US Pharm. 2022;47(8):37-42.
ABSTRACT: Some of the most common questions asked at a community pharmacy are those related to treatment for a rash. There are various types of generalized rashes that pharmacists can quickly assess to determine appropriate self-treatment. Examples include contact dermatitis and insect bites. In other scenarios, referrals may be required. A community pharmacist can utilize a structured framework to evaluate the patient’s rash and help navigate treatment options.
The accessibility of OTC products in a community pharmacy allows patients to address self-care issues without requiring physician oversight. By reducing prescription drug costs and clinical visits, OTC availability results in $146 billion cost-savings for the healthcare system.1 Among the most common OTC product categories identified in an analysis by the Consumer Healthcare Products Association, medicated skin products are used by at least 61% of sufferers to treat their conditions.1 Medicated skin, lower gastrointestinal, and upper gastrointestinal products contribute to 61% of total OTC savings, largely driven by the price difference between these products and their prescription counterparts.1 Thus, a community pharmacy may be the first stop for somebody seeking help with regards to a rash. Community pharmacists are well-trained to triage generalized rashes and recommend proper treatment. This article will review the various types of generalized rashes, corresponding treatment options, and how to best field questions brought to the community pharmacist.
Types of Rashes
A community pharmacist may encounter a variety of generalized rashes. TABLE 1 describes common rashes that patients may address with a pharmacist and corresponding self-treatment options that may be recommended.
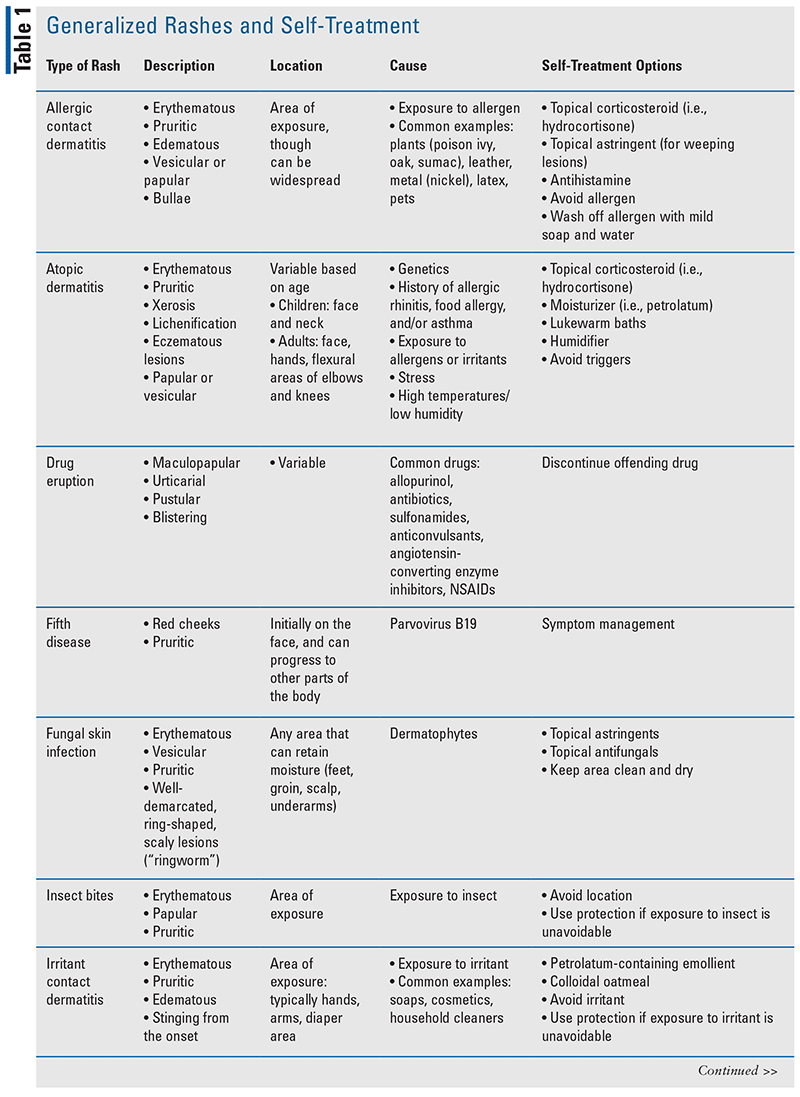

Dermatitis
Dermatitis is one of the most common forms of dermatologic conditions, resulting in 10% to 30% of consultations to dermatology.2 In general, common complaints include erythema and pruritus. The location and causes of dermatitis will determine the type of dermatitis and the corresponding treatment plan.
