US Pharm. 2022;47(11):5-12.
Epilepsy is a common, chronic neurological condition affecting the brain and nervous system. It is characterized by an enduring predisposition to generate spontaneous epileptic seizures, having many neurological, cognitive, and psychosocial consequences. Epileptic seizures may clinically manifest as loss of awareness, unresponsiveness, uncontrolled movement, or unusual behaviors that often occur without warning. Epilepsy is defined as at least two unprovoked seizures occurring more than 24 hours apart; one unprovoked seizure and a probability of further seizures similar to the general recurrence risk (at least 60%) after two unprovoked seizures; or a diagnosis of an epilepsy syndrome. Simply, epilepsy is a brain disorder characterized by repetitive seizures that lead to excessive and uncontrolled neuronal activity in the brain.1
A seizure occurs with sudden disruption in the electrical activity in the brain. The brain contains millions of neurons that network with other parts of the brain to transmit signals in a fast, timely, and orderly manner. The communication between different parts of the brain occurs through electric currents. These neurons could be excitatory or inhibitory, and a balance in the central nervous system (CNS) is essential for normal brain function. In epilepsy, these clusters of neurons are disrupted and behave irregularly; there is an increase in excitation and a decrease in inhibition, which causes many neurons to fire simultaneously. Neuronal hyperexcitability causes seizures to develop.2
Epilepsy affects over 70 million people of all races, genders, classes, and ages worldwide. Although it affects all age groups, it has a bimodal distribution according to age, with peaks in infants aged younger than 1 year and in adults aged older than 50 years. In the United States, approximately 3 million adults and 470,000 children are affected. In older adults, the incidence increases with increasing age, with the highest incidence seen in those aged older than 70 years. It is a condition that also seems to be more prevalent in low- and middle-income countries; approximately 80% of people with epilepsy live in such geographic areas. This increased incidence may be attributed to greater exposure to perinatal risks, poor hygiene, higher rates of infections, and traumatic brain injuries (TBIs).3-5
RISK FACTORS
Many possible risk factors for epilepsy have been identified, including brain injuries, tumors, CNS infections, and neonatal events, but in most patients the underlying etiology is unknown. In children, epilepsy is usually a result of genetics, perinatal insults, malformations of cortical development, or CNS infections. In adults and the elderly, epilepsy is more commonly due to encephalitis, meningitis, TBI, brain tumors, and neurodegenerative disorders, the most common cause being stroke.3,6-8
