US Pharm. 2016;41(3):HS11-HS15.
ABSTRACT: Post–intensive care syndrome (PICS) is a myriad of chronically debilitating symptoms, often including chronic pain, associated with prolonged ICU care. Though the exact mechanism of chronic post-ICU pain is unknown, it is postulated that the severity of inflammation associated with many forms of critical illness leads to chronic pain in patients long after resolution of their acute critical illness. Increasing emphasis on long-term outcomes of ICU survivors makes prevention of chronic pain and PICS a priority for multidisciplinary ICU teams. This article discusses the prevalence and mechanisms of chronic post-ICU pain and suggests strategies to reduce the impact of chronic pain on quality of life in ICU survivors.
Acute pain is a common and distressing complication of critical illness experienced by the majority of patients while admitted to the ICU. Pain is often identified by patients as a leading cause of stress and lack of sleep during critical illness, and many patients report severe pain as the most traumatic memory of their ICU stay.1,2 Acute ICU pain may be caused by underlying illness and inflammation, diagnostic or therapeutic procedures, or invasive medical devices. In addition to acute pain experienced during critical illness, many ICU survivors continue to experience significant pain for months or years after ICU discharge as part of post–intensive care syndrome (PICS).3
Chronic pain, or pain that persists beyond the predicted healing period, can affect quality of life long after resolution of the acute critical illness. This article will discuss risk factors and the suspected mechanisms of transition from acute to chronic post-ICU pain, as well as investigational strategies to mitigate acute ICU pain and prevent the development of chronic post-ICU pain.
Prevalence of Chronic Post-ICU Pain and PICS
Increasing emphasis on long-term outcomes of ICU survivors has resulted in a number of observational studies identifying severe functional limitation and a high incidence of pain persisting long after ICU discharge. Schelling et al surveyed 80 patients treated for acute respira-tory distress syndrome (ARDS) at a median follow-up of 4 years post-ICU discharge.4 Their questionnaire identified many ICU survivors with a high incidence of chronic pain (38%), posttraumatic stress disorder (PTSD) symptoms (27%), and a lower health-related quality of life (21%). Other systematic reviews have estimated PTSD incidence as high as 64% based upon clinical interviews.5 In a survey-based, quality-of-life assessment of 164 patients 2 years post-ICU stay, 60% of patients had signs of depression, almost 60% had problems in usual living activities, and 56% continued to experience pain.6 A similar quality-of-life study evaluating 575 patients 6 to 11 years after ICU discharge also reported a high incidence of long-term sequelae of critical illness; many patients experienced persistent difficulty with mobility (52%), self-care (19%), usual activity (52%), pain/discomfort (57%), and cognition (43%).7
Though direct correlations with pain severity experienced in the ICU and long-term quality-of-life indicators have not been established, these reports have led to the creation of forums and informational websites by the Society of Critical Care Medicine for patients and families post-ICU stay.8 Early interventions to decrease the duration of illness and pain experience are targets of transitional team management for all ICU patients.
Consequences of Chronic Pain
Consequences of uncontrolled pain include both short- and long-term harm. Acutely, inadequate pain control is associated with development of anxiety, depression, and sleep disturbances. For the ICU patient, pain dysregulation has also been correlated to immunosuppression, coagulopathies, ventilator dyssynchrony, glucose dysregulation, and myocardial ischemia.9,10 The stress response evoked from uncontrolled pain results in increased catecholamine release, leading to arteriolar vasoconstriction, impaired perfusion, and reduced tissue oxygenation. Additional stress response mechanisms include endogenous steroid release and trigger hyper-catabolism, hyperglycemia, impaired wound healing, and increased risk of infection.11,12 This rotating mechanism of pain and illness leads to increased morbidity and mortality among ICU patients. Optimized pain pharmacotherapy may lead to improved patient outcomes within and beyond the ICU.
