US Pharm. 2023;48(5):37-42.
ABSTRACT: There is an abundance of published literature highlighting the negative impact of healthcare disparities with respect to access to treatment, routine healthcare, and clinical outcomes in those with prediabetes and diabetes. Healthcare disparities can be classified as racial/ethnic, socioeconomic, and geographical. Research has also shown that certain racial/ethnic groups and individuals with lower income levels are at a heightened risk of developing diabetes and diabetes-related complications. In an effort to identify and address healthcare disparities and improve clinical outcomes for all individuals with prediabetes and diabetes, many professional organizations, including updates in the 2023 American Diabetes Association’s Standards of Medical Care, have issued recommendations that clinicians can employ to identify and reduce the incidence of healthcare disparities. As one of the most accessible healthcare providers, pharmacists are well poised to implement patient education measures tailored to patient needs and direct patients to the various patient support and education resources for diabetes care. These educational efforts may improve patient access to therapy, encourage patients to take an active role in their care, decrease healthcare disparities in diabetes care, and improve overall clinical outcomes.
Despite continual advances in understanding the progressive and multifaceted etiology of diabetes, ongoing education initiatives to expand awareness about the significance of early detection and treatment of diabetes and the approval and availability of an array of pharmacologic therapies that target underlying pathophysiologies, the incidence of prediabetes and diabetes continues to soar, principally due to the ongoing obesity epidemic among both adult and pediatric patients.
According to the latest statistics from the CDC, in the United States an estimated 37.3 million individuals, representing 11.3% of the population, have diabetes.1 Of that number, 28.7 million (including 28.5 million adults) have been officially diagnosed, and the remaining 8.5 million individuals (23%) are unaware of diabetes status and are undiagnosed.1 An additional 96 million aged 18 years and older are classified as prediabetic, representing 38% of the U.S. adult population.1 Moreover, the CDC indicates that 26.4 million people aged 65 years and older, representing 48.8% of the older adult population, are considered prediabetic.1 In the past 2 decades, the incidence of diabetes diagnosed in adults has more than doubled, and in 2021, more than 100,000 Americans died from diabetes and its related complications.2 Diabetes is the seventh-leading cause of death and the principal cause of kidney failure, lower limb amputations, and adult blindness, according to the CDC.2
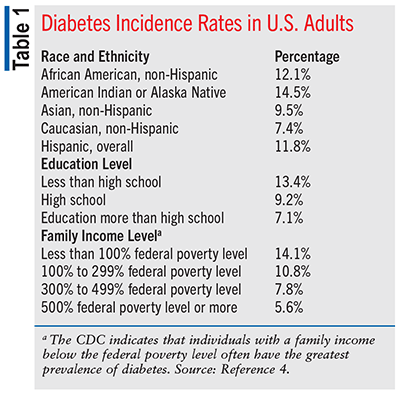
Numerous publications have revealed that diabetes disproportionately impacts individuals of lower socioeconomic status and certain racial/ethnic groups, and statistics indicate greater incidence rates among these groups.3 The most recent statistics from the National Health Interview Survey among those aged 18 years and older with diagnosed diabetes, the incidence rates according to race/ethnic groups, level of education, and income levels are indicated in TABLE 1.
