US Pharm. 2012;37(6)(Generic suppl):46-50.
Back in 1931, it was thought that “the treatment of hypertension itself is a difficult and almost hopeless task…for ought we know the hypertension may be an important compensatory mechanism which should not be tampered with.”1 Today, of course, we recognize that this is not true. Uncontrolled hypertension is a major risk factor for cardiovascular disease (CVD), which is the leading cause of death for American men and women.2 One in three American adults has hypertension, defined as a systolic blood pressure (SBP) ≥140 mmHg or a diastolic blood pressure (DBP) ≥90 mmHg. Notably, 69% of people who have their first heart attack, 77% who have their first stroke, and 74% who have heart failure also have blood pressure greater than 140/90 mmHg.2 While there are some data to suggest that blood pressure that is too low leads to increased cardiac events (known as the J-curve phenomenon), it is also clear that treating high blood pressure leads to a 40% decrease in fatal stroke and prolongs life expectancy.1-3
Treatment of high blood pressure should be relatively simple, considering that there are multiple drugs in 10 different classes that are FDA-approved for hypertension—ranging from diuretics, such as hydrochlorothiazide, approved in 1959, to azilsartan, an angiotensin II receptor blocker (ARB), approved in 2011. However, medications will not work if patients do not take them. In the case of hypertension management, noncompliance leads to uncontrolled blood pressure that, in turn, leads to increased cardiovascular death.4
In clinical trials, compliance with drug therapy is, at best, 78% for patients with chronic conditions.4 In the case of hypertension, compliance with therapy is particularly abysmal because of the side-effect profile of the drugs that are used to treat an otherwise asymptomatic condition.4 The World Health Organization (WHO) estimates that 70% of hypertensive patients do not take antihypertensive medications as prescribed.1 To help improve compliance with blood pressure medications, it has been suggested that shared decision making—a model in which the patient plays an integral role in making decisions about his or her therapy—be adopted in practice. In addition, using drugs that are “more forgiving” with longer half-lives, or developing a simplified drug-dosing regimen, may improve adherence to therapy.4
A meta-analysis performed in 2004 examined the effectiveness of interventions used to increase adherence to blood pressure–lowering medications.5 Of the 38 trials included in the meta-analysis, 19 studies reported an improvement in adherence; seven of these 19 studies showed a decrease in blood pressure along with an improvement in adherence. Of all the interventions examined, simplification of the dosing regimen had the largest impact on improving adherence. The use of once-daily, instead of twice-daily, therapies improved adherence from approximately 8% to 20%.5
Such findings are important for patients who have stage 2 hypertension, defined as SBP ≥160 mmHg or DBP ≥100 mmHg, and for patients who are 20/10 mmHg above their blood pressure goal. For these populations, The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7) recommends treatment with a two-drug combination from the outset.6 In addition, even for individuals who are not categorized as stage 2 hypertensives, it is a fact that most patients will require more than one medication to achieve their blood pressure goal.6 Hence, one method to simplify a potentially complex multiple-drug regimen is to use fixed-dose combination drug therapy.
Benefits of Combination Therapy
Combination therapy in the treatment of hypertension improves both blood pressure and tolerability.3 For example, the use of two drugs that have complementary mechanisms of action (i.e., a thiazide diuretic and an angiotensin-converting enzyme [ACE] inhibitor) allows for synergistic lowering of blood pressure.3 In a meta-analysis of 42 trials published by Wald et al, it was found that combining antihypertensive drugs from two different classes lowered blood pressure five times more than doubling the dose of a single agent.7 In addition to synergistic blood pressure lowering, combination therapy allows for lower dosage requirements of each individual agent. This, in turn leads to decreased side effects,3 thereby improving compliance.