Atopic Dermatitis
Also known as eczema, atopic dermatitis (AD) occurs most commonly in children, though it can occur in adults, and particularly in patients with a history of asthma, allergic rhinitis, or food allergy.3,4 Various triggers may include irritants such as skin products, stress, or allergens. Dry skin and pruritus are prominent characteristics of AD. The use of moisturizers can help to minimize acute flare-ups of AD; more specifically, moisturizing with petrolatum after a bath or shower can help to keep the skin moist and thereby reduce the risk of AD flare-ups. Pharmacologic therapy is determined based on disease severity; though there are a variety of treatment options, topical corticosteroids are the standard first-line therapy in AD and available as an OTC product (hydrocortisone 1%) for mild cases.4
Contact Dermatitis
An irritant contact dermatitis (ICD) causes a rash limited to the area that had contact with the irritant and is often associated with pain and discomfort, in addition to pruritus and red macules.2 The skin may have been exposed to a chemical causing the irritation, including common household products (e.g., cleaning supplies). Symptoms typically occur soon after exposure to the irritant. Questions pharmacists may ask patients to determine ICD may include those related to the exposure of any new irritants or products, ranging from household cleaners to new detergents to new clothing or cosmetics. Treatment may be as simple as application of petrolatum if the ICD is minor. Oftentimes, due to infrequent changing of diapers or excessive exposure to urine or feces, diaper dermatitis—considered a type of ICD—may occur in both children and adults who experience incontinence. Diaper rashes can be prevented and treated by changing diapers as soon as they are soiled and applying a skin protectant such as petrolatum or zinc oxide.5
Allergic contact dermatitis (ACD) can be the result of allergens, such as plants, metals, and cosmetics, and is not always limited to the area of exposure to the allergen but may spread beyond the area.2,5 Unlike ICD, ACD symptoms may not occur right away: The first exposure sensitizes the patient and causes a delayed hypersensitivity reaction resulting in the rash symptoms later on, or even after the second exposure to the allergen.
Drug-Induced Rashes
As medication experts, pharmacists are well-positioned to triage drug-induced rashes, which may be the first type of rash that comes to mind when assessing a patient’s symptoms. Drug-induced rashes as adverse reactions could present for various reasons, including genetics, rate of administration, or type of drug formulation.5 They can be characterized as exanthematous, urticarial, blistering, or pustular (eruptions).5-7 Common medications that trigger the different types of drug-induced rashes are found in TABLE 2.
