US Pharm. 2011;36(5):HS-15-HS-26.
Chest pain is a common occurrence in primary, acute, and urgent care settings, and it is one of the most cited reasons for which people seek medical attention.1 Chest pain accounts for an estimated 5% of all emergency department visits and 1% to 2% of outpatient visits.2-4 Additionally, chest pain is a leading cause of hospital admission and a common complaint in the acute care setting.5
SIGNIFICANCE OF CHEST PAIN
Chest pain has varied etiologies, from life-threatening conditions to benign pathologies and simple muscle strains. A broad differential diagnosis is necessary, leading to challenges in the evaluation and management of chest pain. Additionally, the assessment of chest pain is complicated by the disassociation between the intensity of the signs and symptoms and the seriousness of the underlying cause of chest pain, as well as by the often vague presentation and indistinct localization of the pain.1,2
In general, pain is a complex, subjective experience. Visceral pain, including chest pain, is difficult to localize, diffuse in character, and usually referred to somatic structures.1,2 Visceral pain is also associated with more autonomic and motor responses than somatic pain. Specifically, chest pain is usually characterized by an unpleasant sensation localized to the thorax.1 Descriptions of chest pain vary widely, involving terms like “burning,” “aching,” “stabbing,” or “pressure.”2
One of the most significant factors in the appraisal of chest pain is the distinction between cardiac and noncardiac chest pain. It is often difficult to discriminate between these two types of pain, and patients may have simultaneous cardiac and noncardiac causes.6,7 Noncardiac causes are common, but cardiac causes must not be overlooked, since cardiac chest pain may be an indicator of cardiovascular disease (CVD).4 Heart disease remains the leading cause of death in the United States; each year, 36% of deaths (roughly 870,000 cases) in the U.S. are attributed to CVD.2-4 In 2009, the direct and indirect costs of CVD totaled more than $165 billion in the U.S.3 Early detection of cardiac chest pain and early intervention are critical for decreasing the morbidity and mortality associated with CVD.8
EVALUATING CHEST PAIN
A thorough medical history and physical examination are essential in the evaluation of chest pain.2,3 In order to recognize patients in need of prompt and potentially life-saving intervention, the National Heart Attack Alert Program recommends the immediate assessment of patients with the following symptoms: chest pain, pressure, tightness, or heaviness, or pain that radiates to the neck, jaw, shoulders, back, or arms; indigestion, heartburn, or nausea and/or vomiting associated with chest pain; persistent shortness of breath; or weakness, dizziness, lightheadedness, or loss of consciousness.6
If the symptoms do not warrant immediate intervention for life-threatening causes, the initial evaluation should include a medical history that emphasizes the characteristics and location of the pain, time of pain onset, activity at time of onset, duration of symptoms, alleviating or aggravating factors, history of prior pain, presence of risk factors, and other associated symptoms.1,2,4,6 Coronary risk factors should also be evaluated, as well as the possibility of illegal drug use.6 Common risk factors for coronary artery disease (CAD) include advanced age, male gender, family history of CAD, and comorbid illnesses such as diabetes mellitus, hypertension, hypercholesterolemia, and tobacco use.3,9
In addition to a medical history and physical examination, most adults with chest pain should have an ECG and a chest radiograph, unless an obvious non–life-threatening cause of chest pain is determined in the initial investigation.2,4 Also, blood markers for myocardial injury, decision aids to stratify patients according to their risk of complications, early exercise testing, and various imaging techniques and clinical pathways provide enhanced accuracy and efficiency of chest pain evaluation. For patients with a low risk of complications or CVD, the benefit of further testing and evaluation must be balanced against the costs and inconvenience that accompany tests and procedures with a low probability of improving outcomes and a risk of false-positive results.6
MANAGEMENT OF CHEST PAIN
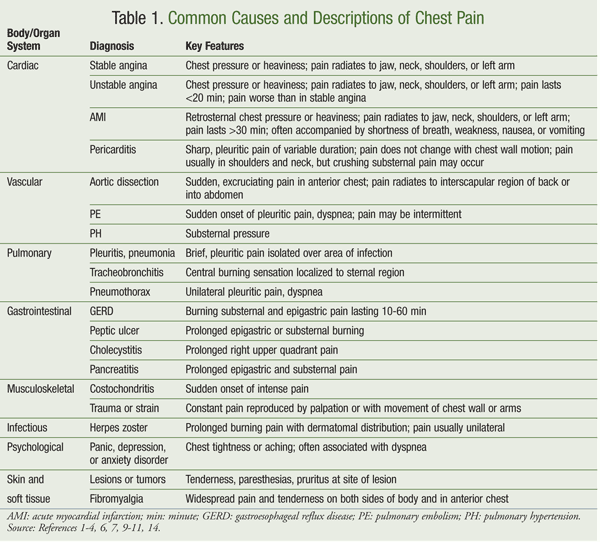
