US Pharm. 2022;47(1):4-12.
The average person will spend one-third of their life sleeping. Sleep plays an important role in our health and well-being; both the quality and quantity of sleep can have major impacts on a variety of health outcomes. Sleep deprivation can lead to an increased risk of hypertension, obesity, diabetes, depression, heart attack, and/or stroke. In addition, lack of sleep represents a major cause of reduced productivity, increased healthcare utilization, increased likelihood of injury, and an overall decreased quality of life.1-3
Although individual sleeping needs will vary, the American Academy of Sleep Medicine (AASM) and Sleep Research Society developed a consensus statement, recommending that adults aged 18 to 60 years obtain 7 or more hours of sleep per night on a regular basis to promote optimal health. The National Heart, Lung, and Blood Institute and the National Sleep Foundation have also recommended that most adults get 7 to 8 hours of sleep a night. Unfortunately, many are not reaching this target; more than a third of U.S. adults report sleeping fewer than 7 hours a night, and an estimated 28% of adults report insufficient rest or sleep for 14 or more days during a 30-day period. Insufficient sleep is becoming an increasing concern among adolescents, with six out of 10 middle schoolers and seven out of 10 high schoolers not getting their recommended 8 to 12 hours of sleep per night. Decreasing sleep duration has become a public health concern; goals of Healthy People 2030 include increasing the proportion of adults and high school students who get enough sleep.3-6
Sleep insufficiency can be attributed to many societal factors, such as work schedules, round-the-clock access to technology, lifestyle, and travel. But if patients are spending enough time in bed and are still waking up tired, they may be suffering from some type of sleep disorder. Sleep disorders include problems with falling or staying asleep, waking up too early or too late, and problems with poor sleep quality. It is estimated that 50 million to 70 million Americans suffer from some type of chronic sleep and wakefulness disorder, which may cause significant impairment of daytime functioning.2,7
Prevalence
The most prevalent sleep disorder is insomnia, with up to 40% of U.S. adults reporting symptoms of insomnia at some point each year. The reported prevalence of insomnia disorder among the adult population appears to be increasing; over a 10-year period, the unadjusted prevalence of insomnia increased by 8% from 17.5% in 2002 to 19.2% in 2012. A higher prevalence is seen in women, the elderly, and patients with psychiatric and medical disorders. This condition accounts for more than 5 million physician office visits annually and more than 60 million prescriptions.1,8,9
Pharmacists are often the first healthcare professional that patients approach for conditions that may be treated with selfcare recommendations. Understanding the appropriate management of insomnia is vital for pharmacists to effectively help patients with this condition. The pharmacist should be familiar with the definition of insomnia and be mindful of the limitations of the various OTC products utilized in the management of insomnia. It is also important to recognize medications that may be contributing to patients’ sleep disorders.
What Is Insomnia?
Insomnia is characterized by chronic dissatisfaction with sleep quantity or quality that is associated with difficulty falling asleep, frequent nighttime awakenings with difficulty returning to sleep, and/or awakening earlier in the morning than desired, resulting in some form of daytime impairment, such as daytime sleepiness, impairment in functioning, and/or mood disturbances. This sleep difficulty occurs at least 3 nights per week and is present for at least 3 months despite adequate opportunity to sleep. Insomnia differs from sleep deprivation in that it is not defined by a specific sleep amount; individuals have difficulty sleeping despite having ample opportunity to sleep.9-11
Insomnia can be classified as episodic, persistent, or recurrent. Episodic insomnia includes symptoms that last at least 1 month but fewer than 3 months. Persistent insomnia is described as having symptoms that last for 3 months or longer. A patient with recurrent insomnia is someone who has experienced two or more episodes within the span of 1 year.11
Etiology of Insomnia
Current research suggests that insomnia is predominantly a disorder of hyperarousal or an abnormality in the wake/arousal system. Many identified factors can cause an imbalance in the wake/arousal system, such as lifestyle, environmental, anxiety, medical factors, genetics, and immune factors. One model utilized to help better understand these factors is the “3Ps.” The 3Ps refer to predisposing, precipitating, and perpetuating factors. Predisposing factors are not sufficient on their own to produce insomnia but rather serve as a contributing factor; they may cause the occasional night of poor sleep. These factors include genetics, personality traits, and social factors. These factors alone typically do not lead to dramatic sleep problems or to chronic insomnia. Insomnia symptoms are more likely to be triggered by various precipitating factors that may or may not be self-limiting. If the precipitating factor is improved or resolved, the symptoms of insomnia will also resolve. Precipitating factors usually involve changes in a patient’s life and can include medical or psychiatric conditions, stressful events, shift work, and medications. Medications that cross the blood-brain barrier can either inhibit or increase arousal. TABLE 1 lists common medications that can cause insomnia.
