US Pharm. 2021;46(2):17-20.
ABSTRACT: Coronavirus disease 2019 (COVID-19) is an infection caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Although COVID-19 primarily affects the respiratory system, it can also cause cardiovascular complications. Patients with pre-existing cardiovascular comorbidities are at risk for greater severity of illness and mortality. The cardiovascular effects of medications that may be used to treat COVID-19, as well as the impact of medications used for underlying cardiovascular conditions, are important considerations. Pharmacists should be aware of the potential cardiovascular impact of COVID-19.
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is a new type of coronavirus that causes coronavirus disease 2019 (COVID-19).1 COVID-19 has emerged as a pandemic, with documented cases of over 24 million people in the United States and 97 million people worldwide as of January 21, 2021.2,3 COVID-19–related deaths have risen to over 400,000 in the U.S. and 2 million worldwide.2,3 Individuals with COVID-19 may remain asymptomatic or display symptoms ranging from mild to severe.1 Complications can include cardiovascular manifestations that affect the heart, blood vessels, and coagulation system.1 Notably, patients with pre-existing cardiovascular comorbidities who are infected with COVID-19 are at risk for greater severity of illness and mortality.4,5 This article provides an overview of the interactions and implications of cardiovascular comorbidities and manifestations of COVID-19 given the known risk for increased morbidity and mortality in this patient population. As data are rapidly evolving, treatment guidelines and other resources should be consulted for the most updated information.
COVID-19 AND THE CARDIOVASCULAR SYSTEM
Comorbidities and Risk Factors
The CDC lists several medical conditions in adults that are associated with an increased risk for severe illness from COVID-19, as well as medical conditions in adults that might be associated with an increased risk for severe illness.5 TABLE 1 includes selected cardiovascular risk factors that are included in this list of medical conditions.5
Pathophysiology
The mechanisms of cardiovascular disruption from COVID-19 are likely multifactorial and have not been fully elucidated. It is known that severe infection, especially respiratory infection, can cause systemic changes (e.g., sepsis, shock, hypoxemia, stress) that affect the cardiovascular system.6-8 While these manifestations can also occur with COVID-19, additional mechanisms with pathogenesis specific to COVID-19 are further discussed.
One proposed mechanism is an interaction between the virus, angiotensin-converting enzyme 2 (ACE2) expression, and the renin-angiotensin-aldosterone system (RAAS).4,9-11 SARS-CoV-2 is an enveloped RNA virus that uses the ACE2 receptor (present in lungs, kidneys, heart, and blood vessels) to bind and enter human cells.4,9-12 The availability of ACE2 on myocardial and endothelial cells provides a possible explanation for SARS-CoV-2 entry into cells and resultant direct cardiotoxicity.4,9-12
ACE2 is known to have protective effects by counteracting angiotensin II and the excessive activation of RAAS that occurs in cardiovascular disease (CVD) states such as hypertension, congestive heart failure, and atherosclerosis.9,10 In patients with diabetes mellitus and CVD, ACE2 levels have been shown to be upregulated.11 Given that SARS-CoV-2 uses ACE2 to enter cells, it is suggested that those with pre-existing CVD are more susceptible to the virus and associated morbidity.11,12 Furthermore, once SARS-CoV-2 enters a cell it has been shown to decrease expression of ACE2.10-12 Therefore, cardiovascular manifestations in COVID-19 patients may be due to a downregulation and loss of ACE2-mediated protection in the heart and blood vessels.10-12 The dual implications of ACE2 expression require further research on clinical significance as it can both increase susceptibility to COVID-19 and protect the cardiovascular system.
