US Pharm. 2017;42(5)15-20.
Pertussis, commonly known as whooping cough, is a severe respiratory infection. It was first identified in the 16th century. In 1906, Bordet isolated the most common causative organism, Bordetella pertussis, an aerobic, gram-negative coccobacillus.1 The disease is a significant cause of morbidity and mortality, especially for children aged <2 years, but may also pose a serious medical illness for preteens, teens, and adults.
In the prevaccination era, pertussis was a leading cause of infant death. As a result of vaccination, the number of cases decreased more than 99% from the 1930s to the 1980s. However, because of outbreaks, the number of cases reported in the United States increased by more than 2,300% between 1976 and 2005.2
The clinical presentation of symptoms in adolescents and adults often differs from classic symptoms observed in infants and children. A persistent cough may be the only symptom in adolescents and adults. Because the symptoms are nonspecific, providers may overlook pertussis as the source of infection in these patients.3 Infected adults are a reservoir of infection that can spread to children, so it is particularly important that all family members and caregivers of young infants be properly vaccinated.4
Epidemiology
Since the early 1980s, the incidence of pertussis has trended upward, with peaks occurring every 2 to 5 years.5 Some reasons for this increase include the fact that the vaccine a young child receives eventually wears off, leaving most teenagers and adults susceptible to the infection during an outbreak; and children are not fully immune until they have received at least three shots in the recommended series, leaving infants aged 6 months at high risk of becoming infected. Protection typically wanes 3 to 5 years after vaccination and is not measurable after 12 years.6-8 Neither acquisition of the disease nor vaccination provides lifelong immunity.
The increase in reported pertussis cases that began in the 1980s spanned all age groups. Although the largest increase in pertussis cases has been among adolescents and adults, the annual reported incidence has been highest among infants aged <1 year.9 The majority of deaths occurred among infants aged <3 months.
In 2012, the second-highest rates of disease, after infants, were observed in children aged 7 through 10 years. Pertussis rates also increased in teens aged 13 and 14 years.10 Age-incidence rates in 2013 and 2014 were similar to those of 2012.10
In a study of pertussis cases in four states, out of 264 infants with the disease, the infant’s mother was the source of pertussis in 32% of cases, and another family member was the source in 43% of cases (P <.0001).11 Although mothers have historically been the most common source of transmission of pertussis to their infant, data from a recent study found that the most common source of transmission to infants was through their siblings.12,13
Risk Factors
Risk factors for contracting the disease include living in the same household with an infected person; being around unimmunized people; and being exposed to those who were immunized when they were much younger, but whose immunity has worn off. Young infants, especially those born prematurely, and patients with underlying cardiac, pulmonary, neuromuscular, or neurologic diseases, are also at risk.12,13
Etiology and Pathophysiology
Pertussis is a highly contagious disease.4 Infected children often wheeze and gasp for breath. In many patients, pertussis is marked by a severe hacking cough and a high-pitched intake of breath that sounds like “whoop.” Pertussis is characterized by a paroxysmal cough lasting more than 2 weeks.3 Transmission can occur through direct face-to-face contact; through sharing a confined space; or through contact with oral, nasal, or respiratory secretions from an infected source.11 When an infected individual coughs or sneezes, tiny microbe-laden droplets are expelled into the air and may be breathed into the lungs by anyone nearby. Inhaled bacterium produce a toxin that severely damages the cilia and respiratory epithelium that coat the lining of the lungs, thereby preventing them from clearing airways of pollen, mucus, and microbial invaders and causing uncontrollable coughing episodes.4
B pertussis multiplies on the respiratory epithelium, beginning in the nasopharynx and ending in the bronchi and bronchioles. A mucopurulent sanguineous exudate forms in the respiratory tract, which compromises small airways (especially those of infants) and predisposes the affected individual to atelectasis, cough, cyanosis, and pneumonia.11 Lung parenchyma and bloodstream are generally not invaded; therefore, blood culture labs are usually negative.
Complications
A number of complications from pertussis are attributed to strenuous coughing.4,9,11,14 These include bruised/fractured ribs; abdominal hernias; cerebral hemorrhages; broken blood vessels in the sclera portion of the eyes; pneumonia; pulmonary hypertension; ear infections; seizures; weight loss; and dehydration. Because infants and toddlers are at greatest risk of complications, they are more likely to need medical treatment in a hospital. In infants aged <6 months, complications are often more severe and can be life threatening. These include pneumonia; slowed respiration rate or stopped breathing; dehydration or weight loss due to feeding difficulties; seizures; and brain damage. With appropriate treatment in the hospital, infants usually recover well; teenage and adult patients often recover without hospitalization and have no major health-related problems.