Fixed-dose combination therapy provides another option to improve compliance. Polypharmacy is a determinant of poor medication adherence.8 Therefore, simplification of a medication regimen to a single-dosage form would be expected to improve compliance. This notion was proven to be true in a meta-analysis of nine studies of fixed-dose combinations in the treatment of tuberculosis, hypertension, and HIV.8 In the four hypertension studies included in the meta-analysis, the risk of nonadherence was reduced by 24% in patients who were treated with a fixed-dose combination, rather than with free-drug regimens.8 In addition, fixed-dose combinations were found to be more effective than free-drug combinations in lowering blood pressure, although this finding did not achieve statistical significance.8
In a more recent meta-analysis published in 2010, fixed-dose combinations of antihypertensive agents not only improved compliance by 21%, but also allowed for a 50% increase in persistence with therapy.9
While the benefit of improved compliance is certainly promising, fixed-dose combination products do have some important limitations. First of all, there is no flexibility with the dose of each agent in the product.10 Second, insurance plans may not pay for the single-pill combination, creating an increased cost-burden for the patient,10 which defeats the whole purpose of simplifying therapy. Third, some commercially available combinations may not be safe or practical as first-line therapy in some cases.10 However, the benefit of improved compliance with fixed-dose combination products may outweigh these limitations, making them an important consideration when designing an antihypertensive therapy plan.
Beyond improving compliance, combination therapy in the setting of hypertension management allows for decreased blood pressure variability.11 Variability in SBP is associated with an increased risk of myocardial infarction (MI) and stroke. Evidence suggests that combination therapy, particularly with a calcium channel blocker, diuretic, or ACE inhibitor, is associated with less SBP variability, and therefore improved outcomes.11
The benefit of combination therapy in the treatment of hypertension is clear and is likely necessary for most patients. This begs the question, “Which combination makes the most sense?”
Choice of Combination Therapy
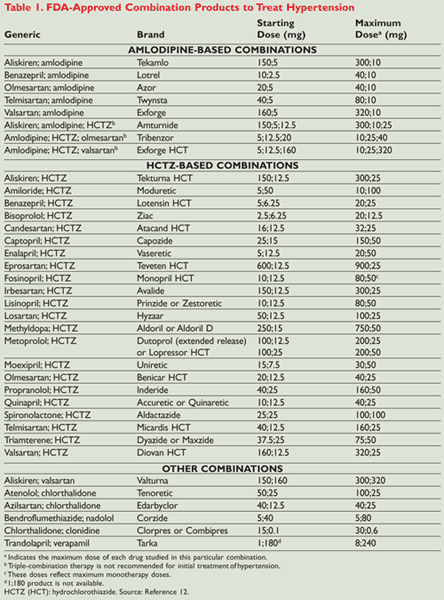
According to the JNC 7 guidelines, the use of a thiazide or thiazide-like diuretic is first-line therapy in most hypertensive patients.6 If the patient has a compelling indication, then treatment decisions are relatively straightforward—patients with diabetes should receive an ACE inhibitor; patients who are post-MI or who have congestive heart failure (CHF) should get a beta-blocker; and so on. Sometimes, however, the decision is not so clear, and careful consideration is required when recommending combination therapy. TABLE 1 provides a list of FDA-approved combination products.12
Renin-Angiotensin-Aldosterone System Inhibitors + Calcium Channel Blockers
ACE inhibitors, ARBs, and direct renin inhibitors (DRIs) inhibit the renin-angiotensin-aldosterone system (RAAS). Dihydropyridine calcium channel blockers (CCBs), such as amlodipine, block the influx of calcium into coronary and systemic arteries, allowing for vasodilation. Together, a RAAS inhibitor and a CCB lower blood pressure additively. Moreover, the addition of an ACE inhibitor to a CCB alleviates peripheral edema associated with the CCB,11 and thus may improve compliance for patients who are bothered by this side effect.
Evidence from the primary literature supports the combination of a RAAS inhibitor with a CCB. In the ACCOMPLISH trial, a fixed-dose of benazepril and amlodipine was superior to the combination of benazepril and hydrochlorothiazide (HCTZ) in reducing cardiovascular events, as well as death, in patients with hypertension.13 In the EX-STAND trial, African-American patients who were given valsartan and amlodipine had improved blood pressure control as compared to patients given amlodipine alone.14 In the ACCELERATE trial, patients who took aliskiren and amlodipine achieved a greater reduction in SBP than patients taking either drug as monotherapy.15 It should be noted that there are no outcome studies with ARB/CCB or DRI/CCB combinations. Regardless, the combination of a RAAS inhibitor with a CCB is a rational and effective choice for use in hypertension.
RAAS Inhibitors + Diuretics
Diuretics decrease volume, which in turn activates the RAAS. This activation leads to vasoconstriction, salt and water retention, and increased blood pressure. Therefore, when added to a thiazide or thiazide-like diuretic, an inhibitor of the RAAS system overcomes these untoward effects and provides additional BP lowering.11 Furthermore, hypokalemia and glucose intolerance, commonly associated with diuretic use, are both alleviated with the addition of a RAAS inhibitor,11 making this a rational combination for hypertensive patients.