TBI is one of the most common causes of acquired epilepsy. There is a 50% risk of developing epilepsy with more serious head trauma. In a population of patients with epilepsy, an estimated 5% of incident cases and approximately 20% of prevalent cases may be due to a previous TBI. Patients who experience penetrating brain injuries have the highest risk of epilepsy development.9,10 Cerebrovascular diseases such as stroke are the most common cause of new-onset epilepsy in the elderly population; up to 50% of cases can be attributed to stroke. The risk of developing epilepsy in the first year after suffering a stroke increases by 20 times.11 Viral, bacterial, fungal, and parasitic infections of the CNS may induce seizures and epilepsy. The risk for developing seizures appears to be related to the pathogen, the degree of cortical involvement, maturation of the brain, the patient’s genetic makeup, and the degree of cytokine-mediated inflammatory response. These CNS infections are the most preventable risk factors for epilepsy.12 Alzheimer’s disease is another risk factor for seizures but is not among the most common causes. The risk is age-dependent, with a higher prevalence in patients with early-onset Alzheimer’s disease.13
CLASSIFICATION OF EPILEPSIES
The classification of the type of epilepsy a patient has is determined by gathering a good medical history and assessing the type of seizures experienced. The International League Against Epilepsy has established a framework for the classification of epilepsies, based on three levels: seizure type, epilepsy type, and epilepsy syndrome (see TABLE 1).14

Seizures are classified based on where the electrical activity starts in the brain: focal, generalized, or unknown. Focal seizures originate in a localized area of the brain, whereas generalized seizures involve the entire cerebral cortex. When the distinction between focal and generalized cannot be made, the seizure is classified as an unknown-onset seizure. After the seizure type has been determined, epilepsy should be classified into one of four categories: focal epilepsy, in which the patient only has focal-onset seizures; generalized epilepsy, in which the patient only has generalized-onset seizures; combined generalized and focal epilepsy; and unknown. After establishing the epilepsy type, epilepsy syndrome should be determined if possible. An epilepsy syndrome refers to a cluster of signs and symptoms, as well as a known etiology, that tends to occur together. Common epilepsy syndromes include childhood absence epilepsy, Dravet syndrome, juvenile myoclonic epilepsy, juvenile absence epilepsy, Lennox-Gastaut syndrome, and West syndrome.14,15
PHARMACOLOGIC MANAGEMENT
For most patients with epilepsy, antiseizure drugs (ASDs) are the mainstay of treatment. The goal of treatment is seizure remission without adverse effects; however, only about 50% of patients taking antiseizure medications have achieved this goal.16
Today, we have an array of medications used in the management of epilepsy (see TABLE 2). In selecting the appropriate antiepileptic agent, it is important to know the seizure type and syndrome. Other important factors to take into consideration include mechanisms of action, adverse effects, potential drug interactions, gender, economic factors, and lifestyle. ASDs should always be initiated as monotherapy, and doses should be slowly titrated upwards to the maximum tolerated dose to minimize the occurrence of adverse events. If the patient experiences no benefit at the maximum tolerated dose, an alternative first-line agent should be initiated. If all first-line agents fail, a second-line option should be added.17
