US Pharm. 2007;32(6):HS5-HS18.
The term sexuality has many definitions. A simple definition is "the state of being sexual or sexually active."1 A more complex definition, however, comes from a subcommittee appointed by the World Health Organization (WHO) in 2002, who chose the working definition that sexuality is "a central aspect of being human throughout life and encompasses sex, gender, identities, roles, sexual orientation, eroticism, pleasure, intimacy, and reproduction."2 While both definitions are acceptable, we often fail in our society to recognize and acknowledge sexuality in people ages 65 and older. It is a common myth that the elderly have no interest in or are unable to maintain healthy sexual relationships; numerous surveys and studies indicate that both elderly men and elderly women remain sexually active throughout their lives.
If sexual activity is associated with self-reported good to excellent health, then nearly 80% of people between 65 and 74 years of age are sexually active, and 70% of those older than 85 are sexually active.3 While these numbers cannot absolutely correlate, in a study of 1,600 men and women ages 65 to 95, 52% of men and 30% of women reported being sexually active.4 In a survey by the National Council on Aging, the percentage of men and women in their 60s engaged in sexual activity at least once a month was 71% and 51%, respectively, while 50% of men and 58% of women 80 years and older reported being sexually active.5 In a 2004 survey by the American Association of Retired Persons, up to 26% of people over age 60 report having tried medicines, hormones, and other treatments to improve sexual function, giving credence to their sexual interests.6
It is important to note that most research on this topic is tainted by gaps in social scientific research methodologies. For example, study subjects for "the aging population" may include people in their 40s. Another problem when evaluating the literature related to sexual activity in this population is that many researchers define "sexually active" only as "vaginal intercourse." In addition, many subjects included in the research are those with a heterosexual spouse. Despite these limitations, it is universally recognized that this is a subject that warrants more thorough investigation, but more important, it is a subject that needs to be better addressed with all senior patients.
In 1974, the sexologist Dr. Alex Comfort was asked, "Why do old people stop having sex?" He replied, "Old folk stop having sex for the same reason they stop riding a bicycle--general infirmity, thinking it looks ridiculous, or no bicycle."7 This metaphor will be used in this article to explain age-related changes that can impact sexual response and the many barriers to sexual expression that may exist in the elderly. Medications known to cause sexual dysfunction and opportunities for the pharmacist in counseling these patients will also be discussed.
"General Infirmity"
Aging is marked by many physiologic and psychological changes that can impact
a person's capacity and desire for sexual activity. In 1966, Masters and
Johnson defined the human sexual response cycle; these phases are excitement,
plateau, orgasm, and resolution.4 As we age, biological changes can
disrupt or inhibit any of these phases, leading to sexual dysfunction.
The excitement or desire phase requires functioning neurotransmitters, androgens, and an intact sensory system.4,8 Sexual desire is linked to levels of androgen, testosterone, and dehydroepiandrosterone (DHEA). DHEA, the precursor of androstenedione, testosterone, and estrogen, begins to decline in the third decade, and levels are quite low by age 60. Men in their 50s begin to experience a decline in their serum testosterone, and the decline continues steadily as men age. Bioavailable testosterone has been linked to the frequency of sexual thoughts and degree of sexual desire.4 Although controversial, the decline in a woman's estrogen level has been associated with diminished sexual desire. The decline in estrogen can affect the comfort of sexual intercourse; one third of postmenopausal women experience dyspareunia--painful intercourse caused by poor vaginal lubrication. Personal lubricants (e.g., KY Liquid) can be used to diminish pain due to vaginal dryness. The excitement phase is also influenced by environmental, psychosocial, and cultural processes (discussed later in this article).