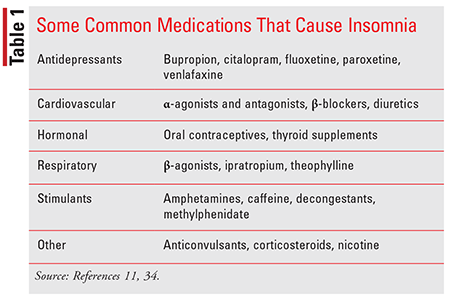
It is important to recognize that precipitating factors do not need to be single events; they can be multiple or recurrent events that build over time, contributing to the manifestation of symptoms. If the precipitating factors do not resolve, patients will begin to develop maladaptive behaviors and attitudes about sleep, perpetuating their insomnia and leading to chronic insomnia. Examples of perpetuating factors include poor sleep hygiene and negative thoughts about insomnia and its effects, such as “If I don’t fall asleep by 10:30, I’m probably going to be up all night.” Other perpetuating factors include distracting activities, such as eating or looking at social media/surfing the Web, watching television in bed, or drinking alcohol to help promote sleep. Over time, perpetuating factors become habit and counterproductive to a good night’s sleep.10,12-15
Management
When eliminating or appropriately managing a precipitating cause of insomnia does not resolve symptoms or when a cause is not identified, treatment is warranted. Cognitive behavioral therapy for insomnia (CBT-I) with or without relaxation therapy is considered the standard of care and is recommended by the AASM and the American College of Physicians. CBT-I targets the underlying issues that exacerbated sleep disturbances. It consists of psychoeducation, sleep hygiene counseling, relaxation training, stimulus control therapy, sleep restriction therapy, and cognitive therapy. It is usually a short-term treatment that involves four to eight sessions, with the patient using a mix of these approaches. Although extremely effective, patients are rarely referred to this treatment. There are many reasons for this, including demand for CBT-I providers drastically exceeding supply; clinician’s lack of knowledge about CBT-I and lack of motivation to refer; and finally, patients’ lack of awareness of nonpharmacological treatment options and their effectiveness compared with pharmacologic therapies.16-19
If insomnia symptoms do not resolve with CBT-I alone, pharmacotherapy can be initiated, but it should be in conjunction with CBT-I. There are several agents approved for the management of insomnia (TABLE 2). The choice of medication should be based on treatment goals and patient-specific characteristics. Risk and benefits should be assessed on an individual basis due to the potential of adverse effects and drug interactions.16,17
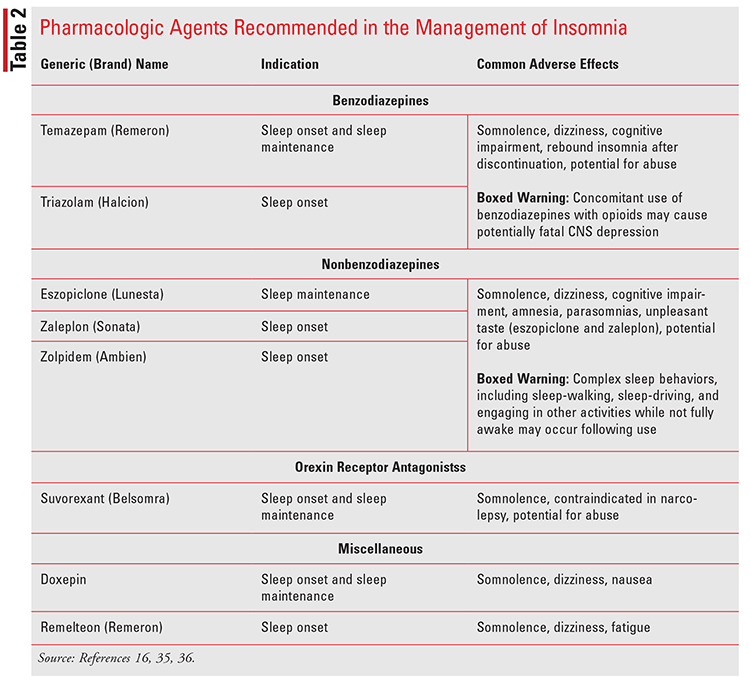
Nonpharmacologic Therapy
Many patients suffering from sleep disorders such as insomnia will approach the pharmacist seeking advice on how to best approach their sleep difficulties. It is important for the pharmacist to accurately assess a patient with insomnia to differentiate a sleep disturbance from insomnia. Questions such as “How long does it take you to fall asleep?” and “How many hours do you sleep?” should be compared with the patient’s normal sleep patterns. Inadequate opportunities to sleep represent sleep disturbances. There are several questionnaires, such as the Epworth Sleepiness Scale, that can be used to help this discussion.20
The first approach by the pharmacist to the treatment of insomnia should include nonpharmacologic interventions. This includes addressing sleep hygiene and stimulus control. Sleep hygiene includes recommendation of various behavioral and environmental changes to help promote sleep. Examples include maintaining a regular sleep schedule, avoiding alcohol and nicotine near bedtime, avoiding caffeine after noon, avoiding daytime naps, avoiding heavy meals close to bedtime, and adjusting the bedtime environment to decrease stimuli. Stimulus control is meant to help the patient reconnect the bedroom and bed with sleep. Patients should be advised not to go to bed until they are sleepy; to use the bed primarily for sleep; to avoid reading, watching TV, or using electronics while in bed; to leave the bedroom if they are unable to fall asleep for longer than 20 minutes; and to keep a fixed wake time in the morning.14,21