Another proposed mechanism linking cardiovascular disruption to COVID-19 involves the immune system. A prominent proinflammatory response can occur in patients with COVID-19 and lead to a more severe disease course.11,12 The hyperinflammation and overproduction of cytokines, often called a “cytokine storm,” can cause vascular and myocardial inflammation, plaque instability, endothelial dysfunction, and a hypercoagulable state.4,11,12 Hyperinflammation can also lead to systemic conditions such as sepsis and disseminated intravascular coagulation, which may further promote cardiovascular injury.4,13
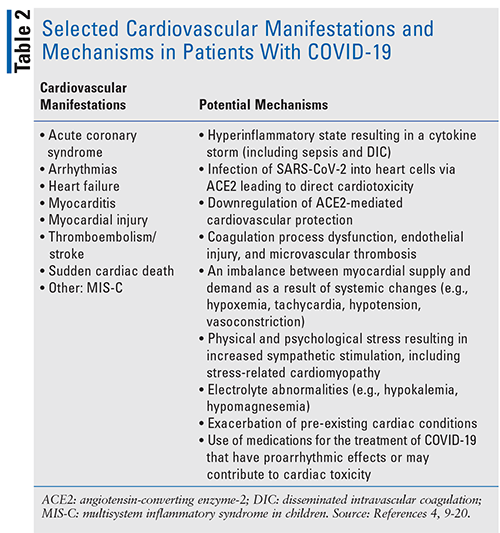
A summary of the mechanisms and cardiovascular manifestations that have been identified in patients with COVID-19 are included in TABLE 2.4,9-20
IMPACT OF MEDICATIONS
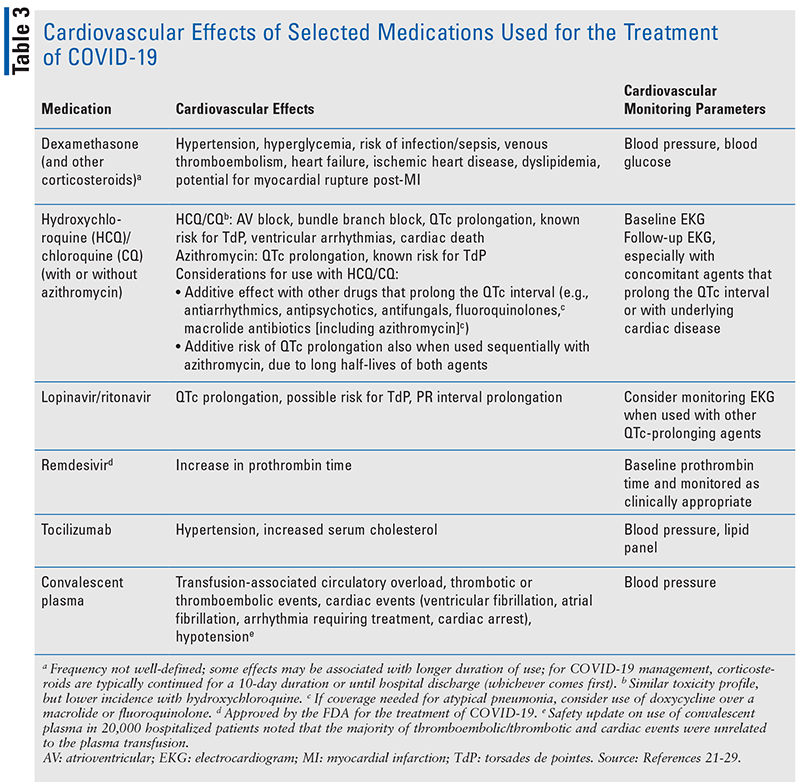
Medications that are approved or under evaluation for the treatment of COVID-19 may also have an impact on the cardiovascular system, either through direct effects or via drug interactions with other medications (TABLE 3).21-29 The reader is referred to the National Institutes of Health (NIH) guidelines for the most recent recommendations for use of these agents for the treatment of COVID-19.21
Treatment Considerations
ACE Inhibitors, ARBs, NSAIDs: Since ACE2 has been shown to be the human cell receptor for SARS-CoV-2, a hypothetical concern has been suggested that agents that increase ACE2 expression (e.g., angiotensin-converting enzyme [ACE] inhibitors, angiotensin receptor blockers [ARBs], ibuprofen) may increase the risk for, or worsen the course of, COVID-19.30-32 However, according to the American Heart Association, the Heart Failure Society of America, and the American College of Cardiology, there are no experimental or clinical data that demonstrate either beneficial or adverse outcomes with background use of ACE inhibitors or ARBs.33 These societies released a joint statement that recommends continuation of these agents in those who have an indication and that any RAAS-related treatments should not be added or removed beyond actions based on standard clinical practice.33 This is supported by the NIH guidelines, which recommend continuing prescribed ACE inhibitors or ARBs for CVD (or other indications) in those with COVID-19.21
The FDA released a statement in March 2020 indicating that there is no scientific evidence establishing an association between ibuprofen and worsening COVID-19 and encouraged patients to take all medications in accordance with label instructions and as directed by a healthcare professional.34 The NIH guidelines recommend no difference in the use of antipyretic agents for those with or without COVID-19 and recommend continuing therapy for those previously directed to take a nonsteroidal anti-inflammatory drug (NSAID).21
Statins: Although some authors have suggested that statins may be useful for the treatment of patients with severe infection, the NIH guidelines recommend against the use of statins for the treatment of COVID-19 except in the context of a clinical trial.21,35 The guidelines recommend continuing prescribed statin therapy for the treatment or prevention of CVD in those with COVID-19.21
Anticoagulation: Given the known risk of thrombosis in patients with COVID-19, the American College of Chest Physicians has released a guideline for the prevention, diagnosis, and treatment of venous thromboembolism in patients with COVID-19.13 In the absence of a contraindication, hospitalized patients with COVID-19 should receive anticoagulation prophylaxis, and all COVID-19 patients with proximal deep-vein thrombosis or pulmonary embolism should receive anticoagulation therapy for a minimum of 3 months.13 The complete CHEST guideline is available at https://doi.org/10.1016/j.chest.2020.05.559.
