US Pharm. 2018;43(10):HS2-HS6.
ABSTRACT: Hypoglycemia is a condition that occurs when a patient’s blood glucose reaches dangerous levels below 70 mg/dL. Severe hypoglycemia is a medical emergency, and it is important for patients with diabetes and their close contacts—including pharmacists and other healthcare providers—to recognize symptoms of hypoglycemia and proceed with proper treatment. Established guidelines and protocols should be followed based on the severity of the hypoglycemic event. Pharmacists can help reduce a patient’s risk for hypoglycemia, as well as ensure the condition’s proper recognition and treatment, should it occur.
Hypoglycemia is defined as a blood glucose (BG) level ≤70 mg/dL. However, not all patients with a level ≤70 mg/dL have symptoms. Conversely, some patients (especially those with long-standing, poorly controlled diabetes) may experience hypoglycemic symptoms at higher BG levels. Therefore, the term clinical hypoglycemia refers to a plasma glucose concentration that is sufficiently low to cause signs and/or symptoms.1
Classification
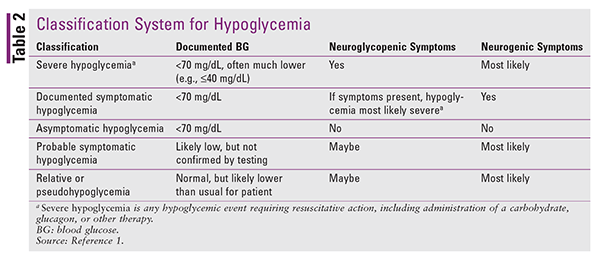
In 2017, hypoglycemia was categorized into three levels of clinical relevance for standardized use in clinical trials (TABLE 1).2 These definitions are being rapidly adopted in clinical practice. Some clinicians may prefer to classify patients with hypoglycemic symptoms according to five categories (TABLE 2), as most recently reaffirmed by a consensus workgroup of the American Diabetes Association and the Endocrine Society in 2013.

Causes
In many cases, hypoglycemia is iatrogenic, often pharmacologically induced upon administration of insulin or other drugs that increase insulin secretion, particularly sulfonylureas and the shorter-acting glinides (meglitinides).3 In fact, antithrombotic and antidiabetic drugs (e.g., warfarin and insulin) have been identified as the two chief causes of adverse drug events resulting in emergency hospitalizations in older adults in the United States.4
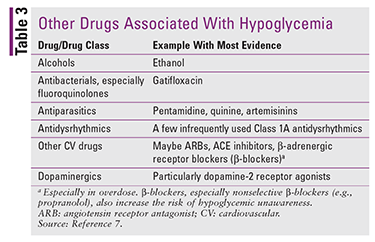
Some drugs, such as salicylates and beta-adrenergic receptor antagonists (beta-blockers), commonly cause hypoglycemia in overdose, but infrequently can cause it with standard dosing. Note also that beta-blockers, particularly nonselective beta-blockers, can cause hypoglycemic unawareness by reducing the adrenergic symptoms of hypoglycemia-like tremor and palpitations. Many other drugs have also been linked to hypoglycemia, but with lower-quality evidence than for insulin-based drugs (TABLE 3).3
Hypoglycemia is a common occurrence in hospitalized patients and is caused by sepsis or another critical illness, nothing-by-mouth (NPO) status, or IV or other parenteral medication (e.g., insulin). Additional comorbidities that increase hypoglycemia risk in diabetes patients (and are possible causes of hypoglycemia in patients without diabetes) include malnourishment and/or alcohol-use disorder, critical illness, septic shock and features of patients in intensive care, cortisol deficiency (with the other key clinical features first), and additional pancreatic disorders (e.g., autoimmune attack, beta-cell tumors, non–islet-cell tumors).5 Alcohol inhibits gluconeogenesis, but not glycogenolysis; during sustained alcohol abuse (over several days to weeks), glycogen can be depleted; these patients may respond poorly to glucagon treatment.6
In conditions other than diabetes, glucose/dextrose supplementation is typically used for initial treatment, but other short-term and long-term treatments are necessary as well. For example, long-term treatment for Addison disease involves physiological glucocorticoid supplementation. Conditions that lead to increased endogenous insulin secretion—e.g., pancreatic tumor—may also result in hypoglycemia. Interim therapy would consist of glucose supplementation and a somatostatin analogue (e.g., octreotide) until a longer-term solution is determined.7
Effect on Achieving Aggressive Glycemic Control
Patients with diabetes experience glucose dysregulation regardless of drug therapy. Patients with a baseline profound endogenous insulin deficiency (e.g., type 1 diabetes and advanced type 2 diabetes) are at greatest risk for hypoglycemia. Insulin-based therapies exert high potential maximal glucose reduction. Given the direct action of insulin to increase cellular uptake and utilization of glucose, drugs that directly increase insulin concentrations as their primary mechanism of action are associated with the highest rates of hypoglycemia.5
Several landmark clinical trials showed that hypoglycemia is the chief limitation to achieving intensive glycemic control (e.g., A1C of 6%) and obtaining improved outcomes in the treatment of diabetes.6 To date, prospective clinical trials examining the benefits and safety of pinpointing lower glycemic targets using only drugs with a low hypoglycemia risk, such as metformin, sodium-glucose cotransporter 2 (SGLT2) inhibitors, and glucagon-like peptide-1 (GLP-1) analogues—some of which have recently demonstrated improved cardiac outcomes—have not been completed.