The plateau or arousal phase requires an intact parasympathetic nervous system and vascular system and is the phase most affected by aging.4,8,9 Lower testosterone levels may result in a longer time period required to achieve an erection; additionally, the erection may be less durable. Impotence, the inability to have and keep an erection sufficient for sexual intercourse, is reported in 15% to 25% of elderly men.4,6 Androgen deficiency can lessen genital and breast sensitivity.10 Lower estrogen levels contribute to urogenital atrophy and an increase in vaginal pH, which can increase the risk of vaginitis and cause thinning of the vaginal tissue. Diminution of vaginal lubrication could reduce sexual response. The arousal phase is also aided by memory and the five senses--visual stimuli, smell, taste, sound, and touch. Alterations in any one of these as a result of advancing age (e.g., dementia or severe macular degeneration) can negatively affect the sexual response cycle.4
For both elderly men and elderly women, the ability to achieve an orgasm remains intact; however, compared to those of their youth, the orgasm may be shorter and less intense. Both genders may require longer duration of direct physical stimulation to achieve an orgasm. In women, significant decreases in clitoral perfusion and size are contributory causes. While older women maintain the capacity for multiple orgasms, a diminished peak of orgasm may result. Orgasms in older men may present with decreased ejaculatory force and volume, absence of ejaculate, and/or retrograde ejaculation.4
The resolution to prearousal state, the final phase of the human sexual response cycle, occurs more rapidly in elderly men and women than during their youth. Following an orgasm, it may take 12 to 24 hours before an elderly man can achieve another orgasm, and this time period can increase as he gets older. 9 The refractory phase in women does not generally change with age. 4,9
In addition to the physiologic changes in sexual function with aging men and women, many chronic medical conditions can negatively affect sexual function as well. Comorbid factors are thought to have a major role in the presence of sexual dysfunction in the elderly. Moreover, some researchers speculate that these elements are primary causative factors of sexual dysfunction.9,11 Conditions causing pain, weakness, or cognitive impairment can certainly diminish sexual desire.4,10 Psychological conditions, such as anxiety and depression, may also lead to problems with sexual expression. Musculoskeletal disorders, such as arthritis and Parkinson's disease, can cause pain and discomfort and may also result in muscle weakness. For these patients, a change in sexual position may be required to lessen joint pain, or the timing of the sexual encounter may need to be planned for when pain or dyskinesia is minimal. Patients with chronic pain syndromes can also have diminished sexual desire.
Vascular disease, atherosclerosis, and hypertension are common causes of erectile dysfunction (ED). Diabetes has also been shown to cause sexual dysfunction. In nonelderly diabetic patients, the incidence of sexual dysfunction is reported between 20% and 27%.12 Diabetes, often a chronic condition in the elderly, is associated with vascular changes and painful neuropathy; it has also been linked to decreased vaginal secretions. 4,13,14 Renal insufficiency, retinopathy, and blindness secondary to diabetes may also adversely affect sexual response.
Angina may be precipitated in an individual who becomes overexerted, thereby instilling fear of participating in sexual intercourse. Additionally, patients with a recent myocardial infarction (MI) or stroke may be fearful that intense sexual activity could precipitate another event. These patients should be counseled that sexual exertion rarely causes a heart attack or stroke, especially when sufficient time for recovery is allowed, and patients should discuss resuming sexual activity with their physician. ED is commonly reported by men following hospitalization for MI.4
Chronic obstructive pulmonary disease (COPD) can negatively impact sexual behavior due to increasing shortness of breath in patients, who often have poor stamina. The use of inhalers prior to sexual intercourse may benefit some patients with COPD. Careful selection of sexual positions may also help patients who quickly become short of breath.14 Some patients may feel less attractive using supplemental oxygen, but it may help patients who develop hypoxemia.13
Genitourinary conditions such as prostate cancer and its many treatments can lead to impotence and sexual dysfunction. Prostatitis can cause decreased sexual desire and pain following ejaculation.13 Stress incontinence can lead to apprehension in engaging in sexual activity for fear of leakage. Patients requiring self-catheterizations may feel less sexual and fear rejection from their partner.
Psychogenic factors such as anxiety and depression are strongly linked to sexual impairment and can be exacerbated by daily stressors such as career, finances, and fatigue. When this occurs, it becomes difficult to ascertain which came first, as problems with sexual expression may lead to an increase in psychological issues. Cognitive behavioral therapy may alleviate anxiety-induced sexual dysfunction.15 Successful treatment of depression may resolve sexual impairment, provided the antidepressant medication does not exacerbate the condition.
