US Pharm.
2008;33(4):29-34.
Adverse drug reactions are a
potential problem with all medications. One common and very notable result
from drug reactions is skin-related manifestations. These are also called
adverse cutaneous drug reactions (ACDRs). Some of the ACDRs include
exanthematous reactions, Stevens-Johnson syndrome, toxic epidermal necrolysis,
urticaria, and photosensitivity. While it is true that these effects can occur
with several types of medications, this article will focus on commonly
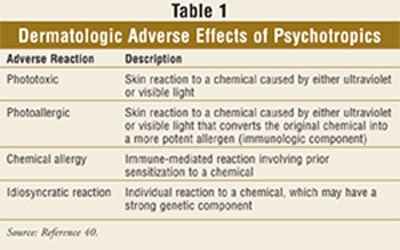
reported ACDRs associated with psychotropics (TABLE 1).
Exanthematous Reactions
Morbilliform or
maculopapular (with flat regions and elevated bumps) eruptions are the most
common type of ACDR.1,2 They are characterized by symmetrically
distributed erythematous macules (flat lesions) and papules (raised bumps)
that originate in the trunk and spread to the extremities.1-3 The
reaction can appear in a few days or in the course of several weeks. One
common symptom is fever.2
Presentation may be unique to
some of the medications. In the case of hydantoin derivatives (i.e.,
phenytoin), there is macular erythema spreading from the face to the trunk and
then to the extremities during the first two weeks of treatment.2,3
Additionally, patients may experience fever, lymphadenopathy, and facial edema.
3 This combination of symptoms is commonly referred to as the "phenytoin
hypersensitivity syndrome."2 If it is not recognized early, it
can lead to enlargement of the liver and spleen and elevation in hepatic
enzymes.4
With phenothiazines,
erythematous macules and small papules appear within the first three weeks of
treatment, spreading from the face to the trunk and then to the extremities;
usually periorbital edema is present.2 In the case of barbiturates,
a diffuse macular eruption is seen, spreading from the face to the extremities
in the first few days of treatment.2 Dispersed erythema, spreading
from the face to the rest of the body, is seen with carbamazepine, usually
after two weeks of treatment.3 Facial edema is also seen with
carbamazepine.3
Case reports with other drugs,
including exanthematous reactions with olanzapine, have been published.5
Discontinuation of the offending agent is the most common treatment option
for exanthematous reactions.
Angioedema and Urticaria
Angioedema and urticaria (hives) are
cutaneous adverse reactions that can occur with any drug. Angioedema involves
swelling of subcutaneous tissues, usually in the face, tongue, extremities,
and larynx, which could be fatal.1 Urticaria presents as round,
red, swollen lesions generally associated with pruritus (itching) that can
appear anywhere on the skin.1 Because these reactions can occur
with all medications, no particular presentation or higher frequency can be
attributed to any specific psychotropic agent.
Photosensitivity
Photosensitivity requires photon
energy absorption (sun exposure) by molecules, which can lead to energy
distribution without any effect or to reactions that can result in damage at
the molecular, cellular, and tissue level.6 There are two different
types of photoreactions to medications: photoallergy and
phototoxicity.1,2 Phototoxicity may present with
erythema, edema, and hyperpigmentation one to two days after treatment
initiation.1,2 Photoallergy is characterized by either itchy
red lesions, swollen itchy areas, or blisterlike lesions and may present
within the first few weeks after starting therapy.1,2 One important
differentiation is the onset of the lesions. Phototoxicity can occur in anyone
after intake of the medication, but only patients who have undergone
sensitization (production of antibodies) can have a photoallergic reaction.
2
Prevention is essential and
can involve avoiding sun exposure, the use of topical sunscreens, and, if
needed, discontinuation of the medication. Additionally, patients may be
treated according to the severity of the skin lesions. These treatments
include wet dressings and topical glucocorticoids; in the case of toxicity,
hospitalization may be required.3
Several psychotropics have
been associated with photosensitivity, including chlorpromazine and
thioridazine, particularly at doses above 400 mg/day.7 Fluoxetine
can produce a painful, burning, and persistent erythema after sun exposure; a
patient may experience this even after being on the same dose for years.8
Additional reports have suggested photosensitivity reactions with risperidone
and alprazolam.9,1
Pigmentation Reactions
Pigmentation
reactions can be a result of stimulation of melanin production by the
medication, pigment deposits by either the drug or its metabolite, or both.