HEALTHCARE DISPARITIES AND DIABETES
Healthcare disparities and inequalities have been a topic of interest for years, and more extraordinary efforts have been focused on identifying and addressing factors that contribute to healthcare disparities. Many health experts note that the burdens identified during the COVID-19 pandemic brought the issue of healthcare disparities to the forefront.3 As a result of the identified gaps in care, numerous healthcare and professional organizations have published statements on the social determinants of health (SDOH) and have implemented measures to identify and address the issues pertinent to healthcare disparities across a spectrum of diseases, including diabetes.3,5-7
In a recent publication in the journal Diabetes Care, the authors indicate that with regard to diabetes care, considerable and ongoing healthcare disparities have been identified. These disparities are of particular concern since diabetes is one of the most prevalent chronic conditions, affecting more than 10% of adults in the U.S.3 The authors also state that multiple research efforts have established that these healthcare disparities may be attributed to race, ethnicity, level of income, occupation, and other indicators for quantifying socioeconomic statuses such as neighborhood and environment.3 Moreover, research has shown that diabetes affects racial/ethnic minorities and individuals of lower economic status with respect to prevalence, diabetes-related complications, and mortality at higher rates.3,8,9
DEFINITION AND CLASSIFICATION OF HEALTHCARE DISPARITIES
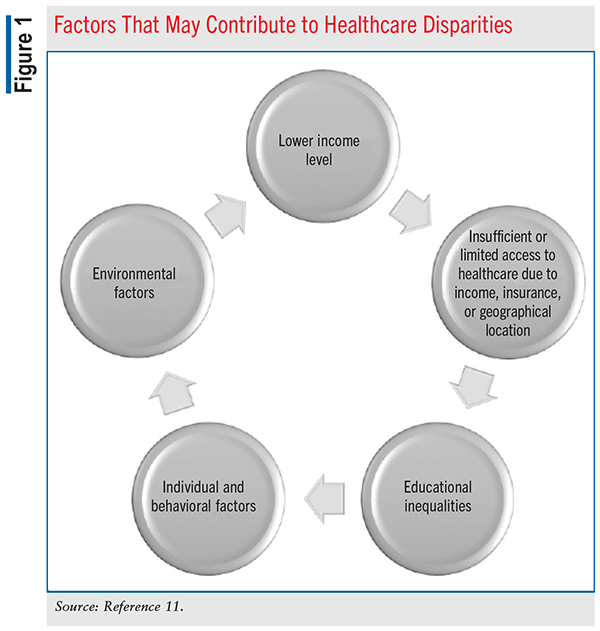
Healthcare disparities can be multifaceted in nature and the result of various factors. Healthcare disparities are generally classified as racial/ethnic, socioeconomic, and geographical. The CDC defines healthcare disparities as “preventable differences in the burden of disease, injury, violence, or opportunities to achieve optimal health that are experienced by socially disadvantaged populations.”10,11 The CDC indicates that examples of factors that may contribute to or expand the prevalence of healthcare disparities may include race/ethnicity, lower economic status, environmental threats, inadequate access to care, individual and behavioral factors, and degree of education.11
The U.S. Department of Health and Human Services (DHHS) Healthy People 2030 program defines a health disparity as “a particular type of health difference that is intricately associated with social, economic, and/or environmental disadvantage. Health disparities adversely affect groups of people who have systematically experienced greater obstacles to health based on their racial or ethnic group; religion; socioeconomic status; gender; age; mental health; cognitive, sensory, or physical disability; sexual orientation or gender identity; geographic location; or other characteristics historically linked to discrimination or exclusion.”12 The DHHS also indicates that healthcare disparities manifest themselves as major differences in the rate of disease prevalence, incidence, morbidity, mortality, or survival of certain patient populations when compared with the health status of the majority population.13
IDENTIFYING AND ADDRESSING HEALTHCARE DISPARITIES
The CDC indicates that health risks and disparities can be diminished by identifying and addressing the various SDOHs.11 Examples of factors that may contribute to healthcare disparities are shown in FIGURE 1.
The Healthy People 2030 and the CDC state that since establishing health equity is a top priority for their agency, they are undertaking several measures to identify and address the SDOH, which are defined as nonmedical factors affecting clinical outcomes that can impact an individual’s health and well-being, centered on where individuals are born, grow, live, work, and age.14-17 An expanding amount of research indicates that SDOH contribute to extensive health disparities and inequities with regard to diabetes and other diseases as well.14-16 The Healthy People 2030 program notes examples of SDOH that include15:
• Safe housing, transportation, and neighborhoods
• Experiencing racism, discrimination, and violence
• Level of education, job opportunities, and income
• Access to nutritious foods and physical activity/exercise programs
• Exposure to air pollution and polluted water
• Language and literacy skills.