Common causes of chest pain and their descriptions are listed in TABLE 1. The goal of chest pain management, as with all pain control, is to find the cause and treat it appropriately, with the right medication at the lowest effective dose with the fewest possible side effects.1,10 The general principles of respiratory, cardiac, musculoskeletal, gastrointestinal (GI), and psychological disorders apply to the treatment of both cardiac and noncardiac chest pain.1,7,10
Cardiac Chest Pain
Several life-threatening causes of chest pain require immediate attention and must be ruled out before other causes can be determined. These conditions include acute coronary syndrome (ACS), pulmonary embolism (PE), and aortic dissection.1-3,9 ACS is the most significant potentially fatal diagnosis of chest pain.2 Fifteen percent to 25% of patients who present with chest pain are diagnosed with ACS, a broad diagnosis that includes any condition that results in myocardial ischemia, ranging from unstable angina to acute myocardial infarction (AMI). Myocardial ischemia usually occurs in the presence of coronary atherosclerosis, but ischemia may accompany any disease or process that occludes a coronary artery or decreases myocardial perfusion, such as a thrombus or embolism, aortic stenosis, or cardiomyopathy.6
Angina, the classic manifestation of myocardial ischemia, is usually described as heavy chest pressure or a squeezing or burning sensation and is often accompanied by difficulty breathing. Angina often radiates to the left shoulder, neck, or arm and builds in intensity over a period of several minutes.6 While exercise or psychological stress can trigger angina, the condition most commonly occurs without obvious precipitating factors.3,6 The typical presentation includes pain that is substernal, provoked by exertion, and relieved by rest or nitroglycerin.3,4 Anginal chest pain indicates a high risk of CAD.4
An atypical presentation of chest pain lessens the likelihood that the chest pain is due to ischemia. The American College of Cardiology and American Heart Association (ACC/AHA) guidelines list several descriptors that are not characteristic of myocardial ischemia: pleuritic pain (sharp pain caused by respiratory movements or cough); pain or discomfort located primarily in the middle or lower abdomen; pain localized to the tip of one finger; pain reproduced with movement or by palpation of the chest wall or arms; constant pain persisting for many hours; brief pain lasting a few seconds; and pain that radiates to the lower extremities.6 However, atypical symptoms cannot rule out the presence of ACS and should be only one consideration in the diagnosis of chest pain.6,8,11
Oxygen supplementation is routine for all patients with chest pain related to ACS. It is recommended for all AMI patients during the first 6 hours after symptom onset, and longer if other disease states causing hypoxemia are present.9 Also, in patients presenting with chest pain consistent with ACS, aspirin should be administered as soon as possible and continued indefinitely if no aspirin allergy exists. Clopidogrel should be substituted in the case of an aspirin allergy or GI intolerance.9,12
Glycoprotein IIb/IIIa inhibitors block platelet aggregation and are recommended for patients with unstable angina and non–ST-elevation myocardial infarction.9,12 Currently available agents include abciximab, tirofiban, and eptifibatide.8 Additionally, the ACC/AHA guidelines recommend anticoagulation with unfractionated heparin (UFH) or low-molecular-weight heparin (LMWH) added to antiplatelet therapy for the treatment of ACS.12 Currently available LMWHs include enoxaparin, dalteparin, and tinzaparin.8 UFH should be adjusted to maintain a partial thromboplastin time of 1.5 to 2.0 times control.9 LMWH is an alternative to UFH in patients younger than 75 years with stable renal function; LMWH is preferred over heparin as an anticoagulant in the absence of renal failure.9,12
Nitroglycerin, the cornerstone of antianginal treatment, provides symptom relief in patients with ongoing cardiac chest pain.9,11 Morphine may also be used to control pain in AMI patients, but should be administered cautiously at low doses.9 Also, IV or oral beta-blockers should be given to AMI patients without a contraindication to such treatment, such as ST-elevation myocardial infarction and moderate left ventricular failure, or bradycardia, hypotension, shock, active asthma, or reactive-airway disease.8,9
