Complex regional pain syndrome (CRPS), previously known as reflex sympathetic dystrophy (RSD), is a syndrome that typically affects one or more extremities but may affect any part of the body.1 A general definition of CRPS includes regional pain that may occur spontaneously without injury involvement or may be triggered by an extremely minor or major injury. This pain can appear out of proportion to the usual course of the known trauma or lesion, if one exists. A definitive pathophysiology is unknown, which makes early diagnosis difficult. In addition, the exact incidence of CRPS is unknown. Early diagnosis is important in preventing the spread of the condition to all extremities and preventing incapacitation. If left untreated, CRPS can result in permanent deformities and chronic pain requiring a range of long-term pharmacologic and nonpharmacologic treatments. If the condition is caught early, physical therapy is a valuable tool to mobilize the affected body part, and sympathetic nerve blocks may be used to stop the progression of disease or cure the disease. In addition to physical therapy and sympathetic nerve blocks, patients may also receive the following therapies: psychotherapy, medications including intrathecal drug pumps, surgical sympathectomy, and spinal cord stimulation.1
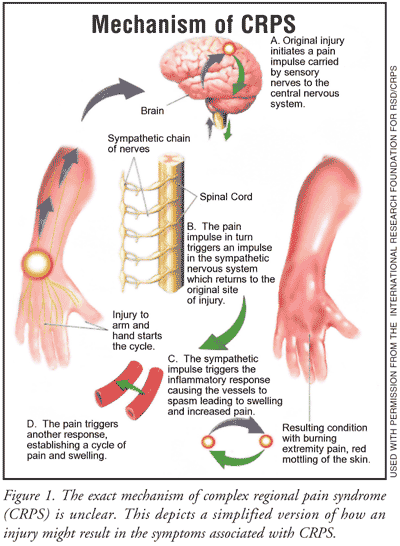
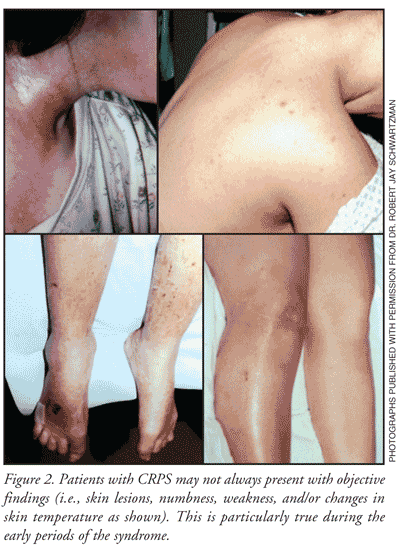
There are two types of CRPS. Type 1 is associated with a history of injury or immobilization without known nerve injury, while type 2 results from known nerve injury.2 Signs of CRPS involve an abnormal function of the sympathetic nervous system such as changes in skin blood flow (color of the skin and temperature changes) or sweating, movement disorders, swelling or edema, changes in tissue growth (either atrophy or dystrophy), hyperalgesia (an exaggerated sense of pain) and/or allodynia (pain occurring as a result of a noninjurious stimulus), and bone changes. FIGURE 1 depicts a possible mechanism for development of CRPS from an injury. Examples of physical presentation are shown in FIGURE 2.1
PHARMACOLOGIC THERAPY
The absence of well-defined criteria for the diagnosis of this syndrome has resulted in a lack of randomized controlled trials (RCTs) for the treatment of CRPS. There are some medications that have shown some efficacy in treating CRPS and others that have been used anecdotally or experimentally. Medications that are commonly used and/or have some clinical data in CRPS are nonsteroidal anti-inflammatory drugs (NSAIDs) such as naproxen or ibuprofen; tramadol; antidepressants such as amitriptyline, doxepin, or trazodone; anticonvulsants (e.g., gabapentin), clonidine, clonazepam, baclofen, topical capsaicin cream, the 5% lidocaine patch, and opioids.1 Additionally, data from neuropathic pain trials and guidelines are often extrapolated, and these medications are used in patients with CRPS even though RCTs are often absent in this patient population.3 Neuropathic pain guidelines include agents such as tricyclic antidepressants, venlafaxine, duloxetine, pregabalin, gabapentin, and the 5% lidocaine patch.3 Currently, there are no drugs that have FDA approval specifically for the treatment of CRPS.
