US Pharm. 2008;33(6):29-36.
In 1991, Mark Beers and an
expert panel developed explicit criteria for potentially inappropriate use of
medications in residents of nursing homes.1 This list of
potentially inappropriate medications (PIMs)--also known as the Beers List or
Beers Criteria--was updated in 1997 and again in 2003.2,3 The 1997
and 2003 versions included more current medications, used updated evidence,
and utilized literature that was generalizable to community-dwelling older
adults. This expert-consensus guideline includes medications for which
evidence of efficacy is scant; for which better alternatives are now
available; and for which dose and disease limitations lead to poor
risk-benefit when used by older adults. This guideline has been both widely
used and criticized. In the absence of evidence, however, expert consensus
remains the standard of care.
The Beers List has two types
of PIM categories. One category includes medications that are potentially
inappropriate independent of disease or condition. The other category
includes medications that are potentially inappropriate based on the
presence of an existing disease or condition in the older patient. For
example, medications with anticholinergic properties would be considered
potentially inappropriate in older adults with chronic constipation because of
their potential to worsen the constipation. Several of these PIMs are
available without a prescription. This article will review some OTC PIMs that
are commonly used by older adults. Specifically, we will concentrate on
diphenhydramine, analgesics, ferrous sulfate, and mineral oil because their
use by older adults is common and poses potentially high risks for adverse
outcomes in this population.4,5
Diphenhydramine
Diphenhydramine is
a first-generation antihistamine. Its two primary uses as an OTC medication
are to treat allergy symptoms and to provide sedation as a sleep aid. As a
treatment for allergies, it is being supplanted by newer second-generation
antihistamines such as fexofenadine, loratadine, and cetirizine. (The last two
are now available OTC.) The absence of anticholinergic and sedative effects
makes the second-generation antihistamines attractive choices for treating
allergy symptoms.6 There is consensus among expert guidelines that
the anticholinergic potential of diphenhydramine outweighs the potential
benefits since equally efficacious alternatives exist.3,7 The
severity rating of this PIM is designated as "high."3
OTC medications are commonly
used to treat insomnia, which is a frequent complaint among older adults. The
issues surrounding diphenhydramine as a short-term sedative have been debated,
and the literature is somewhat conflicting. Few studies have been performed
examining diphenhydramine as a sedative. In younger adults, the primary
benefit of diphenhydramine seems to be to improvement in subjective sleep
complaints, particularly sleep latency.8-10 Richardson et al
reported that the sedative side effects of diphenhydramine subside after four
days; this suggests that the sedative benefit is short-lived and that
tolerance may develop.11 This finding casts doubt on the long-term
efficacy of diphenhydramine as a sedative/hypnotic. None of the studies has
lasted longer than one or two weeks. Thus, diphenhydramine should be strongly
discouraged for chronic use.
Because age-related changes
occur in the cholinergic system, there is concern that strong anticholinergic
effects may lead to a decline in cognitive function or even precipitate
delirium in older adults. Diphenhydramine can have significant cognitive and
performance-related adverse effects even in younger patients.12,13
One study showed no difference in 24-hour pharmacokinetics and
pharmacodynamics between a younger and an older study group; this was a very
small cohort, however.14 Other studies have suggested a significant
elevated risk of adverse outcomes in older adults.15-17 These
studies used doses of 50 mg and greater.15-17 It has not been
documented that lower doses would carry the same efficacy, although side
effects are dose-related. Additionally, Agostini et al included patients with
dementia, which would predispose for cognitive decline and slightly bias the
trial outcome.16 Because alternatives that do not have
anticholinergic effects are available, even the short-term use of
diphenhydramine should be discouraged.