According to a recent publication by CVS pharmacies, numerous factors may contribute to or exacerbate diabetes-related healthcare disparities and affect clinical outcomes in diabetes care, including:
• Affordability: having the economic means to pay for medications
• Awareness: understanding therapy options and the significance of adherence to the therapy plan
• Accessibility: being able to access routine healthcare and treatment easily
• Trust: having a degree of confidence and comfort with healthcare providers.18
ORGANIZATIONS ADDRESSING DIABETES CARE DISPARITIES
The CDC has established the Division of Diabetes Translation (DDT) program, and its mission is to enhance access to healthcare for all Americans with diabetes and eradicate healthcare disparities. The DDT program employs preventative and education programs to identify and address healthcare disparities in patient populations at greater risk of prediabetes, type 2 diabetes mellitus (T2DM), and diabetes-related complications. Moreover, the DDT website indicates that its program aims to implement patient education initiatives tailored to the individual needs of patients.19 The CDC’s DDT program states that its overall goals are to diminish the preventable burden of diabetes via various measures, such as public health leadership, partnership, research, programs, and policies that convert science into practice. Other valuable programs associated with the CDC and DDT include the National Diabetes Prevention Program, the National Diabetes Wellness Program, and the Diabetes Self-Management Education and Support Services.19
AMERICAN DIABETES ASSOCIATION
Updated ADA Standards of Care
The American Diabetes Association (ADA) indicates that diabetes-related healthcare disparities are well documented in the literature, and certain patient populations are at greater risk for diabetes and poorer diabetes outcomes.20,21 The ADA points out that financial barriers that prevent access to medications and routine healthcare remain a primary source of healthcare disparities, and clinicians should consider costs when devising treatment goals.20,21 The ADA notes that decreases in cost-related barriers to medication use are correlated with better biological and psychological outcomes, including quality of life.20,21
The ADA also states that with regard to the incidence of undiagnosed diabetes, substantial racial and ethnic disparities still transpire among many individuals with and/or at risk for diabetes and prediabetes. In the 2023 ADA Standards of Care, the panel focused on measures to diminish healthcare disparities and inequities.20,21
The ADA made the following recommendations to diminish disparities:
• Clinicians should evaluate social context, including potential food insecurity, housing stability, and financial barriers, and use that information to guide treatment decisions.
• Patients should be referred to local community resources when available.
• Patients should be provided with self-management support from lay health coaches, navigators, or community health workers when accessible.21
In a recent press release on the ADA website, Chuck Henderson, ADA CEO, stated, “This year’s annual report provides necessary guidance that considers the role health inequities play in the development of diabetes, particularly for vulnerable communities and communities of color disproportionately impacted by the disease. This guidance will ensure healthcare teams, clinicians, and researchers treat the whole person.”20
Key Points Highlighted by the ADA
• The 2023 ADA Standards of Care state that substantial racial and ethnic disparities exist among those undiagnosed with diabetes.22 The ADA recommends early screening as a primary step to recognize and address these disparities.22
• The ADA recognizes that healthcare disparities negatively affect individuals who have faced more significant barriers to health based on their race or ethnicity, socioeconomic status, gender, disability, or other factors.22 Extensive research shows that these disparities may considerably impact health outcomes, including augmenting the risk for obesity, diabetes, and diabetes-related complications.23 The ADA recommends that clinicians assess systematic, structural, and socioeconomic factors that may influence nutritional selection, access, and ability to afford healthy foods and dietary patterns; adherence to recommended dietary plans; behavioral patterns, such as neighborhood safety and accessibility to safe outdoor spaces for exercise, as well as environmental exposures; access to health care; social contexts; and, eventually, diabetes risk and outcomes.23
• The ADA has created a technology access program to expand equity and compliance with technologies such as insulin pumps and continuous blood glucose monitors.21
The ADA also has established a program known as #HealthEquityNow to improve healthcare access and routine care to all with diabetes, primarily concentrating on those in underserved populations who are at risk for and/or have diabetes.
The ADA has established the Health Equity Bill of Rights, which includes 10 fundamental rights for those with prediabetes and diabetes. More information can be found on the HealthEquityNow website: www.diabetes.org/healthequitynow.