Guidelines and Glycemic Targets
Hypoglycemia in the treatment of diabetes is addressed throughout the ADA’s guideline, Standards of Medical Care in Diabetes—2018, particularly in three of its chapters: 6, Establishing the Glycemic Target; 11, Older Adults; and 14, Diabetes Care in the Hospital.5
The A1C threshold for prediabetes is ≥5.7% and that for diabetes is ≥6.5%; both of these are risk factors for cardiovascular (CV) disease. The most common A1C goal is <7% for most patients with cognizance to avoid hypoglycemia. However, A1C goals are determined on a patient-by-patient basis (< or >7%); those at higher risk for hypoglycemia and its negative consequences (e.g., long-term-care elderly patients on insulin who have previously experienced hypoglycemia) should have a considerably relaxed A1C goal in order to avoid hypoglycemia. This is because evidence to date has established the break-even point for benefit-versus-risk balance in this range, mostly based on patient-specific risk factors for hypoglycemia and its consequences, including CV events. Several recent clinical trials have demonstrated improved CV outcomes with drugs in certain drug classes that typically carry a low risk of hypoglycemia (SGLT2 inhibitors, GLP-1 analogues); however, these data do not support lower-than-currently-recommended glycemic targets.6
Signs and Symptoms
The signs and symptoms of hypoglycemia are divided into two groups based on physiological mechanisms. Hypoglycemia symptoms include those mediated by autonomic nervous system response, as well as direct neuroglycopenic symptoms.7 Autonomic/neurogenic signs and symptoms include those that are adrenergic (epinephrine)—tremor, palpitations, and anxiety—and cholinergic (acetylcholine)—sweating, hunger, and paresthesias. Neuroglycopenic signs and symptoms include cognitive impairment, behavioral changes, and psychomotor changes ranging up to potential seizure, coma, and, ultimately, death (typically due to cardiac arrest).7
Drugs may interfere with these mechanisms. For example, beta-blockers (e.g., propranolol) mask the adrenergic symptoms that potentially lead to hypoglycemic unawareness. This can increase the severity of hypoglycemia by blocking the compensatory effects of endogenous epinephrine in increasing BG levels and resulting in a delay in exogenous treatment.7
Hypoglycemia is part of the differential diagnosis for any patient found in a semiconscious or unconscious state.7
Reducing Hospital Risk
Most hospitals have well-developed protocols to treat hypoglycemia. Hypoglycemia in hospitalized patients has been associated with increased mortality, which could be due to the more severe nature of illness in patients who tend to become hypoglycemic or could be related to the hypoglycemia itself.6
Primary and secondary prevention strategies should consider and mitigate these factors6:
• Adjusting pharmacotherapy for all patients experiencing a BG level <70 mg/dL during the hospital stay. In one study, 84% of patients with a severe hypoglycemic episode (40 mg/dL) had experienced another episode of a hypoglycemic level <70 mg/dL earlier in the same hospital stay. Most patients were receiving basal insulin and most cases were nocturnal hypoglycemic events.
• Reducing nutrition-insulin mismatch—i.e., carefully timing short-acting hypoglycemic medications in relation to meals; accounting for reduced oral intake, including new NPO status, and for losses (e.g., emesis); accounting for reduced parenteral intake—e.g., reduced infusion rate of IV dextrose or interruptions in parenteral feedings.
• Avoiding or accounting for sudden withdrawal of systemic glucocorticoids.
• Altered patient ability to report hypoglycemia symptoms.
