US Pharm. 2016;41(8):13-14.
Intense Thirst and Excessive Urination
Diabetes insipidus is a condition with the hallmark symptoms of intense thirst and excessive urination. These symptoms are a result of abnormal regulation of the fluids in the body. This can occur due to damage to the pituitary gland, hypothalamus, or kidneys. In some cases, no cause can be identified. Diagnosis is made using a combination of symptom history and results from blood and urine tests. Treatment is aimed at correcting the underlying cause if possible, and ensuring enough fluid intake to restore the balance of fluids and electrolytes. If left untreated, complications of diabetes insipidus include dehydration or an imbalance of sodium, potassium, or other electrolytes in the body.
Condition Is Not Related to Diabetes Mellitus
Diabetes insipidus is a relatively rare condition. It is not related to diabetes mellitus, although they share the symptoms of excess thirst and urination.
Causes
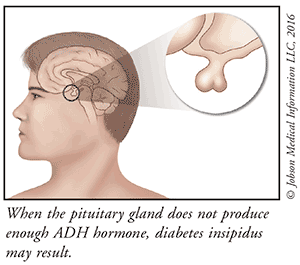
In the body, the kidneys constantly filter the blood, removing water and producing urine. The kidneys are responsible for maintaining a healthy concentration of water in both the urine and blood. This action of the kidneys is controlled by a hormone know as ADH (antidiuretic hormone). ADH is produced in the part of the brain known as the hypothalamus. ADH is stored in the pituitary gland, an organ at the base of the brain. When ADH is released into the bloodstream, the kidneys respond by filtering the correct amount of water from the blood, resulting in the proper balance of fluids and electrolytes in the body. Diabetes insipidus can usually be traced to a problem somewhere in this delicately balanced system.
Sometimes the hypothalamus does not produce enough ADH, or the pituitary gland does not release enough ADH into the bloodstream. This lack of ADH causes central diabetes insipidus. Central diabetes insipidus can be the result of a tumor, head trauma, or infection. The kidneys might not respond correctly to ADH after it is released in the bloodstream, possibly from a drug like lithium or a disease of the kidney. When the kidneys are the cause, the condition is called nephrogenic diabetes insipidus. Gestational diabetes insipidus can occur during a pregnancy when ADH in the mother is destroyed by an enzyme from the placenta.
Symptoms
Diabetes insipidus can develop at any age. Symptoms of diabetes insipidus are primarily excessive thirst, caused by the production of up to five times the normal amount of urine in a day. This excessive urination can lead to multiple trips to the bathroom at night, and can cause nighttime bedwetting. Babies and children with the condition may cry excessively and have trouble sleeping through the night. Less common symptoms in children include vomiting, diarrhea, and fever.
The diagnosis of diabetes insipidus is made using a patient’s history of excess thirst and frequent urination, along with blood tests to check electrolyte levels and urine tests to measure the urine concentration. A fluid deprivation test, which measures urine volume and body weight when fluids are withheld, can help determine the cause of diabetes insipidus. Some patients may require an MRI of the brain to confirm the source of the problem.
Treatment Options
Treatment for diabetes insipidus depends on the cause. Sometimes the cause of this condition can be treated, such as removal of a tumor affecting the hypothalamus or pituitary gland. If symptoms are mild, simply increasing water intake may be the only treatment needed.
In cases of central diabetes insipidus, a synthetic form of ADH (desmopressin) may be prescribed. Desmopressin is available as an injection, tablet, or nose spray. If poor kidney function is causing the condition, a low salt diet and adequate water may be part of the treatment plan, along with a diuretic (water pill) or an anti-inflammatory medication. If diabetes insipidus is caused by a drug such as lithium, the drug may be discontinued to see if kidney function improves.
Patients with diabetes insipidus should be monitored frequently to ensure their treatment plan is working. It is very important to contact a healthcare professional at the first sign of increased thirst or urination so therapy can be adjusted to avoid dehydration or an electrolyte imbalance.
To comment on this article, contact rdavidson@uspharmacist.com.






