US Pharm.
32(11):34-43.
Autistic disorder (AD) is one of the
great modern medical mysteries; the cause of the condition is unknown, and,
despite significant research, no cure is available. Caring for an autistic
child can be frustrating and one of the biggest challenges a parent or
caregiver may ever face. An autistic child resists affection and seems
disconnected from the outside world. In many cases, the child develops
normally during the first few years of life until the disease takes hold,
causing him or her to regress and lose many communication skills. Ultimately,
the parent or caregiver may feel helpless despite his or her best effort to
care for the child.
The term autistic is derived from the Greek word autos, meaning
"self." In 1911, psychiatrist Eugen Bleuler used the term
autistic to describe the social isolation of schizophrenia.1 To
this day, AD and schizophrenia are thought to be closely related. In the
1940s, researchers Leo Kaner and Hans Asperger published separate reports
defining autism as a psychological disorder and provided case studies to
describe its clinical characteristics.1 Although the condition is
commonly referred to as autism in older literature and by the media,
autistic disorder is now the preferred terminology in the medical field.
AD is classified as one of the five types of pervasive developmental
disorders, also known as autistic spectrum disorder (ASD).2
Other pervasive developmental disorders include Asperger's syndrome, childhood
disintegrative disorder, Rett's syndrome, and pervasive developmental disorder
not otherwise specified.2 Although AD and Asperger's syndrome share
many of the same symptoms, children with AD are generally diagnosed at an
earlier age, experience more communication and social impairments, and score
lower on IQ tests than do children with Asperger's syndrome.3
While its clinical presentation varies from individual to individual, AD is
defined broadly as a complex neurologic disorder involving several regions of
the brain.2 The condition is characterized by a triad of
symptoms--an impairment in social interaction, a deficit in communication
skills, and a routine, repetitive pattern of behavior.2 AD affects
approximately one in every 1,000 children and is three to four times more
prevalent in boys than it is in girls.2 Many reports indicate a
recent increase in incidence of AD in the United States, although the rise may
be due in part to better diagnostic procedures.3
Etiology and Pathophysiology
The etiology of AD is unknown.
Although many factors have been hypothesized to have a role in its
development, there is no conclusive evidence. Genetics seems to be linked
strongly to its origin; other possible links include pregnancy/birth
complications and food allergies.4
The most controversial theory regarding the etiology of AD is the alleged link
between the condition and the measles, mumps, and rubella (MMR) vaccine (or
any other vaccine containing thimerosal). The link was postulated based on the
pediatric vaccination timetable. Children receive the MMR vaccine at or after
12 months of age.5 Signs of AD may begin to appear at this time or
a few months later. Opponents of this theory attribute the link to a timing
coincidence. Although a child may be autistic prior to receiving the
vaccination, signs of the condition do not present until the child displays
impairment in communication and interaction skills. Generally, the earliest
signs of impairment are not measurable until the child reaches 12 months,
which coincides with the timing of the vaccination.2 The most
recent studies in this area indicate that no direct relationship exists
between vaccinations and the development of AD.5 In fact, the
American Academy of Pediatrics, the Institute of Medicine, and the Centers for
Disease Control and Prevention do not support the theory due to the lack of
substantial evidence proving a link.2
Because the exact cause of AD is unknown, the pathophysiology is also largely
unknown. Abnormalities seem to originate in the amygdala and the left frontal
cortex of the brain.6 Neurons in these areas appear smaller than
those in healthy individuals and have fewer connections to other regions of
the brain.6 This decrease in neuronal activity may cause the
clinical signs and symptoms that appear in autistic individuals.6
Risk Factors
Certain genetic conditions may predispose an individual to developing autism.
Such conditions include fragile X syndrome, tuberous sclerosis, untreated
phenylketonuria, and congenital rubella syndrome.2 Fragile X
syndrome is one of the most common causes of mental retardation and
neuropsychiatric disease. The syndrome is caused by a trinucleotide repeat at
an inherited fragile site on the X chromosome. Symptoms include delayed
speech, hyperactivity, tactile defensiveness, and gross motor delays.3
Tuberous sclerosis is a rare genetic disease that causes benign tumors
to grow in the brain and other vital organs, such as the kidneys, heart, eyes,
lungs, and skin. Tuberous sclerosis commonly affects the central nervous
system. In addition to benign tumors, other common symptoms include seizures,
mental retardation, behavioral problems, and skin abnormalities.7
Phenylketonuria is an inherited error of metabolism caused by a deficiency
in the enzyme phenylalanine hydroxylase. If left untreated, the enzyme
deficiency results in mental retardation and organ damage.7
Congenital rubella syndrome is an infection by the rubella virus during
the first trimester of pregnancy, causing heart disease, deafness, and
blindness in the newborn.8
Clinical Presentation
Patients with AD experience symptoms that are highly variable in terms of
severity, range, and progression. The first signs of AD typically develop by
age 3 and continue throughout life, although they may be alleviated by
treatment.2
Early signs and symptoms that should alert parents and pediatricians that a
child needs further evaluation for AD include the child's not smiling by six
months of age; not babbling, pointing, or using other gestures by 12 months;
and not using single words by 16 months. Furthermore, the child does not use
two-word phrases by 24 months and demonstrates regression in his or her
development with any loss of language or social skills.