Modulation of Pain Perception
The physiological mechanism of pain involves activation of nociceptive pathways, which arises from direct, local tissue damage.9 The pathway of pain transmission, known as nociception, originates at the site of tissue injury through release of local inflammatory mediators such as bradykinin, substance P, prostaglandins, potassium, histamine, and serotonin. Nociceptors, after exposure to these noxious stimuli and inflammatory mediators, then transmit a nerve impulse (transduction) to the spinal cord and then centrally to the brain through afferent pathways.9,13-17 Interpretation of these pain signals in the higher central areas of the brain, specifically the cortical and limbic systems, typically motivates patients to avoid further stimulation or damage, which is protective of the tissues. Acutely, repeated nociception results in peripheral sensitization, a short-term increase in the sensitivity of the afferent nerve fibers and amplification of the pain signals. This acute hypersensitivity to pain further motivates avoidance behaviors until the inflammation subsides or the injury heals, at which point the hypersensitivity should resolve.3,9,13-17
Prolonged or repeated stimulation of nociceptors can produce hypersensitivity modulation reactions that lead acute pain to develop into chronic pain. Increases in neuronal excitability occur when peripheral nociceptors experience semipermanent modulation via long-term exposure to sensitizing agents and inflammatory mediators such as cytokines, epinephrine, adenosine, and sero-tonin.9,13-17 Hyperalgesia is an increased sensitivity to painful stimuli. It is the result of excessive excitability of nociceptive spinal cord neurons that increase trans-mission of nonpainful stimuli or generate spontaneous signals even in the absence of a stimulus. Perception of nonpainful, nonnoxious stimuli by the central nervous system (CNS) as painful is known as allodynia. Hyperalgesia and allodynia may develop due to either repeated neuronal damage or sustained inflammatory processes. They typically do not resolve on healing of the initial tissue injury, and are therefore considered pathologic or maladaptive causes of chronic pain. This kind of pain is known as neuropathic pain, or pain that is caused by abnormal neuron function rather than by physical tissue injury. The mechanism of developing chronic, neuropathic pain with hyperalgesia and allodynia has been described as neuronal plasticity.13-17
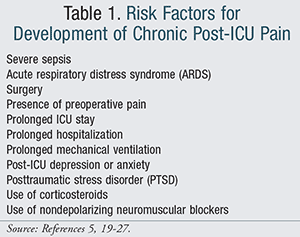
ICU patients are at increased risk of development of hyperalgesic neuromodulation through the neuronal plasticity mechanism. Frequently, invasive devices and techniques in the ICU (e.g., endotracheal tube insertion and placement, suctioning, surgeries, presence of chest tubes, repeated phlebotomy, wound care, gastric tubes, and vascular access devices) result in sustained periods of unresolved procedural pain.3,9,10,18 Prolonged immobility and anxiety also augment the sensation of pain in ICU patients, leading to increased frequency and severity of perceived pain sensation.18 Due to sedative medications, physical restraints or injury, altered mental status, and other disease complications, ICU patients are often unable to engage in avoidance behaviors that would normally serve to minimize painful stimuli. Thus, ICU patients experience neuroplastic hyperalgesia and allodynia more commonly than noncritically ill patients, leading to a high incidence of chronic pain in ICU survivors.3,10,17 Other patient- and disease-specific risk factors for development of chronic post-ICU pain are listed in TABLE 1.5,19-27
Pain Mitigation Strategies
Given the debilitating impact of chronic pain on quality of life, minimizing its occurrence in ICU survivors must become a priority for critical care practitioners. Recognition of risk factors for chronic pain in ICU survivors is a first step in the prevention and management of the condition (TABLE 1). Appropriate management of acute pain may prevent development of chronic pain in high-risk patients by minimizing neuroplastic modulation mechanisms.10,28 Systematic efforts to improve pain management typically focus on mandated pain assessment, which requires physicians and nurses to document pain assessments at regular intervals. Mandated pain assessment is often implemented through the use of protocols that describe pain as the “fifth vital sign” and suggest use of validated pain assessment tools at specified time intervals. Mandated pain assessment not been prospectively studied in relation to decreasing chronic post-ICU pain, but it is still considered the standard of practice in critical care settings to manage acute pain.10,28