General Measures for Patients With Cardiovascular Comorbidities
The CDC has general recommendations for individuals with cardiovascular comorbidities that are associated, or might be associated, with an increased risk for severe illness from COVID-19.5 Additionally, the CDC stresses the importance of ensuring that all individuals have a healthcare provider, as well as resources to find a provider.5 The CDC recommendations for patients include to:
• Receive an annual influenza vaccine
• Take medicines as prescribed for medical conditions
• Have at least a 30-day home supply of medications
• Follow a healthcare provider’s recommendations for diet/nutrition and physical activity while maintaining social distancing precautions
• Contact a provider if there are concerns about illness or a medical condition
• Talk with a provider to ensure vaccinations and other preventive services such as cancer screenings are up to date
• Not delay emergency care (if needed)
• Quit smoking and speak with a provider about medications and/or counseling to help with this process
The Pharmacist’s Role
It is important for pharmacists to understand the impact of COVID-19 on the cardiovascular system since patients with pre-existing cardiovascular comorbidities are at an increased risk for more severe illness. Pharmacists should educate providers about the cardiovascular impact and recommended monitoring parameters for medications used for the treatment of COVID-19. Pharmacists are in a key position to recommend appropriate management for patients with cardiovascular comorbidities who have COVID-19.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Wiersinga WJ, Rhodes A, Cheng AC, et al. Pathophysiology, transmission, diagnosis, and treatment of coronavirus disease 2019 (COVID-19): a review. JAMA. 2020;324(8):782-793.
2. CDC. Coronavirus disease 2019 (COVID-19): cases in U.S. https://covid.cdc.gov/covid-data-tracker/#cases_casesper100klast7days. Accessed January 21, 2021.
3. Johns Hopkins Coronavirus Resource Center. Coronavirus COVID-19 global cases by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU). https://coronavirus.jhu.edu/map.html. Accessed January 21, 2021.
4. Kang Y, Chen T, Mui D, et al. Cardiovascular manifestations and treatment considerations in COVID-19. Heart. 2020;106(15):1132-1141.
5. CDC. People with certain medical conditions. www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html. Accessed November 21, 2020.
6. Smeeth L, Thomas SL, Hall AJ, et al. Risk of myocardial infarction and stroke after acute infection or vaccination. N Engl J Med. 2004;351(25):2611-2618.
7. Corrales-Medina VF, Musher DM, Wells GA, et al. Cardiac complications in patients with community-acquired pneumonia: incidence, timing, risk factors, and association with short-term mortality. Circulation. 2012;125(6):773-781.
8. Merx MW, Weber C. Sepsis and the heart. Circulation. 2007;116(7):793-802.
9. Vaduganathan M, Vardeny O, Michel T, et al. Renin-angiotensin-aldosterone system inhibitors in patients with Covid-19. N Engl J Med. 2020;382(17):1653-1659.
10. Clerkin KJ, Fried JA, Raikhelkar J, et al. COVID-19 and cardiovascular disease. Circulation. 2020;141(20):1648-1655.
11. Wu L, O’Kane AM, Peng H, et al. SARS-CoV-2 and cardiovascular complications: from molecular mechanisms to pharmaceutical management. Biochem Pharmacol. 2020;178:114114.
12. Nishiga M, Wang DW, Han Y, et al. COVID-19 and cardiovascular disease: from basic mechanisms to clinical perspectives. Nat Rev Cardiol. 2020;17(9):543-558.
13. Moores LK, Tritschler T, Brosnahan S, et al. Prevention, diagnosis, and treatment of VTE in patients with coronavirus disease 2019: CHEST guideline and expert panel report. Chest. 2020;158(3):1143-1163.
14. Bansal M. Cardiovascular disease and COVID-19. Diabetes Metab Syndr. 2020;14(3):247-250.
15. Shafi AMA, Shaikh SA, Shirke MM, et al. Cardiac manifestations in COVID-19 patients—a systematic review. J Card Surg. 2020;35(8):1988-2008.