Infants with AD may also avoid eye contact and, as they get older, act as if
they are unaware of when people come and go around them. Although AD is not
usually diagnosed until about age 3, some experts believe that some children
as young as six months begin to show subtle signs. Many autistic individuals
suffer from complications such as seizures, bipolar disorder, and depression.
3 While the majority of children with AD are intellectually challenged,
a small percentage are classified as autistic savants.2
Autistic savants are defined as autistic individuals who display the common
symptoms of AD but also have extraordinary mental abilities, most often in the
fields of numerical calculation, art, and music.2
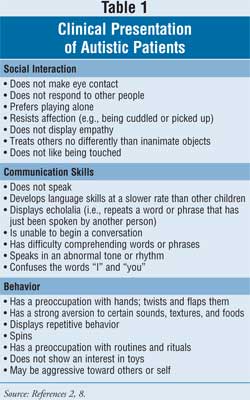
Signs and symptoms of AD can be categorized into three main areas: social
interaction, communication skills, and behavior. Table 1 provides
examples of symptoms specific to each category. Certain deficits in the
child's development may alert parents to the possibility that their child has
AD. Parents should consult a pediatrician if their child does not babble or
make gestures by 12 months of age, does not use single words by 16 months of
age, does not use two-word phrases by 24 months of age, or seems to have lost
a skill he or she previously had at any age.9 These are "red flags"
that are absolute indications for immediate evaluation.
Diagnostic Evaluation
In October 2007, two new clinical reports from the American Academy of
Pediatrics were released to help pediatricians diagnose ASDs earlier and guide
families to effective interventions.10,11 The goal is to improve
the lives of children with ASDs and their families. The first report
advocates universal screening, which implies pediatricians conduct formal ASD
screening on all children at 18 and 24 months regardless of whether there are
any signs of ASD.10 Although tests such as electroencephalography
and computed tomography may appear abnormal, no single laboratory test can
confirm a diagnosis of AD.3 Screenings for AD are performed at
regular visits with a pediatrician. Patients are referred to a specialist if
they display common signs of AD, such as unresponsive or repetitive behavior.
3 The specialist observes the child, performs developmental tests, and
gathers background information from the child's parents or caregivers.
2 Children with AD are usually diagnosed at 2 or 3 years of age.2
Goals of Therapy
As no curative treatment is available for AD, therapy focuses on helping
patients lead more functional lives by alleviating the common triad of
symptoms. Primary goals include improving social interaction, developing
communication skills, and reducing behavioral problems (e.g., aggression,
agitation, hyperactivity, compulsive behavior).3 Other goals
include the treatment of related conditions, such as seizures and bipolar
disorder. Both nonpharmacologic and pharmacologic therapies are used to assist
the patient in reaching these goals.
Treatment Approaches
Treatment of AD must be tailored to
the patient's age and symptoms. Young children (2 to 5 years) with AD
typically display hyperactivity and irritability.12 Usually, this
age-group requires speech therapy, language therapy, and special education.
12 Pharmacotherapy may be used for certain target symptoms.12
Older children (6 to 11 years) commonly display aggression and self-injurious
behavior, while adolescent (12 to 17 years) and adult patients often
experience depression, obsessive-compulsive disorder, and anxiety.1
Patients in these age-groups may require psychotherapy, behavioral or
cognitive therapy, and pharmacotherapy.1
Nonpharmacologic Treatment
Hundreds of nonpharmacologic treatment programs are available for patients
with AD. Nonpharmacologic treatment is the mainstay of any program that aims
to improve an autistic individual's ability to interact with others and
function in daily activities.2 Because nonpharmacologic treatment
programs vary widely in content, they may be grouped into categories according
to their general methods. Popular categories of programs include
neurologic/sensory treatment, psychological treatment, behavioral therapy,
modified diet therapy, and vitamin therapy.2
Neurologic/Sensory Treatment:
Neurologic and sensory treatment targets the complete triad of symptoms and is
perhaps the broadest category.13 A sampling of the most popular and
well-established programs is given below.