OTC Agents
Nonprescription medicines are frequently used to help treat insomnia-related symptoms. In 2020, OTC sales for sleep aids reached $429 million. None of the available products are indicated or recommended for the management of chronic insomnia due to lack of efficacy and safety data. Patients should be educated regarding the limited efficacy and safety of these products when in-quiring about the use of sleep aids.16,17,22
Antihistamines
Many products marketed for sleep disturbances are either single-entity antihistamines or products containing an analgesic in combination with antihistamines for those patients whose insomnia is a result of pain. The FDA has limited the active ingredient for OTC sleep aids to first-generation antihistamines diphenhydramine and doxylamine. There are many OTC products under different brand names that are available that contain diphenhydramine as an active or second active ingredient, which can potentially confuse patients. In 2002, the FDA required manufacturers to place a warning on all products containing diphenhydramine, advising patients to not use oral OTC diphenhydramine products with any other product containing diphenhydramine, including topical products.23,24
Antihistamines can help the symptoms of insomnia by promoting sedation, decreasing the time to sleep onset. However, their use should be limited because of little data and their potential for adverse effects from their anticholinergic properties, particularly a reduction in cognitive function, day-after sedation, development of tolerance, and interaction with other medications.25,26
Melatonin
Melatonin is a natural hormone that is produced by the pineal gland and plays a major role in the control of circadian sleep processes. It is a sleep regulator and is released in response to darkness. Research data available have demonstrated melatonin’s ability to help increase total sleep time in patients suffering from sleep restriction or altered sleep schedules, relieving daytime fatigue associated with jetlag, resetting the body’s sleep-wake cycle, and reducing the time it takes for patients to fall asleep. Meta-analyses have also documented melatonin to significantly reduce sleep-onset latency, increase total sleep time, and improve overall sleep quality in patients with primary sleep disorders.25,27-30
Currently, melatonin is not regulated by the FDA. It is considered a dietary supplement and is available as immediate- and slow-release preparations, with doses ranging from 0.1 to 5 mg. It has a relatively safe side-effect profile; however, further studies with large, high-quality sample sizes are needed to increase confidence in its routine use for the treatment of insomnia.28
Valerian
Many herbal products appear to have sedative properties. The most extensively studied product is valerian. It has been used for more than 2,000 years for the treatment of nervous unrest, stress, and sleep disorders. Evidence suggests that with repeated administration, at least a 2-week course, valerian produces a mild sleep-inducing effect, reducing time to sleep onset, promoting sleep maintenance, and potentially improving sleep quality. Valerian has been found to be generally safe; the rare side effects reported include gastrointestinal upset, contact allergies, headache, restless sleep, and mydriasis. Despite these findings, methodological problems found in many of the studies limit these findings and clinical application of this agent.23,31-33
Role of the Pharmacist
