US Pharm. 2020:45(4)5-7.
Pneumonia is not only a common and often serious infection with considerable morbidity and mortality, it also presents a major human burden and cost burden ($8 billion to treat pneumonia in the United States in 2002); the major burden of pneumonia in the community is borne by the elderly.1
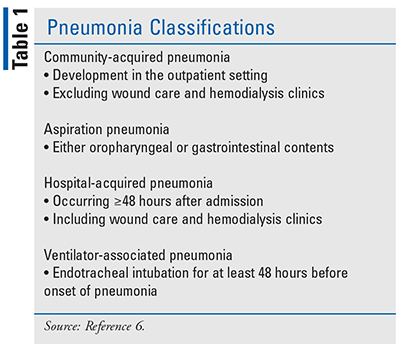
Pneumonia is classified by type (TABLE 1), which is based on bacterial etiology commonly acquired in different settings, such as the community or the hospital; common bacterial pathogens seen in community-acquired pneumonia (CAP) are discussed below.
In patients with CAP, respiratory viruses can be the sole cause of pneumonia (i.e., primary viral pneumonia); can be present as a coinfection (i.e., virus-bacteria or virus-virus); and can act as a predisposing factor to facilitate or worsen bacterial pneumonia.2 Viral infections are generally a more prominent cause of CAP among older adults.3 It has been specifically reported that patients with viral infections were significantly older than those without viral infections (median age, 76 vs. 64 years) and were more likely to have underlying cardiac disease (66% vs. 32%) and to be frail.4 Furthermore, it is common that viruses in the upper respiratory tract are detected in asymptomatic patients and thus may indicate convalescent shedding or asymptomatic infection.5
Respiratory viruses such as influenza and respiratory syncytial virus (RSV) are common causes of CAP.2 The role of Streptococcus pneumonia relative to viral causes of CAP may have decreased due to the widespread use of pneumococcal conjugate vaccines in children (see RESOURCES) and the increasing age of the population.2
Historically, although there has been an appreciation for respiratory viruses as a cause of CAP, they had been reported mostly among children, individuals with serious comorbidities, and military recruits; however, recognition of respiratory viruses as a cause of CAP in adults—particularly older adults—is increasing.2
Signs and Symptoms
Although caused by infection, pneumonia is defined as inflammation of the lung with consolidation (i.e., the lung fills with exudate). TABLE 2 outlines the respiratory symptoms and signs (productive/nonproductive cough, shortness of breath, difficulty breathing) and nonrespiratory (fever, headache, sweats, fatigue, myalgias, mental status changes) of CAP. In elderly patients, confusion, disorientation, and lethargy are common.6 Furthermore, as age increases, both respiratory and nonrespiratory symptoms decrease, which can make early recognition challenging. Chest x-rays, while diagnostic, are only moderately useful in discriminating viral from bacterial CAP.7-10 Successful management of pneumonia, particularly in the elderly, requires considerable skill.1
Pharmacotherapy and Pathogens
Pharmacologic therapy for CAP (TABLE 3) is predominately empiric and distinguishes the previously healthy outpatient from the adult outpatient with comorbidities. In the patient with CAP, comorbidities that have the potential to impact therapy and outcomes include diabetes mellitus; COPD; chronic heart, liver, or renal disease; malignancy; alcoholism; asplenia; and immunosuppressive disease or use of immunosuppressant therapy.11
Differentiating viral CAP from mixed infection and bacterial CAP remains challenging (see Reference 2). Common pathogens in CAP include the aerobic bacteria S pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis. Atypical pathogens seen are Mycoplasma pnemoniae, Chlamydophyla pneumoniae, Legionella pneumophilia, and respiratory viruses. Severe acute respiratory syndrome (SARS) and other coronaviruses have been shown to cause pneumonia in adults; a greater burden is found among patients older than age 65 years.12 In severe CAP (10% of CAP cases), intensive care or mechanical ventilation is required.6 Neuraminidase inhibitors (e.g., oseltamivir, zanamivir) reduce ICU admission and mortality among patients hospitalized with influenza, including those with pneumonia, and should be started when influenza is suspected.2
Viruses as a cause of CAP in adults range from 12% to 29% of cases; mixed infections of viruses and bacteria have been rising and have been identified in 11% to 56% of cases.13-16 There is evidence that respiratory viruses are an important cause of severe pneumonia and respiratory failure in immunocompromised patients, particularly hematopoietic stem-cell transplant recipients.17,18
With regard to coronaviruses, their role in pneumonia has not been completely clarified. In a prospective study of patients with severe pneumonia undergoing bronchoalveolar lavage, about half of whom were transplant recipients, coronaviruses were detected in 5.8%, mostly as the sole pathogen.19 Thus, it seems clear that they cause some cases of CAP in normal hosts and cause severe pneumonia in transplant patients.
