US Pharm. 2014;39(11):46-49.
ABSTRACT: Patients with diabetes often suffer from foot complications, including ulcers, infections, and even amputations. These complications may begin as xerosis (i.e., drying of the skin). Patients are often prescribed a moisturizer to help maintain the physical-chemical barrier of the skin and to reduce complications related to xerosis. Ammonium lactate–containing moisturizers are commonly prescribed, but evidence supporting their use over other moisturizers is lacking. This suggests that any of the products evaluated in this review may be effective for reducing xerosis. Pharmacists in the community can utilize this information to make individualized and evidence-based recommendations according to cost, ease of administration, and adverse effects.
Patients with diabetes often experience foot complications, such as ulcers, infections, and even amputations.1 More than half of all lower-extremity amputations in the United States are caused by diabetes or diabetes-related complications.2 These complications may begin as xerosis, which is described as reddened, dehydrated skin with scaling that resembles cracked porcelain.3 Many patients are prescribed a moisturizer to help maintain the physical-chemical barrier of the skin, which is expected to reduce complications related to foot xerosis.4
An ideal product would be low in cost, easy to administer, and well-tolerated, but would also show evidence that it prevents complications in patients with diabetes. This review was conducted to determine whether the use of ammonium lactate–containing moisturizers in patients with diabetes prevents complications such as ulcers, infections, and amputations.
Available Products
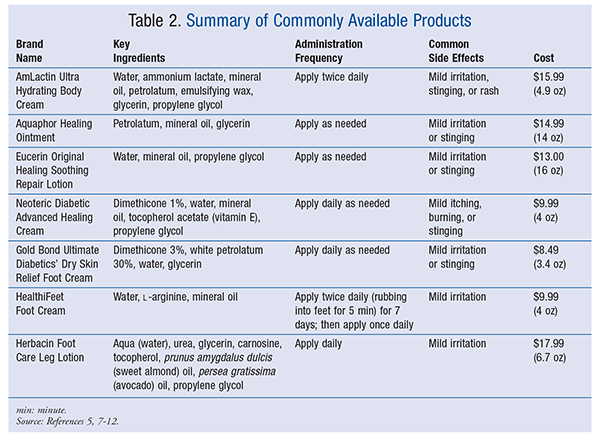
Moisturizers may contain an emollient, which maintains hydration by decreasing evaporation, or a humectant, which increases moisture and skin hydration.3 Ammonium lactate–containing moisturizers—such as AmLactin, which is available OTC—contain water to impart moisture, ammonium lactate as a keratolytic agent, mineral oil and glycerin as moisture barriers, and petrolatum as a skin protectant.5,6 Aquaphor is a healing skin ointment that contains petrolatum as a skin protectant, along with mineral oil and glycerin as moisture barriers.6,7 Eucerin’s ingredients are similar to those in Aquaphor, but it contains glycerin and is a cream base.7,8 Such products may also be used for various skin conditions not specific to diabetes.
Other products are specifically marketed to patients with diabetes. For instance, Neoteric Diabetic Advanced Healing Cream contains water as a moisture barrier, dimethicone as a skin protectant, and vitamin E to promote fast healing.6,9 Gold Bond Ultimate Diabetics’ Dry Skin Relief Foot Cream contains two skin protectants, petrolatum and dimethicone.10 HealthiFeet Foot Cream contains water (moisture barrier) and l-arginine to restore circulation.11 Herbacin Foot Care Leg Lotion is marketed as a more natural product, with its use of carnosine and vitamin E touted as helping improve skin elasticity.12 Herbacin also contains water (moisture barrier) and urea as a keratolytic.12,13 These products contain various other oils and chemicals, but their common goal is to provide moisture, retain moisture, and serve as a protective barrier.
Literature Search
A literature search of the MEDLINE database was conducted via PubMed on August 26, 2013. The initial search attempt included the MeSH terms ammonium lactate, xerosis, and diabetes mellitus combined with the Boolean operator AND, but no results were identified. The term diabetes mellitus was then omitted. The MeSH terms ammonium lactate and xerosis were combined with the Boolean operator AND, and the search was filtered to humans and the English language. Eight articles were retrieved via these parameters. Criteria for inclusion were 1) the measurement of xerosis using a clinician-scored assessment of dryness, 2) the presence of bilateral lower-extremity xerosis at baseline, and 3) a study duration of≥28 days. Application of these criteria excluded one article that evaluated the efficacy of a topical soap in xerosis secondary to atopic dermatitis; the remaining seven articles evaluated the use of ammonium lactate moisturizers in patients with foot xerosis.6,13-18
Study Characteristics
The seven studies chosen for evaluation were randomized, double-blind, bilateral paired comparison trials that examined the effects of two topical products in patients with bilateral foot xerosis. Patients served as their own controls, with the intervention applied to one foot and the comparator to the opposite foot. Five studies explicitly instructed patients to apply each intervention twice daily,13,15-18 whereas the others did not mention a specific dosing frequency.6,14 Xerosis was evaluated using a variety of scales that were either four-point or seven-point scales, with higher scores indicating more dryness. More details about the studies are provided in TABLE 1.