Signs and Symptoms
Typically, the pertussis incubation period ranges from 3 to 12 days; the disease itself is 6 to 12 weeks in duration, and is divided into catarrhal, paroxysmal, and convalescent stages (Table 1). It generally takes individuals 7 to 10 days postexposure, or longer, for signs and symptoms to appear, but they may not appear for up to 3 weeks after the initial exposure. These symptoms are usually mild at first and resemble a common cold.12,15-17 After a week or two, signs and symptoms may become more intense, and may include accumulation of thick mucus inside airways in the lungs; severe uncontrollable coughing; and prolonged coughing attacks that may provoke vomiting, resulting in red- or blue-tinged facial tissue. Some people don’t develop the characteristic “whoop” or persistent hacking cough. Coughing may be the only sign for some adolescents and adults. Infants may not cough much at all; instead, they may struggle to breathe, or may even temporarily stop breathing.

Diagnosing Pertussis
Diagnosing pertussis in its early stages may be difficult because the signs and symptoms resemble other common respiratory illnesses, such as a cold, the flu, or bronchitis. The standard diagnostic criterion is isolation of B pertussis in cultures of the nose and/or throat.18,19 However, clinical laboratory confirmation is difficult, delayed, and often negative. Therefore, diagnosis is often made based on clinical signs and symptoms common for pertussis, exposure to an infected person, and pertussis vaccination history. Clinical lab tests may be needed to confirm the diagnosis; these may include a nasopharynx culture and sensitivity test and/or a blood specimen to check for elevated white blood cell counts—which typically indicates the presence of infection or inflammation, but is not specific for pertussis.20 A chest x-ray may also be performed to check for the presence of inflammation or fluid in the lungs, which may occur when pneumonia complicates pertussis and other respiratory infections.
Pertussis Management
Whenever possible, it is very important to begin antibiotic treatment during the first 1 to 2 weeks before coughing paroxysms occur, and when, in general, all symptoms may be reduced. Inpatient care is generally preferred for infants, especially those aged <3 months; for premature infants; for children with underlying pulmonary, cardiac, or neuromuscular disease; for other patients with intractable nausea and vomiting, dehydration, failure to thrive, seizures, or encephalopathy; or for patients with sustained hypoxemia during coughing paroxysms and who require oxygen.4,19,21 OTC cough medicines generally have little effect on relieving coughing.
Pertussis is a very dangerous disease, especially for infants, because they are at higher risk of serious complications than adults. Consequently, infants are typically hospitalized, where they may receive appropriate nutrition, intravenous fluids, and antibiotics as needed. If necessary, the infected child may also be isolated from others to prevent the infection from spreading. Antibiotic treatment for older children and adults can usually be managed at home.
Antimicrobial Treatment
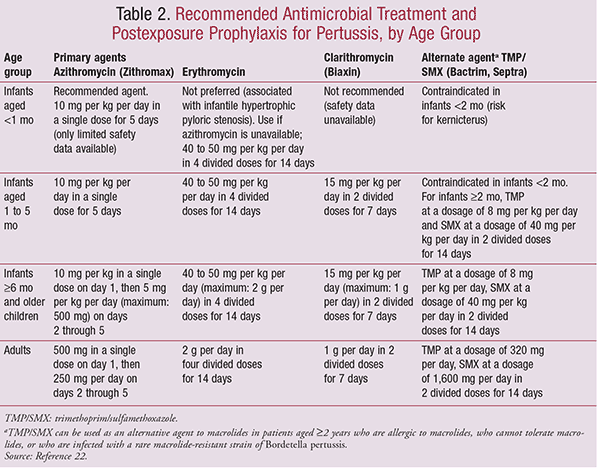
In general, azithromycin is the preferred antibiotic for patients of all ages and is the mainstay of treatment in patients with active infection, together with supportive lifestyle therapy.20,23 The recommended antimicrobial agents for treatment or chemoprophylaxis of pertussis (Table 2) include macrolides (e.g., azithromycin; clarithromycin; and erythromycin). Trimethoprim-sulfamethoxazole can also be used.3,17,22-24 Antimicrobial agents initiated early may reduce symptom severity and disease spread, whereas later administration serves to help reduce the risk of spread and prevent or alleviate secondary infection.