HEALTHY PEOPLE 2030 INITIATIVE
The Healthy People 2030 initiative indicates that identifying healthcare disparities is essential to promoting health equity and is focused on health literacy and SDOH. The program provides valuable tools for clinicians, organizations, and communities to identify and address healthcare disparities.12
In addition, Healthy People 2030 compiles data from the Healthy People in Action program to emphasize how states, communities, and organizations focus on health disparities, improve health equity, and enhance health by the following measures: utilizing evidence-based interventions and approaches; assessing interventions; and developing multisector collaborations.12
RECENT NEWS AND CLINICAL STUDIES
In December 2022, the ADA and CVS Health Today announced the extension of their Project Power, a program designed to boost diabetes awareness, identify and address healthcare disparities, and provide diabetes education to those with T2DM and prediabetes. The overall goals of Project Power are to educate patients about diabetes and to eradicate obstacles to treatment, such as eliminating the stigmas associated with diabetes and recognizing and eliminating barriers that are correlated with SDOH.24
In a recent publication in The Lancet Regional Health, researchers conducted a secondary analysis of the Look AHEAD (Action for Health in Diabetes) trial. The primary objective was to explore the correlation of race/ethnicity with the initiation of newer diabetes medications. The study included 4,892 participants, of whom 63.6%, 15.7%, 12.6%, 5.2%, and 2.9% were Caucasians, African Americans, Hispanics, American Indians or Alaskan Native (AI/AN), or other race/ethnicity, respectively.25 The authors revealed that among individuals of all minority races/ethnicities, there was a lower initiation rate of newer diabetes medications compared with Caucasian participants, with the initiation of newer diabetes medications being significantly lower for African Americans and AI/AN participants.25 Factors for the differences in medication initiation included insurance coverage, patient preference, prescriber patterns, and income level.25 The authors also indicated that among the socioeconomic factors examined, lower annual family income and receiving medical care at a hospital clinic or outpatient department were greatly correlated with lower initiation of newer diabetes medications.25 The authors posited that more research is warranted to address these issues.25
In the journal Telemedicine and e-Health, authors investigated disparities in diabetes management outcomes between African American and Caucasian patients with T2DM in a remote monitoring program. The results revealed that the percentage of Caucasian patients with a glycosylated hemoglobin A1C (HbA1c) >9% decreased from 16% at the baseline to 7% at program completion. The results showed a 30% to 18% reduction among African American patients.26 The authors also reported that after correcting for the effects of baseline HbA1c and other covariates, the average HbA1c compared with the Caucasian patients among African American patients at the end of the program was 0.23 points higher.26 The authors concluded that the remote monitoring and coaching programs reduced the gaps between both study groups. Still, disparities in HbA1c remained, and more research is warranted to understand the contributory factors.26
In another study published in the Annals of Internal Medicine, researchers conducted a cross-sectional study that utilized a logistic regression model to ascertain the BMI levels and age at which the incidence of diabetes in racial and ethnic minority populations is comparable to the incidence of diabetes in Caucasians deemed at risk of diabetes.27 They found that Asian, Hispanic, and black Americans are at augmented risk for diabetes at lower weights and younger ages than Caucasians.27 They concluded that screening Asian, Hispanic, and black Americans for diabetes at lower BMI and younger ages than Caucasians might have the potential to diminish the incidence of undiagnosed diabetes in these groups and, as a result, improve health equity in diabetes care.27
THE ROLE OF THE PHARMACIST
Healthcare disparities are often multifaceted in nature and warrant a multidisciplinary approach to identifying and addressing them. There is an abundance of literature highlighting the pivotal role of pharmacists in the effective management of diabetes care; therefore, pharmacists can be instrumental in addressing diabetes health disparities by providing patient education, reminding patients about the significance of adherence to treatment plans, understanding treatment expectations, providing education about glycemic targets and routine follow-up, and directing patients to the extensive array of patient education resources.
As one of the most accessible healthcare providers, pharmacists are well poised to expand awareness about the risk factors for T2DM and can act as patient identifier, educator, and advocate. Due to routine interaction with patients, pharmacists may be able to identify patients who may be at risk for diabetes and encourage these patients to discuss their risk factors with their primary healthcare provider. Pharmacists can also make clinical recommendations tailored to patients’ needs to expand patient adherence, thus improving clinical outcomes and reducing the incidence of diabetes-related complications.