Anti-inflammatory Drugs
Huygen et al hypothesized that inflammation is a key criterion to the development or continued irritation of CRPS.4 Therefore, NSAIDs, cyclooxygenase-2 (COX-2) inhibitors, and corticosteroids have been used to treat type 1 CRPS. Short courses of corticosteroids (total daily dose of 30 mg/day for 12 weeks), followed by a taper, showed improvement versus placebo in patients (n = 23) with early or acute CRPS.5 Longer courses of therapy beyond 12 weeks would not be recommended due to the risk versus benefit of this therapy.
Anticonvulsants
Gabapentin has large RCTs that have proven efficacy in diabetic peripheral neuropathy and postherpetic neuralgia and some case reports (n = 7) showing success in patients with CRPS.6-9 Another anticonvulsant, carbamazepine, showed an improvement in pain versus placebo in a RCT in patients with CRPS (n = 38). The total daily dose was 600 mg/day, given for 8 days.10
Antidepressants
Meta-analysis of RCTs has shown that antidepressants are efficacious in treating neuropathic pain. Some of these medications include amitriptyline, doxepin, nortriptyline, desipramine, imipramine, and trazodone.11 Selective serotonin reuptake inhibitors (SSRIs) are not recommended in recent neuropathic pain guidelines and have shown much less efficacy when compared to the heterocyclic antidepressants. However, the serotonin-norepinephrine reuptake inhibitors (SNRIs) duloxetine and venlafaxine are currently recommended in neuropathic pain guidelines as first-line neuropathic coanalgesics.3
Opioids
One RCT (n = 38) using sustained-release morphine showed no pain reduction when compared to placebo for 8 days of use in patients with CRPS.10 However, there are several studies that show efficacy of opioids in the treatment of neuropathic pain.12 If a provider is using opioids as part of the pain regimen, typically a long-acting opioid is used for maintenance therapy and a short-acting agent for breakthrough pain. It is recommended that the dose of the short-acting opioid be 10% of the total daily dose of the long-acting agent.13 Dworkin et al and other guidelines recommend a reevaluation of all patients on opioids once they have reached a total daily morphine equivalent dose (MED) above 120 mg.3,14 When doses exceed the MED of 120 mg daily, contributing psychological issues or drug-seeking behavior should be ruled out and improvement in function and pain level over previous lower doses should be clearly demonstrated. A fair trial of other therapies should be tried before opioids in this population. Opioids are not the preferred or initial therapy in patients with CRPS.
The American Academy of Pain Management recommends that all patients on long-term opioid therapy engage in a signed agreement to use only one dispensing pharmacy and one physician. This sample patient consent form can be found online (
www.painmed.org/pdf/
N-methyl-d-aspartate (NMDA) Receptor Antagonists
Anesthetic doses of ketamine, an NMDA receptor antagonist, have been used with a gradually increasing (3-5 mg/kg/hour) dose over a 5-day period.16 Midazolam was given concomitantly to counteract the psychiatric side effects, which included agitation, anxiety, and nightmares. This method was used in a patient with severe refractory CRPS that was spreading. Complete remission had been maintained for 8 years according to the case report. Another study by the same author also used anesthetic doses of ketamine.17 An open-label phase II trial of 20 patients with refractory CRPS showed that anesthetic doses (over 5 days) of ketamine provided a benefit in reducing pain, improving quality of life and the ability to work. All 20 patients experienced complete remission within 1 month of treatment, 17 patients maintained complete remission at 3 months, and 16 patients maintained complete remission at 6 months. In those who relapsed, there was still a significant relief in pain at 3 and 6 months.17
Another NMDA receptor antagonist, amantadine 200 mg IV, has been used to treat neuropathic cancer pain (n = 15).18 In this study, pain was significantly reduced versus baseline for 2 days after amantadine administration. Three patients had mild dryness of the mouth during the infusion. Dextromethorphan, at an average oral dose of 400 mg/day, was also studied for the treatment of diabetic neuropathy and postherpetic neuralgia (n = 26).19 All patients in this study reported side effects during treatment with dextromethorphan, which included sedation, dizziness, lightheadedness, ataxia, or confusion. In contrast, during the placebo period, only one patient reported a side effect. Dextromethorphan was not effective in reducing postherpetic neuralgia pain; however, it did show a reduction in pain (P = .014) in patients with diabetic neuropathy. Dextromethorphan should not be administered with tricyclic antidepressants or agents that inhibit CYP2D6, as a drug interaction can result in toxicity.20
Alpha-adrenergic Antagonists and Antihypertensives
Clonidine transdermal patch has shown some benefit in four CRPS patients with sympathetically maintained pain.21 The patch was applied to the hyperalgesic (i.e., exaggeratedly painful) skin, and a substantial reduction in hyperalgesia to mechanical and cold stimuli occurred. It is also suggested that oral terazosin may be effective in treating sympathetically maintained pain in patients with CRPS.22 One patient had complete relief of sympathetically maintained pain and vasospasm on terazosin.