Standardized hospital-wide, nurse-initiated hypoglycemia treatment protocols are preferred. Primary prevention consisting of identifying and mitigating risk factors and triggers for hypoglycemia is also recommended. As discussed earlier, hypoglycemia encountered in the hospital is often iatrogenic, with a large number of cases related to drug therapy.6 In one study, inpatient pharmacist-led, multidisciplinary task forces were successful in reducing hypoglycemic episodes by 80% (P <.01), with reductions of 70% to 100% across all 11 participating hospitals.8 Similar prevention methods have significantly reduced hypoglycemic episodes in other studies as well.9 Results have demonstrated the efficacy of hospital-wide hypoglycemia treatment protocols designed, implemented, and refined by pharmacists, as well as pharmacist-designed, patient-specific primary and secondary prevention strategies and pharmacotherapy plans for hypoglycemia.8
Treatment
It is important to assess the BG level of any patient with hypoglycemic signs and symptoms. However, unavailability of testing equipment should not delay treatment if hypoglycemia is suspected.6
In the conscious patient, the most practical treatment is the oral administration of a rapid-acting carbohydrate (TABLE 4).6,10 The rule of 15 is most commonly applied: Administer approximately 15 g of rapid-acting carbohydrate and perform a repeat check of blood sugar 15 minutes later. If needed, additional 15-g doses of carbohydrate may be administered to resolve symptoms and increase blood sugar above an established threshold (e.g., >70 mg/dL). Hypoglycemic type 2 diabetes patients taking alpha-glucosidase inhibitors who are treated with oral carbohydrates must receive monosaccharides (e.g., glucose); other patients may be given disaccharides (e.g., sucrose) and other simple carbohydrates.11

Glucagon, a counterregulatory pancreatic hormone, causes the breakdown and release of glycogen from the liver to increase BG concentrations. A glucagon kit for emergency treatment of hypoglycemia is recommended for any patient with a history of severe hypoglycemia or who is at risk for it.12 Glucagon kits are reconstituted with the provided solution to a 1 mg/mL clear, particulate-free solution. The entire 1 mg (1 mL) is administered SC or IM (or even IV, in certain settings) in adults and children weighing >20 kg; in children <20 kg (or aged <6 years, if weight is unknown), 0.5 mg is administered. The kit is particularly useful for patients in the community or in long-term care facilities where IV administration of dextrose is not feasible. Close contacts of the patient (e.g., family, friends, neighbors, caregivers) should be educated on the location and appropriate use of the glucagon kit should they find the person in a state of altered consciousness. Other formulations of glucagon (premixed injectable solutions and nasal sprays) are being developed to improve ease of administration in the community setting. Reversal of hypoglycemia relies on sufficient hepatic glycogen stores and other factors. Patients normally respond within 15 minutes; IV glucose must be administered as soon as possible to any patient failing to respond to glucagon.13
IV dextrose is the best treatment for inpatients and for patients found by emergency medical services personnel. IV dextrose is available in different concentrations. Concentrated IV dextrose 50% (D50W) is most appropriate for severe hypoglycemia, providing 25 g of dextrose in a standard 50-mL bag. It is recommended to administer 10 to 25 g (20-50 mL) over 1 to 3 minutes.14 D50W should be administered slowly via peripheral or central sites, and dilution is required when given centrally. Rapid or excessive administration can induce hyperosmolar syndrome, and prolonged use (especially when insulin levels are high) can lead to hypokalemia.15 After D50W treatment, IV dextrose 5% or 10% in water is used to maintain BG levels >100 mg/dL.16
Patients who are given dextrose and sodium chloride solutions are at risk for hypokalemia, fluid overload, and edema.17 Whether glucagon, IV dextrose, or both are used as treatment, it is important to follow up with sufficient oral or IV intake to restore glycogen stores and prevent recurrent hypoglycemia. This can be achieved via IV dextrose infusions or eating, depending on the patient’s status.
Once recovered, regardless of the method used to increase serum glucose (oral, IV, or liver glycogenolysis due to glucagon), the patient should continue to receive supplementation to prevent recurrence and reestablish glycogen stores as necessary. If NPO, parenteral supplementation should continue to prevent hypoglycemia. If conscious and oral intake is possible, the patient should consume foods with longer-acting sources of energy (complex carbohydrates, fats, proteins) in order to prevent recurrence.6
The Pharmacist’s Role
The pharmacist can:
• Contribute to rational drug selection for diabetes and comorbid conditions.
• Increase the patient’s awareness of hypoglycemia and ability to recognize and treat it early.
• Educate patients about timing meals and snacks relative to medication dosing and about which medications to skip when unable to eat on time.
• Develop inpatient protocols and procedures and foster a multidisciplinary approach to prevent and treat hypoglycemia.
• Design and initiate patient-specific primary and secondary prevention and treatment strategies for patients at risk for or experiencing hypoglycemia.