Acute aortic dissection is the most common and most lethal aortic emergency, and it has the highest mortality rate among life-threatening causes of chest pain.9 Acute aortic dissection causes the sudden onset of excruciating, ripping pain whose location reflects the site and progression of dissection.6,9 Aortic dissection may also present with stroke, heart failure, syncope, lower-extremity pain or weakness, back and flank pain, and abdominal pain.9
Aortic dissection usually occurs in the presence of risk factors such as hypertension, pregnancy, atherosclerosis, illegal drug use, connective-tissue disease, and conditions that lead to the degeneration of aortic tissue.6,9,11 Aortic dissection is treated by eliminating factors that are favorable to the progression of dissection, including elevated blood pressure. Appropriate interventions include sodium nitroprusside administered IV to achieve a systolic blood pressure between 100 and 120 mmHg, and oral or IV beta-blockers to avoid reflex tachycardia secondary to sodium nitroprusside. Prompt surgical consultation is recommended for patients with suspected aortic dissection.9
The annual incidence of PE is estimated to be 200 cases per million people.10 The mortality rate for untreated PE is 18.4%, accounting for up to 200,000 deaths annually in the U.S.9,11 PE often causes dyspnea and pleuritic chest pain, but PE may be asymptomatic. Larger emboli cause severe and persistent substernal pain, whereas smaller emboli cause lateral pleuritic chest pain.6 Anticoagulant therapy with UFH, LMWH, or fondaparinux effectively reduces mortality in PE.11
Noncardiac Chest Pain
Noncardiac chest pain may be caused by musculoskeletal disorders, abnormalities of the abdominal viscera, and psychological conditions, among other anomalies.6,13 Even more than cardiac chest pain, noncardiac chest pain is difficult to define, diagnose, and manage.1,14
Approximately 20% to 30% of patients with chest pain are classified as having noncardiac chest pain based on normal findings of cardiac catheterization or other diagnostic evaluations. Each year, approximately 200,000 new cases of noncardiac chest pain occur in the U.S.14 Morbidity among noncardiac chest pain patients is considerable, and these patients tend to have a high use of health care services and empiric therapies and report a general dissatisfaction with care received.7,14
Respiratory and pleuropulmonary disorders are common causes of noncardiac chest pain. Pleuritis and pleural effusions occur frequently in connective-tissue diseases, and the pain is often relieved by nonsteroidal anti-inflammatory drugs (NSAIDs); corticosteroids may reduce inflammation in patients who remain symptomatic after NSAID treatment. Pneumonia frequently presents with chest pain localized over the area of infection. Pneumonia treatment is based on antimicrobial therapy guided by local surveillance reports.10
GI disorders are a common source of noncardiac chest pain. Gastroesophageal reflux disease (GERD), one of the most common causes of noncardiac chest pain, presents with pain resembling angina.14 GERD may be associated with a squeezing or burning type of substernal pain that radiates to the neck, back, or arms.6,14 The pain is generally worse after meals and in the supine position, and exercise and emotional stress can precipitate GERD-associated pain.11 GERD has been reported in as many as 60% of people with chest pain.13,14
Chest pain associated with GERD is manageable, most often with a proton pump inhibitor. Additionally, weight loss is recommended for overweight or obese patients with GERD and noncardiac chest pain. Other lifestyle modifications, including avoiding trigger foods and raising the head of the bed, may not completely relieve chest pain associated with GERD.14
Psychological factors are significant in the diagnosis and management of chest pain. Approximately 30% of patients with noncardiac chest pain experience panic or anxiety disorders.13 There is a high rate of anxiety and depression among patients with cardiac and noncardiac chest pain, so the pain should not be immediately attributed to psychological factors before organic etiologies are ruled out.15 Treatment of psychogenic causes of chest pain is not specific to chest pain and includes cognitive behavioral therapy and anxiolytic and antidepressant therapy.7
Musculoskeletal conditions are the cause in 25% to 35% of patients with noncardiac chest pain.13 Chest pain reproducible by palpation is most likely musculoskeletal in origin. One common cause of noncardiac chest pain is costochondritis, the inflammation of a rib or cartilage attached to a rib. This condition is relieved by analgesics, local anesthetics, or anti-inflammatory agents. Infectious diseases such as herpes zoster may also cause diffuse chest pain. The pain usually resolves once the infection is adequately treated with antiviral agents.7