To sum up, the use of
diphenhydramine in older adults should be discouraged both as an antihistamine
and as a sedative because of the potential anticholinergic risks, the lack of
superiority over equally efficacious alternatives (antihistamines), and
better-tolerated and more effective alternatives (sedative/hypnotics). Since
the other OTC options are dietary supplements, the regulatory status of these
agents, the potential for adulteration, and the absence of active ingredients
should be considered. It may be prudent simply to review sleep hygiene and
nonpharmacologic interventions with the patient with ongoing sleep complaints
and refer the patient to his or her primary care physician. A number of
guidelines and reviews exist concerning alternative sedative/hypnotics.
18-21
Nonsteroidal
Anti-Inflammatory Drugs (NSAIDs)
Both chronic and acute pain are
common in older adults. Self-treatment may be appropriate for some; however,
many older adults are likely to be using OTC analgesics chronically. Chronic
use of NSAIDs in older adults has been associated with the development of
renal dysfunction, gastrointestinal (GI) bleeding (GIB), hypertension, and
exacerbation of heart failure.22-24
Age greater than 65 years is a
strong risk factor for GIB. GIB in older adults has been associated with
increased hospitalization and mortality.25 Scheiman reported a
relative risk of 5.6 for GIB for age greater than 70 years.26 There
is consistency across younger populations for a strong association between use
of NSAIDs and increased risk of GIB.26-32 There is consistent
suggestion that ibuprofen has a lower risk of GIB than naproxen does; in fact,
ibuprofen does not appear in the Beers List.28 GIB risk with NSAID
use is dose-dependent, may be highest early in the first week to month, and
persists with use (duration).28,32 For ibuprofen, the cutoff dose
seems to be 1,200 mg/day or 400 mg tid ×
1 week. At or below this dose, the relative risk of GIB in the absence of
other risk factors such as excessive alcohol consumption is low and not
statistically significant; doses greater than 1,200 mg/day, however, carry a
significant risk. Even with lower doses, older adults tend to have a
significant risk of dyspepsia with ibuprofen.33 Careful
history-taking may help detect increased use of antacids and other GI
protectants indicative of this adverse effect.
The level of risk of naproxen
at OTC doses is not clear; some studies show elevated risk and others do not.
25 It would make sense, however, for naproxen to carry an increased
risk, since the risk of GIB is accounted for by cyclooxygenase inhibition and
a higher degree of anti-inflammatory activity. On the other hand, ibuprofen up
to 900 mg/day does not exhibit strong anti-inflammatory activity, but remains
an effective analgesic for mild-to-moderate pain. This lower anti-inflammatory
activity may account for the lower risk seen with ibuprofen. Note that this
dose overlaps the dose that has been associated with increased GIB risk. As a
simple analgesic rather than an anti-inflammatory, the efficacy of ibuprofen
up to 1,200 mg/day is comparable to that of acetaminophen 4,000 mg/day.
34,35
The key to avoiding GIB
associated with NSAIDs is to use the lowest effective NSAID dose for the
shortest period of time. Other strategies may be implemented when NSAIDs are
required for analgesia; for example, use of proton-pump inhibitors may
decrease the risk of GIB.36 (However, since use is likely to be
chronic and risk of GIB in this population would remain high, provider
monitoring would be necessary in this situation.) If a patient presents with a
chronic illness such as diagnosed osteoarthritis, consideration should be
given to a trial of acetaminophen before NSAIDs, according to guidelines.
37,38
Ferrous Sulfate
Ferrous sulfate has
one indication: to prevent or treat iron-deficiency anemia. In this context,
this supplement may be used to restore body iron stores. A typical adult dose
would be 325 mg tid. One small trial has suggested that in older adults a
once-daily dosing strategy was as efficacious as multiple daily dosing; also,
there was less potential to cause constipation.39 While this
finding should be confirmed in a larger clinical trial, it has led to the
Beers List recommendation that doses of ferrous sulfate greater than once
daily may be potentially inappropriate.
Mineral Oil
Simply put, safer
and more efficacious alternatives exist. The sole existing study of mineral
oil's efficacy was very small and had poor methodology.40 The
laxative mechanism of mineral oil has no advantage over other laxatives, and
there is a risk of aspiration and development of lipid pneumonia. More than 20
case reports have been published highlighting this rare but serious
complication that occurs primarily in pediatric and geriatric patients.