Oral nifedipine (up to 60 mg/day) showed benefit for the control of extreme vasoconstriction in two uncontrolled case series of patients with CRPS (n = 59). Patients received either nifedipine or oral phenoxybenzamine.23,24 Three out of four patients with CRPS responded to phenoxybenzamine 10 mg/day on a daily or every other day basis for a duration of 6 weeks up to 60 months. The one patient who did not respond to a dose of 30 mg/day was found to have a significant psychogenic component that was discovered through psychotherapy.25 Intravenous phentolamine is not typically used clinically; however, it may be used diagnostically.26
Calcitonin
Controlled studies in CRPS have shown value in the use of intranasal calcitonin in doses of 100 to 300 units per day for the management of CRPS.27,28 Calcitonin regulates bone metabolism and has some analgesic effects. One clinical trial in CRPS reported improvement in pain intensity after 100 units of calcitonin three times daily for 3 weeks,27 but another study using 200 units of calcitonin twice daily for 4 weeks showed no improvement in pain.29
Bisphosphonates
The bisphosphonates (e.g., alendronate, clodronate, pamidronate) are another class of drugs that have been studied in CRPS. In two clinical studies, pain improvement was reported in patients with CRPS who had received IV clodronate 300 mg daily for 10 days, as well as IV alendronate 7.5 mg daily for 3 days.30,31 A smaller RCT in CRPS suggested efficacy for oral alendronate (n = 40; 40 mg daily for 8 weeks, which is in contrast to the popular once-weekly regimen), as well as oral and IV pamidronate. It has been suggested that alendronate might relieve pain by decreasing the rate of bone remodeling.32-34
Other Drug Treatment Options
Thalidomide up to 300 to 400 mg daily has shown improvement in pain in case reports of patients (n = 43) with CRPS. The mechanism of this effect is not fully understood.35 IV and subcutaneous lidocaine have also been used.36 Topical treatments that have been used for CRPS include capsaicin, the 5% lidocaine patch, eutectic mixture of local anesthetics (EMLA) cream, and dimethyl sulfoxide (DMSO).3,37 Dworkin et al recommended oral mexiletine as a third-line option for treating neuropathic pain.3 Treatment for dystonia or muscle cramps may include use of oral baclofen or clonazepam.1
CONCLUSION
If left untreated, CRPS can result in permanent deformities and chronic pain requiring a range of long-term pharmacologic and nonpharmacologic treatments. If the condition is caught early, physical therapy is a valuable tool to mobilize the affected body part, and sympathetic nerve blocks may be used to stop the progression of or cure the disease. Other therapies used to treat patients with CRPS are psychotherapy, surgical sympathectomy, spinal cord stimulation, and intrathecal drug pumps. The absence of well-defined criteria for the diagnosis of this syndrome has resulted in a lack of RCTs for the treatment of CRPS.1 In some of the cases, data have only been reported on posters during clinical meetings.38 The medications that have been used or tried in this population include certain antidepressants, anticonvulsants, anesthetics, antihypertensives, anti-inflammatories, opioids, calcitonin, bisphosphonates, and neuropathic coanalgesics, among others. There are no medications that are FDA approved for the treatment of CRPS. To avoid polypharmacy, it is important to remove agents from the regimen that are not resulting in an improvement in pain or function.