• When treating severe hyperglycemia with IV insulin, help the team recognize the “turnaround” point and when to start adding dextrose to the insulin therapy.
• Recommend alternatives to insulin secretagogues for patients with type 2 diabetes who have experienced—or are at high risk for—hypoglycemia and its negative effects.
• Request a prescription for the glucagon kit in patients at elevated risk of severe hypoglycemia and train the patient and close contacts in recognizing severe hypoglycemia, proper and accessible storage, and use of the kit.
• Optimize insulin therapy in insulin-dependent patients.
• Optimize noninsulin therapy to achieve glycemic goals with low-hypoglycemic-risk medications.
• Suggest relaxed glycemic targets in patients whose risks exceed benefits with aggressive control.
• Direct patients to resources such as diabetes education, dietitians, peer groups, and patient-friendly literature on low blood sugar or low BG, such as the American Diabetes Association’s online article, “Hypoglycemia (Low Blood Glucose).”10
Conclusion
Pharmacists are well positioned to directly prevent, recognize, and treat hypoglycemia, and they can successfully develop institutional protocols and procedures and educate patients, caregivers, and other healthcare practitioners to achieve these goals. Treatment of hypoglycemia depends on the severity and setting, and ranges from self-treatment with oral administration of 15 g of simple carbohydrates to outpatient use of glucagon kits and from oral intake to parenteral dextrose or glucagon administration at an institution. Pharmacist involvement in the care of patients at risk for hypoglycemia and in education on prevention, recognition, and treatment of hypoglycemia for patients and their close family members and associates is critically important in helping reduce complications and improve outcomes.
REFERENCES
1. Seaquist ER, Anderson J, Childs B, Cryer P, et al. Hypoglycemia and diabetes: a report of a workgroup of the American Diabetes Association and the Endocrine Society. J Clin Endocrinol Metab. 2013;98(5):1845-1859.
2. International Hypoglycaemia Study Group. Glucose concentrations of less than 3.0 mmol/L (54 mg/dL) should be reported in clinical trials: a joint position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2017;40(1):155-157.
3. International Hypoglycaemia Study Group. Minimizing hypoglycemia in diabetes. Diabetes Care. 2015;38(8):1583-1591.
4. Budnitz DS, Lovegrove MC, Shehab N, Richards CL. Emergency hospitalizations for adverse drug events in older Americans. N Engl J Med. 2011;365(21):2002-2012.
5. American Diabetes Association. Introduction: Standards of Medical Care in Diabetes—2018. Diabetes Care. 2018;41(suppl 1):S1-S2.
6. Seaquist ER, Miller ME, Bonds DE, et al. The impact of frequent and unrecognized hypoglycemia on mortality in the ACCORD Study. Diabetes Care. 2012;35(2):409-414.
7. Service FJ, Cryer PE, Vella A. Hypoglycemia in adults: clinical manifestations, definition, and causes. UpToDate. Waltham, MA: UpToDate; 2018.
8. Milligan PE, Bocox MC, Pratt E, et al. Multifaceted approach to reducing occurrence of severe hypoglycemia in a large healthcare system. Am J Health Syst Pharm. 2015;72(19):1631-1641.
9. Maynard G, Kulasa K, Ramos P, et al. Impact of a hypoglycemia reduction bundle and a systems approach to inpatient glycemic management. Endocr Pract. 2015;21(4):355-367.
10. American Diabetes Association. Hypoglycemia (low blood glucose). www.diabetes.org/living-with-diabetes/treatment-and-care/blood-glucose-control/hypoglycemia-low-blood.html. Accessed September 12, 2018.
11. Precose (acarbose) package insert. Wayne, NJ: Bayer HealthCare Pharmaceuticals Inc; March 2011.
12. Glucagon: drug information. UpToDate. www.uptodate.com. Accessed June 19, 2018.
13. GlucaGen (glucagon) package insert. Plainsboro, NJ: Novo Nordisk, Inc; July 2018.
14. Diabetes Canada Clinical Practice Guidelines Expert Committee. Diabetes Canada 2018 clinical practice guidelines for the prevention and management of diabetes in Canada. Can J Diabetes. 2018;42(suppl 1):S116.
15. 50% Dextrose Injection package insert. Lake Forest, IL: Hospira, Inc; October 2009.
16. Mahadevan SV, Garmel GM, eds. An Introduction to Clinical Emergency Medicine. 2nd ed. New York, NY: Cambridge University Press; 2012;276.
17. Dextrose Injection package insert. Deerfield, IL: Baxter Healthcare Corp; December 2014.
To comment on this article, contact rdavidson@uspharmacist.com.