Erythromycin, clarithromycin, and trimethoprim-sulfamethoxazole are strong inhibitors of CYP3A4 and CYP2C9 enzymes, respectively, and they may interact with other medication patients take. Common adverse effects of trimethoprim-sulfamethoxazole include gastrointestinal upset (i.e., nausea, vomiting, and loss of appetite).17,22 For infants aged <1 month, azithromycin is generally well tolerated and is preferred for postexposure prophylaxis and treatment because it has not been associated with causing infantile hypertrophic pyloric stenosis.17,22 Macrolides have been shown to pose a risk of QT prolongation and may need to be avoided in patients with QT prolongation, or a history of torsades de pointes, or who are taking Class 1A or class III antiarrythmics.17,22
In infants aged 1 month, erythromycin, clarithromycin, and azithromycin are preferred for the treatment of pertussis. Trimethoprim-sulfamethoxazole is contraindicated for infants aged <2 months.22 Consider targeting postexposure antibiotic use to persons at high risk of developing severe pertussis. Infants aged >1 year who are within 3 weeks of cough onset and infants aged <1 year should be vaccinated.22,23
Prevention
The best way to prevent pertussis is for infants, children, preteens, teens, and adults to get vaccinated. Herd immunity (or community immunity) can occur when, through a widespread vaccination effort, a sufficient proportion of a population becomes immune to an infectious disease, making its spread from person to person unlikely. Even individuals not vaccinated (such as newborns and those with chronic illnesses) are typically protected because the disease has little opportunity to spread within their community. Because pertussis spreads easily, immunity decreases over time, and pertussis vaccines may not prevent colonization, herd immunity cannot be depended upon to protect everyone from pertussis, so it is wise to be vaccinated.25
Immunity to B pertussis decreases after 5 to 10 years following administration of the vaccine.26 Because of this, older children, adolescents, and adults are at risk of becoming infected with pertussis and need revaccination. It is very important for pregnant women and other people who will have close contact with an infant to be vaccinated against pertussis.21
Pertussis Immunization
Pertussis immunizations are often combined with two other vaccines to protect against the serious diseases of diphtheria and tetanus. The pediatric vaccine formulations usually have three to five times more of the diphtheria component than the adult formulation contains.27 The amount of tetanus toxoid in each of the vaccine products is equivalent and is identified in the vaccine name with an upper-case “T.”27
The CDC recommends diphtheria, tetanus, and acellular pertussis vaccination (DTaP) for children aged <7 years; and either tetanus, diphtheria, and acellular pertussis vaccine (Tdap) or tetanus, diphtheria (Td) vaccine for those aged 7 years, across the lifespan, as specified in Table 3.28

Shortly after completing the recommended vaccinations, the person should be immune to B pertussis.22,28 Vaccine side effects are usually mild and may include fever, fussiness, headache, fatigue or soreness at the site of the injection.17,23 Because immunity tends to decrease over time, booster shots are recommended(Table 4).

Role of the Pharmacist
Pharmacists are the most accessible healthcare providers in the community and provide an extremely valuable service by monitoring patients and their drug regimens for adverse effects and drug-drug interactions; administering vaccines and providing drug information on vaccines, especially pertussis; counseling the patient and/or family on the signs and symptoms of pertussis, as well as the need to be immunized and the time interval for first and follow-up injections; and mild and severe adverse side effects. Pharmacists may also provide patients and parents with basic information regarding pertussis infections and the contagious potential of pertussis, as well as the risks and benefits of the vaccine and medication. If a parent thinks his or her child has whooping cough, pharmacists may assist the family in making an appointment with a doctor or pediatrician. Severe symptoms may warrant a visit to an urgent care center or to a hospital’s emergency department. Other general medical information which can be provided to a physician includes a list of all medications, medication allergies, past medical conditions, and dates and names of previous immunizations.
Conclusion
Pertussis is a highly contagious, acute respiratory tract infection. It is of concern because rates of infection continue to increase. Prevention, correct diagnosis and prompt treatment of pertussis are essential components of infection management. Vaccination is a critical aspect of infection prevention. Herd immunity also contributes greatly to decreased transmission and infection in people of all ages, especially infants.
REFERENCES
1. Bordet J, Gengou O. Le microbe de la coqueluche. Annales de l’Institut Pasteur 1906;20:731-741.
2. Outbreaks of respiratory illness mistakenly attributed to pertussis—New Hampshire, Massachusetts, and Tennessee, 2004-2006. MMWR Morb Mortal Wkly Rep. 2007;56(33):837-842.
3. Cornia PB, Hersh AL, Lipsky BA, et al. Does this coughing adolescent or adult patient have pertussis? JAMA. 2010;304:890-896.
4. Walsh PF, Kimmel L, Feola M, et al. Prevalence of Bordetella pertussis and Bordetella parapertussis in infants presenting to the emergency department with bronchiolitis. J Emerg Med. 2011;40(3):256-261.