Auditory training is thought to improve sensory function. During treatment
sessions, patients listen to high and low frequencies of music. The treatment
goal is to desensitize patients to painful stimuli that would normally trigger
behavioral problems. While this method is safe and reportedly effective, it is
expensive.13 Sensory integration therapy is similar to
auditory training and involves listening to various sounds and touching
various textures. The goal is to help patients cope with sensory stimulation,
thereby improving behavior.13
Daily life therapy, also known as Higashi, originated in Japan.
Daily life therapy emphasizes physical education and the arts. Upon entering
high school, patients participate in community work and complete job training.
The program aims to foster independence in individuals with autism.13
Speech and language therapy teaches autistic patients to communicate
more effectively. The program places more emphasis on improving social
interaction through the use of language and communication techniques than on
teaching rudimentary language skills.3 Music therapy
consists of singing, moving to music, and playing instruments. Music therapy
aims to improve socialization and behavior.13
Psychological Treatment:
Logically, psychological therapy is a major component of any autism treatment
program. Integrating psychological treatment with neurologic treatment allows
the practitioner to treat the disorder from different angles.3 The
following therapies are categorized as psychological treatment.
Holding therapy is a variation of sensory integration therapy. During a
session, the parent and child sit face-to-face for a specified length of time.
The parent is instructed to hold the child, even if he or she resists. The
program aims to help the patient adjust to and overcome sensory overload.
12 Psychoanalysis must be performed by a trained health care
professional. A formal diagnostic evaluation often includes psychoanalysis,
which is helpful in directing therapy and determining the areas that require
the most attention.3 Psychotherapy is also performed by a
trained health care professional. Although the type of therapy and methodology
varies among practitioners, the goal of any psychotherapy program is to help
the patient feel more comfortable with social interaction and become more
self-sufficient in activities of daily life.3
Behavioral Therapy:
Behavioral therapy targets behaviors that prevent the patient from being
independent by employing the scientific principle that children are more
likely to repeat behaviors or responses for which they are rewarded and less
likely to continue behaviors that are not rewarded. Therapists often teach
skills in a very structured manner and provide praise and reinforcement.
Aggressive or self-stimulatory behaviors are reduced or replaced by ignoring
them or by introducing more socially acceptable forms of behavior. The
following programs are examples of behavioral therapies.
TEACHH (Treatment and Education of Autistic and Related Communication
Handicapped Children) is not a teaching program but, rather, a behavior
management system. TEACHH uses structure and modified environments to help
children with autism learn self-care skills.13 The Lovaas Method
, developed by Dr. Ivar Lovaas, is a behavior modification program that
involves intensive one-on-one time with a trainer.13 The Lovaas
Method requires a time commitment of 40 hours per week.13
Occupational therapy helps the patient become more independent through the
development of basic skills, such as buttoning a shirt, bathing, and grooming.
3 Adaptive physical therapy uses exercise and other physical
techniques to help patients improve their coordination and control body
movements.3
Modified Diet Therapy:
Modified diet therapy is one of the more controversial therapies used to
treat children with AD. Although many experts dispute the theory, some
specialists believe that food allergies or digestive problems are the cause of
behavioral problems in many autistic children.4 Because autistic
individuals often cannot communicate effectively, they are unable to express
feelings of discomfort. As a result, these patients may become frustrated and
their behavior may worsen.
Modified diet therapy seeks to improve behavior by eliminating certain foods
that commonly cause food allergies in autistic patients.4
Caregivers whose children follow this program may be instructed to avoid
casein (a milk protein) or gluten (a protein found in wheat, oats, barley, and
rye).4 In more severe cases, caregivers must eliminate both
proteins from the patient's diet.4 It is important to realize
that this program does not eliminate the cause of AD, but it may, however,
help alleviate some behavioral symptoms.
Vitamin Therapy:
Another controversial therapy involves the use of vitamins to improve symptoms
associated with AD. While some experts support the use of vitamins as a
supplemental treatment, others do not recognize this therapy as an effective
way of treating autistic behavior. The regimens discussed in this section are
those that have been studied in controlled trials and appear frequently in
resources directed to caregivers of autistic children.