Many patients suffering from symptoms of insomnia will seek management with nonprescription agents. Although this may be helpful with occasional insomnia, this is not the treatment of choice for chronic insomnia. When approached by a patient who is having difficulty sleeping, it is important to appropriately assess the patient, inquiring about symptom duration and severity, and to refer patients to their primary care provider for an appropriate diagnosis. Pharmacists can aid in the patient’s understanding of their condition, identify any medications in the patient’s regimen that may potentially have a negative impact on sleep, and recommend nonpharmacologic treatment options that may help improve sleep quality. Pharmacists are also in a prime position to promote the effectiveness of CBT-I to both patients and providers. When CBT-I and lifestyle changes alone have not improved symptoms, pharmacists can be instrumental in helping health- care providers determine which pharmacologic treatment strategies are most appropriate.
Conclusion
Insomnia has become a public health concern that can have a significant impact on a patient’s well- being physically, functionally, and psychologically. It is a disorder that remains underreported and undertreated. Pharmacists are in a unique position to improve sleep health management by reviewing the patient’s medication history and referring patients to their healthcare provider when symptoms of insomnia are present. Pharmacists will be able to discuss and recommend nonpharmacologic interventions, such as sleep hygiene and stimulus control, to help improve sleep. If a patient does decide to use one of the available OTC products, pharmacists will be able to counsel the patient on the appropriate use and expectations and, most importantly, to avoid chronic use of OTC sleep aids. With pharmacists working together with their patients and their patients’ healthcare providers to improve outcomes, patients will finally be on their way to a good night’s sleep.
What Is Insomnia?
Insomnia is a type of sleep disorder that affects up to 20% of adults. People with insomnia have trouble falling or staying asleep and may wake up earlier than they wanted to. They do not feel rested no matter how much they slept, and they sometimes feel tired, groggy, anxious, or irritable throughout the day. This lack of sleep can also increase the risk of other health problems, such as high blood pressure, obesity, diabetes, depression, heart attack, and stroke.
Is Insomnia a Serious Problem?
Insomnia can be a sign of a more serious sleep problem, such as sleep apnea. Not sleeping well at night can also make you sleepier during your waking hours, which can make you an unsafe driver. Many accidents are caused by people who are sleep deprived. You should aim to get at least 7 hours of sleep each day.
Why Do I Have Trouble Sleeping?
There are many reasons why you may have trouble sleeping. Speak with your pharmacist or doctor to help you determine what the cause may be. Some common causes include stress, changes in your sleep environment, loss of a loved one, physical illness and psychological problems, and certain medications.
How Can I Get a Better Night’s Sleep?
The best way to start getting a better night’s sleep is to practice good sleep hygiene. Sleep hygiene describes habits and practices that lead to sleeping well on a regular basis. Many people can greatly improve the quality of their sleep just by using sleep-hygiene techniques. Some examples of these techniques include:
• Following a regular sleep schedule (going to bed and getting up at the same time every day)
• Avoiding afternoon naps
• Avoiding the use of electronics prior to bed
• Avoiding coffee after noon
• Avoiding heavy meals close to bedtime
• Avoiding smoking
• Exercising at least 5 hours before bedtime?