2,11 Phenothiazines are the most common group of psychotropic
medications associated with pigmentary reactions. The individual agent most
commonly associated with this is chlorpromazine. Chlorpromazine can cause a
blue or slate gray pigmentation, particularly on surfaces that have had sun
exposure.12 This discoloration can also appear in the lens and the
cornea.1 Imipramine, trifluopherazine, and olanzapine have also
been reported to cause hyperpigmentation.13-15
The discoloration produced by
these medications can take several weeks, months, or even years to clear, and
in some instances it might never go away.2 Usually the causative
agent needs to be removed for the discoloration to clear. In one particular
report of four cases of imipramine-induced skin pigmentation, those treated
with creams, laser therapy, and tretinoin without removal of imipramine (n =
2) continued showing the discoloration. For those in which imipramine was
removed (n = 2), the discoloration eventually cleared.16
Stevens-Johnson Syndrome
and Toxic Epidermal Necrolysis
Stevens-Johnson
syndrome (SJS) and toxic epidermal necrolysis are two very serious and
potentially life-threatening ACDRs. Stevens-Johnson syndrome is
characteristically preceded by a prodrome of fever and other flulike symptoms,
followed by inflammation of the mucosal surfaces of the mouth and conjunctiva.
1 Additionally, macules that are dark red and may have a necrotic center
can be seen. If skin detachment reaches more than 30% of the skin surface, the
condition is called toxic epidermal necrolysis.17 Toxic epidermal
necrolysis carries a higher risk of death than SJS, primarily due to sepsis.
1,2 The treatment involves drug removal, IV fluids, and systemic
glucocorticoids.3
Stevens-Johnson syndrome has
been reported with several anticonvulsants or mood stabilizers, including
valproic acid, carbamazepine, and lamotrigine.17-19 With long-term
medications, the increased risk of rash occurs during the first two months of
therapy.17 The mood stabilizers more commonly associated with this
rash are carbamazepine and lamotrigine. The manufacturers of both of these
products have had to provide boxed warnings for the increased risk of rash.
The incidence of serious rash
(including SJS) with lamo!= trigine when used for adjunctive treatment of
epilepsy is 0.8% (8/1,000) in pediatric patients and 0.3% (3/1,000) in adults.
In adults being treated for bipolar disorder with lamotrigine, the incidence
of serious rash is 0.08% (0.8/1,000) when the medication was used as initial
monotherapy and 0.13% (1.3/1,000) when lamotrigine was used as an adjunct.
20 The combination of valproic acid with lamotrigine can increase the
risk for serious rash.20,21
Carbamazepine's incidence of
severe rash is approximately six in every 10,000 new drug users; these data
are from countries with primarily Caucasian populations.22 However,
in Asian countries, the incidence could be ten times higher.22
Recently, the FDA issued a statement in which it recommended that companies
manufacturing carbamazepine include in their labeling a recommendation for
genetic testing of the HLA-B*1502 allele, a human leukocyte antigen, in people
of Asian descent.23 Studies have shown the prevalence of this
allele to correlate with a higher incidence of severe skin reaction with
carbamazepine in the Asian population.
Chung et al conducted a study
in which they genotyped for several CYP450 enzymes as well as several human
leukocyte antigens.24 A total of 238 Han Chinese were screened; 44
had developed rash with carbamazepine, 101 were on carbamazepine but had
developed no rash, and 93 were normal subjects. The researchers found that
100% of the patients who developed rash with carbamazepine were positive for
the HLA-B*1502 allele.
These results were replicated
again, but with lower numbers, by Man et al.25 In this study, the
authors noted that eight patients (all Han Chinese) taking antiepileptic
medications developed a severe cutaneous reaction, which could not be
attributed to anything else, eight weeks after starting the medication. Of
these eight patients, four were taking carbamazepine and 100% of them were
positive for HLA-B*1502. In addition, two more patients were positive for
HLA-B*1502; one of them was taking phenytoin and the other was taking
lamotrigine.
Additional cases of SJS or
toxic epidermal necrolysis have been reported with other drugs, including
zonisamide and chlorpromazine.26,2
Acne
Acneiform reactions
usually present as papules and pustules (small, elevated skin lesions filled
with white blood cells), generally appearing on the face, upper back, and
chest.1,2 Lithium has been associated with severe acneiform
eruptions; more recently, lamotrigine has been reported to have caused
acneiform eruptions as well.28,29
Alopecia
Drug-induced hair
loss primarily affects the scalp,† although the hair loss is usually
reversible. Mood stabilizers are thought to precipitate follicles into a rest
phase leading to telogen effluvium.1,30 Telogen is the final stage
of hair growth before it starts to fall.30 Alopecia has been more
commonly reported with valproic acid and lithium.30,31 Hair loss
has also been reported with lamotrigine, venlafaxine, fluoxetine,
and paroxetine.32-35 The effects can appear after years of
treatment. While discontinuation of treatment is the common option, one report
indicated cessation of hair loss and new hair growth occurring without
stopping the medication.30
Fixed-Drug Eruptions
Fixed-drug
eruptions are drug-mediated reactions that can be characterized by rapidly
appearing lesions after intake, which can be small or large in size and
quantity; they are red and may blister or give a burning sensation.