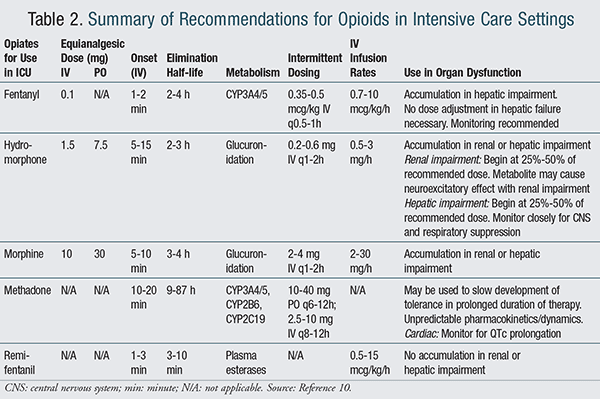
Pharmacists play a vital role in the development of interdisciplinary pain management protocols. Given the severity of pain experienced by ICU patients, opioids should be considered the drugs of choice for acute pain management in critical care settings.10,28 Opioid selection should be based upon pain severity, presence of drug allergies or organ dysfunction, need for rapid onset and/or offset of action, anticipated duration of therapy, and prior response to therapy.10,28 TABLE 2 summarizes recommendations for opioids commonly used in intensive care settings.10
Medications, including opioids, have been implicated as iatrogenic causes of acute pain in the ICU.10,28 Opioids have been associated with hyperalgesia phenomena resulting from neuroplastic sensitization of pain perception pathways, which may contribute to the development of chronic post-ICU pain.29 Practice guidelines recommend minimizing opioid use to prevent excessive harms from oversedation, hyperalgesia, or dependence.10,28 Coadministration of ketamine with opiates has reduced the development of opioid hyperalgesia in animal models.30 Additionally, corticosteroids and nondepolarizing neuromuscular blockers have been strongly associated with critical illness neuromyopathy, a type of disuse atrophy that leads to delayed recovery and prolonged ICU stays that increase the risk of chronic post-ICU pain.27 Use of corticosteroids and neuromuscular blockers should be avoided except in very select circumstances. When their use is necessary, minimization and weaning strategies exist to decrease the adverse effect of chronic pain resulting from these drugs.
Nonopioid analgesics are recommended as adjunctive therapy in ICU pain for an opiate-sparing effect, though their safety profiles have not been well studied in critical illness. Acetaminophen and nonsteroidal anti-inflammatory analgesic drugs (NSAIDs) are commonly employed as adjuncts to opioids, though they are not recommended as monotherapy.10,28 Both carbamazepine and gabapentin have been used successfully as adjuncts to opiates in the ICU, though gabapentin demonstrated greater efficacy than carbamazepine in one comparative study of patients with Guillain-Barré syndrome.31 These agents, used as opiate-sparing adjunctive agents for pain control, provide the benefit of pain management optimization while decreasing the long-term, deleterious effects associated with high-dose, long-duration opiate use. Pharmacists should consider the need for renal dose adjustment of gabapentin and the risk of drug-drug interactions with carbamazepine when using these agents.
Other adjunct agents may offer benefits in reducing the neurocognitive symptoms of PICS, which are known risk factors for chronic post-ICU pain. The selective alpha2-agonist dexmedetomidine, used either intraoperatively or postoperatively, has been associated with increased neurocognitive function post-ICU stay.32 Dexmedetomidine has also been associated with reduced duration of mechanical ventilation, a known risk factor for PICS and chronic post-ICU pain.33
Ketamine, a noncompetitive N-methyl-d-aspartate (NMDA) antagonist, has been shown to reduce PTSD symptoms as well as comorbid depressive symptoms.34 Because the NMDA receptor is thought to play a vital role in the neuroplastic mechanisms of chronic pain development, ketamine continues to be explored in the ICU setting as an adjunctive or alternative sedative.13-17 However, the ability of dexmedetomidine and ketamine to reduce ICU-related stress and improve post-ICU outcomes has not yet been studied on a large scale. The well-described psychotropic side effects of ketamine may limit the agent’s practical use as an adjunct agent for analgesia or sedation.