Patients with Alzheimer's disease (AD) often exhibit changes in their sexual behavior.16 Some patients with AD may lose their sexual desire altogether, while others may lose inhibition and act inappropriately or become physically aggressive at inappropriate times. Public disrobing and/or masturbation may become problematic, and caregivers should be instructed not to ridicule or embarrass the patient. It is important to inform family members that this behavior is due to symptoms of the dementia and is not related to someone's character. It also warrants mentioning that spouses or partners of those diagnosed with AD may avoid sexual intimacy as a result of emotional disconnection.
Surgery can present as another barrier to sexual expression.4 Whether it is related to the type of surgery or to postsurgical pain or scarring, a person's ability and desire to engage in sexual activity following surgery may decline. While neither a hysterectomy nor a mastectomy has been shown to negatively impact a woman's biological sexual response, these surgeries can cause a psychological barrier. A woman may view herself as "less feminine" or "less desirable" to her partner, thereby diminishing her interest in a sexual relationship.8,14
Alcohol and tobacco consumption can also impair sexual performance.8 Alcohol use may be overlooked in a senior patient as a primary cause of sexual dysfunction because of societal stereotypes. While small amounts may improve libido and sexual drive, large and/or chronic use of alcohol can reduce potency and delay or diminish orgasm.17 Alcohol use should always be addressed in elderly patients, as it can also contribute to increased morbidity and mortality.
In addition to biological, physical, and psychological barriers associated with diminished sexuality in the elderly, medications are also a plausible source, with a reported 25% incidence in the general population.17 Forty percent of all prescription medications and one third of all OTC drugs are consumed by the elderly.18 Although sexual side effects are often overlooked and rarely reported in this population, these side effects should be evaluated and addressed before treatment is initiated and at follow-up. The most commonly cited medication-induced sexual adverse effects are decreased libido, erectile and ejaculatory dysfunction, and diminished orgasm. Table 1 summarizes some of the commonly used medications in the elderly that are associated with effects upon sexual response. Most data related to this topic have focused on men, since sexual problems are easier to quantify given men's external genitalia and the treatments available for ED.19 However, female sexual response is being more widely reported, and treatments for sexual dysfunction in women are being more extensively studied.10,20
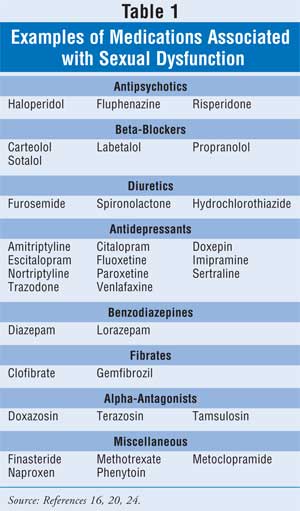
Medications affecting the central nervous system, altering blood flow, or causing dry mucous membranes may disrupt normal sexual function. Benzodiazepines, antipsychotics, and antidepressants, for example, have been shown to decrease libido in both men and women by limiting the ability to process sexual stimulatory signals.21-24 Sexual dysfunction is reported in 66% to 100% of women taking antipsychotic drugs (e.g., haloperidol, risperidone).17 Antipsychotics are known to cause hyperprolactinemia, which can decrease serum testosterone concentrations, altering libido and resulting in impotence.25 The anticholinergic effects of these agents have been shown to cause ejaculatory disorders and problems with arousal and orgasm.17
All classes of antidepressants have been associated with drug-induced sexual disorders; however, selective serotonin reuptake inhibitors (SSRIs), the most widely prescribed agents for depression in the elderly, receive the most attention. While the incidence of SSRI-induced sexual dysfunction in the elderly is not known, the overall incidence is reported to be as high as 30% to 65%.24 Reported problems include arousal difficulties, diminished libido, ED, ejaculatory dysfunction, and delayed or absent orgasm. 24 While the exact mechanism behind the sexual disturbances is unknown, it is postulated to be due to prolonged effects of stimulation of 5-HT2 receptors in the spinal cord, dopaminergic effects, anticholinergic effects, prolactin release, and inhibition of nitric oxide synthetase.22,23 Disruption of the regulation of hormone release by the hypothalamic-pituitary axis has also been theorized.17 Strategies to diminish sexual side effects include using the lowest effective dosage, switching medications (e.g., bupropion, mirtazapine), cognitive behavioral therapy, and using concomitant medications to counteract the sexual side effects.24 For elderly patients, however, using medications to treat side effects promotes polypharmacy and is not recommended due to complicating drug regimens and increasing the likelihood of drug interactions and side effects.