Evidence from the LIFE trial supports using an ARB in combination with HCTZ.16 Patients treated with losartan and HCTZ had less cardiovascular death, stroke, and MI compared to those patients who took atenolol and HCTZ.15 Likewise, in the HYVET trial, the combination of perindopril and indapamide significantly reduced stroke and heart failure in an elderly population, as compared to placebo.17 Hypertension experts will note that chlorthalidone is more effective than HCTZ,11 yet most fixed-dose combination products contain HCTZ.
In December 2011, the FDA approved a new product, Edarbyclor, which is a combination of azilsartan and chlorthalidone.18 As clinicians gain more experience with chlorthalidone, practice habits with HCTZ may change.
Other Acceptable Combinations
Diuretics added to beta-blockers may be appropriate in patients with low-renin hypertension (e.g., African-American patients). However, the benefit of this combination, in terms of morbidity and mortality, must be weighed against the risk of glucose intolerance and new-onset diabetes.11
The combination of a CCB with a diuretic is a suitable option, and is supported by data from the VALUE trial. Patients who received the combination of amlodipine and HCTZ tolerated the combination well, and had mortality reduction similar to the valsartan comparator group.11,19 A dihydropyridine CCB and beta-blocker combination might be appropriate in certain circumstances; however, beta-blockers should generally not be combined with diltiazem or verapamil.11 Verapamil or diltiazem in combination with amlodipine is an alternative for patients with a history of angioedema to an ACE inhibitor and for patients at increased risk of hyperkalemia.11 Finally, spironolactone is recommended in addition to a CCB, RAAS inhibitor, and/or thiazide or thiazide-like diuretic, in the case of resistant hypertension.11 In fact, data from the 2011 ASPIRANT study showed that adding spironolactone to patients already on three antihypertensive medications lowered blood pressure significantly, as compared to placebo.20
Unacceptable Combinations
Based on results from ONTARGET, it is clear that dual inhibition of the RAAS is an ineffective, potentially dangerous combination.21 In this study, patients received telmisartan and ramipril. While there was a slight decrease in blood pressure for patients on combination therapy, there was also a significantly increased risk of adverse events such as syncope, hypotension, and renal dysfunction.21
A similar, unfavorable trend was seen in the more recent ALTITUDE trial, which was designed to evaluate the effectiveness of aliskiren in combination with an ACE inhibitor or ARB.22 Because of an increase in nonfatal stroke, renal complications, hyperkalemia, and hypotension, in December 2011 the study was stopped early.22 Given that there is no clear benefit and instead there is evidence of increased harm, dual RAAS inhibition should be discouraged in hypertensive patients.
Combining an inhibitor of the RAAS with a beta-blocker for the purpose of lowering blood pressure in hypertensive patients is also discouraged. While it is certainly true that treatment with an ACE inhibitor and a beta-blocker is life saving for patients with heart failure, or for patients who are post-MI, there is little additional benefit in the lowering of blood pressure when using this combination.11 Similarly, a beta-blocker in combination with clonidine provides no benefit in lowering blood pressure and may actually precipitate rebound hypertension.23
Conclusion
Treatment of hypertension is not an easy task. Compliance with antihypertensive therapy is often low because patients do not feel symptoms related to high blood pressure.1 Since antihypertensives do not necessarily make one feel better and could instead make one feel worse, convincing a patient to adhere to a blood pressure–lowering regimen is difficult.3 However, it is a fact that CVD is the number one preventable cause of death; controlling blood pressure decreases the risk of CVD, thereby decreasing mortality.2 The use of combination therapy by a single-dosage form via rational fixed-dose formulations or by selection of complementary drug classes in the management of hypertension allows patients to achieve their blood pressure goal quickly, improves adverse drug reactions, and is supported by prospective data.
REFERENCES
1. Messerli FH, Williams B, Eberhard R. Essential hypertension. Lancet. 2007;370:591-603.
2. Roger VL, Go AS, Lloyd-Jones DM, et al. Heart disease
and stroke statistics–2012 update: a report from the American Heart
Association. Circulation. 2012;125:e2-e220.