REFERENCES
1. Clinical practice guidelines–third edition. International Research Foundation for RSD/CRPS.
www.rsdfoundation.org/en/en_
2. Harden RN, Bruehl S, Stanton-Hicks M, et al. Proposed new diagnostic criteria for complex regional pain syndrome. Pain Med. 2007;8:326-331.
3. Dworkin RH, O’Connor AB, Backonja M, et al. Pharmacologic management of neuropathic pain: evidence-based recommendations. Pain. 2007;132:237-251.
4. Huygen FJ, De Bruijn AG, De Bruin MT, et al. Evidence of local inflammation in complex regional pain syndrome type 1. Mediators Inflamm. 2002;11:47-51.
5. Christensen K, Jensen EM, Noer I. The reflex sympathetic dystrophy syndrome response to treatment with systemic corticosteroids. Acta Chir Scand. 1982;148:653-655.
6. Rowbotham M, Harden N, Stacey B, et al. Gabapentin for the treatment of postherpetic neuralgia: a randomized controlled trial. JAMA. 1998;280:1837-1842.
7. Backonja M, Beydoun A, Edwards KR, et al. Gabapentin for the symptomatic treatment of painful neuropathy in patients with diabetes mellitus. JAMA. 1998;280:1831-1836.
8. Mellick GA, Mellick LB. Reflex sympathetic dystrophy treated with gabapentin. Arch Phys Med Rehabil. 1997;78:98-105.
9. Wheeler DS, Vaux KK, Tam DA. Use of gabapentin in the treatment of childhood reflex sympathetic dystrophy. Pediatr Neurol. 2000;22:220-221.
10. Harke H, Gretenkort P, Ladleif HU, et al. The response of neuropathic pain in complex regional pain syndrome 1 to carbamazepine and sustained-release morphine in patients pretreated with spinal cord stimulation: a double-blinded randomized study. Anesth Analg. 2001;92:488-495.
11. Collins SL, Moore RA, McQuay H, et al. Antidepressants and anticonvulsants for diabetic neuropathy and postherpetic neuralgia: a quantitative systematic review. J Pain Symptom Manage. 2000;20:449-458.
12. Dellemijn PL, van Duijn H, Vanneste JA. Prolonged treatment with transdermal fentanyl in neuropathic pain. J Pain Symptom Manage. 1998;16:220-229.
13. Department of Veterans Affairs Department of Defense. VA/DoD clinical practice guidelines for the management of opioid therapy for chronic pain. May 2003.
http://pain-topics.org/pdf/VA_OpioidsChronicPain_Guide.pdf. Accessed April 1, 2009.
14. Washington State Agency Medical Directors Group. Interagency guideline on opioid dosing for chronic non-cancer pain: an educational pilot to improve care and safety with opioid treatment. March 2007.
www.agencymeddirectors.wa.gov/
15. Goodheart CR, Leavitt SB. Managing opioid-induced constipation in ambulatory-care patients. Pain Treatment Topics. August 2006.
http://pain-topics.org/pdf/Managing_Opioid-Induced_Constipation.pdf. Accessed April 1, 2009.
16. Kiefer RT, Rohr P, Ploppa A, et al. Complete recovery from intractable complex regional pain syndrome, CRPS-type 1, following anesthetic ketamine and midazolam. Pain Pract. 2007;7:147-150.
17. Kiefer RT, Rohr P, Ploppa A, et al. Efficacy of ketamine in anesthetic dosage for the treatment of refractory complex regional pain syndrome: an open-label phase II study. Pain Med. 2008;9:1173-1201.
18. Pud D, Eisenberg E, Spitzer A, et al. The NMDA receptor antagonist amantadine reduces surgical neuropathic pain in cancer patients: a double blind, randomized, placebo controlled trial. Pain. 1998;75:349-354.