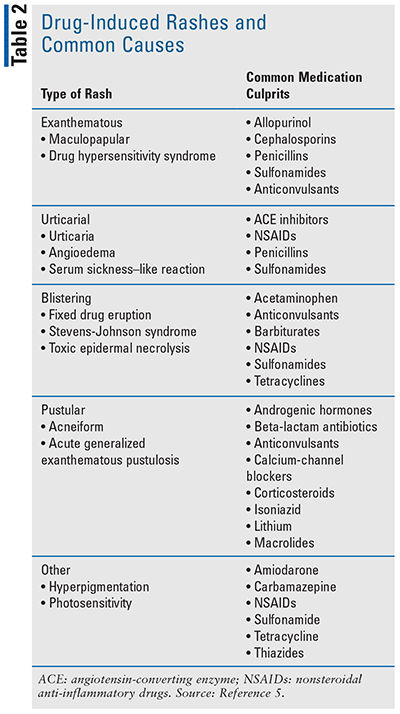
Exanthematous rashes present as erythematous lesions that are pruritic. They could be maculopapular eruptions that resolve with drug continuation. On the other hand, a drug hypersensitivity syndrome includes a fever with organ involvement. Urticaria is often the first sign of an anaphylactic reaction to drug therapy. It is typically accompanied by hives and angioedema, but if a fever or muscle aches are present, then this urticarial rash is more consistent with a serum sickness–like reaction.5,6
A fixed-drug eruption presents as red and pruritic lesions that can blister or progress into lesions and may even exhibit a burning or stinging sensation. These eruptions occur in the same location(s) each time the drug is used. A severe form of blistering lesions can be found in drug-induced reactions called Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN). Not only is a rash present, but also pain, fever, respiratory symptoms, and epidermal sloughing. These reactions are life-threatening and warrant emergent assistance.5-7
Mild pustular eruptions due to medications are acneiform drug reactions that cause acne. A more severe form of this reaction accompanied by fever, many more pustules, and diffuse erythema is called acute generalized exanthematous pustulosis. Other types of drug-induced skin reactions include hyperpigmentation and photosensitivity. Photosensitivity reactions can present like a rash or a severe sunburn; the rash may be more extensive beyond sun-exposed areas.5,6
If any drug-induced skin reactions occur immediately after drug intake, the drug should be discontinued and the prescriber contacted for a substitution if warranted. If a rash is particularly severe—and especially if a fever is present—a referral for more emergent management is needed.5,6
Infection-Induced Rashes
Fifth Disease: Fifth disease is a contagious virus that occurs more commonly in children than adults and is transmitted through respiratory droplets. Bright red cheeks are the characteristic sign of this virus, and hence it can pass off as a rash. Prior to the facial rash, a patient will present with fever, runny nose, and headache.8 Another rash may appear after the facial rash on other parts of the body, including the chest and back, arms, or legs. Adults may also exhibit pain and swelling in their joints. Otherwise, this is a mild virus that can resolve within 2 to 3 weeks.
Fungal Infections: Caused by dermatophytes, fungal skin infections typically occur in moist areas of the body that encourage mycotic growth, including the feet, groin, scalp, and underarms.9,10 The mycotic infections that present commonly as rashes include those on the groin (tinea cruris) and on the body (tinea corporis). Topical antifungals are available OTC to help treat such infections but resolution can take up to 6 weeks. Nonpharmacologic methods are just as important when educating patients regarding treatment.
Varicella and Herpes Zoster: The varicella-zoster virus (VZV) causes varicella (chickenpox) and herpes zoster (shingles). Historically known to affect children before vaccines were developed, the pruritic rash characteristic of chickenpox usually starts as macules and papules on the face and torso, and then spreads to the extremities.7,11 The lesions crop up in successive stages, so “older” lesions may progress to become pustules and crusts as other crops of macules surface.7 Shingles occurs when the VZV reactivates later in life and presents as a unilateral rash on one to three areas of skin.11 Postherpetic neuralgia is a painful complication resulting from shingles. Fortunately, safe and effective vaccines exist to prevent these viruses and consequences from occurring.
Insect Bites
Insect bites may be another common reason for patients to seek treatment at a community pharmacy. However, some insect bites are best treated via prescription medication. For example, ticks may lead to Lyme disease, which requires antibiotic treatment to prevent long-term sequelae.7,12,13 Pharmacists may inquire about recent travel (both local and abroad) to assist in determining the condition and respective treatment. TABLE 3 explains the differences in presentation of common insect bites and whether self-treatment or referral is needed.