Especially if an older adult has swallowing difficulties, mineral oil should
be discouraged as a laxative. Any other laxative would be a better choice in
an older patient.
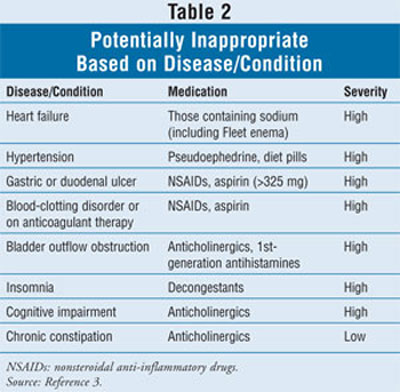
Other PIMs
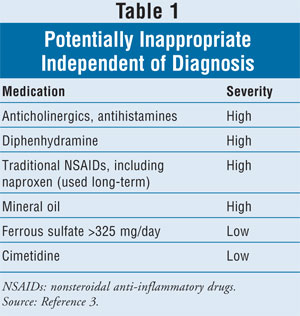
PIMs independent of
diagnosis are listed in TABLE 1; those based on pre-existing diseases
or conditions are given in TABLE 2.3 See Reference 3 for
details concerning the rationale for the potential inappropriateness of
medications not covered in this article. While the Beers List has been
successfully used to prevent potential medication-related problems in older
adults, several things must be kept in mind. First, these medications are
considered potentially inappropriate; the criteria are not rigid. This
means that there may be occasion for appropriate use; this is likely to be the
exception rather than the rule in community-dwelling older adults, however.
Second, one caution with an explicit list of medications is that it has to be
updated regularly. Third, the list does not address medication-related
problems like underuse and potential drug-drug interactions.

A detailed knowledge of these
medications can have a potentially huge influence on the care of
community-dwelling older adults and reduce the occurrence of preventable
medication-related problems. Older adults represent a high proportion of OTC
users. Often, older adults do not discuss these medications with their
physician or pharmacist.41 So, it may be the pharmacist who
initiates the discussion. The FDA has been exploring ways to create a
"pharmacist-only" class of medications, which would increase the demand for
pharmacists with the skills, knowledge, and experience to care for older
adults.42
Conclusion
The use of OTC
medications and PIMs is quite common in older adults. OTC PIMs such as
diphenhydramine, NSAIDs, ferrous sulfate (>325 mg/day), and mineral oil could
potentially lead to significant adverse outcomes in this population.
Pharmacists are in an excellent position to prevent adverse medication-related
outcomes from the use of PIMs, whether prescription or OTC. Thorough knowledge
of the Beers List may be the first step in equipping community pharmacists to
intervene and prevent unnecessary medication-related problems in older adults.
Typically, safer and equally efficacious alternatives exist and should be
given strong consideration prior to the use of these PIMs in older adults.
REFERENCES
1. Beers MH,
Ouslander JG, Rollingher I, et al. Explicit criteria for determining
inappropriate medication use in nursing home residents. UCLA Division of
Geriatric Medicine. Arch Intern Med. 1991;151:1825-1832.
2. Beers MH. Explicit
criteria for determining potentially inappropriate medication use by the
elderly: an update. Arch Intern Med. 1997;157:1531-1536.
3. Fick DM, Cooper JW,
Wade WE, et al. Updating the Beers criteria for potentially inappropriate
medication use in older adults: results of a US consensus panel of experts.
Arch Intern Med. 2003;163:2716-2724.
4. Roumie CL, Griffin
MR. Over-the-counter analgesics in older adults: a call for improved labelling
and consumer education. Drugs Aging. 2004;21:485-498.
5. Hanlon JT,
Fillenbaum GG, Ruby CM, et al. Epidemiology of over-the-counter drug use in
community dwelling elderly: United States perspective. Drugs Aging.
2001;18:123-131.