16. Zhu H, Rhee JW, Cheng P, et al. Cardiovascular complications in patients with COVID-19: consequences of viral toxicities and host immune response. Curr Cardiol Rep. 2020;22(5):32.
17. Madjid M, Safavi-Naeini P, Solomon SD, Vardeny O. Potential effects of coronaviruses on the cardiovascular system: a review. JAMA Cardiol. 2020;5(7):831-840.
18. Atri D, Siddiqi HK, Lang JP, et al. COVID-19 for the cardiologist: basic virology, epidemiology, cardiac manifestations, and potential therapeutic strategies. JACC Basic Transl Sci. 2020;5(5):518-536.
19. Lang JP, Wang X, Moura FA, et al. A current review of COVID-19 for the cardiovascular specialist. Am Heart J. 2020;226:29-44.
20. Kochi AN, Tagliari AP, Forleo GB, et al. Cardiac and arrhythmic complications in patients with COVID-19. J Cardiovasc Electrophysiol. 2020;31(5):1003-1008.
21. National Institutes of Health. Coronavirus disease 2019 (COVID-19) treatment guidelines. www.covid19treatmentguidelines.nih.gov/. Accessed November 16, 2020.
22. Driggin E, Madhavan MV, Bikdeli B, et al. Cardiovascular considerations for patients, health care workers, and health systems during the COVID-19 pandemic. J Am Coll Cardiol. 2020;75(18):2352-2371.
23. Sanders JM, Monogue ML, Jodlowski TZ, Cutrell JB. Pharmacologic treatments for coronavirus disease 2019 (COVID-19): a review. JAMA. 2020;323(18):1824-1836.
24. Giudicessi JR, Noseworthy PA, Friedman PA, Ackerman MJ. Urgent guidance for navigating and circumventing the QTc-prolonging and torsadogenic potential of possible pharmacotherapies for coronavirus disease 19 (COVID-19). Mayo Clin Proc. 2020;95(6):1213-1221.
25. Waljee AK, Rogers MA, Lin P, et al. Short-term use of oral corticosteroids and related harms among adults in the United States: population based cohort study. BMJ. 2017;357:j1415.
26. Joyner MJ, Bruno KA, Klassen SA, et al. Safety update: COVID-19 convalescent plasma in 20,000 hospitalized patients. Mayo Clin Proc. 2020;95(9):1888-1897.
27. Souverein PC, Berard A, Van Staa TP, et al. Use of oral glucocorticoids and risk of cardiovascular and cerebrovascular disease in a population-based case-control study. Heart. 2004;90(8):859-865.
28. Sholter DE, Armstrong PW. Adverse effects of corticosteroids on the cardiovascular system. Can J Cardiol. 2000;16(4):505-511.
29. World Health Organization. Coronavirus disease (COVID-19): dexamethasone. www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub/q-a-detail/q-a-dexamethasone-and-covid-19?gclid=EAIaIQobChMIq9-A37iU7QIVDdvACh05kw6uEAAYASAAEgKHXPD_BwE. Accessed November 21, 2020.
30. Fang L, Karakiulakis G, Roth M. Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection? Lancet Respir Med. 2020;8(4):e21.
31. Esler M, Esler D. Can angiotensin receptor-blocking drugs perhaps be harmful in the COVID-19 pandemic? J Hypertens. 2020;38(5):781-782.
32. Sommerstein R, Kochen MM, Messerli FH, Gräni C. Coronavirus disease 2019 (COVID-19): do angiotensin-converting enzyme inhibitors/angiotensin receptor blockers have a biphasic effect? J Am Heart Assoc. 2020;9(7):e016509.
33. Bozkurt B, Kovacs R, Harrington B. HFSA/ACC/AHA statement addresses concerns re: using RAAS antagonists in COVID-19. www.acc.org/latest-in-cardiology/articles/2020/03/17/08/59/hfsa-acc-aha-statement-addresses-concerns-re-using-raas-antagonists-in-covid-19. Accessed November 17, 2020.
34. FDA. FDA advises patients on use of non-steroidal anti-inflamma¬tory drugs (NSAIDs) for COVID-19. www.fda.gov/drugs/drug-safety-and-availability/fda-advises-patients-use-non-steroidal-anti-inflammatory-drugs-nsaids-covid-19. Accessed November 17, 2020.
35. Fedson DS, Opal SM, Rordam OM. Hiding in plain sight: an approach to treating patients with severe COVID-19 infection. mBio. 2020 ;11(2):e00398-20.
To comment on this article, contact rdavidson@uspharmacist.com.