• Keeping a peaceful sleeping environment
Can OTC Medicines Help Me Sleep Better?
Nonprescription sleep aids are often used to help manage symptoms of insomnia. The active ingredient in these products is an antihistamine, such as diphenhydramine or doxylamine. Antihistamines can help the symptoms of insomnia by promoting sleepiness and decreasing the time to sleep onset. They can be helpful if taken approximately 30 minutes before desired bedtime. However, continued use of these medications is strongly discouraged. They carry many side effects and have not been shown safe or effective when used long term. Also, they should not be used in patients who are over age 65 years, have glaucoma, difficulty urinating, a large prostate, or thyroid disorders. Dietary and herbal supplements, such as melatonin and valerian, are sometimes used to help manage insomnia. However, they are not regulated by the FDA and have not been greatly studied for safety or efficacy. Lastly, since insomnia may be a symptom of another medical condition, it is important to speak with your doctor or pharmacist before trying these products.
Where Can I Go for More Information?
National Sleep Foundation: www.thensf.org
American Academy of Sleep Medicine: https://aasm.org/clinical-resources/patient-info/
National Heart, Lung, and Blood Institute—Sleep Deprivation and Deficiency: https://www.nhlbi.nih.gov/health-topics/sleep-deprivation-and-deficiency.
REFERENCES
1. Ford ES, Wheaton AG, Cunningham TJ, et al. Trends in outpa¬tient visits for insomnia, sleep apnea, and prescriptions for sleep medications among US adults: findings from the National Ambula¬tory Medical Care survey 1999-2010. Sleep. 2014;37(8):1283-1293.
2. Institute of Medicine (US) Committee on Sleep Medicine and Research. Colten HR, Altevogt BM, eds. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Washington, DC: National Acade¬mies Press (US); 2006. www.ncbi.nlm.nih.gov/books/NBK19960/. Accessed December 23, 2021.
3. Liu Y, Wheaton AG, Chapman DP, et al. Prevalence of healthy sleep duration among adults—United States, 2014. MMWR Morb Mortal Wkly Rep. 2016;65:137-141.
4. CDC. Sleep and sleep disorders: how much sleep do I need? www.cdc.gov/sleep/about_sleep/how_much_sleep.html. Accessed December 10, 2021.
5. Wheaton AG, Jones SE, Cooper AC, Croft JB. Short sleep duration among middle school and high school students–United States, 2015. MMWR Morb Mortal Wkly Rep. 2018;67:85-90.
6. Watson NF, Badr MS, Belenky G, et al. Recommended amount of sleep for a healthy adult: a joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society. J Clin Sleep Med. 2015;11(06):591-592.
7. Noor ZM, Smith AJ, Smith SS, Nissen LM. A study protocol: a community pharmacy-based intervention for improving the manage¬ment of sleep disorders in the community settings. BMC Health Serv Res. 2014;14:74.
8. Dopheide JA. Insomnia overview: epidemiology, patho¬physiology, diagnosis and monitoring, and nonpharmacologic ther¬apy. Am J Manag Care. 2020;26(4 suppl):S76-S84.
9. Buysse DJ. Insomnia. JAMA. 2013;309(7):706-716.
10. Levenson JC, Kay DB, Buysse DJ. The pathophysiology of insomnia. Chest. 2015;147(4):1179-1192.
11. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: 2013.
12. Spielman AJ. Assessment of insomnia. Clin Psychol Rev. 1986;6:11-25.
13. Wright CD, Tiani AG, Billingsley AL, et al. A framework for understanding the role of psychological processes in disease devel¬opment, maintenance, and treatment: the 3P-Disease Model. Front Psychol. 2019;10:2498.
14. Ebben MR, Spielman AJ. Non-pharmacological treatments for insomnia. J Behav Med. 2009;32(3):244-254.
15. Saper CB, Scammell TE. Emerging therapeutics in sleep. Ann Neurol. 2013;74(3):435-440.
16. Sateia MJ, Buysse DJ, Krystal AD, et al. Clinical practice guide¬line for the pharmacologic treatment of chronic insomnia in adults: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2017;13(2):307-349.