Minimizing known risk factors for development of chronic post-ICU pain through early use of physical therapy services may also help prevent development of chronic pain in ICU survivors. Initial studies of early mobilization and physical rehabilitation of ICU patients, including mobilization of ventilated patients, demonstrate significant reductions in ICU length of stay and duration of mechanical ventilation. Additionally, early mobility of ICU patients improves the physical and mental health outcomes of ICU survivors.35 Appropriate acute pain management is of vital importance to patient participation in early mobilization efforts.10
Conclusion
Chronic post-ICU pain, a component of PICS, is thought to develop as the result of repeated neuronal damage or sustained inflammation resulting from prolonged critical illness. Critical care practitioners are increasing focused on post-ICU outcomes, including quality-of-life components such as the presence of chronic pain. Thus, addressing causes and risk factors for development of chronic pain during the ICU stay is an important part of patient care during ICU admissions. Some possible strategies to manage acute pain and prevent development of chronic post-ICU pain may include protocolized acute pain management, opioid-sparing adjunct analgesics, prevention of post-ICU depression and PTSD, and early mobilization. Pharmacists can play an important role in appropriate analgesic selection and risk factor minimization as part of the interdisciplinary healthcare team.
REFERENCES
1. Jones J, Hoggart B, Withey J, et al. What the patients say: a study of reactions to an intensive care unit. Intensive Care Med. 1979;5:89-92.
2. Schelling G, Richter M, Roozendaal B, et al. Exposure to high stress in the intensive care unit may have negative effects on health-related quality-of-life outcomes after cardiac surgery. Crit Care Med. 2003;31:1971-1980.
3. Kyranou M, Puntillo K. The transition from acute to chronic pain: might intensive care unit patients be at risk? Ann Intensive Care. 2012;2:36.
4. Schelling G, Stoll C, Haller M, et al. Health-related quality of life and posttraumatic stress disorder in survivors of the acute respiratory distress syndrome. Crit Care Med. 1998;26:651-659.
5. Griffiths J, Fortune G, Barber V. The prevalence of post traumatic stress disorder in survivors of ICU treatment: a systematic review. Intensive Care Med. 2007;33(9):1506-1518.
6. Jagodic HK, Jagodic K, Podbregar M. Long-term outcome and quality of life of patients treated in surgical intensive care: a comparison between sepsis and trauma. Crit Care. 2006;10:R134.
7. Timmers TK, Verhofstad MH, Moons KH, et al. Long-term quality of life after surgical intensive care admission. Arch Surg. 2011;146:412-418.8. Davidson JE, Hopkins RO, Louis D, Iwashyna TJ. Post-intensive care syndrome. Society of Critical Care Medicine. 2013. www.myicucare.org/Adult-Support/Pages/Post-intensive-Care-Syndrome.aspx. Accessed November 30, 2015.
9. Fisham S, Ballantyne J, Rathmell J. Bonica’s Management of Pain. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2010.
10. Barr J, Fraser GL, Puntillo K, et al. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. Crit Care Med. 2013;41(1):263-306.
11. Peterson PK, Chao CC, Molitor T, et al. Stress and pathogenesis of infectious disease. Rev Infect Dis. 1991;13:710-720.
12. Puntillo KA, Miaskowski C, Summer G. Pain. In: Carrieri-Kohlman V, Lindsey AM, West CM, eds. Pathophysiological Phenomena in Nursing: Human Responses to Illness. 3rd ed. St. Louis, MO: Saunders; 2003:235-255.
13. Woolf CJ. Neural plasticity: increasing the gain in pain. Science. 2000;288(5472):1765-1769.
14. Sandkuhler J. Models and mechanisms of hyperalgesia and allodynia. Physiol Rev. 2009;89:707-758.
15. Kelly DJ, Ahmad M, Brull SJ. Preemptive analgesia I: physiological pathways and pharmacological modalities. Can J Anaesth. 2001;48:1000-1010.