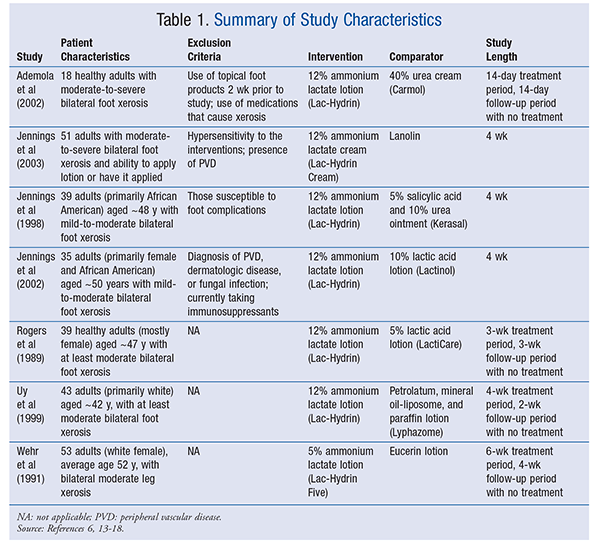
Overall Study Results
An improvement from baseline was observed for both interventions in four studies.13,16-18 Ademola et al found that, from baseline to the end of the follow-up period, both ammonium lactate lotion and urea cream improved xerosis by approximately one point (P <.05).13 Similarly, Wehr et al concluded that both interventions significantly improved xerosis at weeks 6 and 10 compared with baseline (P <.0001).18 Rogers et al reported a statistically significant improvement in dry skin for both interventions from day 3 through the end of the study (P ≤.0001).16 In Uy et al, both treatments showed significant differences in xerotic grade from baseline (P <.001).17
In comparing the improvement in xerosis between each intervention, Ademola et al found a small but statistically significant improvement in the urea group after 14 days of treatment (P <.05); however, this difference did not persist after 14 days of follow-up during which no treatment was administered.13 Rogers et al found a difference between interventions during the treatment period and at the end of the regression period.16 In that study, ammonium lactate lotion resulted in a small, but statistically significant, difference in xerosis scores compared with lactic acid lotion at the end of the 3-week treatment period (0.25; P ≤.05) and at the end of the 3-week follow-up period (0.5; P ≤.05).16 In Wehr et al, a comparison of the two interventions during treatment revealed that ammonium lactate lotion showed a small, but statistically significant, difference in xerosis scores at weeks 6 (0.58; P <.0001) and 10 (0.36; P <.0001) compared with Eucerin lotion.18
Four studies found that, in a head-to-head comparison, neither topical moisturizer was better at improving xerosis.6,14,15,17 There was no statistically significant difference in improvement of xerotic grade, but these studies did not appear to be powered to detect differences in that outcome.
Discussion
A limitation common to all of these studies was the use of a per-protocol analysis. Patients were removed from the analysis if they experienced adverse effects or failed to remain compliant with the treatment regimens. In Ademola et al, noncompliance was defined as missing more than 1 day of moisturizer application.13 Removing these patients may have overestimated product efficacy and tolerability. Lastly, the failure to mention a treatment dosage6,15-18 and the use of different subjective scales made it difficult to interpret true differences in xerosis across studies.
In a comparison of the improvement in each intervention from baseline, four of the studies showed that the use of either ammonium lactate or the comparator product can significantly reduce xerosis.13,16-18 When the interventions were compared, only three studies detected a small—but statistically significant—difference at the end of treatment,13,16,18 with two of the studies favoring ammonium lactate.16,18 However, the xerosis scores differed by only approximately 0.5 points, which makes it difficult to conclude that this difference is clinically important.
Patients with xerosis may experience an improvement with any of the moisturizers evaluated in this review, but it is misleading to state that patients with diabetes-related xerosis will benefit, since patients with diabetes were included in only one study.17 In addition, three studies excluded patients at greatest risk for foot complications,6,14,15 and none of the studies evaluated moisturizers’ effects on minimizing or preventing lower-extremity complications such as ulcers, infections, and amputations.
Conclusion
In this literature search, no randomized, controlled trials examining moisturizers for the prevention of diabetes-related foot complications could be identified. Additionally, the recommendation of ammonium lactate–containing products over other products for the treatment of lower-extremity xerosis in patients without diabetes does not appear to be supported. Although ammonium lactate–containing moisturizers appeared to decrease xerosis in some studies, the absolute differences were not clinically significant. This suggests that the use of any moisturizer described above may be effective for reducing xerosis. Moreover, only one study included patients with diabetes, and these constituted a small proportion of patients recruited.17 Most other studies specifically excluded patients at greatest risk for developing foot complications.