17. Qaseem A, Kansagara D, Forciea MA, et al. Management of chronic insomnia disorder in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2016;165(2):125-133.
18. Williams J, Roth A, Vatthauer K, McCrae CS. Cognitive behav¬ioral treatment of insomnia. Chest. 2013;143(2):554-565.
19. Koffel E, Bramoweth AD, Ulmer CS. Increasing access to and utilization of cognitive behavioral therapy for insomnia (CBT-I): a narrative review. J Gen Intern Med. 2018;33(6):955-962.
20. Schutte-Rodin S, Broch L, Buysse D, et al. Clinical guideline for the evaluation and management of chronic insomnia in adults. J Clin Sleep Med. 2008;4(5):487-504.21. Siebern AT, Suh S, Nowakowski S. Non-pharmacological treat¬ment of insomnia. Neurotherapeutics. 2012;9(4):717-727.
22. Statista. Sleeping aid OTC revenue in United States from 2011 to 2020. www.statista.com/statistics/506604/otc-revenue-of-sleeping-aid-in-the-us/. Accessed December 12, 2021.
23. Meolie AL, Rosen C, Kristo D, et al. Oral nonprescription treatment for insomnia: an evaluation of products with limited evi¬dence. J Clin Sleep Med. 2005;1(2):173-187.
24. FDA, HHS. Labeling of diphenhydramine-containing drug products for over-the-counter human use. Final rule. Fed Regist. 2002;67(235):72555-72559.
25. NIH State of the Science Conference statement on Manifesta¬tions and Management of Chronic Insomnia in Adults statement. J Clin Sleep Med. 2005;1(4):412-421.
26. Morin CM, Benca R. Chronic insomnia. Lancet. 2012;379(9821):1129-1141.
27. Wade AG, Ford I, Crawford G, et al. Nightly treatment of pri¬mary insomnia with prolonged release melatonin for 6 months: a randomized placebo controlled trial on age and endogenous melato¬nin as predictors of efficacy and safety. BMC Med. 2010;8:51.
28. Costello RB, Lentino CV, Boyd CC, et al. The effectiveness of melatonin for promoting healthy sleep: a rapid evidence assessment of the literature. Nutr J. 2014;13:106.
29. Buscemi N, Vandermeer B, Hooton N, et al. The efficacy and safety of exogenous melatonin for primary sleep disorders. A meta-analysis. J Gen Intern Med. 2005;20(12):1151-1158.
30. Ferracioli-Oda E, Qawasmi A, Bloch MH. Meta-analysis: mela¬tonin for the treatment of primary sleep disorders. PloS One. 2013;8(5):e63773.
31. Salter S, Brownie S. Treating primary insomnia—the efficacy of valerian and hops. Aust Fam Physician. 2010;39(6):433-437.
32. Gooneratne NS. Complementary and alternative medicine for sleep disturbances in older adults. Clin Geriatr Med. 2008;24(1):121-138, viii.
33. Morin CM, Koetter U, Bastien C, et al. Valerian-hops combination and diphenhydramine for treating insomnia: a randomized placebo-controlled clinical trial. Sleep. 2005;28(11):1465-1471.
34. Neel AB Jr. Drugs & supplements: 10 medications that can cause sleeplessness. AARP. www.aarp.org/health/drugs-supplements/info-04-2013/medications-that-can-cause-insomnia.html. Accessed December 12, 2021.
35. Liu MT. Current and emerging therapies for insomnia. April 12, 2020. www.ajmc.com/view/current-and-emerging-therapies-for-insomnia. Accessed December 12, 2021.
36. Rosenberg R, Citrome L, Drake CL. Advances in the treatment of chronic insomnia: a narrative review of new nonpharmacologic and pharmacologic therapies. Neuropsychiatr Dis Treat. 2021;17:2549-2566.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