Examination of Darkly Pigmented Skin
The examination of darkly pigmented skin has been historically undertaught in medical professional education, making it difficult for the trained clinician to triage patients with darker skin and thus potentially underdiagnosing those with dermatologic concerns.15 To address this, a recent compilation of online databases, dermatology journals, and dermatology-organization websites was published to reflect the growing expanse of skin-of-color images that can assist in the education and learning of dermatologic conditions in people of color.16 Erythema in darker skin may appear dark brown or violet in color, as is the possible case of eczema.17 When evaluating a rash on darkly pigmented skin, pharmacists should consider the rash in the context of the respective skin color and provide a recommendation for self-treatment or referral accordingly.
Addressing Generalized Rashes Using QuEST SCHOLAR-MAC
Using a structured framework to elicit information will ensure a comprehensive evaluation of a patient’s symptoms before offering a well-informed recommendation. QuEST SCHOLAR-MAC is a simple process to quickly—but properly—evaluate a patient’s concerns to determine a self-treatment that is individualized to the patient; this process can be applied to address generalized rashes. The final step of the process should include documentation and follow-up.18,19 The components of the mnemonic can be found in TABLE 4.
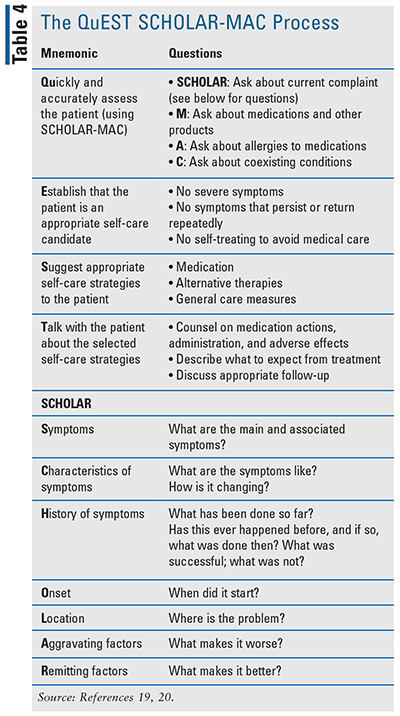
If after completing the QuEST SCHOLAR-MAC process the pharmacist determines that the patient is not a self-treatment candidate, patients or caregivers should be advised to discuss their rashes with their primary care providers or specialists. Reasons for which a patient would need a referral include those rashes that are worsening, severe rashes that need a more definitive diagnosis for an appropriate treatment, rashes of an unknown etiology, symptom-specific exclusions to self-treatment, and the pharmacist is doubtful of the patient’s medical condition.20 If a rash is accompanied with symptoms that may indicate a possible infection, including fever, pain, redness, swelling, warmth, and/or pus, a prompt referral for further care is required. If a rash is accompanied by other signs of an allergic reaction, such as shortness of breath, wheezing, or hypotension, emergency services are warranted. Although parents may first contact their community pharmacist due to accessibility, children younger than age 2 years should be referred to their pediatrician for an appropriate assessment and treatment recommendation.
Pharmacologic and Nonpharmacologic Treatment
For self-treatment purposes, pharmacologic treatment recommended by the pharmacist will generally treat the symptoms of the rash a patient may be experiencing. Symptoms can include pain or discomfort, pruritus, irritation, and inflammation. Short-term use of systemic analgesics can include NSAIDs or acetaminophen. Skin protectants for treatment and prevention include emollients and moisturizers that promote healing. Examples include petrolatum, glycerin, and lanolin. Topical first-aid antibiotics may be helpful to prevent infections and should not be used to treat an existing infection. In fact, it has been found that petrolatum is as effective as first aid antibiotic topical products in preventing infection.21 Topical corticosteroids such as hydrocortisone can reduce inflammation and pruritus in many generalized rashes. Nonpharmacologic treatment will depend on the type of rash and can range from simply avoiding a trigger or allergen to using a cold compress.
Conclusion
Community pharmacists are well-positioned to triage patients at the point of care when determining self-treatment for generalized rashes. By using the QuEST SCHOLAR-MAC process, pharmacists can help by providing an appropriate treatment recommendation. Many rashes can be managed with OTC products and nonpharmacologic methods. Questionable or severe rashes that cannot be self-treated would need to be referred to a provider for further management.