19. Nelson KA, Park KM, Robinovitz E, et al. High dose oral dextromethorphan versus placebo in painful diabetic neuropathy and postherpetic neuralgia. Neurology. 1997;48:1212-1218.
20. Forget P, le Polain de Waroux B, Wallemacq P, Gala JL. Life-threatening dextromethorphan intoxication associated with interaction with amitriptyline in a poor CYP2D6 metabolizer: a single case re-exposure study. J Pain Symptom Manage. 2008;36:92-96.
21. Davis KD, Treede RD, Raja SN, et al. Topical application of clonidine relieves hyperalgesia in patients with sympathetically maintained pain. Pain. 1991;47:309-317.
22. Stevens DS, Robins VF, Price HM. Treatment of sympathetically maintained pain with terazosin. Reg Anesth. 1993;18:318-321.
23. Muizelaar JP, Kleyer M, Hertogs IA, DeLange DC. Complex regional pain syndrome (reflex sympathetic dystrophy and causalgia): management with the calcium channel blocker nifedipine and/or the alpha-sympathetic blocker phenoxybenzamine in 59 patients. Clin Neurol Neurosurg. 1997;99:26-30.
24. Prough DS, McLeskey CH, Poehling GG, et al. Efficacy of oral nifedipine in the treatment of reflex sympathetic dystrophy. Anesthesiology. 1985;62:796-799.
25. Inchiosa MA, Kizelshteyn G. Treatment of complex regional pain syndrome type 1 with oral phenoxybenzamine: rationale and case reports. Pain Practice. 2008;8:125-132.
26. Raja SN, Treede RD, Davis KD, et al. Systemic alpha-adrenergic blockage with phentolamine: a diagnostic test for sympathetically maintained pain. Anesthesiol. 1991;74:691-698.
27. Gobelet C, Waldburger M, Meier JL. The effect of adding calcitonin to physical treatment on reflex sympathetic dystrophy. Pain. 1992;48:171-175.
28. Perez R, Kwakkel G, Zuurmond W, et al. Treatment of reflex sympathetic dystrophy (CPRS type I): a research synthesis of 21 randomized clinical trials. J Pain Sympt Manage. 2001;21:511-526.
29. Bickerstaff DR, Kanis JA. The use of nasal calcitonin in the treatment of post-traumatic algodystrophy. Br J Rheum. 1991;30:291-294.
30. Varenna M, Zucchi F, Ghiringhelli D, et al. Intravenous clodronate in the treatment of reflex sympathetic dystrophy syndrome. A randomized, double blind, placebo controlled study. J Rheumatol.
2000;27:1477-1483.
31. Adami S, Fossaluzza V, Gatti D, et al. Bisphosphonate therapy of reflex sympathetic dystrophy syndrome. Ann Rheum Dis. 1997;56:201-204.
32. Manicourt DH, Brasseur JP, Boutsen Y, et al. Role of alendronate in therapy for posttraumatic complex regional pain syndrome type I of the lower extremity. Arthritis Rheum. 2004;50:3690-3697.
33. Robinson JN, Sandom J, Chapman PT. Efficacy of pamidronate in complex regional pain syndrome type I. Pain Med. 2004;5:276-280.
34. Kubalek I, Fain O, Paries J, et al. Treatment of reflex sympathetic dystrophy with pamidronate: 29 cases. Rheumatology (Oxford). 2001;40:1394-1397.
35. Schwartzman RJ, Chevlen E, Bengtson K. Thalidomide has activity in treating complex regional pain syndrome. Arch Intern Med. 2003;163:1487-1488.
36. Mao J, Chen LL. Systemic lidocaine for neuropathic pain relief. Pain. 2000;87:7-17.
37. Attal N, Brasseur L, Chauvin M, et al. Effects of single and repeated applications of a eutectic mixture of local anaesthetics (EMLA) cream on spontaneous and evoked pain in post-herpetic neuralgia. Pain. 1999;81:203-209.
38. Rowbotham MC. Pharmacologic management of complex regional pain syndrome. Clin J Pain. 2006;22:425-429.