Based on this review, it is recommended that burden of application, cost, and risk of adverse effects be considered in choosing a topical foot product for xerosis in patients with or without diabetes. Details about commonly available products are provided in TABLE 2. In the community setting, it may be appropriate to encourage patients who are reluctant to use an additional topical medication to simply use their regular daily moisturizer, if applicable. However, some patients may be more inclined to regularly use a prescription product, such as ammonium lactate or Lac-Hydrin 12%, since a physician’s prescription often carries a greater sense of credibility. Therefore, before these products can be recommended for the prevention of diabetes-related complications, studies of longer duration that specifically recruit patients with diabetes should be performed. Community pharmacists can use this information, along with patient preferences and characteristics, to direct each patient to an appropriate product that will act as a protective barrier and maintain or impart moisture. Patients with diabetes also should be counseled on the importance of diabetic foot examinations to reduce foot xerosis and the risk of complications.
REFERENCES
1. American Diabetes Association. Standards of medical care in diabetes—2014. Diabetes Care. 2014;37(suppl 1):S14-S80.
2. Amputee Coalition of America. Fact sheet: diabetes and lower extremity amputations. www.amputee-coalition.org/fact_sheets/diabetes_leamp.pdf. Accessed September 4, 2013.
3. Arnold HL Jr, Odom RB, James WD, eds. Andrews’ Diseases of the Skin: Clinical Dermatology. 8th ed. Philadelphia, PA: WB Saunders; 1990:81.
4. American Diabetes Association. Foot care. www.diabetes.org/living-with-diabetes/complications/foot-complications/foot-care.html. Accessed March 19, 2014.
5. AmLactin. AmLactin Ultra Hydrating Body Cream: ingredients. http://amlactin.com/product/amlactin-ultra-hydrating-body-cream. Accessed March 19, 2014.
6. Jennings MB, Logan L, Alfieri DM, et al. A comparative study of lactic acid 10% and ammonium lactate 12% lotion in the treatment of foot xerosis. J Am Podiatr Med Assoc. 2002;92:143-148.
7. EucerinUS. Aquaphor Healing Ointment: ingredients. www.eucerinus.com/products/aquaphor/aquaphor-healing-ointment.html. Accessed March 19, 2014.
8. EucerinUS. Eucerin Original Healing: ingredients. www.eucerinus.com/products/soothe/eucerin-original-healing-soothing-repair-lotion.html. Accessed March 19, 2014.
9. Neoteric Cosmetics, Inc. Neoteric Diabetic Advanced Healing Cream: ingredients. www.neotericcosmetics.com/product-details.aspx?iid=88. Accessed March 19, 2014.
10. Gold Bond Ultimate. Gold Bond Ultimate Diabetics’ Dry Skin Relief skin protectant foot cream. www.goldbondultimate.com/diabetics-foot-cream.html. Accessed March 19, 2014.
11. Tender Corporation. Material safety data sheet. HealthiFeet Cream. www.tendercorp.com/media/import/1186-0035_blob05.pdf. Accessed March 19, 2014.
12. Herbacin. Herbacin Foot Care Leg Lotion: product description. www.herbacin.us/foot-care/herbacin-foot-care-leg-lotion-tube-1-0-fl-oz. Accessed September 3, 2014.
13. Ademola J, Frazier C, Kim SJ, et al. Clinical evaluation of 40% urea and 12% ammonium lactate in the treatment of xerosis. Am J Clin Dermatol. 2002;3:217-222.
14. Jennings MB, Alfieri DM, Parker ER, et al. A double-blind clinical trial comparing the efficacy and safety of pure lanolin versus ammonium lactate 12% cream for the treatment of moderate to severe foot xerosis. Cutis. 2003;71:78-82.
15. Jennings MB, Alfieri D, Ward K, Lesczczynski C. Comparison of salicylic acid and urea versus ammonium lactate for the treatment of foot xerosis. A randomized, double-blind, clinical study. J Am Podiatr Med Assoc. 1998;88:332-336.
16. Rogers RS III, Callen J, Wehr R, Krochmal L. Comparative efficacy of 12% ammonium lactate lotion and 5% lactic acid lotion in the treatment of moderate to severe xerosis. J Am Acad Dermatol. 1989;21:714-716.
7. Uy JJ, Joyce AM, Nelson JP, et al. Ammonium lactate 12% lotion versus a liposome-based moisturizing lotion for plantar xerosis. J Am Podiatr Med Assoc. 1999;89:502-505.
18. Wehr RF, Kantor I, Jones EL, et al. A controlled comparative efficacy study of 5% ammonium lactate lotion versus an emollient control lotion in the treatment of moderate xerosis. J Am Acad Dermatol. 1991;25:849-851.
To comment on this article, contact rdavidson@uspharmacist.com.