REFERENCES1. Consumer Healthcare Products Association. The value of OTC medicines to the U.S. healthcare system. www.chpa.org/about-consumer-healthcare/research-data/research-reports/value-otc-medicines-us-healthcare-system-0. Accessed May 27, 2022.2. Howe W. Overview of dermatitis (eczematous dermatoses). In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. April 15, 2022. www.uptodate.com/contents/overview-of-dermatitis-eczematous-dermatoses. Accessed May 31, 2022.3. Eichenfield LF, Tom WL, Chamlin SL, et al. Guidelines of care for the management of atopic dermatitis: section 1. Diagnosis and assessment of atopic dermatitis. J Am Acad Dermatol. 2014;70(2):338-351.4. Law RM, Gulliver WP, Kwa P. Atopic dermatitis. In: DiPiro JT, Yee GC, Posey L, et al, eds. Pharmacotherapy: A Pathophysiologic Approach, 11e. McGraw Hill;2020.5. Law RM, Law DTS, Maibach HI. Dermatologic drug reactions, contact dermatitis, and common skin conditions. In: Dipiro JT, Yee GC, Posey L, et al, eds. Pharmacotherapy: A Pathophysiologic Approach, 11th ed. McGraw Hill; 2020.6. Broyles AD, Banerji A, Barmettler S, et al. Practical guidance for the evaluation and management of drug hypersensitivity: specific drugs. J Allergy Clin Immunol Pract. 2020;8(9 Supplement):S16-S116.7. Ely JW, Stone MS. The generalized rash: part I. Differential diagnosis. Am Fam Physician. 2010;81(6):726-734.8. CDC. Parvovirus B19 and fifth disease. www.cdc.gov/parvovirusb19/fifth-disease.html. Accessed June 2, 2022.9. Brown TR, Dresser L. Superficial fungal infections. In: DiPiro JT, Yee GC, Posey L, et al, eds. Pharmacotherapy: A Pathophysiologic Approach, 11th ed. McGraw Hill; 2020.10. Smith MG. Chapter 42: fungal skin infections. In: Handbook of Nonprescription Drugs: An Interactive Approach to Self-Care, 20th ed. American Pharmacists Association; 2020.11. Epidemiology Branch, Division Viral Diseases National Center for Immunization and Respiratory Diseases. Varicella (chickenpox) and herpes zoster (shingles). Lecture presented at: Centers for Disease Control and Prevention; Atlanta, GA; August 2, 2013.12. CDC. Signs and symptoms of Lyme disease. www.cdc.gov/lyme/signs_symptoms/index.html. Accessed June 2, 2022.13. CDC. Signs and symptoms of Rocky Mountain spotted fever. www.cdc.gov/rmsf/symptoms/index.html. Accessed June 2, 2022.14. CDC. Scabies. www.cdc.gov/parasites/scabies/index.html. Accessed May 31, 2022.15. Louie P, Wilkes R. Representations of race and skin tone in medical textbook imagery. Soc Sci Med. 2018;202:38-42.16. Chang MJ, Lipner SR. Resources for skin of color images. J Am Acad Dermatol. 2021;84(6):e275-e277.17. Armstrong CA. Approach to the clinical dermatologic diagnosis. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA.18. Taylor J, Rocchi M. The art and science of counselling patients on minor ailments/OTC medicines. SelfCare. 2018;9(3):3-22.19. Buring SM, Kirby J, Conrad WF. A structured approach for teaching students to counsel self-care patients. Am J Pharm Educ. 2007;71(1):8.20. Dlugosz CK. The “QuEST” approach to self-care encounters. In: Handbook of Nonprescription Drugs Quick Reference: A Practitioner’s Guide, 2nd ed. American Pharmacists Association; 2021.21. Draelos ZD, Rizer RL, Trookman NS. A comparison of postprocedural wound care treatments: do antibiotic-based ointments improve outcomes? J Am Acad Dermatol. 2011;64(3 Supplement):S23–S29.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