Erection is triggered by both parasympathetic and sympathetic neuronal stimulation and is adversely affected by anticholinergic agents, such as tricyclic antidepressants (TCAs) that block this neurotransmitter. TCAs also have peripheral alpha-adrenergic blocking effects, which can cause emission failures and retrograde ejaculation. Examples of TCAs include amitriptyline and nortriptyline. In the elderly, nortriptyline is preferred because, as a secondary amine, it has fewer anticholinergic side effects. Thus, in addition to possibly lowering the risk of ED, it causes less sedation and confusion and less drying of the mucous membranes.
Antihypertensives are well implicated in causing sexual dysfunction in patients of all ages.17,25 Diuretics, including spironolactone and thiazides, reportedly cause impotence, decreased libido, and decreased vaginal lubrication. While the occurrence of diuretic-induced sexual dysfunction is infrequent, it is more commonly reported in patients who are prescribed unusually high doses.17,25 A reduction in testosterone production through inhibition of dihydrotestosterone, vascular smooth muscle vasodilation, and reduction of extracellular fluid volumes are proposed mechanisms.17
The highest incidence of antihypertensive-induced sexual side effects occurs with nonselective beta-adrenergic receptor antagonists (e.g., propranolol, labetolol, sotalol, carteolol), as these have a stronger correlation to ED than cardioselective agents (e.g., atenolol, metoprolol).17 The proposed mechanism involves peripheral vascular vasoconstriction, which decreases corporal filling in the penis. Lipophilic beta-blockers (e.g., propran != olol, pindolol, penbutolol) can penetrate the blood-brain barrier and may cause sedation and depression. Although calcium channel blockers, alpha-blockers, and angiotensin-converting enzyme inhibitors are all noted to cause occasional difficulties with erection, these drugs are associated with fewer problems than the aforementioned agents.25
While the sexual side effects exhibited by all of these agents are not life-threatening, compliance and subsequent achievement of therapeutic benefit could be reduced. Sexual difficulties for both men and women can perpetuate depression, anxiety, and problems with self-esteem and confidence. Elderly patients may not discuss the suspected "personal" side effects of their medications and may not admit to medication noncompliance. When identified, the causative agent should be assessed and discontinued if possible. A decrease in dosage may also prove helpful if the agent cannot be stopped or changed to another drug class.
"Thinking It Looks Ridiculous"
Alex Comfort's second explanation for why seniors stop having sex can be
attributed, in part, to the physical changes that occur with advancing age.
For example, common age-related changes resulting in loss of skin elasticity
and subcutaneous fat and a decline in muscle mass can lead to wrinkles and
sags. Poor dentition or ill-fitting dentures could also translate into lower
self-esteem and feelings of insecurity. Scars from surgery, excess weight, and
problems with ED may also directly influence sexual desire. In one study
examining the prevalence of sexual concerns of elderly women, 50% of
respondents stated that "body image" was a specific sexual concern. It is
important to note that self-perception has a major role in a woman's sexuality.
10
Intimacy, an element of the WHO's working definition of sexuality, is usually thought to involve more of a psychological component to sexual expression than a physical one and is considered a viable part of a healthy sexual relationship among the elderly.6 For patients unable to perform sexual intercourse, touching, hugging, and holding hands can help provide the emotional needs of intimacy. However, for all individucals, fear can impact sexual desire and response, including expressions of intimacy, and this is especially true in the elderly. Contributory causes of fear may include historical factors (e.g., history of abuse, prior sexual experiences), feelings of guilt, and everyday life stressors (e.g., financial problems, family issues). In a new relationship, fear of embarrassment or rejection can affect sexual expression, while boredom can do the same in a long-term relationship.