Although many vitamins are reported to improve a patient's general well-being,
a few vitamins and herbal preparations have demonstrated some benefit in
treating symptoms associated with AD. Vitamin B6 combined with
magnesium is one popular regimen.14 Studies have demonstrated that
vitamin B6 may decrease hyperactivity and improve behavior, as well
as increase attention span.14 Magnesium appears to enhance the
action of vitamin B6.14
Another common regimen is cod liver oil, containing vitamins A and D.4
Some clinicians recommend this regimen because children with food allergies
may have damaged mucosal surfaces, which impairs their ability to absorb
vitamin A palmitate found in infant formula and low-fat milk. Cod liver oil is
rich in vitamin A and is more readily absorbed in these children. Vitamin D
acts as a supplement for children who have allergies to milk proteins and
therefore do not consume milk fortified with vitamin D.4
Vitamin C may help treat depression and behavioral symptoms through a
dopaminergic mechanism of action.15 Of course, vitamin therapy
should only be used in conjunction with other behavioral, psychological, and
sensory therapies and should not be implemented without the full knowledge of
the attending physician.
The Role of the Pharmacist
The pharmacist can help the
caregiver understand that no standard treatment exists for autistic patients.
Because each case of AD is different due to the severity and range of
symptoms, effective treatment programs vary widely from patient to patient.
2 Even the most established treatments work only for a small fraction of
patients. A good specialist will tailor a treatment regimen to fit the
patient's specific needs. Because no cure exists, treatment is aimed at
alleviating lifelong symptoms.2 The pharmacist should also
recognize that many of his or her patients will be using nonstandard therapies
and should become knowledgeable about complementary and alternative medicine.
The pharmacist should remain nonjudgmental and show sensitivity and help
families learn to evaluate scientific evidence and recognize unsubstantiated
treatment claims.11
Coping Strategies and Resources:
Caregivers are under a great deal of stress; they should be advised to take
time for themselves, along with their spouse or other children, to cope with
their situation and avoid feelings of resentment toward the autistic child.
Some states provide funding for respite programs, which provide care for the
autistic patient in emergency and planned support situations. Respite services
can be provided in the patient's home, a caregiver's home, community
locations, a camp, or a respite house.3
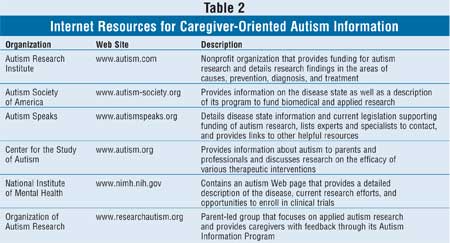
Family counseling and support groups may benefit those who care for autistic
patients. Parents and caregivers may find many helpful resources and support
services on the Internet, and the pharmacist can direct them to useful sites.
Some organizations and support services for caregivers are listed in TABLES
2 and 3.
Funding:
Insurance coverage is a major concern of caregivers of autistic patients, who
may need assistance in obtaining funding for the treatment programs that best
suit their child. Treatment programs are often costly due to the intensity and
time involved and the need for trained specialists. Because AD is not
categorized solely as either a neurologic or psychological disorder, insurance
companies will often deny coverage because the treatment does not fit into a
specific category of covered services.3 The concept is similar to
that of nonformulary medications. For example, the patient's physician may
want the patient to be enrolled in a behavioral therapy program, such as the
Lovaas Method. However, the insurance company may only cover medical and
psychological therapy and may deny payment of behavioral therapy because it is
not recognized as a covered service. As a result, the patient's family cannot
afford treatment and the patient may not receive optimal therapy for his or
her symptoms. In younger patients with AD, timing of treatment is critical,
and waiting for insurance coverage may hinder the child's development.

When caregivers are concerned about
financing treatment, the pharmacist can be a valuable resource in counseling
them on the most effective ways to use their resources. Pharmacists can offer
the following advice to help caregivers strategically utilize their funds and
achieve appropriate care for the autistic child.
When visiting a specialist, caregivers should be advised to request a plan of
action from the diagnostic team to identify the types of programs that will
best suit their child.3 The more informed the caregiver is, the
less likely he or she is to invest time and resources in programs that do not
match the patient's needs. Caregivers who are seeking pharmacologic therapy
for a child with severe symptoms should try to identify the behaviors that
interfere most with the patient's daily functioning, to assist the physician
in choosing optimal therapy.3 Providing the physician with detailed
descriptions of symptoms will help avoid alterations to the patient's
medication regimen.