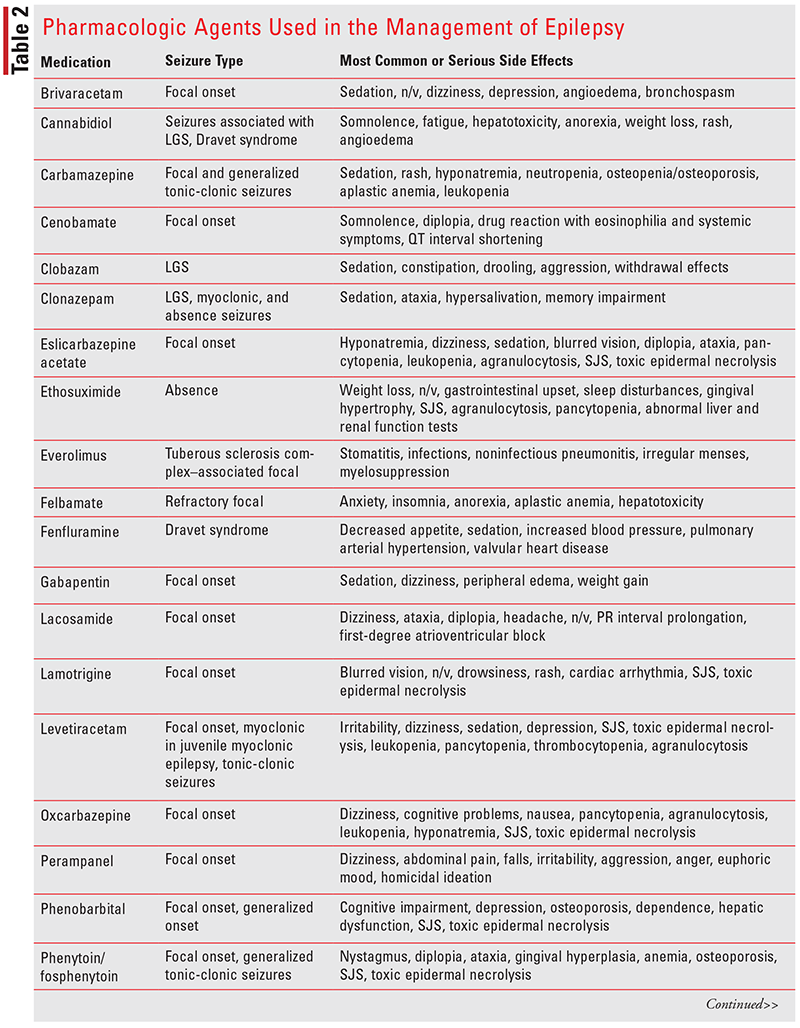
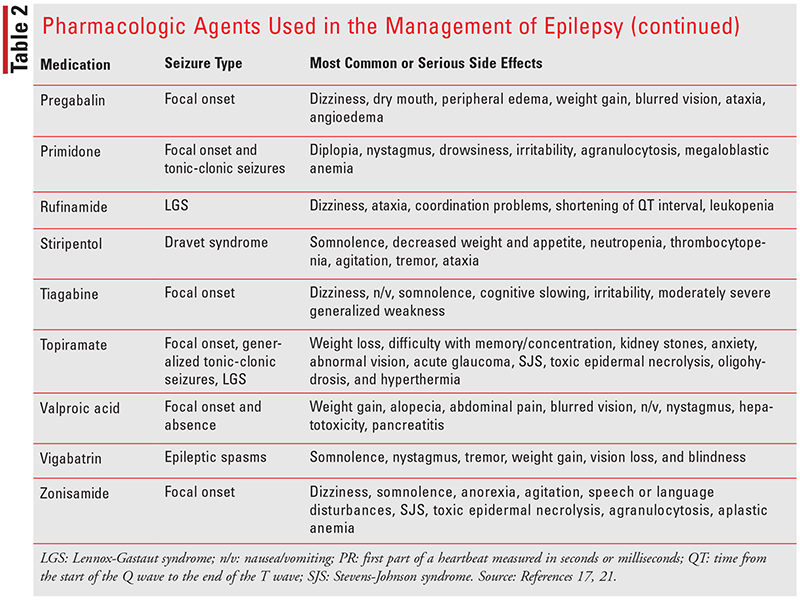
All ASDs are associated with adverse effects. Most commonly, ASDs are associated with neuropsychiatric symptoms, including sedation, fatigue, dizziness, unsteadiness, and irritability. Psychiatric adverse effects include depression, anxiety, irritability, mood changes, impaired concentration, and in some severe cases psychosis. All ASDs have a warning for suicidal thoughts. Patients need to be monitored regularly for depression and mood changes. With chronic use, many of the ASDs, including carbamazepine, phenytoin, phenobarbital, oxcarbazepine, and valproate, can cause osteoporosis. Patients on these medications for 6 months or longer should also take a calcium supplement and vitamin D. Routine monitoring for osteoporosis should occur every 2 years.17,18
The most common idiosyncratic adverse effect is rash, typically occurring during the first 6 to 12 months of therapy. This rash occurs in up to 10% of patients on carbamazepine but is also seen in those treated with phenytoin, oxcarbazepine, phenobarbital, lamotrigine, valproate, and felbamate. These medications should be stopped immediately when the appearance of a rash occurs. Most rashes are self-limiting upon discontinuation, but some can be severe, leading to Stevens-Johnson syndrome and toxic epidermal necrolysis.17,19
In women of childbearing age, it is important to keep in mind the teratogenicity risk associated with all the ASDs. Lamotrigine and levetiracetam have the lowest incidence of congenital malformations, while valproic acid should be avoided in all women of childbearing age because of its high risk for CNS, cardiac, urologic, and facial malformations, as well as developmental problems. Another concern is decreased levels of lamotrigine, oxcarbazepine, levetiracetam, carbamazepine, and phenytoin during pregnancy. These medications are metabolized more rapidly during pregnancy and accordingly require monitoring of blood levels and dose adjustments.17,18
In addition to the adverse effects associated with the use of ASDs, there are various drug interactions that can have potentially serious implications. Several of the older ASDs are known enzyme inducers (i.e., carbamazepine, phenytoin, phenobarbital, and primidone) that increase the clearance of other medications metabolized through these pathways. Others can act as inhibitors (i.e., valproic acid), decreasing the clearance of medications metabolized by the same pathways and increasing the risk for adverse effects due to toxic accumulation. Whenever a change in therapeutic regimens is implemented, it is important to consider appropriate dose reductions in the ASDs to help minimize the occurrence of effects attributable to drug interactions.