One of the most fundamental aspects of effective diabetes management is patient education, and pharmacists are in an ideal position to educate patients in various clinical settings. During counseling, pharmacists should remember that patient education and counseling initiatives should be geared to patient need and level of understanding. Both verbal and written instructions are also valuable tools, and using the teach-back method will enable pharmacists to assess a patient’s level of understanding. These measures are integral components of diabetes care and are also vital in improving patient adherence and clinical outcomes.
In a recent publication, the authors state that a one-size-fits-all approach to diabetes care is not the best approach to treatment, and it is essential that clinicians employ a patient-centered approach considering a patient’s culture, beliefs, and level of understanding when educating patients about diabetes and treatments.28
CONCLUSION
Diminishing healthcare disparities is an ongoing effort for the healthcare system, and measures are being implemented to expand healthcare access and foster equity. While incredible advances have been made in grasping a better understanding of the complex and progressive nature of T2DM, it is essential to note that expanding patient education initiatives is the key to identifying and decreasing healthcare disparities.
Pharmacists need to take advantage of their access to patients and their frequent encounters to monitor adherence to diabetes therapy and help prevent the unnecessary progression of the disease. It has been demonstrated that pharmacist-managed diabetes care can help patients attain glycemic goals in a shorter time frame than standard care.29 Pharmacists can teach patients about the importance of self-management strategies since diabetes self-management education and support have proven cost-effective by reducing hospital admissions and readmissions and projected lifetime healthcare costs related to a lower risk for T2DM complications.30
Many professional organizations and healthcare providers have taken a critical first step by acknowledging that health disparities exist and undertaking measures to address them. Implementing patient-centered measures to identify and address healthcare disparities starts with educating patients about diabetes, risk factors, complications, and the significance of adherence to treatment plans, encouraging patients to take an active role in their care, and directing patients to the numerous education and support resources tailored to patient need that may aid all patients in obtaining quality diabetes care.
REFERENCES
1. CDC. National diabetes statistics report. June 29, 2022. www.cdc.gov/diabetes/data/statistics-report/index.html. Accessed February 20, 2023.2. CDC. What is diabetes? July 7, 2022. www.cdc.gov/diabetes/basics/diabetes.html. Accessed February 24, 2023.3. Hill-Briggs F, Adler NE, Berkowitz SA, et al. Social determinants of health and diabetes: a scientific review. Diabetes Care. 2020;44(1):258-279.
4. CDC. By the numbers: diabetes in America. October 25, 2022. www.cdc.gov/diabetes/health-equity/diabetes-by-the-numbers.html. Accessed April 4, 2023.5. Byhoff E, Kangovi S, Berkowitz SA, et al. A Society of General Internal Medicine position statement on the internists’ role in social determinants of health. J Gen Intern Med. 2020;35:2721-2727.
6. Council on Community Pediatrics. Poverty and child health in the United States. Pediatrics. 2016;137(4):e20160339.7. Daniel H, Bornstein SS, Kane GC, Health and Public Policy Committee of the American College of Physicians. Addressing social determinants to improve patient care and promote health equity: an American College of Physicians position paper. Ann Intern Med. 2018;168:577-578.
8. King CJ, Moreno J, Coleman SV, Williams JF. Diabetes mortality rates among African Americans: a descriptive analysis pre and post Medicaid expansion. Prev Med Rep. 2018;12:20-24.9. Golden SH, Brown A, Cauley JA, et al. Health disparities in endocrine disorders: biological, clinical, and nonclinical factors—an Endocrine Society scientific statement. J Clin Endocrinol Metab. 2012;97(9):E1579-E1639.
10. CDC. Health disparities. January 31, 2017. www.cdc.gov/aging/disparities/index.htm. Accessed April 5, 2023.11. CDC. Health disparities. November 24, 2020. www.cdc.gov/healthyyouth/disparities/index.htm. Accessed February 24, 2023.