6. Spangler DL, Brunton
S. Efficacy and central nervous system impairment of newer-generation
prescription antihistamines in seasonal allergic rhinitis. South Med J.
2006;99:593-539.
7. Pugh MJ, Hanlon JT,
Zeber JE, et al. Assessing potentially inappropriate prescribing in the
elderly Veterans Affairs population using the HEDIS 2006 quality measure. J
Manag Care Pharm. 2006;12:537-545.
8. Kudo Y, Kurihara M.
Clinical evaluation of diphenhydramine hydrochloride for the treatment of
insomnia in psychiatric patients: a double-blind study. J Clin Pharmacol.
1990;30:1041-1048.
9. Borbely AA,
Youmbi-Balderer G. Effect of diphenhydramine on subjective sleep parameters
and on motor activity during bedtime. J Clin Pharmacol.
1988;26:392-396.
10. Rickels K, Morris
RJ, Newman H, et al. Diphenhydramine in insomniac family practice patients: a
double-blind study. J Clin Pharmacol. 1983;23:234-242.
11. Richardson GS,
Roehrs TA, Rosenthal L, et al. Tolerance to daytime sedative effects of H1
antihistamines. J Clin Psychopharmacol. 2002;22:511-515.
12. Bender BG, Berning
S, Dudden R, et al. Sedation and performance impairment of diphenhydramine and
second-generation antihistamines: a meta-analysis. J Allergy Clin Immunol.
2003;111:770-776.
13. Kay GG. The effects
of antihistamines on cognition and performance. J Allergy Clin Immunol.
2000;105(suppl):S622-S627.
14. Scavone JM,
Greenblatt DJ, Harmatz JS, et al. Pharmacokinetics and pharmacodynamics of
diphenhydramine 25 mg in young and elderly volunteers. J Clin Pharmacol.
1998;38:603-609.
15. McEvoy LK, Smith
ME, Fordyce M, Gevins A. Characterizing impaired functional alertness from
diphenhydramine in elderly with performance and neuropsychological measures.
Sleep. 2006;29:957-966.
16. Agostini JV,
Leo-Summers LS, Inouye SK. Cognitive and other adverse effects of
diphenhydramine use in hospitalized older patients. Arch Intern Med.
200;161:2091-2097.
17. Sands L, Katz IR,
DiFillippo S, et al. Identification of drug-related cognitive impairment in
older individuals. Challenge studies with diphenhydramine. Am J Geriatr
Psychiatry. 1997;5:156-166.
18. Wolkove N, Elkholy
O, Baltzan M, Palayew M. Sleep and aging: 1. Sleep disorders commonly found in
older people. CMAJ. 2007;176:1299-1304.
19. Wolkove N, Elkholy
O, Baltzan M, Palayew M. Sleep and aging: 2. Management of sleep disorders in
older people. CMAJ. 2007;176:1449-1454.
20. Bain KT. Management
of chronic insomnia in elderly persons. Am J Geriatr Pharmacother.
2006;4:168-192.
21. Morin CM, Hauri PJ,
Espie CA, et al. Nonpharmacologic treatment of chronic insomnia.
An American Academy of Sleep
Medicine review. Sleep. 1999;22:1134-1156.
22. Griffin MR, Yared
A, Ray WA. Non-steroidal antiinflammatory drugs and acute renal failure in
elderly persons. Am J Epidemiol. 2000;151:488-496.
23. Phillips AC,
Polisson RP, Simon LS. NSAIDs and the elderly.
Toxicity and economic
implications. Drugs Aging. 1997;10:119-130.
24. Furey SA, Vargas R,
McMahon FG. Renovascular effects of nonprescription ibuprofen in elderly
hypertensive patients with mild renal impairment. Pharmacotherapy.
1993;13:143-148.
25. Zullo A, Hassan C,
Campo SMA, Morini S. Bleeding peptic ulcer in the elderly: risk factors and
prevention strategies. Drugs Aging. 2007;24:815-828.