ROLE OF THE PHARMACIST
As one of the most accessible healthcare professionals, pharmacists can greatly impact the education of epilepsy patients about their disease and therapy. Pharmacists can monitor therapy adherence and help patients understand that adherence is crucial to staying seizure-free. ASD nonadherence drives up healthcare utilization and direct medical costs, as it is correlated with increased inpatient admissions, length of hospital stays, and emergency department visits. In promoting adherence, pharmacists can minimize these costs and improve the quality of care. Pharmacists can work in collaboration with patients and their prescribers in choosing the appropriate ASD individualized to other patient factors such as comorbidities or lifestyle considerations.
ASDs come with side effects that the pharmacist can provide counseling on so that the patient understands what to expect and when to seek medical attention. All ASDs are known for the risk of suicidal ideation and drowsiness. Some agents, including carbamazepine, lamotrigine, oxcarbazepine, and phenytoin, can lead to a severe rash. Teratogenicity is another factor that pharmacists can communicate to patients and help them consider another agent if needed. Furthermore, pharmacists can screen for drug-drug interactions and the need for any dosage adjustments. Since ASDs require serum drug-concentration monitoring, pharmacists can oversee to optimize therapy. Epilepsy patients are often advised to supplement their diets with calcium and vitamin D, and a pharmacist can guide them in selecting the appropriate OTC products.20
CONCLUSION
Epilepsy is a condition that can negatively impact a patient’s quality of life and become very dangerous. Patient education is crucial so that patients stay adherent to their pharmacotherapeutic regimens, preventing seizure occurrences. Pharmacists can play a role in monitoring therapy, counseling on side effects, and promoting adherence. In these ways pharmacists can lower the overall economic burden that epilepsy poses as well as help patients optimize their therapy.

What Is Epilepsy?
Epilepsy is a neurological disorder that leads to seizures, which are a disruption of electrical activity in the brain. This is not a contagious condition or a mental illness. This disease affects people of all ages. Different types of seizures vary from uncontrolled, jerking movements (known as tonic-clonic seizures) to subtle seizures that lead to moments of loss of awareness (known as absence seizures). Seizures are classified based on where in the brain the seizure starts.
What Are the Symptoms of Epilepsy?
Symptoms vary based on where in the brain this disruption of electrical activity begins and how far it spreads. Temporary symptoms can include loss of consciousness, disturbance in movement or sensation (including visual and hearing disturbances), or disturbance in cognitive function.
What Causes Epilepsy?
Oftentimes, the cause of epilepsy is unknown. Some known causes are major head injury, stroke, brain tumor, genetic conditions, or infection. Motor vehicle accidents, gunshot wounds, and other causes of severe head trauma that can lead to brain damage can trigger seizures. An electroencephalogram is a test used to diagnose epilepsy by recording electrical activity in the brain.
How Is Epilepsy Treated?
Seizures can be controlled with antiepileptic medications that help stabilize the electrical activity in the brain. These medications are known to cause drowsiness, pose a risk for suicidal ideation, and have many drug-drug interactions. Seizures that are resistant to medications may require surgery to be treated. Surgery is an option when the clinician can determine the location within the brain causing the seizure and if the removal of this portion is possible without damage to other vital areas of the brain. Vagal nerve stimulation is another method for seizure control in which a pacemaker is implanted. The pacemaker is connected to the vagus nerve and is programmed to deliver normal, scheduled electrical stimulation to the brain.
First Aid for Seizures
It is important to know how to respond to someone who is actively seizing.1. Make sure to clear the area around the person. Watch out for sharp or hard objects to prevent injury.
2. Ease the individual onto the floor. It is a good idea to place something soft but fat under the head and turn the individual gently onto one side to help keep the airway clear.