Characteristically, they disappear after drug removal, but in the case of
rechallenge, they appear in the same surface areas as the first time.1-3
Carbamazepine and temazepam have been reported to have caused this type of
ACDR.36,37
Lichenoid Reactions
Lichen planus is an
inflammatory idiopathic condition of the skin characterized by pruritic
"reddish-purple, flat-topped bumps."38 Certain
medications can produce a lichenoid-type eruption. The manifestations of this
reaction can take several months to appear, manifest primarily in the trunk
and extremities, and usually avoid the mucosa and genitalia, which is unlike
lichen planus.1,2 Lichenoid-type eruptions have been reported with
carbamazepine.39
Conclusion
While there may be
additional types of ACDRs, the most common associated with psychotropics have
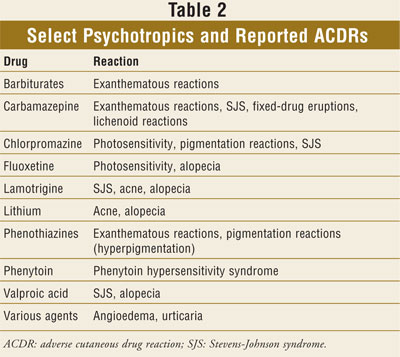
been reviewed here (TABLE 2). What is important to note is that these
reactions can occur with several psychotropics, and they may cause discomfort
or present a danger to the patient. Therefore, it is important to be aware not
only of their existence, presentation, and treatment, but also the fact that
while they usually appear early in treatment, they may also appear after
chronic and consistent dosing.
REFERENCES
1. Kimyai-Asadi A,
Harris JC, Nousari HC. Critical overview: adverse cutaneous reactions to
psychtropic medications. J Clin Psychiatry. 1999;60:714-725.
2. Garnis-Jones S.
Dermatologic side effects of psychopharmacologic agents. Dermatol Clin.
1996;14:503-508.
3. Wolff K, Johnson RA,
Suurmond D. Part 2, Section 20. In: Fitzpatrick Color Atlas & Synopsis of
Clinical Dermatology. 5th ed. New York, NY: McGraw-Hill; 2005:542-572.
4. Bongard FS, Sue DY,
eds. Current Critical Care Diagnosis and Treatment. 2nd ed. New York,
NY: McGraw-Hill; 2003.
5. Christen S, Gueissaz
F, Anex R, Zullino DF. Acute generalized exanthematous pustulosis induced by
olanzapine. Acta Medica (Hredec Kralove). 2006;49:75-76.
6. Wolff K, Johnson RA,
Suurmond D. Part 1, Section 10. In: Fitzpatrick Color Atlas & Synopsis of
Clinical Dermatology. 5th ed. New York, NY: McGraw-Hill; 2005:226-266.
7. Satanove A, McIntosh
JS. Phototoxic reaction induced by high dose chlorpromazine and thioridazine.
JAMA. 1967;200:209-212.
8. Gaufberg E, Ellison
JM. Photosensitivity reaction to fluoxetine. J Clin Psychiatry.
1995;56:486.
9. Almond DS, Rhodes
LE, Pirmohamed M. Risperidone-induced photosensitivity. Postgrad Med J.
1998;74:252-253.
10. Watanabe Y, Kawada
H, Ohnishi Y, et al. Photosensitivity due to alprazolam with positive oral
photochallenge after 17 days administration. J Am Acad Dermatol.
1999;40:832-833.
11. Granstein RD, Sober
AJ. Drug- and heavy-metal induced hyperpigmentation. J Am Acad Dermatol
. 1981;5:1-18.
12. Lal S, Lal S.
Chlorpromazine-induced cutaneous pigmentation--effect of replacement with
clozapine. J Psychiatry Neurosci. 2000;25:281.
13. Angel TA, Stalkup
JR, Hsu S. Photodistributed blue-gray pigmentation of the skin associated with
long-term imipramine use. Int J Dermatol. 2002;41:327-329.
14. Buckley C, Thomas
V, Lewin J, et al. Stelazine-induced pigmentation. Clin Exp Dermatol.
