.
13. PriorityHealth. CMS/Medicare high-risk medication list. www.priorityhealth.com/provider/clinical-resources/medication-resources/high-risk-meds. Accessed May 10, 2015.
14. Siris ES, Harris ST, Eastell R, et al. Skeletal effects of raloxifene after 8 years: results from the continuing outcomes relevant to Evista (CORE) study. J Bone Miner Res. 2005;20:1514-1524.
To comment on this article, contact rdavidson@uspharmacist.com.