26. Scheiman JM. Unmet
needs in non-steroidal anti-inflammatory drug-induced upper gastrointestinal
diseases. Drugs. 2006;suppl 1:15-21.
27. Lewis JD, Kimmel
SE, Localio AR, et al. Risk of serious upper gastrointestinal toxicity with
over-the-counter nonaspirin nonsteroidal anti-inflammatory drugs.
Gastroenterology. 2005;129:1865-1874.
28. Lewis SC, Langman
MJS, Laporte JR, et al. Dose-response relationship between individual
nonaspirin nonsteroidal anti-inflammatory drugs (NANSAIDs) and serious upper
gastrointestinal bleeding: a meta-analysis based on individual patient data.
Br J Clin Pharmacol. 2002;54:320-326.
29. Thomas J, Straus
WL, Bloom BS. Over-the-counter nonsteroidal anti-inflammatory drugs and risk
of gastrointestinal symptoms. Am J Gastroenterol. 2002;97:2215-2219.
30. Kellstein DE,
Waksman JA, Furey SA, et al. The safety profile of nonprescription ibuprofen
in multiple-dose use: a meta-analysis. J Clin Pharmacol.
1999;39:520-532.
31. Kaufman DW, Kelly
JP, Wiholm BE, et al. The risk of acute major upper gastrointestinal bleeding
among users of aspirin and ibuprofen at various levels of alcohol consumption.
Am J Gastroenterol. 1999;94:3189-3196.
32. Griffin MR, Piper
JM, Daugherty MR, et al. Nonsteroidal anti-inflammatory drug use and increased
risk for peptic ulcer disease in elderly persons. Ann Intern Med.
1991;114:257-263.
33. Henry D, Lim LL,
Garcia Rodriguez LA, et al. Variability in risk of gastrointestinal
complications with individual non-steroidal anti-inflammatory drugs: results
of a collaborative meta-analysis. BMJ. 1996;213:1563-1566.
34. Boureau F, Schneid
H, Zeghari N, et al. The IPSO study: ibuprofen, paracetamol study in
osteoarthritis. A randomized comparative clinical study comparing the efficacy
and safety of ibuprofen and paracetamol analgesic treatment of osteoarthritis
of the knee or hip. Ann Rheum Dis. 2004;63:1028-1034.
35. Hyllested M, Jones
S, Pedersen JL, Kehlet H. Comparative effect of paracetamol, NSAIDs or their
combination in postoperative pain management: a qualitative review. Br J
Anaesth. 2002;88:199-214.
36. Targownik LE, Metge
CJ, Leung S, Chateau DG. The relative efficacies of gastroprotective
strategies in chronic users of non-steroidal anti-inflammatory drugs.
Gastroenterology. ePub January 11, 2008.
37. AGS Panel on
Persistent Pain in Older Persons. The management of persistent pain in older
persons. J Am Geriatr Soc. 2002;50 (suppl 6):S205-S224.
38. American College of
Rheumatology Subcommittee on Osteoarthritis Guidelines. Recommendations for
the medical management of osteoarthritis of the hip and knee: 2000 update.
Arthritis Rheum. 2000;43:1905-1915.
39. Rimon E, Kagansky
N, Kagansky M, et al. Are we giving too much iron? Low-dose iron therapy is
effective in octogenarians. Am J Med.2005;118:1142-1147.
40. Mulinos MG,
Maloney AJ. Treatment of constipation in the aged. Effectiveness of mineral
oil and milk of magnesia emulsion. J Med Soc N J. 1969;66:619-622.
41. Sleath B, Rubin RH,
Campbell W, et al. Physician-patient communication about over-the-counter
medications. Soc Sci Med. 2001;53:357-369.
42. Barlas S. FDA
considers new avenue for pharmacist reimbursement: customers must consult with
pharmacists to buy behind-the-counter drugs. Pharm Ther. 2008;33:10.
To comment on this article, contact
rdavidson@jobson.com.