1994;19:149-151.
15. Jhirwal OM, Parsad
D, Basu D. Skin hyperpigmentation induced by olanzapine, a novel antipsychotic
agent. Int J Dermatol. 2004;43:779-780.
16. Ming ME, Bhawan J,
Stefanato CM, et al. Imipramine-induced hyperpigmentation: four cases and
review of the literature. J Am Acad Dermatol. 1999;40:159-166.
17. Roujeau JC, Kelly
JP, Naldi L, et al. Medication use and the risk of Stevens Johnson syndrome or
toxic epidermal necrolysis. N Engl J Med. 1995;333:1600-1607.
18. Tsai SJ, Chen YS.
Valproic acid-induced Stevens Johnson syndrome. J Clin Psychopharmacol.
1998;18:420.
19. Hilas O, Charneski
L. Lamotrigine induced Stevens-Johnson syndrome. Am J Health Syst Pharm
. 2007;64:273-275.
20. Lamictal
(lamotrigine) package insert. Research Triangle Park, NC: GlaxoSmithKline; May
2007.
21. Kocak S, Girisgin
SA, Gul M, et al. Stevens-Johnson syndrome due to concomitant lamotrigine and
valproic acid. Am J Clin Dermatol. 2007;8:107-111.
22. Equetro
(carbamazepine) package insert. Parsippany, NJ: Validus Pharmaceuticals, Inc;
December 2007.
23. FDA. Carbamazepine
prescribing information to include recommendation of genetic test for patients
with Asian ancestry. December 12, 2007.
www.fda.gov/bbs/topics/NEWS/2007/NEW01755.html. Accessed February 8, 2008.
24. Chung WH, Hung SI,
Hong HS. Medical genetics: a marker for Stevens-Johnson syndrome. Nature
. 2004;428:486.
25. Man CB, Kwan P,
Baum L, et al. Association between HLA-B*1502 allele and antiepileptic drug
induced cutaneous reactions in Han Chinese. Epilepsia.
2007;48:1015-1018.
26. Majeres KD, Suppes
T. A cautionary note when using zonisamide in youths: a case report of
association with toxic epidermal necrolysis. J Clin Psychiatry.
2004;65:1720.
27. Purcell P, Valwana
A. Toxic epidermal necrolysis following chlorpromazine ingestion complicated
by SIADH. Postgrad Med J. 1996;72:186.
28. Ruiz-Maldonado R,
Perez de Francisco C, Tamayo L. Lithium dermatitis. JAMA.
1973;224:1534.
29. Nielsen JN, Licht
RW, Fogh K. Two cases of acneiform eruption associated with lamotrigine. J
Clin Psychiatry. 2004;65:1720-1722.
30. McKinney PA,
Finkenbine RD, DeVane CL. Alopecia and mood stabilizer therapy. Ann Clin
Psychiatry. 1996;8:183-185.
31. Yassa R. Hair loss
during lithium therapy. Am J Psychiatry. 1986;143:943.
32. Hillemacher T,
Bleich S, Kornhuber J, Frieling H. Hair loss as a side effect of lamotrigine
treatment. Am J Psychiatry. 2006;163:1451.
33. Pitchot W, Ansseau
M. Venlafaxine-induced hair loss. Am J Psychiatry. 2001;158:1159-1160.
34. Bhatara VS, Gupta
S, Freeman JW. Fluoxetine-associated paresthesias and alopecia in a woman who
tolerated sertraline. J Clin Psychiatry. 1996;57:227.
35. Zalsman G, Sever J,
Munitz H. Hair loss associated with paroxetine treatment: a case report.
Clin Neuropharmacol. 1999;22:246-247.
36. Shuttleworth D,
Graham-Brown R. Fixed drug eruption due to carbamazepine. Clin Exp Dermatol
. 1984;9:424-426.
37. Archer CB, English
JS. Extensive fixed drug eruption induced by temazepam. Clin Exp Dermatol
. 1988;13:336-338.
38. American Academy of
Dermatology. Lichen planus. www.aad.org/public/publications/
pamphlets/common_lichen.html. Accessed February 13, 2008.
39. Atkin SL, McKenzie
TM, Stevenson CJ. Carbamazepine induced lichenoid eruption. Clin Exp
Dermatol. 1990;15:382-383.
40. Brunton L, Lazo J,
Parker K. Goodman & Gilman's The Pharmacological Basis of Therapeutics.
11th ed. New York, NY: McGraw-Hill; 2006.
To comment on this article, contact
rdavidson@jobson.com.