Another aspect to Dr. Comfort's reasoning may be society's views on aging and sexuality. Cultural norms usually depict sexual expression among people of youth, potentially making older people feel ashamed of their sexual desires. 26 Societal views have typically been different for women than for men. 27 For example, a woman may be considered "indecent" while a man may be viewed as "virile" if interest in sexual activity is shown.28 However, the perception of a "dirty old man" may also be assumed if an expression of sexual interest is made. These stereotypes, combined with the fear of "What will people think," may keep patients from addressing sexual problems with their physician or pharmacist.
Assumptions of a lack of desire for intimacy or sexual contact, as well as the myth that sexual dysfunction in the elderly is a normal part of the aging process, may keep the health care worker from discussing the topic with the patient.15 Society's mindset, however, is slowly changing with the emergence of medications available to treat ED and the transition of the baby boomer generation into the modern aging adult.14 While many people in our current elderly population were raised to believe that sexuality was mainly for procreation and ended after menopause, the introduction of the first oral contraceptive in the 1960s gave women substantial control over their sexuality. The addition of drugs for ED in the late 1990s extended additional choices to patients.29 With direct-to-consumer advertising for ED drugs in print and on television, seniors are more likely than ever before to discuss sexual dysfunction with health care providers or obtain information on the Internet.
"No Bicycle"
Of all the barriers to normal sexual functioning, the lack of a partner is
cited as the most frequently encountered obstacle by the elderly.30
Common reasons for the lack of a partner can be categorized by the three D's:
death, divorce, and displacement.
Women have a longer lifespan than men, and by age 83, women outnumber men 2.3:1. 31 According to the U.S. Census Bureau's 2003 survey, 27% of men ages 65 to 84 and 82% of women in the same age-group were widowed. In survey participants older than 85, 35% of men and 78% of women were widowed. Therefore, the availability of a suitably aged partner can be a hindrance for an elderly woman if she is interested in pursuing a new relationship. Following the death of a spouse, the remaining partner may experience sexual performance difficulties and/or anxiety when the opportunity for sexual intimacy occurs for the first time. This has been termed widower's syndrome , a subconscious feeling of unfaithfulness to the deceased spouse; consequently, a person may avoid intimacy at all levels.29
Divorce was reported by 17% of elderly men and 22% of elderly women in the U.S. Census Bureau's 2003 survey. Despite divorce being common in our society, the psychological consequences of divorce in elderly men and women may mimic widowhood, with consequent depression, sadness, anger, and guilt. The divorced senior often copes with a decline in physical health, concurrent other losses, and the ending of an often long-standing relationship. As a result, feelings of despair, increased anxiety, and decreased self-esteem can also negatively affect sexual behavior.32
As health and independence decline, aging adults often become displaced, turning to family members or nursing facilities for living arrangements. Caregivers may respond negatively to or be unsupportive of the senior's need for intimacy and privacy. The elderly adult may be too embarrassed to discuss such sensitive issues with family members or health care providers. For example, if both parents reside with an adult child, sexual expression may be impeded due to lack of privacy or fear of being heard.
Moving into an assisted living facility or nursing home presents many obstacles to sexual expression. Although the U.S. Department of Health and Human Services' Centers for Medicare and Medicaid Services states that married nursing home residents have the right to share a room together, barriers to privacy and intimacy usually include doors that do not lock and the lack of full-size beds and "Do Not Disturb" signs.28,33 Family members of a nursing home resident may discourage sexual contact with another resident, placing pressure on the facility to uphold the wishes of the family. Another stated right of the nursing home resident is the "right to personal privacy Ö but the facility does not have to provide a private room." 33 Therefore, even while expressions of intimacy or self-pleasuring activities may be suitable alternatives when sexual intercourse is not an option, a private place may not be available. The facility must also grapple with the issue of informed consent. It must be assured that residents who are sexually active are participating voluntarily, have mental competence, and understand the possible risks of losing a partner through transfer, discharge, or death and the emotional effects that may result.28 Assurance of these factors is difficult; consequently, sexual activity is not usually encouraged by most nursing homes.