3. Remove any eyeglasses. Loosen ties or anything else around their neck to make sure there are no barriers to breathing.
4. Time the seizure. If it occurs for longer than 5 minutes, and/or if the person is having trouble breathing, call 911.
5. Do not hold the person down during a seizure.
6. Do not put anything in the person’s mouth.
7. Do not attempt artificial respiration. Do so only if the person is not breathing after the seizure has stopped.
REFERENCES
1. Fisher RS, Acevedo C, Arzimanoglou A, et al. ILAE official report: a practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475-482.2. Stafstrom CE, Carmant L. Seizures and epilepsy: an overview for neuroscientists. Cold Spring Harb Perspect Med. 2015;5(6):a022426.
3. Beghi E. The epidemiology of epilepsy. Neuroepidemiology. 2020;54(2):185-191.
4. CDC. Epilepsy data and statistics. www.cdc.gov/epilepsy/data/index.html. Accessed September 28, 2022.
5. Saxena S, Li S. Defeating epilepsy: a global public health commitment. Epilepsia Open. 2017;2(2):153-155.
6. Sokka A, Olsen P, Kirjavainen J, et al. Etiology, syndrome diagnosis, and cognition in childhood-onset epilepsy: a population-based study. Epilepsia Open. 2017;2(1):76-83.
7. Walsh S, Donnan J, Fortin Y, et al. A systematic review of the risks factors associated with the onset and natural progression of epilepsy. Neurotoxicology. 2017;61:64-77.
8. Chen J, Ye H, Zhang J, et al. Pathogenesis of seizures and epilepsy after stroke. Acta Epileptol. 2022;4(1):2.
9. Fordington S, Manford M. A review of seizures and epilepsy following traumatic brain injury. J Neurol. 2020;267(10):3105-3111.
10. Lowenstein DH. Epilepsy after head injury: an overview. Epilepsia. 2009;50(Suppl 2):4-9.
11. Liu S, Yu W, Lü Y. The causes of new-onset epilepsy and seizures in the elderly. Neuropsychiatr Dis Treat. 2016;12:1425-1434.
12. Vezzani A, Fujinami RS, White HS, et al. Infections, inflammation and epilepsy. Acta Neuropathol. 2016;131(2):211-234.
13. Pandis D, Scarmeas N. Seizures in Alzheimer disease: clinical and epidemiological data. Epilepsy Curr. 2012;12(5):184-187.
14. Scheffer IE, Berkovic S, Capovilla G, et al. ILAE classification of the epilepsies: position paper of the ilae commission for classification and terminology. Epilepsia. 2017;58(4):512-521.
15. Fisher RS, Cross JH, French JA, et al. Operational classification of seizure types by the International League Against Epilepsy: position paper of the ILAE Commission for Classification and Terminology. Epilepsia. 2017;58(4):522-530.
16. Tian N, Boring M, Kobau R, et al. Active epilepsy and seizure control in adults—United States, 2013 and 2015. MMWR Morb Mortal Wkly Rep. 2018;67:437-442.
17. Kanner AM, Bicchi MM. Antiseizure medications for adults with epilepsy: a review. JAMA. 2022;327(13):1269-1281.
18. Thijs RD, Surges R, O’Brien TJ, Sander JW. Epilepsy in adults. Lancet. 2019;393(10172):689-701.
19. Devinsky O, Vezzani A, O’Brien TJ, et al. Epilepsy. Nat Rev Dis Primer. 2018;4:18024.
20. Koshy S. Role of pharmacists in the management of patients with epilepsy. Int J Pharm Pract. 2012;20(1):65-68.
21. Vossler DG, Gidal BE. A summary of antiseizure medications available in the United States: 2020 update. American Epilepsy Society. September 10, 2020. www.aesnet.org/docs/default-source/pdfs-clinical/2020-september-aes_summary_of_asms.pdf?sfvrsn=c1a0ed0b_2. Accessed October 11, 2022.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