The pharmacist can direct caregivers to information on alternative funding for
services not covered through private insurance. Organizations such as the
National Autism Association have programs that offer funding to parents of
autistic children. Caregivers of autistic children should also be directed to
their state's Developmental Disabilities Council.3 Each state
has different programs available for individuals with disabilities, and more
states continue to pass legislation to provide funds for the treatment of AD.
Many states will waive a parent's income when determining eligibility for
Medicaid programs.3 Some states also offer family reimbursement
programs to assist caregivers with the cost of respite services, educational
materials, and therapies. Each state's Developmental Disabilities Council can
provide specific information regarding such programs. The caregiver should be
aware that requests for funding are more likely to be granted at the beginning
of the fiscal year, when funds have not yet been expended and/or depleted.
3
Due to the higher incidence of AD and increased news and media coverage, state
and federal governments are responding with efforts to expand funding for AD
research and treatment programs. On December 20, 2006, President George W.
Bush signed into law the Combating Autism Act of 2006. The act
authorizes research under the National Institutes of Health to address the
entire scope of ASD. Furthermore, it authorizes regional Centers of Excellence
for Autism Spectrum Disorder Research and Epidemiology. The act authorizes
activities to increase public awareness of autism, improve the ability of
health care providers to use evidence-based interventions, and increase early
screening for autism. The act calls on the Interagency Autism Coordinating
Committee to enhance information sharing. This committee provides a forum to
facilitate the efficient and effective exchange of information about autism
activities, programs, policies, and research among the federal government,
several nonprofit groups, and the public.16
Conclusion
Autistic patients and their families face great challenges, but hope persists
as public awareness and attention to the disease have increased dramatically
over the past few years. With continued support from caregivers, researchers,
and funding agencies, the mystery of AD may be decoded, allowing patients to
receive more targeted care. Understanding the role of nonpharmacologic therapy
in the treatment of autistic behaviors allows pharmacists and other health
care professionals to provide optimal therapy for autistic patients.
REFERENCES
1. Frith U. Autism: Explaining the Enigma. United Kingdom: Blackwell
Publishing; 2003.
2. Mayo Clinic. Autism. Available at: www.mayoclinic.com/
health/autism/DS00348. Accessed May 31, 2006.
3. Powers MD, ed. Children with Autism: A Parents' Guide.
Bethesda, MD: Woodbine House; 2000.
4. Kidd PM. Autism, an extreme challenge to integrative medicine. Part 2:
medical management. Altern Med Rev. 2002;7:472-499.
5. Chen W, Landau S, Sham P, Fombonne E. No evidence for links between autism,
MMR, and measles virus. Psychol Med. 2004;34:543-553.
6. Brambilla P, Hardan AY, di Nemi SU, et al. The functional neuroanatomy of
autism. Funct Neurol. 2004;20:9-17.
7. Dirckx JH, ed. Stedman's Concise Medical Dictionary for the Health
Professions. Baltimore, MD: Williams & Wilkins; 1997.
8. Beers MH, Berkow R, ed. Autism. In: The Merck Manual of Diagnosis and
Therapy. 17th ed. Whitehouse Station, NJ: Merck & Co.; 1999.
9. Information from your family doctor. What you should know about autism.
Am Fam Physician. 2002;66:1667-1674.
10. Johnson CP, Myers SM, the Council on Children with Disabilities.
Identification and evaluation of children with autism spectrum disorders.
Pediatrics. 2007;120:1183-1215.
11. Myers SM, Johnson CP, the Council on Children with Disabilities.
Management of children with autism spectrum disorders. Pediatrics.
2007;120:1162-1182.
12. Sigman M, Capps L. Children with Autism: A Developmental Perspective.
Cambridge, MA: Harvard University Press; 1997.
13. Ives M, Munro N. Caring for a Child with Autism: A Practical Guide for
Parents. Philadelphia, PA: Jessica Kingsley Publishers; 2002.
14. Nye C, Brice A. Combined vitamin B6-magnesium treatment in autism spectrum
disorder. Cochrane Database Syst Rev.2002:CD003497.
15. Dolske MC, Spollen J, McKay S, et al. A preliminary trial of ascorbic acid
as supplemental therapy for autism. Prog Neuropsychopharmacol Biol
Psychiatry. 1993;17:765-774.
16. S. 843--The Combating Autism Act. Available at: olpa.od.nih.gov/tracking/
109/senate_bills/session1/s-843.asp. Accessed August 28, 2007.
To comment on this article, contact
editor@uspharmacist.com.