Role of the Pharmacist
Pharmacists are often the first health care provider seniors approach with
questions and disclosure of medication-related problems; therefore,
pharmacists should familiarize themselves with age-related changes that can
impact sexual response. Never assume that an elderly patient is no longer
sexually active or has no interest in a sexual relationship. Being proactive
and providing patient counseling can enhance the overall health and well-being
of senior patients. Medication profiles should be screened for drugs that can
cause sexual side effects, and pharmacists can serve as an educational
resource for patients and health care professionals. While the subject is
often awkward to approach, for a new prescription the pharmacist could advise,
"Patients taking this medication often have problems with sexual intimacy, so
if this happens to you, please notify me or your physician." For a
prescription refill, perhaps an anecdotal experience from the pharmacist may
be useful: "Patients taking this medication often have problems with sexual
intimacy. Have you experienced anything like that?" In the presence of sexual
side effects, especially with psychoactive and antihypertensive agents,
patients should be instructed not to abruptly stop their medications but to
contact their physician. Consultant pharmacists in long-term care can serve on
committees drafting nursing facility policies and provide resident, staff, and
family education.34 Suggested Web sites of educational resources
for the community and long-term care pharmacist can be found in Table 2.
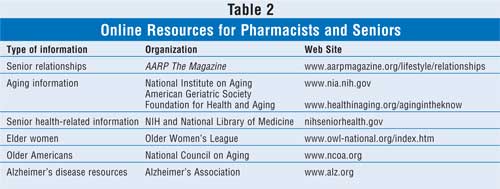
Pharmacotherapy for the treatment of sexual dysfunction in men and women is a trendy topic. While the literature is not specific for senior patients, it is well accepted that nonpharmacologic treatment strategies (e.g., smoking cessation, weight loss measures if necessary, and limiting alcohol consumption) should be given priority over drug therapy. An in-depth discussion about the pharmacologic treatments of sexual dysfunction, including ED, is beyond the scope of this article; however, the pharmacist should be familiar with intracavernosal alprostadil and the phosphodiesterase type-5 inhibitors (e.g., sildenafil, vardenafil, taldalafil), as they have transformed the treatment of ED. Common side effects should be shared with the patients, and the pharmacist should screen for potential drug or concomitant disease interactions.
An important role for the pharmacist is serving as an educational resource. Seniors should be provided with instruction about safe sex practices in an effort to prevent HIV and sexually transmitted diseases (STDs).35 In our society, the elderly have not been targeted as a high-risk group, and many seniors believe they are not at risk for HIV or STDs. The Centers for Disease Control and Prevention reports that nearly one fourth of all HIV cases in the U.S. are those 50 years and older, and by 2015, this number is expected to double.36 Since 2001, the rate of new HIV diagnoses in adults 50 and older has steadily increased.36 Between 1991 and 1996, the rate of AIDS doubled in the same age-group.37 Moreover, the number of HIV-infected elderly is expected to increase as survival improves with advances in treatment of disease. Incidence will also rise with expanding treatment options for sexual dysfunction and the aging of the baby boomer generation.37,38 Most people, including health care providers, do not recognize that seniors are at the same risk for HIV and STDs as other age-groups, and elderly women may be at higher risk. Atrophy of the vaginal mucosa and immunologic vulnerability to infection may increase their risk of contracting HIV and STDs.39
Condoms are not routinely promoted to or used by senior patients because they are past childbearing age and because they are not typically associated with risky sexual behaviors. Lindau et al. studied older women's attitudes, behavior, and communication about sex and HIV; the subjects were ages 58 to 93. 39 Twenty-one percent with a current sexual partner stated that a condom was not necessary due to the inability to become pregnant.39 In addition, many seniors do not know how HIV is transmitted or believe the infection only affects people who are young and/or homosexual. Moreover, physicians do not routinely test for HIV and often misdiagnose initial symptoms as general infirmity in the older population. In the 2005 National Health Interview Survey, only 13% of those ages 65 to 74 and 6% of those older than 75 reported ever being tested for HIV.3 For elderly individuals who remain undiagnosed, it is difficult to separate opportunistic infections and advanced AIDS from conditions that may be seen in uninfected seniors, such as dementia, weight loss, tuberculosis, and pneumonia.38
STDs, such as chlamydia, herpes simplex virus, syphilis, and gonorrhea, can occur in seniors who have unprotected sex and/or in those who engage in sexual activity with multiple partners. Routine screening for syphilis may be warranted since latent syphilis and neurosyphilis commonly manifest in the older population.35
Conclusion
While the incidence of sexual dysfunction is high in elderly patients, it is
not an inevitable occurrence. These patients should be educated about their
aging bodies and the many other precipitating factors that can hinder sexual
function. Lack of knowledge and understanding can become a major barrier to
sexual expression and lead to feelings of inadequacy. Reassurance can also
help eliminate older patients' fears.