5. Cherry JD, Heininger U. Pertussis and other Bordetella infections. In: Feigin RD, Demmler GJ, Cherry JD, Kaplan SL eds. Textbook of Pediatric Infectious Diseases. Vol 1. 5th ed. Philadelphia, PA: WB Saunders; 2004:1588-1608.
6. CDC. Notes from the field: use of tetanus, diphtheria, and pertussis vaccine (Tdap) in an Emergency Department - Arizona, 2009-2010. MMWR Morb Mortal Wkly Rep. 2012;61(3):55-56.
7. Winter K, Harriman K, Zipprich J, et al. California pertussis epidemic, 2010. J Pediatr. 2012;161(6):1091-1096.
8. CDC. Pertussis epidemic - Washington, 2012. MMWR Morb Mortal Wkly Rep. 2012;61:517-522.
9. CDC. Pertussis - United States, 2001-2003. MMWR Morb Mortal Wkly Rep. 2005. 54(50):1283-1286.
10. CDC. Pertussis outbreak trends. Updated September 8, 2015. www.cdc.gov/pertussis/outbreaks/trends.html. Accessed 4/2/2017.
11. Bisgard KM, Pascual FB, Ehresmann, et al. Infant pertussis: who was the source? Pediatr Infect Dis J. 2004;(11):985-989.
12. Skoff TH, Kenyon C, Cocoros N, et al. Sources of infant pertussis infection in the United States. Pediatrics. 2015;136(4):635-641.
13. Skwarecki B. Infants more likely to contract pertussis from siblings. September 10, 2015. www.medscape.com/viewarticle/850781. Accessed April 8, 2017.
14. CDC. Pertussis (Whooping Cough): Outbreaks. Updated September 8, 2015. www.cdc.gov/pertussis/outbreaks.html. Accessed April 8, 2017.
15. CDC. Pertussis (Whooping Cough): Surveillance and reporting. Updated January 10, 2017. www.cdc.gov/pertussis/surv-reporting.html. Accessed April 8, 2017.
16. Atkinson W, Wolfe S, Hamborsky J, et al. Pertussis. In: Atkinson W, Wolfe S,Hamborsky J, et al, eds. Epidemiology and Prevention of Vaccine-Preventable Diseases. 12th ed. Washington, DC: Public Health Foundation; 2012:215-230.
17. Kline JM, Lewis WD, Smith EA, et al. Pertussis: a reemerging infection. Am Fam Physician. 2013;88:507-514.
18. Waknine Y. Infant Pertussis: early white blood cell counts crucial. January 16, 2013. www.medscape.com/viewarticle/777732. Accessed April 26, 2017.
19. Murray E, Nieves D, Bradley J, et al. Characteristics of severe Bordetella pertussis infection among infants older than 90 days of age admitted to pediatric intensive care units – Southern California, September 2009–June 2011. J Ped Infect Dis Soc. 2013;2(1):1-6.
20. Bettiol S, Thompson MJ, Roberts NW, et al. Symptomatic treatment of the cough in whooping cough. Cochrane Database Syst Rev. January 20, 2010. CD003257.
21. Bocka JJ, Steele RW, et al. Pertussis treatment and management, approach considerations. June 7, 2016. http://emedicine.medscape.com/article/967268-treatment. Accessed April 20, 2017.
22. Tiwari T, Murphy TV, Moran J. National Immunization Program, CDC. Recommended antimicrobial agents for the treatment and postexposure prophylaxis of pertussis: 2005 CDC guidelines. MMWR Recomm Rep. 2005;54:1-16.
23. Spector TB, Maziarz EK. Pertussis. Med Clin North Am. 2013;97:537-552.
24. Altunaiji S, Kukuruzovic R, Curtis N, et al. Antibiotics for whooping cough (pertussis). Cochrane Database Syst Rev. 2007;(3):CD004404.
25. U.S. Department of Health and Human Services. Community Immunity (“Herd Immunity”) Vaccines.gov.https://www.vaccines.gov/basics/protection/. Accessed April 5, 2017.
26. Al Dajani N, Scheifele D. How long can we expect pertussis protection to last after the adolescent booster dose of tetanus-diphtheria-pertussis (Tdap) vaccines? Pediatr Child Health. 2007;12(10):873-874.
27. Immunization Action Coalition. Ask the experts: diseases and vaccines. Diphtheria, tetanus, pertussis. www.immunize.org/askexperts/experts_per.asp. Accessed April 21, 2017.
28. CDC. Diphtheria, tetanus, and pertussis recommendations. Updated November 22, 2016.
www.cdc.gov/vaccines/vpd/dtap-td/hcp/recommendations.html. Accessed April 5, 2017.
To comment on this article, contact rdavidson@uspharmacist.com.