12. U.S. Department of Health and Human Services. Health equity in Healthy People 2030. www.health.gov/healthypeople/priority-areas/health-equity-healthy-people-2030. Accessed April 4, 2023.13. National Heart, Lung, and Blood Institute. Health disparities. April 2017. www.nhlbi.nih.gov/health/educational/healthdisp/index.htm. Accessed April 4, 2023.
14. CDC. Social determinants of health at CDC. December 8, 2022. www.cdc.gov/about/sdoh/index.html. Accessed April 4, 2023.15. U.S. Department of Health and Human Services. Social determinants of health. www.health.gov/healthypeople/priority-areas/social-determinants-health. Accessed April 4, 2023.
16. World Health Organization. Closing the gap in a generation: health equity through action on the social determinants of health. 2008. https://apps.who.int/iris/bitstream/handle/10665/43943/9789241563703_eng.pdf. Accessed April 4, 2023.17. Howell CR, Harada CN, Fontaine KR, et al. Perspective: acknowledging a hierarchy of social needs in diabetes clinical care and prevention. Diabetes Metab Syndr Obes. 2023;16:161-166.18. CVS Health. Understanding health disparities in diabetes to improve health. November 17, 2020. www.cvshealth.com/news/diabetes/understanding-health-disparities-in-diabetes-to-improve-health.html. Accessed February 26, 2023.
19. CDC. Advancing health equity. April 6, 2022. www.cdc.gov/diabetes/health-equity/index.html. Accessed February 27, 2023.20. American Diabetes Association. American Diabetes Association releases 2023 Standards of Care in diabetes to guide prevention, diagnosis, and treatment for people living with diabetes. December 12, 2022. www.diabetes.org/newsroom/press-releases/2022/american-diabetes-association-2023-standards-care-diabetes-guide-for-prevention-diagnosis-treatment-people-living-with-diabetes. Accessed February 20, 2023.
21. ElSayed NA, Aleppo G, Aroda VR, et al. Improving care and promoting health in populations: Standards of Care in diabetes—2023. Diabetes Care. 2023;46(Suppl 1):S10-S18.22. ElSayed NA, Aleppo G, Aroda VR, et al. Classification and diagnosis of diabetes: Standards of Care in diabetes—2023. Diabetes Care. 2023;46(Suppl 1):S19-S40.
23. ElSayed NA, Aleppo G, Aroda VR, et al. Obesity and weight management for the prevention and treatment of type 2 diabetes: Standards of Care in diabetes—2023. Diabetes Care. 2023;46(Suppl 1):S128-S139.24. American Diabetes Association. Project Power. February 22, 2023. www.diabetes.org/get-involved/community/project-power. Accessed February 25, 2023.
25. Elhussein A, Anderson A, Bancks MP, et al. Racial/ethnic and socioeconomic disparities in the use of newer diabetes medications in the Look AHEAD study. Lancet Reg Health Am. 2022;6:100111.26. Andersen JA, Scoggins D, Michaud T, et al. Racial disparities in diabetes management outcomes: evidence from a remote patient monitoring program for type 2 diabetic patients. Telemed J E Health. 2021;27(1):55-61.
27. Aggarwal R, Bibbins-Domingo K, Yeh RW, et al. Diabetes screening by race and ethnicity in the United States: equivalent body mass index and age thresholds. Ann Intern Med. 2022;175(6):765-773.28. Valentino AS, Nguyen TT, Pauling EE, et al. Collaborating with pharmacists to advance health equity for patients with diabetes through communication. J Am Pharm Assoc. 2022;62(3):693-696.
29. Yam FK, Adams AG, Divine H, et al. Clinical inertia in type 2 diabetes: a retrospective analysis of pharmacist-managed diabetes care vs. usual medical care. Pharm Pract (Granada). 2013;11(4):203-210.30. Powers MA, Bardsley JK, Cypress M, et al. Diabetes self-management education and support in adults with type 2 diabetes: a consensus report of the American Diabetes Association, the Association of Diabetes Care & Education Specialists, the Academy of Nutrition and Dietetics, the American Academy of Family Physicians, the American Academy of PAs, the American Association of Nurse Practitioners, and the American Pharmacists Association. Diabetes Educ. 2020;46(4):350-369.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.