Identifying possible drug-induced causes of sexual impairment may help sexual response and eliminate the need for additional medications. Patients should be counseled not to abruptly stop any medication until they have discussed it with their physician. Encouraging senior patients to discuss their concerns with their health care providers and to ask for HIV and STD testing is paramount.
Pharmacists and other health care providers should dispel societal stereotypes and recognize that sexuality in the aging population is perfectly normal and fulfills a basic human need.
References
1. Merriam-Webster Online Dictionary. Available at:
www.m-w.com/dictionary/sexuality. Accessed January 5, 2007.
2. World Health Organization's Progress in Reproductive Health Research
Newsletter 2004; No. 67. Available from:
www.who.int/reproductive-health/gender/sexual_health.html. Accessed January
13, 2007.
3. Centers for Disease Control and Prevention [online]. Vital and Health
Statistics 2006; Series 10, No. 232. Summary Health Statistics for US Adults:
National Health Interview Survey, 2005. Available at:
www.cdc.gov/nchs/data/series/sr_10/sr10_232.pdf. Accessed February 2, 2007.
4. Duthie EH, Katz PR. Practice of Geriatrics
. 3rd ed. Philadelphia, PA: WB Saunders; 1998:48-55.
5. The National Council on Aging [online]. Healthy Sexuality and Vital Aging ñ
Executive Summary; September 1998. Available at:
www.ncoa.org/attachments/SexualitySurveyExecutiveSummary%2Epdf.
6. Jacoby S. AARP Sex in America, 2005. Available at:
www.aarpmagazine.org/lifestyle/relationships/sex_in_america.html. Accessed
December 9, 2006.
7. Comfort A. Sexuality in old age. J Am Geriatr Soc
. 1974;22:440-442.
8. Ginsberg TB. Aging and sexuality. Med Clin N Am
. 2006;90:1025-1036.
9. Sharpe TH. Introduction to sexuality in late life. The Family Journal:
Counseling and Therapy for Couples and Families
. 2004;12(2):199-205.
10. Nusbaum MR, Singh AR, Pyles AA. Sexual healthcare needs of women aged 65
and older. J Am Geriatr Soc
. 2004;52:117-122.
11. Araujo AB, Mohr BA, McKinlay JB. Changes in sexual function in middle-aged
and older men: longitudinal data from the Massachusetts male aging study. J
Am Geriatr Soc
. 2004;52:1502-1509.
12. Enzlin P, Mathieu C, et al. Prevalence and predictors of sexual
dysfunction in patients with Type 1 diabetes. Diabetes Care
. 2003;26:409-414.
13. Beers MH, Berkow M. The Merck Manual of Geriatrics
. 3rd ed. Whitehouse Station: Merck Research Laboratories; 2000:1156-1165.
14. Nusbaum MRH, Hamilton C, Lenahan P. Chronic illness and sexual
functioning. Am Fam Physician
. 2003;67:347-354.
15. Agronin ME. Addressing sexuality and sexual dysfunction. Geriatric
Times.
2001;1. Available at: www.geriatrictimes.com/g010132.html. Accessed December
15, 2006.