Respiratory Viral Infection and Risk of Asthma Exacerbations
According to the CDC, individuals with asthma who get the flu are more likely to develop pneumonia as a complication.20 Viral infection is primarily responsible for exacerbations of asthma; the most common is rhinovirus, while other viral causes include RSV, parainfluenza virus, coronavirus, and influenza viruses.21-23 Other respiratory infections (e.g., M pneumoniae, C pneumoniae) and additional trigger categories (i.e., allergens, environment, exercise, occupational stimuli) can contribute to exacerbations as well; additionally, host factors such as allergic rhinitis, gastroesophageal reflux disease, or obesity may also cause or worsen symptoms.21,22 Pharmacists should consider these contributing factors during counseling discussions and medication-management sessions with patients.
The Inflammatory Response
As discussed, inflammation of the lung defines pneumonia. The complement system, part of the innate immune system, is the heat-labile cascade system of at least 20 serum glycoproteins that enhances (i.e., complements) the ability of antibodies and phagocytic cells to clear microbes and damaged cells from the body, promotes inflammation, and attacks the cell membrane of a pathogen.24 Pharmacists should have an understanding of the important role of local host defenses of the upper respiratory tract (i.e., mucociliary apparatus of the nasopharynx, nasal hair, normal bacterial flora, IgA, complement) and the lower respiratory tract (i.e., cough, mucociliary apparatus of the trachea and bronchi, antibodies [IgA, IgM, and IgG], complement, alveolar macrophages) in fighting CAP.6
Supporting the Immune System
Recently there have been efforts to raise the awareness of the public regarding the importance of immune-system support, and pharmacists may choose to incorporate this guidance, outlined below, in patient-centric, comprehensive medication-management plans. Keeping the immune system functioning optimally via interventions or lifestyle modifications is recommended through25:
• Keeping stress levels down so that the stress hormone cortisol does not have an opportunity to “turn off” cells in the immune system; engaging in relaxing activities (e.g., meditation) may help with this goal
• Low and moderate exercise, which can naturally lower cortisol levels and help improve the function of the immune system
• Getting adequate sleep—e.g., 7 to 8 hours for adults
• Keeping vaccines up-to-date, particularly the flu vaccine (see resources)
• Supporting the microbiome—daily yogurt consumption may help to achieve this goal
• Maintaining a healthful, balanced diet to obtain zinc, vitamin D, and other important vitamins and minerals; supplementation may be required if vitamin D levels are low; avoid ultralow-carbohydrate diets so the immune system is fuelled adequately
• Stopping smoking or vaping (see RESOURCES)
• Drinking plenty of water
• Reducing alcohol consumption
Conclusion
In older adults, pneumonia is associated with significant morbidity and mortality. In addition to the human burden, pneumonia poses a significant burden on healthcare resources. With age as a risk factor for CAP, pharmacists working with older adults are encouraged to promote prevention through appropriate immunization, awareness of respiratory and nonrespiratory symptoms and signs, appropriate pharmacologic treatment, and awareness of the importance of immune system support through interventions and lifestyle-modification measures.
REFERENCES
1. Marrie TJ. Pneumonia. Hazzard's Geriatric Medicine and Gerontology, 6th ed. Chapter 126. Pneumonia. https://accessmedicine.mhmedical.com/content.aspx?bookID=371§ionID=41587749&jumpsectionID=41600292&CAClickthru=96722. Accessed February 9, 2020.
2. Pavia AT. What is the role of respiratory viruses in community acquired pneumonia; what is the best therapy for influenza and other viral causes of CAP? Infect Dis Clin North Am. 2013;27(1):157-175.