16. Woolf CJ, Chong MS. Preemptive analgesia—treating postoperative pain by preventing the establishment of central sensitization. Anesth Analg. 1993;77:362-379.
17. Reardon DP, Anger KE, Szumita PM. Pathophysiology, assessment, and management of pain in critically ill adults. Am J Health-Syst Pharm. 2015;72(18):1531-1543.
18. Chanques G, Sebbane M, Barbotte E, et al. A prospective study of pain at rest: incidence and characteristics of an unrecognized symptom in surgical and trauma versus medical intensive care unit patients. Anesthesiology. 2007;107:858-860.
19. Dowdy DW, Eid MP, Dennison CR, et al. Quality of life after acute respiratory distress syndrome: a meta-analysis. Intensive Care Med. 2006;32:1115-1124.
20. Marx G, Zimmer A, Rothaug J, et al. Chronic pain after surviving sepsis. Crit Care. 2006;10(suppl 1):421.
21. Der Schaaf M, Beelan A, Dongelmans D, et al. Poor functional recovery after critical illness: a longitudinal study. J Rehabil Med. 2009;41:1041-1048.
22. Perkins FM, Kehlet H. Chronic pain as an outcome of surgery. A review of predictive factors. Anaesthesiology. 2000;93:1123-1133.
23. Battle CE, Lovett S, Hutchings H. Chronic pain in survivors of critical illness: a retrospective analysis of incidence and risk factors. Crit Care. 2013;17:R101.
24. Boyle M, Murgo M, Adamson H, et al. The effect of chronic pain on health related quality of life amongst intensive care survivors. Aust Crit Care. 2004;17(3):104-106.
25. Mok LC, Lee IF. Anxiety, depression and pain intensity in patients with low back pain who are admitted to acute care hospitals. J Clin Nurs. 2008;17(11):1471-1480.
26. Rattray JE, Hull AM. Emotional outcome after intensive care: literature review. J Adv Nurs. 2008;64:2-13.
27. Fan E, Zanni JM, Dennison CR, et al. Critical illness neuromyopathy and muscle weakness in patients in the intensive care unit. AACN Adv Crit Care. 2009;20(3):243-253.
28. Sessler CN, Varney K. Patient-focused sedation and analgesia in the ICU. Chest. 2008;133(2):552-565.
29. Lee M, Silverman SM, Hansen H, et al. A comprehensive review of opioid-induced hyperalgesia. Pain Physician. 2011;14(2):145-161.
30. Joly V, Richebe R, Guignard B, et al. Remifentanil-induced postoperative hyperalgesia and its prevention with small-dose ketamine. Anesthesiology. 2005;103:147-155.
31. Pandey CK, Raza M, Tripathi M, et al. The comparative evaluation of gabapentin and carbamazepine for pain management in Guillain-Barré syndrome patients in the intensive care unit. Anesth Analg. 2005;101:220-225.
32. Li B, Wang H, Wu H, Gao C. Neurocognitive dysfunction risk alleviation with the use of dexmedetomidine in perioperative conditions or as ICU sedation: a meta-analysis. Medicine (Baltimore). 2015;94(14):e597.
33. Jakob SM, Ruokonen E, Grounds RM. Dexmedetomidine vs midazolam or propofol for sedation during prolonged mechanical ventilation: two randomized controlled trials. JAMA. 2012;21;307(11):1151-1160.
34. Feder A, Parides MK, Murrough JW. Efficacy of intravenous ketamine for treatment of chronic posttraumatic stress disorder: a randomized clinical trial. JAMA Psychiatry. 2014;71(6):681--688.
35. Adler J, Malone D. Early mobilization in the intensive care unit: a systematic review. Cardiopulm Phys Ther J. 2012;23:5-13.
To comment on this article, contact rdavidson@uspharmacist.com.