16. The Alzheimer's Association Fact Sheet on Sexuality. Available at:
www.alz.org/national/documents/FSsexuality3.pdf. Accessed January 8, 2007.
17. Tisdale JE, Miller DA. Drug-Induced DiseasesñPrevention, Detection, and
Management.
Bethesda, MD: American Society of Health-System Pharmacists; 2005;455-467.
18. American Society of Consultant Pharmacists. Seniors at risk: designing the
system to protect America's most vulnerable citizens from medication-related
problems. Available at:
www.ascp.com/publications/seniorsatrisk/upload/AtRisk.pdf. Accessed February
1, 2007.
19. American Association of Clinical Endocrinologists Medical Guidelines for
Clinical Practice for the Evaluation and Treatment of Male Sexual Dysfunction:
2003 Update. Endocrine Pract
. 2003;9(1):78-91.
20. Basson R. Sexual desire and arousal disorders in women. NEJM
. 2006;354:1497-1506.
21. Clayton AH, Pradko JF, et al. Prevalence of sexual dysfunction among newer
antidepressants. J Clin Psychiatry
. 2002;63:357-366.
22. Rosen RC, Lane RM, Menza M. Effects of SSRIs on sexual function: a
critical review. J Clin Psychopharmacol
. 1999,19(1):67-85.
23. Ferguson JM. The effects of AD on sexual functioning in depressed
patients: a review. J Clin Psychaitry
. 2001;62(suppl 3):22-34.
24. Fava M, Rankin M. Sexual functioning and SSRIs. J Clin Psychiatry
. 2002;63(suppl 5):13-16.
25. Drugs that cause sexual dysfunction: an update. The Medical Letter on
Drugs and Therapeutics
. 1992;34(876):73-78.
26. Carpenter LM, Nathanson CA, Kim YJ. Sex after 40: gender, ageism, and
sexual partnering in midlife. Journal of Aging Studies
. 2005;20:93-106.
27. Levy A, Freyberg Z. Sexual dysfunction and aging: building a bridge
between genders. Clin Geriatr.
2004;12:36-41.
28. Messinger-Rapport BJ, Dandhu SK, Hujer ME. Sex and sexuality: is it over
after 60? Clin Geriatr
. 2003;(11)10:45-53.
29. Wallace M. Sexuality and aging in long term care. Annals of Long-Term
Care
. 2003;11(2):53-59.
30. Duffy L. Lovers, loners, and lifers: sexuality and the older adult.
Geriatrics
. 1998;53:S66-S69.
31. Federal Interagency Forum on Aging Related Statistics. Older Amercians
2000. Available at: www.agingstats.gov/chartbook2000/OlderAmericans2000.pdf.
Accessed December 29, 2006.
32. Lanza M. Divorce experienced as an older woman. Geriatr Nursing
. 1996;17(4):166-170.
33. Code of Federal Regulation ñ 42 CFR 483.10†
34. Kaiser FE. Core concepts: disorders of sexual function. Clin Geriatr
. 2002;10(3):47-60.
35. Calvet HM, Bolan G. STDs in older adults: the need for increased
awareness. Clinical Geriatr.
2000. Available at: clinicalgeriatrics.com/article/1086. Accessed February 3,
2007.
36. Centers for Disease Control and Prevention HIV/AIDs Surveillance Report
2005 [online]. Available at:
www.cdc.gov/hiv/topics/surveillance/resources/reports/2005report/pdf/2005SurveillanceReport.pdf.
Accessed January 15, 2007.
37. National Association on HIV Over Fifty. Educational tipsheet: HIV/AIDs and
Older Adults [online]. Available at: www.hivoverfifty.org/tip.html. Accessed
December 29, 2006.
38. Baldwin J. AIDs may escape diagnosis in older people. Geriatric Times
. 2001. Available at: www.geriatrictimes.com/g010106.html. Accessed February
4, 2007.
39. Lindau ST, Leitsch SA, et al. Older women's attitudes, behavior, and
communication about sex and HIV: a community-based study. J Womens Health
. 2006;15(6):747-753.
To comment on this article, contact editor@uspharmacist.com.