Treatment
With a broad differential diagnosis, a definitive cause is not always established for chest pain, and continued evaluation is often the best course.2 In the absence of a definitive diagnosis, systemic analgesia for chest pain is appropriate. First-line analgesics, including acetaminophen and NSAIDs, may be used safely for mild pain in most patients. Opioids and adjuvant analgesics may be added if first-line therapy does not relieve the pain. Doses of analgesic agents should be adjusted individually based on level of pain, medication history, and allergies.7,8
Appropriate evaluation and management of chest pain, whether its origin is cardiac or noncardiac, involves treating the underlying cause of the pain while improving patient outcomes and minimizing drug interactions and adverse events. For patients in the acute care setting, chest pain may occur as part of the symptoms or sequelae that require attention and pharmacologic management.8
ROLE OF THE PHARMACIST
Pharmacists are well positioned to provide comprehensive management of multiple disease states to improve quality of life, reduce chest pain recurrence, and minimize complications. Pharmacists should review medications and make recommendations to prescribers based on the best available evidence. Since the pace of clinical research is rapid, pharmacists must be vigilant about being up-to-date on current evidence-based recommendations and act on those recommendations in clinical practice. Pharmacists also play an important role in educating patients about their medications and reinforcing lifestyle modifications as part of comprehensive treatment. Acute care pharmacists can facilitate a smooth transition to the community setting for patients who will remain on chronic therapy for conditions causing chest pain. By improving medication therapy management and optimizing quality of care, pharmacists are important members of the multidisciplinary health care team.8
REFERENCES
1. Lee-Chiong T, Gebhart GF, Matthay RA. Chest pain. In: Mason RJ, Broaddus VC, Martin T, et al, eds. Murray and Nadel’s Textbook of Respiratory Medicine. 5th ed. Philadelphia, PA: Saunders Elsevier; 2010.
2. Brown JE, Hamilton GC. Chest pain. In: Marx JA, Hockberger RS, Walls RM, et al, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 7th ed. Philadelphia, PA: Mosby Elsevier; 2009.
3. Jones ID, Slovis CM. Pitfalls in evaluating the low-risk chest pain patient. Emerg Med Clin North Am.
4. Cayley WE Jr. Diagnosing the cause of chest pain. Am Fam Physician. 2005;72:2012-2021.
5. Karnath B, Holden MD, Hussain N. Chest pain: differentiating cardiac from noncardiac causes. Hosp Physician. 2004;40:24-27,38.
6. Cannon CP, Lee TH. Approach to the patient with chest pain. In: Libby P, Bonow RO, Mann DL, Zipes DP, eds. Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine. 8th ed. Philadelphia, PA: Saunders Elsevier; 2007.
7. Yelland M, Cayley WE Jr, Vach W. An algorithm for the diagnosis and management of chest pain in primary care. Med Clin North Am. 2010;94:349-374.
8. DiPiro JP, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 7th ed. New York, NY: McGraw-Hill Medical; 2008.
9. Haro LH, Decker WW, Boie ET, Wright RS. Initial approach to the patient who has chest pain. Cardiol Clin. 2006;24:1-17,v.
10. Brims FJ, Davies HE, Lee YC. Respiratory chest pain: diagnosis and treatment. Med Clin North Am.
11. Woo KM, Schneider JI. High-risk chief complaints I: chest pain—the big three. Emerg Med Clin North Am. 2009;27:685-712,x.
12. Braunwald E, Antman EM, Beasley JW, et al. ACC/AHA guideline update for the management of patients with unstable angina and non-ST-segment elevation myocardial infarction—2002: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on the Management of Patients With Unstable Angina). Circulation.
13. Ruigómez A, Massó-González EL, Johansson S, et al. Chest pain without established ischaemic heart disease in primary care patients: associated comorbidities and mortality. Br J Gen Pract. 2009;59:e78-e86.
14. Oranu AC, Vaezi MF. Noncardiac chest pain: gastroesophageal reflux disease. Med Clin North Am.
15. Eken C, Oktay C, Bacanli A, et al. Anxiety and depressive disorders in patients presenting with chest pain to the emergency department: a comparison between cardiac and non-cardiac origin. J Emerg Med. 2010;39:144-150.
To comment on this article, contact rdavidson@uspharmacist.com.