3. Sood N, Reinhart KM, Baker WL. Combination therapy for the management of hypertension: a review of the evidence. Am J Health-Syst Pharm. 2010;67:885-894.
4. Osterberg L, Blaschke T. Adherence to medications. N Engl J Med. 2005;353:487-497.
5. Schroeder K, Fahey T, Ebrahim S. How can we improve adherence to blood pressure-lowering medication in ambulatory care? Arch Intern Med. 2004;164:722-732.
6. Chobanian AV, Bakris GL, Black HR, et al. The Seventh
Report of the Joint National Committee on Prevention, Detection,
Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA. 2003;289:2560-2572.
7. Wald DS, Law M, Morris JK, et al. Combination therapy
versus monotherapy in reducing blood pressure: meta-analysis on 11,000
participants from 42 trials. Am J Med. 2009;122:290-300.
8. Bangalore S, Kamalakkannan G, Parkar S, Messerli F. Fixed-dose combinations improve medication compliance: a meta-analysis. Am J Med. 2007;120:713-719.
9. Gupta AK, Arshad S, Poulter NR. Compliance, safety and
effectiveness of fixed dose combinations of antihypertensive agents, a
meta-analysis. Hypertension. 2010;55:399-407.
10. Epstein BJ. Improving blood pressure control rates by optimizing combination antihypertensive therapy. Expert Opin Pharmacother. 2010;11:2011-2026.
11. Sever PS, Messerli FH. Hypertension management 2011: optimal combination therapy. Eur Heart J. 2011;32:2499-2506.
12. Clinical Pharmacology [online database]. Tampa, FL:
Gold Standard, Inc.; 2011. www.clinicalpharmacology-ip.com. Accessed
March 7, 2012.
13. Jamerson K, Weber MA, Bakris GL, et al. Benazepril plus amlodipine or HCTZ for hypertension in high-risk patients. N Engl J Med. 2008;359:2417-2428.
14. Flack JM, Calhoun DA, Satlin L, et al. Efficacy and
safety of initial combination therapy with amlodipine/valsartan compared
with amlodipine monotherapy in black patients with stage 2
hypertension: the EX-STAND study. J Hum Hypertens. 2009;23:479-489.
15. Brown MJ, McInnes GT, Papst CC, et al. Aliskiren and
the calcium channel blocker amlodipine combination as an initial
treatment strategy for hypertension control (ACCELERATE): a randomized,
parallel-group trial. Lancet. 2011;377:312-320.
16. Dahlof B, Devereaux RB, Kjeldsen SE, et al.
Cardiovascular morbidity and mortality in the losartan intervention for
endpoint reduction in hypertension study (LIFE): a randomized trial
against atenolol. Lancet. 2002;359:995-1003.
17. Beckett NS, Peters R, Fletcher AE, et al. Treatment of hypertension in patients 80 years of age and older. N Engl J Med. 2008;358:1887-1898.
18. FDA approves Edarbyclor (azilsartan medoxomil and
chlorthalidone) for treatment of hypertension. Takeda Pharmaceuticals
North America, Inc. December 20, 2011.
www.tpna.com/newsroom/press_release_detail.aspx?year=2011&id=228.
Accessed January 9, 2012.
19. Julius S, Kjeldsen SE, Brunner H, et al. VALUE trial:
long-term blood pressure trends in 13,449 patients with hypertension and
high cardiovascular risk. Am J Hypertens. 2003;16:544-548.
20. Vaclavik J, Sedlak R, Plachy M, et al. Addition of
spironolactone in patients with resistant arterial hypertension
(ASPIRANT). Hypertension. 2011;57:1069-1075.
21. Yusuf S, Teo KK, Pogue J, et al. Telmisartan, ramipril or both in patients at high risk for vascular events. N Engl J Med. 2008;358:1547-1559.
22. Novartis announces termination of ALTITUDE study with
Rasilez/Tekturna in high-risk patients with diabetes and renal
impairment. Novartis Global Communications. December 20, 2011.
www.novartis.com/newsroom/media-releases/en/2011/1572562.shtml. Accessed
January 9, 2012.
23. Bailey RR, Neale TJ. Rapid clonidine withdrawal with blood pressure overshoot exaggerated by beta-blockade. Brit Med J. 1976;6015:942-943.
To comment on this article, contact rdavidson@uspharmacist.com.