3. Falsey AR, Walsh EE. Viral pneumonia in older adults. Clin Infect Dis. 2006;42:518-524.
4. Johnstone J, Majumdar SR, Fox JD, Marrie TJ. Viral infection in adults hospitalized with community-acquired pneumonia: prevalence, pathogens, and presentation. Chest. 2008;134:1141-1148.
5. Jartti T, Jartti L, Peltola V, et al. Identification of respiratory viruses in asymptomatic subjects: asymptomatic respiratory viral infections. Pediatr Infect Dis J. 2008;27(12):1103-1107.
6. Cappelletty DM. Lower respiratory tract infections. In: Chisholm-Burns MA, Schwinghammer TL, Malone PM, et al, eds. Pharmacotherapy: Principles & Practice, 5th ed. New York, NY: McGraw Hill Education. 2019:1091-1103.
7. Ruuskanen O, Lahti E, Jennings LC, Murdoch DR. Viral pneumonia. Lancet. 2011;377:1264-1275.
8. Virkki R, Juven T, Rikalainen H, et al. Differentiation of bacterial and viral pneumonia in children. Thorax. 2002;57:438-441.
9. Franquet T. Imaging of pulmonary viral pneumonia. Radiology. 2011;260:18-39.
10. Guo W, Wang J, Sheng M, et al. Radiological findings in 210 paediatric patients with viral pneumonia: a retrospective case study. Br J Radiol. 2012;85(1018):1385-1389.
11. Mandell LA, Wunderink RG, Anzueto A, et al. Infectious Diseases Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults. Clin Infect Dis. 2007;44(suppl 2):S27-S72.
12. Cesario TC. Viruses associated with pneumonia in adults. Clin Infect Dis. 2012;55(1):107-113.
13. Cilloniz C, Martin-Loeches I, Garcia-Vidal C, et al. Microbial etiology of pneumonia: epidemiology, diagnosis and resistance patterns. Int J Mol Sci. 2016;17:2120.
14. Jennings LC, Anderson TP, Beynon KA, et al. Incidence and characteristics of viral community-acquired pneumonia in adults. Thorax. 2008;63:42-48.
15. Van Gageldonk-Lafeber AB, Wever PC, van der Lubben IM, et al. The aetiology of community-acquired pneumonia and implications for patient management. Neth J Med. 2013;71(7):418-425.
16. Self WH, Balk RA, Grijalva CG, et al. Procalcitonin as a marker of etiology in hospitalized patients with community-acquired pneumonia. Clin Infect Dis. 2017;65(2):183-190.
17. Ison MG, Michaels MG. RNA respiratory viral infections in solid organ transplant recipients. Am J Transplant. 2009;9(Suppl 4):S166-S172.
18. Kim YJ, Boeckh M, Englund JA. Community respiratory virus infections in immunocompromised patients: hematopoietic stem cell and solid organ transplant recipients, and individuals with human immunodeficiency virus infection. Semin Respir Crit Care Med. 2007;28:222-242.
19. Garbino J, Crespo S, Aubert JD, et al. A prospective hospital-based study of the clinical impact of non-severe acute respiratory syndrome (Non-SARS)-related human coronavirus infection. Clin Infect Dis. 2006;43:1009-1015.
20. Pietrangelo A. Asthma and pneumonia: what are the differences. April 30, 2018. www.healthline.com/health/asthma/asthma-and-pneumonia. Accessed March 26, 2020.
21. Sears MR. Epidemiology of asthma exacerbations. J Allergy Clin Immunol. 2008;122:662-668.
22. Global Initiative for Asthma (GINA). Global strategy for asthma management and prevention. Updated 2017. www.ginasthma.org/. Accessed March 8, 2020.
23. Maniscalco-Feichtl M, Melin K. Asthma MTM data set. In: Whalen K, Hardin HC, eds. Medication Therapy Management: A Comprehensive Approach. 2nd ed. New York, NY: McGraw Hill Education. 2018:203-223.
24. Janeway CA Jr., Travers P, Walport M, et al. The complement system and innate immunity. In: Immunobiology: The Immune System in Health and Disease. New York: Garland Science. 2001.
25. Reddy S. What works (and doesn’t work) to boost your immune system. Special Report: Navigating the coronavirus. Wall Street Journal. March 13, 2020:R2.
To comment on this article, contact rdavidson@uspharmacist.com.